Abstract
Background: In 2018, Ontario implemented a pharmacare program (Ontario Health Insurance Plan Plus [OHIP+]) to provide children and youth younger than 25 years with full coverage for prescription medications in the provincial formulary. We aimed to assess the use of public drug plans and costs of publicly covered prescriptions before and after the program’s implementation and modification.
Methods: We conducted a population-based, interrupted time-series analysis using data on prescription drug claims, from the Canadian Institute for Health Information’s National Prescription Drug Utilization Information System, for people younger than 25 years from January 2016 to October 2019 in Ontario, using British Columbia as the control. We assessed changes in the level and trend of publicly covered prescriptions and expenditures after the introduction of OHIP+ in January 2018 and after program modifications in April 2019. We also assessed plan use and expenditures for publicly covered prescriptions for diabetes and asthma.
Results: Publicly covered prescriptions in Ontario increased by 290%, from 756 per 1000 people before OHIP+ to 2952 per 1000 (p < 0.001) after its implementation. After program modification, prescriptions decreased by 52% to 1421 per 1000 (p < 0.001). Similarly, total public drug expenditures increased by 254%, from $379 million in 2017 to $839 million in 2018, then reduced by 49% to $204 million in 2019. Monthly public plan expenditures increased by $115.94 (95% confidence interval [CI] $100.93 to $130.94) post-OHIP+ implementation and decreased by $99.97 (95% CI −$119.79 to −$80.15) per person per month after April 2019.
Interpretation: Adopting OHIP+ increased use of public drug plans and expenditures for publicly funded prescription medicines, and the program modification was associated with decreases in both outcomes. This study’s findings can inform the national pharmacare debate; future research should investigate associations with health outcomes.
Universal health coverage promotes access to necessary care and protects patients from health-related financial hardship that may affect health outcomes. The World Health Organization declared that governments are obligated to promote universal coverage of essential health care services, including prescription drugs.1–4 Given the importance of reducing out-of-pocket spending for prescription drugs, universal access to affordable, safe and appropriately prescribed treatments is an important goal for health systems in all countries.2–5 However, approaches to universal health coverage for prescription medications or universal pharmacare varies according to the population covered (who), health products and technologies (what) and the extent of coverage (proportion of direct costs covered). The amount spent on prescription drugs, including per capita spending, has significantly increased over time.4–7 Health system expenditure on prescription drugs has also increased in many countries, often growing faster than other health system costs.5–14 Therefore, implementing universal pharmacare can enhance equitable access to needed care and medicines,7–33 which is central to the ongoing debate about the need for a national pharmacare program in Canada.11
Although Canada’s provincial and territorial health systems provide a single-payer system with coverage for medically necessary hospital and physician-based care, this universality does not extend to outpatient prescription medications.2–5 Instead, prescription drugs are funded by a fragmented patchwork of public and private drug plans that varies by province and leaves many Canadians with little or no drug coverage.4–6 Children and youth are a vulnerable population, and studies that have investigated coverage variation have shown that younger adults are the most disadvantaged in coverage.7–23 In Ontario, the provincial government implemented the Ontario Health Insurance Plan Plus (OHIP+) in January 2018, which offered full coverage for publicly covered prescription medications to children and youth younger than 25 years. According to the provincial government, the estimated predicted additional annual investment was $465 million to expand coverage of young people through OHIP+.25,26 However, the initial scope of OHIP+ was modified in April 2019, restricting eligibility to those without private drug plans, most often from parental coverage.25–27 We sought to assess the impact of the introduction and subsequent modification of OHIP+ on the number of publicly covered prescriptions and plan expenditures. Using the same metrics, we also sought to assess prescription medications among the 2 most common chronic conditions (asthma and diabetes) affecting Canadian children and youth.23–27
Methods
Study design
We used an interrupted time-series design to estimate changes in the number of publicly covered prescriptions and plan expenditures. It is a rigorous method to examine the longitudinal effects of introducing new programs and policies, including changes in outcomes of interest, while controlling for pre-existing trends.17–30
Setting and policy intervention
The implementation of OHIP+ in January 2018 and its modification in April 2019 provides 2 time points of interest. The original program offered full coverage for more than 4400 medication products from the Ontario Drug Benefit formulary for children and youth younger than 25 years. In April 2019, the program was modified to exclude those covered by private drug plans and those eligible for the Ontario Drug Benefit program (e.g., through the Trillium Drug Program and those receiving social assistance). We used the province of British Columbia as a nonequivalent control jurisdiction, as it had comparable coverage for youth and children and similar social assistance programs during the study period.
Data sources
The National Prescription Drug Utilization Information System (NPDUIS) provided anonymized, aggregated data on public prescriptions and drug plan reimbursement benefits for Ontario and BC for the 24 months preceding and 15 months following the adoption of OHIP+, and the 7 months after its modification. The NPDUIS, operated by the Canadian Institute for Health Information, is a data repository of public drug coverage plans from all provinces and territories except Quebec, Nunavut and the Northwest Territories, excluding those covered by provincial workers’ compensation boards or federal drug programs. The NPDUIS has additional formulary data on which drugs are included in public drug plans, and the posted costs of prescribed drugs (as opposed to the negotiated price deductions), as well as prescription utilization. The data set for Ontario and BC included medication class, product name, the dose of the drug, the number of active beneficiaries enrolled in the plan over each month, the number of paid beneficiaries, the number of prescriptions and the amount the program paid for reimbursed claims.8
Outcomes
The primary outcome variables included the number and rate of publicly covered prescriptions, and public plan expenditures in Ontario and BC through the study period. To calculate the overall utilization rate of public drug plans, we used the number of publicly covered prescriptions, recorded as the total number of claims accepted per month, divided by the population aged 24 years and younger for both provinces, linearly interpolated for each month from annual Statistics Canada population estimates. We made the same calculations for the secondary analysis on prescription medications for asthma and diabetes. Overall, we calculated public plan expenditure as the average monthly public reimbursement in dollars per person and per 1000 population for all prescription drugs for Ontario and BC. The Ontario and BC population were linearly interpolated for each month from annual Statistics Canada population estimates over the study period.
Statistical analysis
We used a segmented regression analysis model. We calculated utilization rates in the following 3 segments for Ontario and BC based on the utilization aggregate numbers provided in the NPDUIS data, each with multiple observation periods: before adoption of OHIP+, after the adoption of OHIP+ and after the modification of OHIP+. We fit the segmented regression models using a generalized least squares model and incorporated appropriate autocorrelation parameters for each model based on standard diagnostic criteria.19 The intervention and control group models included terms for the existing level and linear trend in the outcome and changes or shifts on both the level and linear trend. They also had an indicator variable for January, when use and cost change with a rollover of OHIP+. Our underlying model assumption was that the Ontario trend would change similarly to BC, without OHIP+. We differenced the outcomes between the intervention and the control group and plotted the counterfactuals from the models for both groups. We did not conduct any sensitivity analyses.
Ethics approval
Ethics approval was provided by the Hamilton Integrated Research Ethics Board before conducting the study (no. 10991-C).
Results
Table 1 contains data on the monthly counts and selected characteristics of the Ontario residents younger than 25 years who were eligible for OHIP+ and who filled publicly covered prescriptions during the study period. The study sample from Ontario was evenly balanced by age group (0–17 yr and 18–25 yr) and gender, but not by socioeconomic status, as 60% of those who received the publicly covered prescriptions during the pre-OHIP+ period were of either low or low–middle socioeconomic status. Use of public drug plans was evenly distributed by income quintile when the full OHIP+ plan was in place. The number of people covered by all public drug plans in Ontario and BC averaged 260 930 and 119 881 per month, respectively.
Characteristics of the Ontario sample
Overall use of public drug plans
Overall, 24 869 544 publicly covered prescriptions were paid for by the benefits plan over the 46-month study period.
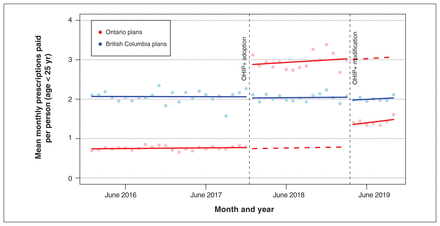
As shown in Figure 1 and Table 2, we found a level increase rate of 2.13 publicly covered prescriptions per person (age < 25 yr) per month paid for by the plans at OHIP+ implementation (95% confidence interval [CI] 1.89 to 2.37) and a significant immediate level drop of −1.61 (95% CI −1.95 to −1.26) at its modification; we did not observe a statistically significant increase in the trends after that time point. Compared with BC, where utilization was stable, publicly covered prescriptions in Ontario increased by 290%, from 756 per 1000 young people in the 2 years before OHIP+ implementation to 2952 per 1000 from January 2018 to April 2019, then decreased by 52% to 1421 per 1000, as shown in Table 3. Government total annual costs increased by $460 million, then decreased by 49% to 204 million.
Average monthly number of publicly covered prescriptions per person (age < 25 yr), where at least a portion was paid by the provincial public benefits plan, before and after the adoption and modification of the Ontario Health Insurance Plan Plus (OHIP+) in January 2018 and in April 2019, respectively. Note: The solid lines represent the estimated monthly rates, and dashed lines (counterfactual) represent predicated estimates.
Effect of Ontario Health Insurance Plan Plus (OHIP+) on rate change in monthly publicly covered prescriptions and plan expenditure volumes
Changes in publicly covered prescriptions and plan expenditure volumes after the adoption and modification of Ontario Health Insurance Plan Plus (OHIP+)
Use of public drug plans for asthma and diabetes prescriptions
As shown in Table 2, we found an immediate increase of 0.27 publicly covered prescriptions per person per month for asthma paid for by the plans after the adoption of OHIP+ (95% CI 0.20 to 0.35) and an immediate drop of 0.16 of the same after its modification (95% CI −0.24 to −0.08). On the other hand, we found a level increase of 0.02 (95% CI 0.01 to 0.04) publicly covered drug prescriptions per person per month for diabetes paid for by the plans after the adoption of OHIP+ and a significant immediate drop of −0.02 (95% CI −0.04 to −0.02) after its modification. There was no statistically significant change in the trends for either policy interventions.
There were substantial increases of 100% or more in the monthly mean publicly covered prescriptions for asthma and diabetes, and then decreases for overall and individual prescriptions by 50% or more, with the adoption and modification of OHIP+, respectively (Table 3). The largest increases (> 900%) for asthma prescriptions were reported for omalizumab, mometasone, vilanterol fluticasone and budesonide (Table 3 and Appendix 1, available at www.cmajopen.ca/content/10/3/E848/suppl/DC1). The largest declines (> 90%) were for ivacaftor and mometasone. For diabetes prescriptions, the largest increase was for insulin glulisine and empagliflozin (both with > 700% change). The largest decline (> 65%) was found for insulin detemir, insulin aspart and diagnostic test strips (Table 3 and Appendix 1).
Prescription drug plan expenditures
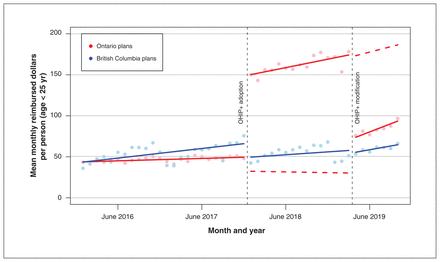
The total number of publicly covered prescription and plan expenditures reimbursed by the benefits plan over the 46 months was $1 421 248 106. As shown in Figure 2, there was an increased plan expenditure rate of $115.94 (95% CI $100.93 to $130.94) per person (age < 25 yr) per month after the adoption of OHIP+ and a level drop of $99.97 (95% CI −$119.79 to −$80.15) after its modification. The estimated trend change noted a slight monthly increase of $1.86 (95% CI −$0.27 to $3.46) per person per month, with a trend change in the opposite direction after modification. Compared with the stable BC utilization, plan expenditures in Ontario increased by 252%, from a mean of $4602 per 1000 young people in the 2 years before OHIP+ implementation to $16 202 per 1000 from January 2018 to April 2019, which then decreased by 99% to $1606 per 1000 after modification.
Interrupted time-series analysis of overall reimbursed dollars per person (age < 25 yr), before and after the adoption and modification of the Ontario Health Insurance Plan Plus (OHIP+) in January 2018 and in April 2019, respectively. Note: The solid lines represent the estimated monthly rates and dashed lines (counterfactual) represent predicated estimates.
Plan expenditures for asthma and diabetes drug prescriptions
As shown in Table 2, we found an immediate increase in the plan expenditure rate of $12.80 (95% CI $10.85 to $14.76) per person per month for asthma prescriptions reimbursed by the benefits plans after the adoption of the first OHIP+ policy, and a subsequent immediate drop of $8.58 (95% CI −$10.82 to −$6.33) per person per month after modification. After the adoption of OHIP+, the estimated trend change was $0.04 (95% CI −$0.23 to $0.31) per person per month. For diabetes, drug plan expenditure increased by $2.80 (95% CI $1.15 to $4.10) per person per month after adopting OHIP+ and a level drop of $2.30 (95% CI −$3.60 to −$1.80) after the program modification. There was no statistically significant change in the trend for either policy interventions.
Many of the changes in plan expenditures for asthma and diabetes were substantial, with reimbursements increasing by 100% or more and dropping for the overall and individual prescriptions by 50% or more after the program modification (Table 3). The largest increases in the monthly mean for publicly covered asthma prescriptions plan expenditures was for omalizumab, mometasone, ipratropium, tiotropium and budesonide (above 900% change), and the largest declines were for ivacaftor and ipratropium (> 90% change). For diabetes prescriptions, the most significant increases were for empagliflozin, dapagliflozin and insulin glulisine (> 800%), and the largest declines were for dapagliflozin and insulin detemir (> 70% change) (Appendix 1).
Interpretation
Findings from this study have implications both for policy and future research. For policy, our results can be used to inform the ongoing discussions regarding a national, universal pharmacare program in Canada. Expanding coverage would increase access to prescription medicines (essential and nonessential) and would likely reduce cost burdens on many people in lower socioeconomic strata, but would increase costs for governments by an amount that appears to be predictable. Future research should focus on implementing and modifying OHIP+ by type of insuree — based on age, sex and social economic status (i.e., income quantile categories) — and their health outcomes, as this would generate the crucial data for cost-effectiveness analysis.
Our study aligns with others that have found that public prescription drug plans that provide noncatastrophic, first-dollar coverage increase use of public coverage for medications. 5–7,34–43 Expanded coverage, on the other hand, may not improve clinical outcomes because access or adherence is not sufficiently improved, or because the benefit of essential medicines is outweighed by the lack of benefit from nonessential or harmful medicines, which would likely reduce cost burdens for many people but would increase costs for governments.41 Other studies have suggested that higher financial coverage promotes higher use of and financial access to drugs among populations.1,16,41 In contrast, a more restrictive model of universal drug coverage offers limited access and mixed drug expenditure based on the payer.1,4,6,16
From a societal perspective (i.e., total use and costs from both private and public plan coverage), the total cost of medications would change if the total use per person changed after OHIP+ coverage or the total costs per medication changed. The utilization patterns in our study partially support those from the Telus report,44,45 which found a 54% decrease in private plan expenditures and a similar increase in use of government public coverage after the implementation of OHIP+, and a 28% increase in private plans and an equal decrease in use of public plan coverage after the restriction of OHIP+ coverage to those without private coverage in 2019.44 The cost to private insurance plans for drug therapies would likely be higher than the cost to public plans for the same drugs.44,45
Given limitations in data access, we did not assess impacts by type of insuree or clinical outcomes. This is crucial data to pursue, as improving health outcomes is the ultimate goal of these policy changes. Randomized trials were undertaken in the United States and Canada to examine the health outcomes and adherence of patients who were provided free access to their medications,41,46 and reported no improvement in health outcomes. However, the recently published CLEANMeds randomized trial, which involved Ontario patients with cost-related nonadherence, showed improved adherence and reduced health care costs over the 2-year follow-up period.42 Further work on the cost-effectiveness of various drug coverage policies is essential.42,43,46 We are not aware of a randomized trial that has evaluated free essential medications just for children and youth, which is arguably the group likely to prove the most cost effective, given lower per-person costs and longer life-years remaining. Expanded financial coverage likely accounted for the increase in use of the publicly covered prescription drug plans found in our study.
We used province-wide data to calculate utilization rates and plan expenditure, which provides a robust assessment of the impact of OHIP+ and its modification on these outcomes. Although we could not conduct an assessment from a societal perspective given a lack of access to data from private drug plans, our findings still provide a clear picture for health care planners on the likely cost of implementing universal pharmacare. Therefore, public plans across Canada can use these data with their current utilization data to estimate the probable cost of providing first-dollar coverage for prescription drugs for children and youth of their population. Similarly, the study findings help inform the national debate in Canada about a national pharmacare program, which would enhance equitable access to medications.
Limitations
The limitations of our study include selecting a small number of indicators based on what was available through NPDUIS. In addition, although we are unaware of any changes that may have affected plan beneficiaries around the time of the OHIP+ policy change, there is potential for bias in our estimates if such changes did occur and these confounders were not included in our models. Other limitations are lack of data on offsets on utilization and costs from private plans and from self-pay, on patient clinical outcomes and on impacts by type of insuree.
Conclusion
Adopting a universal pharmacare (OHIP+) for Ontarians aged younger than 25 years increased the number of publicly covered prescriptions and public expenditures considerably, with a decrease in both after the modification of the program. Our findings can inform the debate over national pharmacare, which would enhance equitable access to medications, and largely confirmed the government-predicted additional cost of OHIP+. Future research should focus on examining associations of implementing OHIP+ and changes in policy with health outcomes so that cost-effectiveness can be estimated.
Acknowledgements
The authors acknowledge Florence Mwango and Lawrence Mbuagbaw for contributing to the analyses of the manuscript.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: All authors contributed to the study conception and design. Benard Miregwa carried out the analyses and drafted the manuscript. All of the authors revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: Data were provided from the Canadian Institute for Health Information National Prescription Drug Utilization Information System through the Graduate Student Access Program. This study was funded in part by a Foundation Scheme Grant from the Canadian Institutes of Health Research (FDN-148412).
Data sharing: All data for this study are available to inform stakeholders and enhance knowledge in the field so long as it is cited appropriately.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/10/3/E848/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2022 CMA Impact Inc. or its licensors