J Transcat Intervent.2020;28:eA20200009.
Impact of social isolation during COVID-19 pandemic on arrivals at emergency department and on percutaneous coronary intervention for myocardial infarction at a cardiology hospital
DOI: 10.31160/JOTCI202028A20200009
ABSTRACT
Background
Social isolation and marketing campaign to avoid “unnecessary” use of healthcare system to fight against COVID-19 pandemic might impact on the decision to seek medical care. The aim of this study was to evaluate the effect of social isolation during COVID-19 pandemic on trends in numbers of visits to emergency department, non-elective admissions, and percutaneous coronary intervention procedures for treatment of patients with acute myocardial infarction, at a reference cardiology hospital.
Methods
Daily numbers of visits to emergency department, non-elective admissions, and percutaneous coronary intervention procedures for the treatment of patients with acute myocardial infarction, at a high-volume cardiology hospital, were compared in two contiguous 3-week periods, before and during social isolation officially implemented for COVID-19. Mean and standard deviation for each variable were calculated. Comparisons were performed using two-tailed t test with p-value <0.05 for significance.
Results
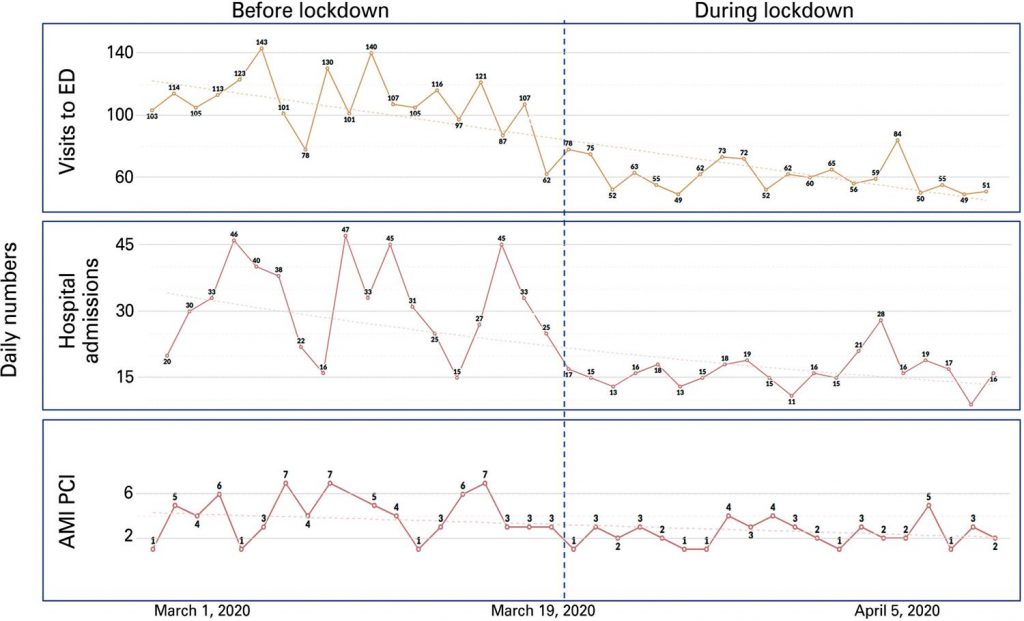
During social isolation, compared to the immediately previous period, the number of visits to emergency department per day decreased by 45% (before: 110.6±16.7 versus during lockdown: 61.1±10.2; p<0.0001), non-elective hospital admissions decreased by 50% (before: 31.7±10.2 versus during social isolation: 16.4±3.8; p<0.0001), and percutaneous coronary intervention procedures for acute myocardial infarction treatment decreased by 29% (before: 7.4±4.0 versus during social isolation: 5.0±2.6; p=0.032).
Conclusion
A marked reduction in number of visits to emergency department, non-elective hospital admissions, and percutaneous coronary intervention for acute myocardial infarction treatment were observed during social isolation, as compared to the period immediately before the COVID-19 pandemic. Such trends raise concerns of underdiagnosis of acute myocardial infarction related to barriers.
1,097