Published online May 7, 2006. doi: 10.3748/wjg.v12.i17.2798
Revised: January 7, 2006
Accepted: January 14, 2006
Published online: May 7, 2006
A 23-year-old man with post-traumatic hepatic artery pseudo-aneurysm and subphrenic liver abscess was admitted. He underwent coil embolization of hepatic artery pseudo-aneurysm. The pseudo-aneurysm was successfully obstructed and subphrenic liver abscess was controlled. Super-selective trans-catheter coil embolization may represent an effective treatment for hepatic artery pseudo-aneurysm combined with subphrenic liver abscess in the absence of other therapeutic alternatives.
- Citation: Sun L, Guan YS, Wu H, Pan WM, Li X, He Q, Liu Y. Post-traumatic hepatic artery pseudo-aneurysm combined with subphrenic liver abscess treated with embolization. World J Gastroenterol 2006; 12(17): 2798-2799
- URL: https://www.wjgnet.com/1007-9327/full/v12/i17/2798.htm
- DOI: https://dx.doi.org/10.3748/wjg.v12.i17.2798
Hepatic artery pseudo-aneurysm is a rare complication of blunt abdominal trauma. Diagnosis is frequently delayed and made by splanchnic angiography. Most of the indications for surgical treatment may disappear after selective catheterization and embolization. We report a case of a 23-year-old man with a history of hepatic trauma. Subphrenic abscess formation after laparotomy and right hepatic artery pseudoaneurysm were diagnosed by enhanced computer tomography (CT). The lesion was confirmed by arteriography and managed with trans-catheter embolization.
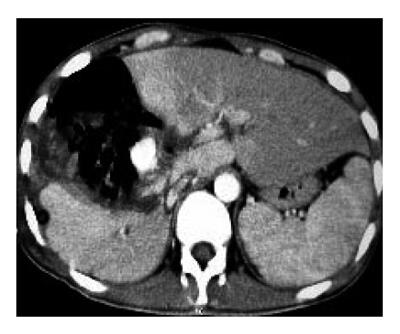
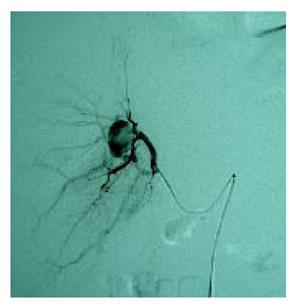
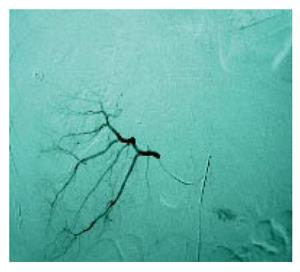
We report a case of a 23-year-old man with a severe blunt abdominal trauma caused by a car accident. An immediate laparotomy was performed due to a severe collapse upon admission and a liver fracture was observed. He gradually recovered and a subphrenic abscess occurred on day 10 after operation. Abdominal CT scanning revealed a complex subphrenic abscess and a pseudo-aneurysm of the right hepatic artery (Figure 1). Selective angiography confirmed the diagnosis of right artery pseudo-aneurysm (Figure 2) and the aneurysm was occluded by trans-catheter embolization. This was accomplished uneventfully with placement of two 5mm coils into the aneurysm and right hepatic artery was unblocked (Figure 3). The 14-F drainage catheters containing semi-solid necrotic material were placed into these collections. Eventually, recovery was complete. The classical embolization could avoid surgical treatment with a high morbidity.
The liver is the largest solid abdominal organ with a relatively fixed position, which makes it prone to injury. The most common cause of liver injury is blunt abdominal trauma, secondary to motor vehicle accidents in most instances. In the past, most of these injuries were treated surgically. However, surgical literature indicates that as high as 86% of liver injuries have stopped bleeding at the time when surgical exploration is performed, and 67% of operations performed for blunt abdominal trauma are non-therapeutic[1-2].
As a result of this high mortality rate, emergency surgery is frequently indicated in patients with hepatic injury in the past. However, with better monitoring facilities and imaging techniques, most patients with blunt abdominal trauma are now treated conservatively. Pseudoaneurysms are better depicted by spiral or multi-section CT because of the ability to image during peak contrast enhancement[3].
Complications of liver trauma occur in approximately 20% of patients, including delayed rupture (very rare), hemobilia, arterio-venous fistula, pseudo-aneurysm, biloma and abscess formation[4]. There are many potential causes of liver abscesses, such as appendicitis, diverticulitis, or a perforated bowel, infection in blood, infection of the biliary (liver secretion) tract, or trauma with bruised liver infection[5].
The most common bacteria that cause liver abscesses are escherichia coli, klebsiella, enterococcus, and bacteroides. The death rate is 10%-30% in treated pa-tients, and higher in those with multiple abscesses. Life-threatening sepsis can develop. The treatment usually consists of surgical or percutaneous (through the skin, with a needle) drainage of the abscess. This is accompanied with a prolonged antibiotic therapy. Sometimes antibiotics alone can cure the infection. Occasionally, patients with blunt abdominal trauma do well initially, but subsequently develop a liver abscess, presumably due to unrecognized liver damage. These patients have signs and symptoms of deep-seated infection[6-7].
A dynamic angiographic study may demonstrate the site of active bleeding and the sac of pseudoaneurysms. Trans-catheter embolization may be the only treatment required. Superselective catheterization should be performed as far as possible. Both afferent and efferent vessels of pseudo-aneurysms or aneurysms should be occluded to prevent their retrograde filling[8]. Initially, the surgeon may control the hemorrhage by temporary perihepatic packing. Recurrent liver parenchymal bleeding can be treated successfully with trans-catheter embolization, and placement of an intravenous stent can control bleeding from a major hepatic vein[9].
Embolization can be performed for the control of persistent arterial hemorrhage which may occur due to stab wounds of the liver, and for the occlusion of pseudo-aneurysm. Trans-catheter arterial embolization may reduce transfusion requirements and allow healing of hepatic injuries without surgery. Because hepatic arteries are not the end arteries, occlusive devices should be deployed distal to the lesion to prevent collateral backdoor filling. The entire hepatic artery may be occluded if required, as long as the portal vein is patent. If the portal vein is occluded, only selective embolization can be performed to prevent liver infarction due to the presence of intrahepatic collaterals[10].
S- Editor Wang J L- Editor Wang XL E- Editor Liu WF
| 1. | Keller MS. Blunt injury to solid abdominal organs. Semin Pediatr Surg. 2004;13:106-111. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 20] [Cited by in F6Publishing: 20] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 2. | Ott R, Schön MR, Seidel S, Schuster E, Josten C, Hauss J. [Surgical management, prognostic factors, and outcome in hepatic trauma]. Unfallchirurg. 2005;108:127-134. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 5] [Cited by in F6Publishing: 5] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 3. | Romano L, Giovine S, Guidi G, Tortora G, Cinque T, Romano S. Hepatic trauma: CT findings and considerations based on our experience in emergency diagnostic imaging. Eur J Radiol. 2004;50:59-66. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 47] [Cited by in F6Publishing: 28] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 4. | Gopanpallikar A, Rathi P, Sawant P, Gupta R, Dhadphale S, Deshmukh HL. Hepatic artery pseudoaneurysm associated with amebic liver abscess presenting as upper GI hemorrhage. Am J Gastroenterol. 1997;92:1391-1393. [PubMed] [Cited in This Article: ] |
| 5. | Zibari GB, Maguire S, Aultman DF, McMillan RW, McDonald JC. Pyogenic liver abscess. Surg Infect (Larchmt). 2000;1:15-21. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 41] [Cited by in F6Publishing: 33] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 6. | Hsieh CH. Comparison of hepatic abscess after operative and nonoperative management of isolated blunt liver trauma. Int Surg. 2002;87:178-184. [PubMed] [Cited in This Article: ] |
| 7. | Szentkereszty Z, Péter M, Erdélyi G, Sápy P. [Results of surgical treatment of liver abscess, with special emphasis of percutaneous puncture and drainage]. Magy Seb. 2000;53:259-262. [PubMed] [Cited in This Article: ] |
| 8. | Forlee MV, Krige JE, Welman CJ, Beningfield SJ. Haemobilia after penetrating and blunt liver injury: treatment with selective hepatic artery embolisation. Injury. 2004;35:23-28. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 43] [Cited by in F6Publishing: 46] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 9. | Baha B, Meyer PG, Brunelle F, Orliaguet G, Michel JL, Carli P. A case of hepatic pseudoaneurysm treated with percutaneous embolization in a child with multiple trauma. Ann Fr Anesth Reanim. 2001;20:786-790. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 11] [Cited by in F6Publishing: 11] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 10. | Mahi M, Chellaoui M, Chat L, Achabaan F, Alami D, Najid A, el Hassani M, Benamour-Ammar H. Post-traumatic hepatic artery pseudoaneurysm. A case report. Arch Pediatr. 2001;8:720-723. [PubMed] [DOI] [Cited in This Article: ] [Cited by in Crossref: 5] [Cited by in F6Publishing: 5] [Article Influence: 0.2] [Reference Citation Analysis (0)] |