Abstract
Sedative agents are widely used in the management of patients with head injury. These drugs can facilitate assisted ventilation and may provide useful reductions in cerebral oxygen demand. However, they may compromise cerebral oxygen delivery via their cardiovascular effects. In addition, individual sedative agents have specific and sometimes serious adverse effects. This review focuses on the different classes of sedative agents used in head injury, with a discussion of their role in the context of clinical pathophysiology. While there is no sedative that has all the desirable characteristics for an agent in this clinical setting, careful titration of dose, combination of agents, and a clear understanding of the pathophysiology and pharmacology of these agents will allow safe sedative administration in head injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Sedation in any intensive care setting is used to provide anxiolysis, amnesia and to relieve agitation. In head-injured patients undergoing mechanical ventilation, sedation enables the manipulation of respiration, which may be essential in the treatment of raised intracranial pressure (ICP). Sedative agents are also an intrinsic part of the treatment of raised ICP because of their actions on cerebral metabolic rate (CMRO2) and cerebral blood flow (CBF). Pain relief may also be required, usually by the addition of an intravenous opioid, which has an additive effect on the sedative agent used. The purpose of this review is firstly to discuss the pathophysiology of head injury, then to discuss the sedatives available for the treatment of adult head-injured patients. It is important to make two additional points.
First, the use of sedative agents in head-injured patients should be viewed as part of their overall management. Such management is ideally based on guidelines that have been provided by the Brain Trauma Foundation and the American Association of Neurological Surgeons.[1] While these guidelines provide comprehensive evaluation of the scientific basis of clinical head injury management in many areas, guidance on sedative use is limited, with the exception of barbiturate use for refractory intracranial hypertension.
Second, much of the scientific basis for making decisions regarding sedative use in this context derives from studies in the operating theatre setting. While such data are extremely valuable, they cannot always be directly extrapolated to provide a foundation for intensive care practice. Results from studies in the operating room are usually ‘contaminated’ by the use of other anaesthetic drugs. On the other hand, the critical care scenario may be confounded by other factors. Extracranial injuries may alter haemodynamic responses, organ dysfunction may substantially delay drug elimination, and concomitant drug treatment can result in pharmacokinetic interactions. Perhaps most importantly, the duration of sedation in the intensive care unit (ICU) setting (days to weeks) may result in problems that would not be detectable, even with long anaesthesia-based studies, which last hours.
A recent position paper from the Society of Critical Care Medicine[2] provides valuable guidelines on the sustained use of sedatives and analgesic agents in critically ill adults. Unfortunately, although the paper contains a useful discussion of the pharmacology of many of the agents used, it provides little specific guidance regarding such treatments in the head-injured population. In particular, there is no discussion on the titration of sedative agents in patients with neurological injury, in whom standard sedation scales are inappropriate.
1. Pathophysiology in Head Injury
The effects of head injury occur not only in the CNS,[3] but are widespread throughout many body systems.
1.1 Pathophysiology: Secondary Neuronal Injury and Cerebrovascular Homeostasis
Damage to the CNS due to head injury can be divided into the primary and secondary injury. The primary injury occurs with the initial impact and is caused by direct damage, flexion, extension and shearing forces. These insults may cause diffuse axonal injury, cerebral oedema and intracranial haematomas, leading to raised ICP, a reduction in cerebral perfusion pressure (CPP), and cerebral ischaemia. Secondary damage occurs after the initial trauma as a result of insults such as hypoxia, hypercapnia, systemic hypotension and intracranial hypertension. It is these derangements that appropriate resuscitation and subsequent intensive care management aim to avoid. Secondary damage occurs due to a number of processes at the subcellular level. These include accumulation of excitatory amino acids (EAA) that cause accumulation of intracellular calcium ions by their action on N-methyl-D-aspartate (NMDA) receptors,[4] phospholipase activation,[5] free radical generation and lipid peroxidation.[6]
There is an intimate and continuing interplay between the various steps of the cascade described above.[3] Un-evacuated intracranial haematomas may not only raise ICP and worsen cerebral hypoxia, but may also be responsible for the activation or intensification of EAA release, inflammation and microvascular dysfunction. The microvascular dysfunction, in turn, may limit the ability of the injured brain to cope with minor variations in physiology. Indeed, while the normal brain has the autoregulatory capacity to cope with mild hypotension that results in CPP reduction to 50mm Hg, it has been well documented that patients with acute head injury, as a group, tend to require CPP values above 60–70mm Hg in order to maintain cerebral perfusion (see later in this section). Further, at later stages after head injury, the presence of extravascular blood may predispose to large vessel spasm, with the potential for distal hypoperfusion and ischaemia.
The varied pathophysiological consequences of a single structural pathology are well reflected by sequential changes in cerebrovascular physiology that are observed following head injury. Classically, CBF is thought to show a triphasic behaviour (figure 1).[7] Soon after head injury (<12 hours), global CBF is reduced, sometimes to ischaemic levels. Between 12 and 24 hours post-injury, CBF increases, and the brain may exhibit supranormal CBF. Many reports refer to this phenomenon as hyperaemia, and CBF levels may be inappropriately high for metabolic needs in many patients beyond the first 24 hours after head injury. However, some patients may not exhibit reductions in cerebral oxygen extraction, suggesting that metabolism and blood flow often remain coupled, and a more appropriate label in these patients would be hyperperfusion. CBF values begin to fall several days following head injury, and in some patients these reductions in CBF may be associated with marked increases in large vessel flow velocity on transcranial Doppler ultrasound, which suggest vasospasm.
Schematic diagram of cerebral blood flow (CBF) responses following closed head injury (lower panel). The upper panel shows the relationship of these changes to pathophysiological mechanisms responsible for intracranial hypertension, with ischaemic cytotoxic oedema contributing at early time points, and vascular engorgement and vasogenic oedema due to blood-brain barrier leak contributing later (reproduced from Bullock[8] with permission). ICP = intracranial pressure.
These time-varying haemodynamic responses also define the vascular contribution to ICP elevation in time.[3] Immediately after head injury, there is no vascular engorgement, and although a transient blood-brain barrier (BBB) leak has been reported in the immediate period after impact in animals, there is no evidence of BBB disruption at this stage in humans. Apart from surgical lesions (e.g. intracranial haematomas), ICP elevation during this phase is often the consequence of cytotoxic oedema, usually secondary to cerebral ischaemia. Increases in CBF and cerebral blood volume (CBV) from the second day post-injury onward make vascular engorgement an important contributor to intracranial hypertension. The BBB appears to become leaky between the second and fifth days post-trauma, and vasogenic oedema then contributes to brain swelling. If these patterns were consistent and predictable, they would allow the rational selection of treatment at each stage following trauma. Unfortunately, patients vary enormously, and different mechanisms responsible for intracranial hypertension may operate concurrently, even within a single individual at any given time point. However, the discussion above does apply to groups, and provides a useful basis on which to select initial ‘best guess’ therapy in an individual patient, especially when data from multimodality monitoring are also available to help guide treatment choices.
The ability of the cerebral circulation to maintain CBF at a relatively constant level in the face of changes in CPP by altering cerebrovascular resistance (CVR) is termed autoregulation (figure 2).[9] In normal circumstances, as both ICP and cerebral venous pressure are low, systemic arterial perfusion pressure becomes the primary determinant of CPP. In pathological states, however, ICP becomes a significant factor in determining CPP. Autoregulation has limits above and below which CBF is directly related to perfusion pressure. Above the higher limit of autoregulation, increases in mean arterial pressure (MAP) lead to forced dilatation of cerebral arterioles, an increase in CBV, disruption of the BBB and formation of cerebral oedema, with a resultant increase in ICP. Below the lower autoregulatory limit, CBF falls linearly with decreasing perfusion pressure. Brain injury is known to disrupt autoregulation in many patients. In this setting, changes in MAP modulate cerebral perfusion at levels that would normally be associated with preservation of CBF at constant levels. Intensive care management of head-injured patients therefore focuses on minimising the ICP and maintaining the CPP. It has been well reported that intracranial hypertension is associated with a poor outcome following head injury,[10–12] and evidence suggests that cerebral autoregulation is preserved when CPP is kept above 60–70mm Hg,[13–15] with recent evidence favouring the lower of these two figures.[16] Local mechanisms for the control of CBF are also disturbed following head injury, leading to altered coupling between CBF and metabolic demands. Clinical studies suggest an initial severe reduction in CBF in the first 3–8 hours after head injury, followed by a gradual increase until metabolic demands are met.[17–20] The level of cerebral metabolism, the preservation of flow metabolism coupling, and the efficiency of autoregulation are crucial issues in predicting the effect of sedation on cerebral blood flow and intracranial pressure. Agents that reduce cerebral metabolism may be beneficial in head injury for two reasons. First, they may reduce oxygen demands in the setting of limited oxygen delivery. Second, these reductions in cerebral metabolism will be coupled to reductions in CBF when flow-metabolism coupling is preserved. Since such CBF reductions are accomplished by reductions in vascular calibre, this will result in reductions in cerebral blood volume, and (especially in patients with a non-compliant intracranial cavity), consequent reductions in ICP and increases in CPP. However, these benefits may be substantially attenuated or absent if baseline metabolism is low and not suppressible by depressant drugs, e.g. in the setting of an isoelectric or burst-suppressed electroencephalogram (EEG), or if flow metabolism coupling is deranged (as in hyperaemia). Under such circumstances, the dominant effects may be due to cardiovascular depression, which is a recognised adverse effect of most sedative agents. This may result in MAP reduction below autoregulatory thresholds and result in reductions in CBF. MAP reduction may also trigger autoregulatory vasodilatation and result in increases in CBV and ICP.
Pressure autoregulation. A change in cerebrovascular resistance in the face of changes in cerebral perfusion pressure to maintain cerebral blood flow (CBF). Note that cerebral vasodilatation and thus a decrease in cerebrovascular resistance (CVR) maintains CBF, with reductions in cerebral perfusion pressure. This increases cerebral blood volume (CBV), which results in critical increases in intracranial pressure in patients with poor intracranial compliance. The process is reversed with elevation of cerebral perfusion pressure (CPP), and increases in mean arterial pressure (MAP) may induce reductions in intracranial pressure due to reflex vasoconstriction in patients with preserved cerebrovascular pressure autoregulation.
1.2 Extracranial Injury — Pathophysiology and Clinical Impact
The effects of sedative agents on cardiorespiratory function are further enhanced by extracranial injuries, or by complications that directly result from head injury. A study of 734 patients with severe head injury showed that electrolyte disturbances were the most frequent complication, occurring in 59% of patients, followed by pulmonary infections (41%), shock (29%), coagulopathy (19%) and septicaemia (10%).[21] Haemodynamic abnormalities[22,23] and dysrhythmias[24,25] are common following head injury, and overt myocardial damage was shown to occur in up to 50% of head-injured patients in the absence of coronary artery disease.[26] These abnormalities sensitise patients to the cardiovascular depressant effects of common sedative agents. Further, abnormal autonomic responses following head injury[27,28] may result in exaggerated or unusual responses to sedation and its associated attenuation of sympathetic activity. Tracheal intubation and/or ventilatory support are often required in severe head injury because of depressed airway reflexes, hypoventilation, or the development of aspiration pneumonia or neurogenic pulmonary oedema.[29–32] Ventilation to mild hypocapnia, with or without neuromuscular blockade, may also be required for ICP control. These factors necessitate the used of sedative agents to facilitate ventilation, since patients who exhibit substantial ventilator asynchrony may suffer substantial increases in intrathoracic pressure (and hence ICP). Patients who receive neuromuscular blocking agents usually receive intravenous benzodiazepines or anaesthetic agents in Europe, but it is not uncommon for such patients to receive only opioids in the US. There are no systematic investigations of the risks of awareness in such patients, but there is no suggestion that this is a problem, even in those patients who receive opioids as their sole sedative agent.
In many patients with severe head injury, gastric emptying is delayed, and this may persist for up to 2 weeks after traumatic head injury.[33] Delayed gastric emptying may be a direct consequence of raised ICP.[34] This may be more of a problem with more severe head injury,[35] and may be due to activity of inhibitory vagal pathways that reduce the amplitude of gastric contractions.[36]
Although at least one study showed no improvement in gastric emptying as a result of withholding morphine in head injury,[34] it is generally felt that sedative and analgesic agents (particularly opioids) can further exacerbate this problem. Impaired gastric emptying may delay the establishment of enteral nutrition; this may result in malnutrition, a need to resort to parenteral nutrition, and/or a perceived requirement for prophylaxis against stress ulceration.[37]
2. Overview of Sedative Agents
2.1 Context for Use of Sedation in Head Injury
Following head injury, sedation may be instituted in emergency situations in the pre-hospital phase. More commonly, it is instituted in the Accident and Emergency Department, usually to allow airway control. Continued use may be required in the short term, e.g. to allow an agitated patient to undergo radiological imaging. It may be required in the longer term on the neurocritical care unit (NCCU). Sedation on the NCCU is required to provide the amnesia, anxiolysis and compliance with treatment that is required on any intensive care unit. In addition, it may represent an intrinsic part of the management of the head-injured patient, by reduction of cerebral metabolism, with coupled reductions in CBV and hence ICP. Such agents may also be required for the control of refractory acute post-traumatic epilepsy.
2.2 Properties of the Ideal Sedative Agent
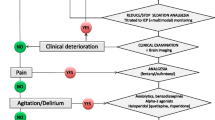
The concept of the ‘ideal’ sedative agent must be modified for use on the NCCU. Traditional properties of the ideal sedative, and the additional demands made by neurointensive care are specified in table I and figure 3. Perhaps more so than in any other critical care setting, there is a need for ease of ability to titrate for sedation in head injury. Such patients may require rapid increases in levels of sedation to cover clinical procedures or other stimuli, which could result in dangerous ICP elevations if left untreated. Some patients may require high doses of sedatives to achieve metabolic suppression. Indeed, several of the drugs that we use can not produce such profound metabolic suppression, and it is important to understand the pharmacodynamic profiles of the agents commonly used in this setting (figure 4).
Desirable organ-specific effects of the ideal sedative agent. Several organ systems may be compromised by extracranial injury and by the pathophysiological consequences of head injury, making patients more susceptible to unwanted effects of sedative agents. CMRO 2 = cerebral metabolism; ↓ = decrease.
Schematic diagram showing the effect of different sedative agents on cerebral metabolism (CMRO2) and coupled cerebral blood flow (CBF). It demonstrates the ‘ceiling’ effect on these parameters of benzodiazepines and opioids. Barbiturates and other anaesthetics, in sufficient doses, will reduce metabolism to a point where the electroencephalogram (EEG) is isoelectric and metabolism has been reduced to basal levels. IV = intravenous.
On the other hand, there may be a clinical need to achieve a rapid reversal of sedation to enable neurological assessment, and it would be highly desirable to be certain that a depressed conscious level after cessation of sedation was not the consequence of residual effects of the drugs used. These considerations underline the need for drugs that not only have a rapid onset, but also a rapid offset. Commonly used agents, such as thiopental sodium (thiopentone) and fentanyl, have apparently short lasting effects when used as a single bolus. However, cessation of drug action in these settings is achieved by rapid redistribution of the drug to a large volume of distribution (Vd), rather than by rapid drug metabolism or elimination. Repeated doses or prolonged infusions of such agents may saturate the Vd, and drug effects (which are now critically dependent on clearance rather than redistribution) may be significantly prolonged. The dependence of offset of drug effects on the duration of therapy has led to the concept of context-sensitive half time, which takes account of the cumulative effects of drugs with prolonged administration (figure 5). By this yardstick, the most desirable agents are those that have a short duration of action as a consequence of rapid excretion or metabolism (with no active metabolites), and show little or no prolongation of their duration of effect with increases in duration of administration. Even short acting agents, such as propofol and alfentanil, may show some prolongation of effect with long-term use (figure 6). Perhaps the only current agent that seems substantially immune to this phenomenon is remifentanil (figure 6; see section 5).
Schematic diagram showing the context-sensitive half-times for thiopental sodium (thiopentone) and propofol. Note that the recovery characteristics of both drugs worsen with increasing duration of administration, but that this effect is much more prominent for thiopental sodium (reproduced from Shafer,[38] with permission from Elsevier Inc.).
Schematic diagram showing the context-sensitive half-times for different opioids. Unlike the other agents, remifentanil has constant recovery characteristics irrespective of duration of administration.[39]
2.3 Pattern of Sedative Use
Many different sedatives have been used over the years in the NCCU. A survey of sedative use in the UK and Ireland in 1995 showed the frequency of use of different sedative and analgesic agents in neurointensive care units.[37] Most centres used a combination of a hypnotic and an opioid, the usual agents being propofol (65%), midazolam (80%), morphine (60%), fentanyl (46%), and alfentanil (26%). It is important to note that these figures predate the introduction of remifentanil as an ICU sedative agent, and do not include the use of anaesthetic drugs as metabolic suppressants in the context of refractory intracranial hypertension. A repeat survey by the same authors in 2001[40] showed little change from this pattern, but data collection preceded recent concerns regarding problems with high dose propofol.
None of these agents are ideal, and there are few published studies that compare sedative drugs either within or between the different pharmacological subclasses. The following discussion reviews the existing evidence for their use in head injury (see table II for a summary of the main classes of sedatives).
Summary of the main sedative agents used in the treatment of head-injured patients in the neurointensive care unit[41]
3. Benzodiazepines
Benzodiazepines (BZD) are non-specific CNS depressants that augment the action of GABA at GABAA receptors, causing increased conductance of chloride ions. Their clinical effects include anxiolysis, amnesia, and sedation, and they are also anticonvulsant. They remain the most frequently used sedatives on the NCCU, although their use appears to be on the decline in favour of propofol. Midazolam is the most commonly used BZD in the UK,[37] although diazepam has been used in the past and lorazepam is commonly used in the US.[41]
3.1 Pharmacokinetics
The principal difference between the BZDs that is important in their use on the NCCU is their differing pharmacokinetic profiles. Diazepam has a prolonged elimination half-life of 20–40 hours, due to a combination of high lipid solubility and low hepatic clearance.[45] This compares unfavourably with the elimination half-lives of lorazepam (10–20 hours)[46] and midazolam (2–2.5 hours).[47] Diazepam also has an active metabolite, desmethyldiazepam, with an elimination half-life of 93 hours, which adds to the prolonged sedation associated with the use of diazepam.[45] Lorazepam has a moderately long elimination half-life. It is metabolised in the liver to inactive metabolites, but may accumulate with repeated administration due to its long elimination half-life.[46] In a comparative study in critically ill surgery trauma patients, lorazepam was cost effective when compared with propofol or midazolam, but its use was more frequently associated with oversedation.[48]
Midazolam is also highly lipid soluble at physiological pH due to the closure of its imidazole ring, although at low pH it is water soluble. This causes a rapid onset of action. It is rapidly metabolised by the liver to a mixture of active (α-hydroxymidazolam = 63% of midazolam potency, α-hydroxymidazolam glucuronide = 9% of midazolam potency) and inactive (4-hydroxymidazolam) metabolites, accounting for its rapid offset of action.[47] This may make midazolam the more desirable BZD in terms of ease of titration,[48] with more predictable wake-up times in head-injured patients. However, accumulation of active metabolites may result in significant sedation,[49] and the pharmacokinetics of midazolam may be altered by different disease and physiological states and the use of concurrent medications. The metabolism of midazolam in critically ill patients may be impaired,[50] and multiple doses or prolonged infusions may cause drug accumulation and prolonged sedative effects after cessation of midazolam administration.[51] The elimination halflife of midazolam is increased in elderly patients, following surgery,[52,53] and in patients with severe liver disease.[50] While lorazepam has a longer halflife than midazolam (8–15 vs 3–11 hours) in healthy subjects, its clearance may be increased following neurotrauma[54] but its pharmacokinetics seem relatively unaltered by critical illness or organ failure.[54,55] Therefore, the more predictable pharmacokinetics of lorazepam represent a considerable advantage in sedating critically ill patients with multiorgan failure.[2]
3.2 Cerebral Effects
BZDs all increase the seizure threshold and may be used as anticonvulsants.[56,57] Lorazepam, in particular, has a role in the treatment of epilepsy.[57] Midazolam causes a number of electroencephalogram (EEG) changes, including a decrease in alpha activity, an increase in theta-delta activity, low-voltage beta activity and high-frequency beta activity.[58,59] Animal studies have shown that BZDs improve neurological outcome following ischaemic brain injury[60] and have a protective effect against cerebral hypoxia following convulsions.[61] There are no reports of such effects in humans.
Benzodiazepines reduce CBF and CMRO2 but there is a ceiling effect above which there is no additional effect on CMRO2 (see figure 4),[9] and burst suppression or an isoelectric EEG cannot be achieved.[62] A study of head-injured patients showed a decrease in CBF and CMRO2 during the administration of diazepam,[63] and CPP was unaffected. No associated decrease in ICP has been reported with diazepam therapy.[64] Similarly, midazolam decreased CBF and CMRO2 in animals[62,65] and healthy volunteers,[66] although a study in patients undergoing craniotomy demonstrated no change in these indices.[67] ICP was not altered in patients with severe head injury who were treated with midazolam.[68] There was a significant decrease in CPP but this was due to a concomitant reduction in MAP.
Tolerance to the sedative effects of BZD occurs after only a few hours of treatment, leading to reduced efficacy and escalating doses,[69,70] or the requirement for the use of alternative drugs. A further adverse effect that has been reported during discontinuation of longer-term BZD therapy is a withdrawal syndrome,[71] manifested by tremors, seizures, hypertension and insomnia.
3.3 Extracerebral Effects
In the cardiovascular system, BZDs reduce systemic vascular resistance.[72] The reported effect on MAP is also variable, with midazolam causing no reduction in MAP in adult intensive care and normotensive neurosurgical patients,[64,73] a slight reduction in previously hypertensive neurosurgical patients[64] and a significant reduction in severely head-injured patients.[68] This latter study is the only one in which head-injured patients were studied. Although only 12 patients were included in the study, the results suggested that midazolam boluses should be used with extreme caution in head-injured patients, especially when CPP is already critical. Several of the authors suggested that the haemodynamic effects of BZDs may become more significant in hypovolaemic patients. There is controversy as to whether BZDs preserve normal cardiovascular homeostatic reflexes.[74,75] BZDs are potent inhibitors of respiration by a central action and inhibit the cough reflex, effects that may become important when weaning patients off mechanical ventilation.
3.4 Flumazenil
This is an imidazodiazepine that is a specific benzodiazepine antagonist. Its use to reverse BZD sedation is not to be recommended in head-injured patients since it has been shown to increase ICP and decrease CPP in this situation.[76] It can also cause tachycardia, hypertension and seizures when used to reverse BZD sedation.[77]
3.5 Summary
Midazolam, by virtue of its shorter half-life and more rapid onset and offset of action, is the arguably the most appropriate BZD for use in the NCCU. It reliably reduces CMRO2 and CBF, but with no associated decrease in ICP. It has the advantage of reducing the seizure threshold, but cannot induce burst suppression. It may cause significant systemic hypotension, with a detrimental effect on the CPP. Care must still be taken to avoid accumulation in prolonged use, especially in liver disease and in elderly patients. Midazolam has an established role in the NCCU, either for maintenance of sedation, or as an adjunct to other sedatives. However, its potential to accumulate (especially in severely ill patients) and to cause hypotension, and its inability to reliably reduce ICP mean that it is not an ideal agent. Lorazepam may be a useful and inexpensive agent for patients who require prolonged sedation but do not require rapid reversal of sedation for neurological evaluation. An additional advantage is its predictable pharmacokinetic behaviour, even in the setting of multiorgan failure.
4. Propofol
Propofol is a phenol derivative that has high lipid solubility but is almost insoluble in water. It is formulated as an emulsion in a combination of soya bean oil, glycerol and egg phosphatide, and it is this, rather than the drug itself, that is responsible for some of its adverse effects, as outlined below. Since the introduction of propofol in 1986, it has gained widespread use as an induction agent and is now commonly used as a sedative agent on intensive care units, including the NCCU,[37,40] where it is given as an infusion with additional boluses as required. It is presented as a 1% or 2% solution. It has a rapid onset of action, is rapidly cleared from the plasma, and is metabolised by the liver to quinol and propofol glucuronides and 4-quinol sulphate, which are inactive. Propofol has an elimination half-life of 3–4.8 hours. After even prolonged infusions, recovery of consciousness following its cessation is reliable, reported as 15 minutes after an infusion lasting several days.[78] Despite these reports, it must be recognised that the kinetics of the drug at the effect site (where the drug exercises it pharmacodynamic effects) can substantially vary with the duration of treatment — i.e. the half-time for the clinical effects of propofol are context-sensitive (figure 5).[79] These effects have been carefully considered in the design of dosage regimens for total intravenous anaesthesia (TIVA),[80] but are rarely considered during use in critical care sedation, even with other agents.[81] There are several difficulties in extending TIVA protocols to sedation in critical care, including altered pharmacokinetics in critically ill patients, pharmacokinetic interactions with other drugs, and the effects of non-drug therapy. For example, there is concern that hypothermia[82] and catecholamines[83] (both of which are commonly used in head injury) may alter propofol metabolism. Also of some concern are reports of the development of both pharmacokinetic and pharmacodynamic tolerance[84] to propofol during prolonged use. These issues probably need more attention when propofol is administered for long periods of sedation in high doses in critically ill patients.
4.1 Cerebral Effects
Propofol reduces CBF, CMRO2 and ICP reliably in a number of studies but this is often compounded by a reduction in CPP, usually as a result of a lowering of the MAP. Ten patients with closed head injury were given an infusion of propofol (150 μg/kg/min) during an operation for orthopaedic injuries.[85] There were significant reductions in CPP, regional CBF and ICP in all patients during the propofol infusion, which returned to baseline when propofol was stopped. An infusion of propofol (mean rate 2.88 mg/kg/h) was administered to 10 patients with severe head injury in intensive care, causing a significant reduction in ICP, significant only at 2 hours, and an increased CPP, significant only at 24 hours.[86] In a larger study, 42 patients with severe head injury received either a combination of morphine and a propofol infusion (propofol 55 ± 42 μg/kg/min and morphine 1.3 ± 0.7 mg/h) or morphine alone (10 ± 6.7 mg/h).[87] The propofol group required less neuromuscular blocking agents, BZDs, barbiturates and CSF drainage (p < 0.05), and had a lower ICP, but the latter difference was only significant at 3 days post-injury. A further study in 15 severely head-injured patients who received either an infusion of propofol (mean rate 232 mg/h) or morphine (mean rate 2.3 mg/h) and midazolam (mean rate 2.8 mg/h) showed a reduction in global brain metabolism in the propofol group but no difference in MAP, ICP or CPP.[88] A bolus of propofol (2 mg/kg over 90 seconds) produced a significant reduction in ICP and CPP in six severely head-injured patients.[89]
Many authors have compared propofol with midazolam for sedation in critically ill patients.[90–92] Propofol is reported to be as safe as midazolam in terms of adverse effects, and may be associated with a shorter wake-up time[90] and a better quality of sedation[91] than midazolam.
Propofol has been used successfully to treat status epilepticus,[93–96] and one study confirmed successful treatment of status epilepticus with EEG recordings.[96] This is despite initial reports of induction-related epileptiform movements following its introduction,[97] and other reports of grand mal seizures associated with propofol therapy.[98,99] Myoclonic activity has been reported following propofol induction,[100] which may be confused with epileptic activity. Propofol is also effective in achieving burst suppression.[101] Animal studies suggest a large reduction in CBF (3858%) and CMRO2 (22–43%) at doses that produce burst supression,[102–104] but usually at the expense of a fall in MAP (see later). Propofol may have neuroprotective effects other than those attributable to cerebral metabolic suppression,[105] but this finding has not been confirmed in other studies.
4.2 Extracerebral Effects
Propofol, either by infusion or bolus is reported to cause a reduction in MAP or an increased inotrope requirement in many studies of head-injured patients,[85–87,89] and neurosurgical patients,[101,102,106,107] although one study reported no effect on MAP. At a dosage required to achieve burst suppression in neurosurgical patients (100–200 μg/kg/min), one paper demonstrated significant decreases in heart rate (19%), MAP (20%), cardiac index (23%) and left ventricular stroke work index (26%), which were attributed to venodilation and cardiac depression at this dosage.[101]
4.3 Adverse Effects Attributable to the Carrier
As mentioned earlier, the formulation of propofol may be responsible for a number of adverse effects. The lipid component can cause hypertriglyceridaemia, especially in large doses over long time periods,[108] an effect that could be reduced with the use of the 2% solution. It also has a significant calorific content, providing 1.1 kcal/mL, which should be taken into account during nutritional assessments. Anaphylactoid reactions following propofol usage have also been attributed to the carrier .[109,110]
Propofol administration has been associated with an elevation in pancreatic enzyme levels[111] and frank pancreatitis.[112,113] In one study, 40 surgical patients were randomly assigned to receive either anaesthesia with propofol (2.5 mg/kg bolus followed by maintenance of 4–10 mg/kg/h), or thiopental sodium induction (5–7 mg/kg) followed by maintenance with 0.5% isoflurane.[114] Both groups received 50% nitrous oxide in oxygen. The two groups showed no differences in plasma cholesterol, triglyceride, amylase or lipase levels postoperatively. However, this was a short-term study, and may not reflect the biochemical changes occurring after prolonged use of propofol, e.g. as in the NCCU. A further potential adverse effect of the carrier is infection[115,116] and some authors suggest that propofol infusions are changed every 6 hours. A more recent formulation of propofol that contains edetic acid (EDTA)[117] reduced the risk of infection without any significant change in sedative profile or trace element metabolism.[118,119] Initial reports that this formulation of propofol was associated with an improved outcome compared with the standard preparation[120] require confirmation in further studies.
4.4 The ‘Propofol Infusion Syndrome’
Prolonged propofol administration has been associated with a ‘propofol infusion syndrome’, which was first reported in critically ill paediatric patients[121,122] and is of uncertain aetiology. The syndrome comprises metabolic acidosis, lipaemic serum, hepatomegaly, rhabdomyolysis and cardiac failure. A review of the reported cases of propofol infusion syndrome in children published in 1995[123] found that factors associated with development of the syndrome included:
-
1.
Prolonged propofol infusion of more than 48 hours duration.
-
2.
Dosage of propofol greater than 4 mg/kg/h.
-
3.
Age: 13 of the 18 case reports reviewed involved children aged 4 years or younger.
-
4.
Respiratory tract infections: present in the majority of children who developed the syndrome.
Propofol infusion syndrome has been specifically reported in the NCCU setting in a case report of a 13-year old girl with closed head injury,[124] and in adults with head injury.[125] In the latter study, a retrospective cohort analysis of head-injured patients reported seven patients whom the authors judged to have died from the propofol infusion syndrome out of 67 patients at risk. Increased mortality was associated with high dosage, and long-term propofol infusion. The risk of developing the syndrome showed an odds ratio of 1.93 (95% CI 1.12–3.32, p = 0.018) for every mg/kg/h increase in mean propofol dose above 5 mg/kg/h. Patients exhibited refractory tachyarrhythmias, although left ventricular dysfunction was not always present. Rhabdomyolysis, hyperkalaemia and prolonged or terminal acidosis were observed, but hyperlipidaemia was not a feature. The median onset of the syndrome was 67 hours after starting high dose propofol, and the median time to death was 91 hours. While it is clearly important to avoid high dose propofol, it has been questioned whether the patients actually died of a specific cardiac effect of propofol, or this simply represented cardiac depression and changes in electrolyte homeostasis that might be observed with high doses of many anaesthetic agents,[126,127] including barbiturates.[128]
It has been suggested that head-injured patients are at particular risk of the propofol infusion syndrome because of the prolonged need for anaesthetic doses of propofol to act as a metabolic depressant, and the possible contribution to metabolic acidosis and cardiac failure of the frequent use of vasopressors.[125] The actual mechanism of propofol infusion syndrome is the cause of some debate. It is unclear whether it is the drug itself, its metabolites, the lipid emulsion, or a combination of these factors that is responsible. Recent evidence has implicated abnormalities in acylcarnitine handling.[129] It is notable that major cardiovascular instability has also been reported with burst-suppression doses of thiopental sodium and has been attributed to its effects on Na+/K+ channels.[128]
In addition to these extracerebral effects on the cardiovascular system, which might be expected in a potent intravenous anaesthetic, propofol has also been reported to have other properties that may be of therapeutic relevance.[130] Perhaps the most prominent of these is a significant antioxidant capacity, which may protect against oxidant-mediated haemolysis, provide cytoprotection in hepatic ischaemia reperfusion injury, and contribute to the neuroprotective effects of the agent.
4.5 Summary
Propofol, unlike the other sedatives discussed (with the exception of remifentanil), is unique in its rapid clearance and reliable offset of action, even after long-term infusions. Other advantages include a reliable reduction in CMRO2, CBF and ICP, factors that have increased its use in head-injured patients. It is useful both as a continuous infusion to provide sedation, and also as rescue treatment during episodes of increased ICP. Disadvantages include the reduction in MAP during infusion and bolus therapy, and the many adverse effects associated with the emulsion in which propofol is formulated. In the absence of alternatives, propofol will, however, remain a well-used drug in the treatment of head-injured patients.
5. Opioids
Opioids are an intrinsic part of the sedative regimen for most head-injured patients. Not only do they provide analgesia and improved tolerance of mechanical ventilation and other therapeutic interventions, but they add to the sedation provided by other sedative agents, and are thus included in this review. In the UK, the most frequently used opioids are morphine (60% of NCCUs using this routinely), fentanyl (46%), alfentanil (26%) and codeine (20%).[37] Sufentanil has also been widely reported in the literature. Remifentanil is a new opioid currently undergoing clinical trials. Its particular attraction for use in the NCCU is that it has an ester linkage that is rapidly hydrolysed by plasma esterases to in inactive metabolite, and therefore has a rapid and reliable offset of action and does not accumulate.[131]
Four subclasses of opioid receptors have been identified: μ, κ, δ and σ.[132] They are found widely in the CNS and peripherally. μ Receptors are further sub-classified into μ1 and μ2 receptors.[133] Table III summarises the effects of stimulation of the different opioid receptors and the differential actions of opioid agonists at these receptors.
As with the BZDs, the main differences between the opioids lie in their pharmacokinetics (figure 6). Morphine has a low lipid solubility and slow CNS penetration, so its onset of action is relatively slow. It has a half-life of 2–3 hours,[134] but this is increased in renal failure as about 10% of the parent drug is excreted unchanged in the urine.[135] In addition, morphine is metabolised in the liver to morphine-3-glucuronide and morphine-6-glucuronide, the latter of which has a potency several times that of morphine, and accumulates in renal failure.[42] By contrast, fentanyl, alfentanil and sufentanil are highly lipid soluble, so have a fast onset of action. Alfentanil, by virtue of its shorter half-life, is less likely to accumulate than fentanyl when given by infusion. They are metabolised by the liver to inactive metabolites,[43] so renal impairment does not prolong their action but metabolism is delayed in various disease states. Cardiac failure reduces the clearance of fentanyl.[44] Critical illness[136] and cirrhosis,[137] respectively, reduce the clearance and increase the half-life of alfentanil.
The recent introduction of remifentanil into ICU practice represents a substantial advance in the management of sedation in patients with head injury. Remifentanil is broken down by nonspecific plasma and tissue esterases.[131] Its rapid onset and offset, ease of titration, and stable pharmacokinetics could potentially make it an ideal agent in this group of patients. In particular, it has a constant context-sensitive plasma half-life, and its duration of offset is largely uninfluenced by the duration of therapy or dosage used.[138] While formal evaluation of its use in ICU sedation for head injury is limited, its effect on CNS and cerebrovascular physiology have been well studied in neuroanaesthesia.[139–143] The pharmacodynamics of remifentanil seem similar to those of other opioid agents, with expected cerebrovascular effects. Warner et al. showed that remifentanil and alfentanil had similar effects on systemic haemodynamics, but no effect on ICP in patients undergoing craniotomy.[140] Remifentanil and fentanyl have similar effects on baseline cerebral blood flow and CBF carbon dioxide reactivity,[144] and magnetic resonance techniques suggest that the agent has no adverse effects on measures of cerebral compliance in healthy volunteers.[145]
The real benefit of this agent would be expected to relate to its pharmacodynamics, and the agent has been widely evaluated in general intensive care settings.[146–151] Early publications suggest that remifentanil is likely to a useful agent in neurotrauma,[152] and a preliminary report suggested that its pharmacokinetic properties may be beneficial in this setting.[153] Karabinis et al.[153] studied the time taken to allow neurological evaluation after down-titration of sedative agent in patients with neurotrauma receiving remifentanil, fentanyl and morphine, and found that remifentanil showed a substantially less increase in offset time with prolonged therapy compared with the other two agents. This limited experience in neurotrauma is consistent with experience in other critically ill patient populations. In particular, remifentanil showed little accumulation even in patients with severe renal failure, and levels of its main metabolite, remifentanil acid, did not reach levels that were clinically significant.[154] While reductions in body temperature reduced remifentanil clearance by 3% per 1°C,[155] these effects are unlikely to be clinically significant in neurotrauma patients who are treated with moderate hypothermia.
5.1 Cerebral Effects
Opioids have the advantage of having minimal effect on CBF and CMRO2.[156,157] However, their effects on ICP and CPP seem to be less favourable. Many authors have reported an increase in ICP during opioid therapy in head-injured patients.[158–162] Thirty patients with severe head injury who were given a bolus of morphine (0.2 mg/kg) or fentanyl (2 μg/kg) had an increase in ICP, decrease in MAP and consequent reduction in CPP.[158] CBF in these patients was reported as unchanged and carbon dioxide reactivity as preserved, but autoregulation in response to a hypertensive challenge was impaired or abolished in 56.7% of patients. Similar changes in ICP and MAP were reported following boluses of sufentanil or fentanyl in another study of patients with severe head injury.[162] A further study reported the effects of boluses and subsequent infusions of sufentanil, fentanyl and alfentanil in 10 head trauma patients.[159] Administration of all drugs was associated with a significant increase in the ICP, although the effect was transient, peaking at between 3 and 5 minutes, and returned to baseline at 15 minutes. These rises in ICP are associated with reductions in MAP and CPP in all cases and are thought to be mediated by autoregulatory vasodilatation and increases in CBV. Indeed, even a large bolus dose of sufentanil (3 mg/kg) had no effects on ICP if MAP was maintained using vasopressors, although ICP elevations were observed if MAP was not maintained.[160]
There have been a number of case reports of epileptiform activity following opioid therapy during anaesthesia,[163–165] but it is unclear whether this reflects true seizure activity. In high doses, all opioids can cause seizures, but an EEG recording during one episode of epileptiform activity in humans showed no seizure activity.[166]
5.2 Extracerebral Effects
Opioids produce hypotension by reducing sympathetic tone and increasing parasympathetic tone,[167] but they have no effect on cardiac contractility.[168] All opioids can cause a vagally-mediated bradycardia,[169] although this is less common with infusions than rapid injections.
A further mechanism for opioid-associated hypotension is histamine release. There are many reports of histamine release following opioid therapy,[170–173] with associated haemodynamic changes, including hypotension and tachycardia. The mechanism appears to be a direct action of the opioids on histamine-containing cells rather than an allergic-type response, and the action appears to be restricted to morphine-like drugs; synthetic opioids such as fentanyl and sufentanil are free of this adverse effect.[170] The hypotension produced is of particular importance in head-injured patients, where maintenance of CPP is of paramount importance in preventing secondary neuronal injury.
Opioids cause profound respiratory depression and suppression of the cough reflex. These may be helpful in ventilated patients, but are a disadvantage in the weaning phase of NCCU care. As discussed previously, the effects of morphine may be prolonged, especially in renal impairment, but fentanyl is also associated with a delayed ‘rebound’ effect that can be delayed for up to 4 hours after stopping an infusion. This is thought to be due to enterohepatic circulation or mobilisation of sequestered stores. Opioids can also cause muscle rigidity,[174] an effect that can affect the respiratory muscles and interfere with ventilation.
Gastrointestinal effects of opioids include nausea and vomiting, although this is not an important problem in unconscious patients. However, reduced gastrointestinal motility is a concern in sedated and awake subjects, and leads to delayed gastric emptying,[175,176] intolerance of nasogastric feeding, and constipation. These effects of opioid drugs add to the altered gastrointestinal motility that occurs as a direct consequence of head injury (see section 1.2).
Less well documented potential adverse effects of opioids include suppression of the immune response,[130] a factor that may contribute to hospital-acquired infections in the NCCU. Initial fears that high-dose opioids may be directly neurotoxic have not been justified.[177,178]
5.3 Summary
Despite many potential disadvantages for the use of opioids in the NCCU, these agents remain in widespread use. In practice, the potential adverse effects of these agents can be minimised with care, and they are extremely useful because of their ability to complement sedation, improve tolerance of mechanical ventilation and to provide effective analgesia. Opioids are frequently used in combination with hypnotic agents such as benzodiazepines and propofol, and can reduce sedation requirements with improved haemodynamic consequences. Boluses of opioids have been reliably shown to cause hypotension and rises in ICP, so care should be taken when administering opioids in this way to patients with a critical CPP.
There is little to choose between the frequently used opioids in terms of detrimental effects (increases in ICP and decreases in MAP and CPP with bolus administration), but the shorter acting drugs have advantages in terms of a shorter duration of action and a reduced tendency to accumulate. The availability of remifentanil as an ICU agent (now approved in the US and the UK) provides a sedative agent with unique pharmacokinetic characteristics that enable easy titration and rapid emergence. Clinical experience with remifentanil in this setting is still relatively limited, but it appears likely that this agent will play a major role in sedation in head injury. While longer acting opioids can be effectively antagonised by naloxone, a specific μ-receptor antagonist, this does not provide a risk-free alternative. Naloxone reversal does have the potential to allow rapid neurological assessment during opioid therapy, although rapid reversal of opioid narcosis can be associated with adverse effects, such as hypertension and myocardial ischaemia, and rises in ICP. While these adverse effects would also be observed with the rapid offset of opioid effects with remifentanil cessation, the presence of naloxone could make re-sedation more difficult and limit ability to titrate.
6. Barbiturates
Barbiturates, particularly pentobarbital (pentobarbitone), have been extensively studied in head injury. In the UK, thiopental sodium is the most commonly administered barbiturate, used in 56% of NCCUs.[179] Barbiturates exert their effects by stimulating GABA receptors[180] and inhibiting excitatory α-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid (AMPA) receptors in the CNS to produce dose-dependent sedation and general anaesthesia. Barbiturates are very lipid soluble, allowing rapid diffusion into the CNS and rapid onset of action. Thiopental sodium is predominantly metabolised in the liver, although a small amount is excreted unchanged by the kidneys. It has a long elimination half-life of 11.6 hours in surgical patients and is metabolised by zero-order kinetics at the higher plasma levels that result from prolonged infusions and high dosages.[181] These figures are broadly in agreement with data obtained from longer infusion periods in critically ill adults and children with neurotrauma.[182–185] This causes an accumulation of thiopental sodium, especially after repeated doses or prolonged infusions, which are often employed to achieve burst suppression in refractory intracranial hypertension. Drug level measurement suggests that the elimination of thiopentone shifts from first- to zero-order kinetics when plasma concentrations exceed 30 mg/L, and plasma levels >40 mg/L are required to produce burst suppression.[185] It is therefore important to identify the dosage of thiopental sodium that provides the maximal degree of cerebral metabolic suppression, since a higher dosage results in no additional CNS effects and produces increasing and dangerous cardiovascular depression with a greater prolongation of emergence times. This is particularly detrimental in the NCCU, where rapid offset of action is desirable to assess neurological status.
Ideally, barbiturate dosage requirements are defined using EEG monitoring, in order to achieve a burst-suppressed EEG, in which periods of isoelectricity (suppression) are interspersed with bursts of electrical activity, with the former typically representing greater than 50% of the trace. However some guidance is also available from the literature. Following a loading dose (typically 40 mg/kg),[186] infusion rates of 4–8 mg/kg/h are usually required to maintain burst-suppression patterns on EEG. More recent data[185] suggest that the lower end of this dose range may be more appropriate in most patients who require long-term thiopentone in the ICU setting. Measurement of plasma drug levels may provide useful guidance during the recovery periods following thiopental coma,[187] with recovery of pupillary function at plasma levels of 50 mg/L and motor responsiveness at 12 mg/L.
Pentobarbital also has a long half-life, measured as 15.6 ± 3.9 hours in head-injured patients.[188] Methohexital (methohexitone) is unusual in having a shorter half-life of 4 hours, and has been shown to have a more rapid elimination than thiopental sodium after prolonged infusion.[189] However, methohexital has not been widely studied in head injury, so further discussion of the barbiturates will include only pentobarbital and thiopental sodium.
6.1 Cerebral Effects
Barbiturates have long been known to reduce ICP and CBF[190] and have been shown to reduce ICP that is refractory to other medical and surgical interventions.[191] This may be due to a combination of suppression of brain metabolism[192] and altered cerebral vascular tone.[193] EEG effects include an increase in fast beta activity at low concentrations and burst suppression at higher doses.
Evidence for the use of barbiturates in head injury falls into two categories that will be discussed next.
6.1.1 Treatment of Elevated Intracranial Pressure (ICP)
Several studies have linked the administration of barbiturates with outcome. The administration of barbiturates in severe head injury was associated with improved ICP control and an improved outcome in one study.[194] These results were echoed by a second study in 60 patients.[195] There was improved control of elevated ICP in the group receiving pentobarbital in a further study of 73 severely head-injured patients.[196] However, this translated into a survival advantage only in a subgroup of patients who had no preceding cardiac complications. Despite this, a recent meta-analysis[197] of the use of barbiturates in head injury found no evidence that barbiturate therapy in head injury improves outcome. However, the conclusions of this meta-analysis are in conflict with expert recommendations provided in internationally accepted guidelines.[1]
A study investigating a link between cerebral vasoreactivity and ICP showed that in patients in whom there was an intact CBF response to hyperventilation, barbiturate therapy was associated with a decrease in CBF, CMRO2 and ICP.[198] These responses were absent in patients in whom cerebral vascular reactivity to hyperventilation was reduced or abolished. In another study of head-injured patients, pentobarbital was compared with mannitol for initial treatment of raised ICP, with no difference in outcome.[199] Pentobarbital appeared to fare worse, with a significant reduction in the CPP, and, in a subgroup of patients with diffuse cerebral injury, those treated with pentobarbital had a mortality of 77% compared with that in the mannitol group of 41%.
6.1.2 Prophylaxis Against Raised ICP and Ischaemic Neuroprotection
In a study of 53 head-injured patients, subjects were randomised to receive conventional treatment plus or minus prophylactic pentobarbital.[200] Pentobarbital was started as soon as possible after head injury, at a dose sufficient to cause burst suppression. There were no differences between the groups in terms of outcome, the incidence of elevated ICP, the duration of ICP elevation or the response of the ICP elevations to treatment, and the authors concluded that they could not recommend the administration of barbiturates in prophylaxis of raised ICP in head injury. Similarly, while there is substantial evidence of barbiturate neuroprotection in experimental focal ischaemia, these results have not translated into general clinical benefit,[201] despite isolated positive studies.[186]
6.2 Extracerebral Effects
Barbiturates are widely known to reduce MAP by a combination of myocardial and central vasomotor depression.[202,203] Studies of barbiturate use in head injury confirm this phenomenon.[196,197,199] They depress respiration and decrease smooth muscle tone, an effect that reduces tolerance of nasogastric feeding.[204] There is loss of thermoregulation in experimental models,[202] which is confirmed in some clinical studies.[197] Barbiturates also inhibit leucocyte phagocytosis and respiratory burst,[205s] causing increased susceptibility to infection. High doses of barbiturates may suppress the bone marrow and reduce neutrophil production in sepsis.[206]
In addition to these well documented adverse effects, there is emerging concern regarding the occurrence of refractory cardiac dysrhythmias and cardiac failure with high dose barbiturates, particularly during emergence from coma.[128] This has often been associated with severe hyperkalaemia, and while attempts have been made to relate this to the documented effects of barbiturates at K+ channels,[207] the mechanism of cardiovascular dysfunction in this setting remains unclear.
6.3 Summary
Barbiturates produce reliable reductions in CBF, control of ICP and suppression of epileptic foci. This is at some cost, however. In particular, the reduction in MAP may produce significant reductions in CPP, a factor that may worsen the outcome of head-injured patients. In addition, the undesirable pharmacokinetics means that the prolonged elimination and accumulation of barbiturates, especially after repeated doses, may delay neurological assessment. There are also emerging concerns regarding the development of poorly explained cardiovascular failure in association with high dose barbiturate use. No causal association has been demonstrated, but caution is advisable. While barbiturates remain a valuable tool in the treatment of refractory intracranial hypertension and status epilepticus, they must be used with caution.
7. Ketamine
Ketamine is a phencyclidine derivative that acts as a non-competitive antagonist at the NMDA receptor, which is a subtype of EAA receptor within the CNS. It has a short elimination half-life of 2.6 hours, but some of its metabolites may have anaesthetic effects, particularly norketamine,[208] leading to potential accumulation with repeated doses. Ketamine has a number of advantages that would make it a useful drug in the NCCU. Its cardiovascular profile makes it useful when cardiovascular depression is best avoided. It is well known to cause an increase in systemic blood pressure and heart rate,[209–211] and is therefore useful in hypovolaemic or hypotensive patients.
The antagonism of NMDA receptors by ketamine may have a specific protective role in the treatment of head-injured patients. It antagonises excitatory amino acids at the NMDA receptor and may reduce the consequent calcium ion mobilisation and neuronal damage that occurs in head injury.[212] Ketamine has been shown to be neuroprotective in studies of ischaemic and traumatic head injury in rats.[212–215] In addition, cerebrovascular responsiveness to arterial partial pressure of carbon dioxide (PaCO2) is preserved[216] and burst suppression can be achieved.[217]
Despite the potential benefits of ketamine in head-injured patients, it has not gained widespread use because of reported detrimental effects on CBF, CMRO2 and ICP. Studies have repeatedly reported increases in CMRO2, increases in CBF by 50–80% and consequent increase in ICP,[216,218–220] with recommendations not to use it in the NCCU. Some studies have been published, however, describing the use of ketamine in head injury. In one report, patients with severe head injury were given either ketamine and midazolam or fentanyl and midazolam.[209] The ketamine group had a lower requirement for catecholamines, a CPP that was on average 8mm Hg higher and an ICP that was 2mm Hg higher than the fentanyl group, and no difference in overall outcome. The authors suggested it is an appropriate therapy in head-injured patients. In another study, three different doses of ketamine, in addition to a propofol infusion, were administered to deepen sedation in eight artificially ventilated head-injured patients.[217] All three doses of ketamine were associated with a statistically significant decrease in ICP and no change in CPP, jugular bulb venous oxygen saturation and middle cerebral artery blood flow velocity. The authors concluded that ketamine may not cause adverse cerebral haemodynamics in head-injured patients sedated with propofol, and recommended larger studies.
A further disadvantage of ketamine therapy is its reduction of the seizure threshold, demonstrated by EEG changes,[221] an increase in epileptiform movements in epileptic patients[222] and an increased frequency of seizures in epileptic patients for months after receiving a ketamine anaesthetic.[223] Despite these reports, ketamine has been successfully used for control of status epilepticus.[224]
7.1 Summary
Ketamine is unusual among potential sedative agents in its maintenance of systemic blood pressure. However, it is not recommended for use in head injury because of the reported increase in CMRO2, CBF and ICP during its administration, and the possible lowering of the seizure threshold.
8. Etomidate
Etomidate is a carboxylated imidazole derivative, most commonly used as an intravenous induction agent in cardiovascular instability. It has a number of features that would make it useful on the NCCU. It is rapidly cleared, with an elimination half-life of 2.6 hours.[225] It reduces both CBF and ICP,[226–229] can achieve burst suppression,[230] causes minimal cardiovascular depression[231,232] and is non-cumulative.[233] Several studies have reported the efficacy of etomidate in head-injured patients.[229,234–236] Etomidate is reliably shown to reduce ICP and preserve CPP, with variable effects on MAP. Generally, MAP is preserved or only slightly reduced, however one group reported that boluses of etomidate were associated with ‘occasionally serious’ episodes of hypotension that may be associated with hypovolaemia.[193] Consequent reductions in CPP were usually small at less than 10mm Hg.
Despite the many advantages of etomidate, its use in the NCCU is limited by associated adrenal suppression. Etomidate is a reversible inhibitor of the enzyme 11-β-hydroxylase, which converts 11-deoxycortisol to cortisol.[237,238] The enzyme is also involved in the synthesis of aldosterone, causing decreased mineralocorticoid effect.[239] While a single dose of etomidate can reduce the synthesis of cortisol and aldosterone for up to 24 hours,[240] the clinical significance is unclear. Prolonged infusions of etomidate have been shown to cause a significant increase in mortality in the general ICU.[241] Although coincident use of corticosteroids may enable the safe use of etomidate, these problems have limited its use in the intensive care setting. An additional concern relates to the development of renal failure and other adverse effects when an etomidate preparation formulated in propylene glycol is used for long-term infusions.[242–246] This preparation is no longer marketed in the UK, but is available in other countries, including the US (Bedford Laboratories, Bedford, Ohio, USA).
8.1 Summary
Etomidate causes less cardiovascular instability than the other sedatives, except ketamine, and produces a reduction in CBF and ICP. It is not often used as a long-term sedative in many intensive care units because it causes adrenal suppression and an associated increase in mortality, although this is managed in some units with associated corticosteroid therapy. Formulations in propylene glycol may have adverse effects attributable to the solvent.
9. α2-Adrenoceptor Agonists
These include clonidine and dexmedetomidine. They cause sedation, anxiolysis and amnesia by their action at central α2-adrenoceptors and also have the advantages of a lack of respiratory depression and a significant anaesthetic sparing effect.[247]
Dexmedetomidine is the newer agent, and has greater specificity for the α2-adrenoceptor than clonidine.[248] It has an elimination half-life of 2 hours[249] and is metabolised in the liver to methyl and glucuronide metabolites. Its clearance is reduced in liver failure, and it inhibits the CYP2D6 component of the enzyme cytochrome P450 (CYP).[250]
α2-Adrenoceptors are found throughout the CNS,[251] and their direct stimulation by dexmedetomidine may be responsible for the reduction in CBF without a reduction in cerebral metabolism that has been demonstrated in animals.[252,253] Despite the altered CBF/CMRO2 ratio, there is no evidence that global cerebral ischaemia occurs. Other animal work suggests that α2-agonists have a neuroprotective effect. They have been shown to improve neurological outcome following cerebral ischaemia.[254] The only study of dexmedetomidine in neurosurgical patients showed that lumbar CSF pressure did not alter in patients undergoing transsphenoidal pituitary surgery who received dexmedetomidine,[255] but MAP, heart rate and CPP were all reduced. The cardiovascular effects result from a reduced central sympathetic output.[256] Clearly, further studies are required to investigate the usefulness of dexmedetomidine in head injury.
Clonidine has been investigated in head-injured patients for its role in reducing catecholamine release and causing cerebral vasoconstriction, rather than as a sedative. In a study of seven patients 3–5 days after severe head injury, clonidine administration caused a significant reduction in plasma noradrenaline (norepinephrine) and adrenaline (epinephrine) concentrations with no change in global cerebral perfusion.[257] This was thought to be due to α2-adrenoceptor blockade in the medulla. A further study demonstrated no effect on ICP, CBF or cerebral metabolism of a bolus of clonidine in headinjured patients.[258] In recent years, clonidine has been used in the ‘Lund’ protocol. This is a method of treating head injury that avoids the use of therapies to raise MAP, a manoeuvre that theoretically increases cerebral oedema by increasing the hydrostatic forces across cerebral blood vessels.[259,260] The cerebral haemodynamic tolerance to clonidine in severe head injury was investigated in one study, showing a reduction in MAP and CPP with little associated change in ICP in most patients, while in three patients there was a significant but transient increase in ICP sufficient to cause a profound fall in jugular bulb venous oxygen saturation.[261]
10. Antipsychotics
Antipsychotics act as dopamine antagonists within the CNS. Their actions are sedative, antipsychotic and antiemetic. They tend to be used to sedate agitated patients, for instance to reduce the effects of drug withdrawal syndromes during weaning from mechanical ventilation, or to allow radiological imaging. Drugs in this class include butyrophenones, phenothiazines and thioxanthenes. They have the advantage of rendering the patient calm without major respiratory depression.
10.1 Butyrophenones
The butyrophenones include haloperidol and droperidol. Haloperidol acts within 30–60 minutes of an intravenous dose and its effects last 4–8 hours.[262] It has an elimination half-life of 21 hours. Droperidol has a more delayed onset of action, attributed to its higher molecular weight and extensive protein binding, which inhibit its passage into the CNS. It also has a longer duration of action of 2–24 hours, which may be due to avid receptor binding.[263] Both drugs are metabolised by the liver.
Butyrophenones can cause hypotension because of α-adrenergic blockade.[264] In the CNS, droperidol was found to produce a slight fall in ICP in patients with head injury in whom ICP was raised.[265] This may be due to the decrease in CBF as a result of cerebral vasoconstriction, which was discovered in dogs.[266] Haloperidol use was not associated with an improved outcome following head injury in humans, and was associated with a longer period of amnesia.[267] Other adverse effects include extrapyramidal effects,[268,269] neuroleptic malignant syndrome[270] and, in high doses, prolonged QT interval and torsade de pointes.[271]
10.2 Phenothiazines
Phenothiazines are not only dopamine antagonists but also have antiadrenergic and anticholinergic effects. Chlorpromazine, promazine and thioridazine are the most frequently used agents in this category. Because of their antipsychotic action in addition to sedation, they are most widely used to treat confusional states in which agitation is a major feature.[272] As with the butyrophenones, phenothiazine therapy can cause hypotension, extrapyramidal adverse effects and the neuroleptic malignant syndrome. While these agents may have a role in confusional states, there are no data to support the use of antipsychotics for routine sedation in head-injured patients.
10.3 Phenothiazines
Phenothiazines are not only dopamine antagonists they also have anti-adrenergic and anticholinergic effects. Chlorpromazine, promazine and thioridazine are the most commonly used drugs in this class. Due to their antipsychotic action in addition to sedation, they are most widely used to treat confusional states where agitation is a major feature.[272] As with the butyrophenones, phenothiazines therapy can cause hypotension, extrapyramidal adverse effects and the neuroleptic malignant syndrome. While these agents may have a role in confusional states, there are no data to support the use of antipsychotics for routine sedation in head-injured patients.
10.4 Atypical Antipsychotics
Recent publications report early experience with the, use of risperidone for post-traumatic confusional states.[273,274] While this agent appears to be effective, its eventual role in this setting remains to be defined.
10.5 Summary
The antipsychotics are commonly used to control agitation in head injured patients, but there is little data to choose between individual agents. A recent supplement addresses this issue in the setting of agitation in the ICU,[275] but provides limited guidance for their administration to neurotrauma patients, in whom such drugs can unavoidably confound neurological assessment. The avoidance of respiratory depression and cardiovascular stability are particular concerns.
11. Conclusion
There is no ideal sedative for use in head injury and there are few studies that directly compare the effectiveness and adverse effects of different agents in this group of patients. Among the existing drugs, propofol appears to have most of the properties required but, as with all commonly used agents, this is at the expense of systemic blood pressure. It also has a number of potential problems associated with its formulation. The other frequently used agents, such as opioids and benzodiazepines, also have features to recommend them. In the absence of new, improved drugs, sedation of head-injured patients is likely to continue to involve a number of agents. The introduction of remifentanil is promising, with its unique metabolic pathway allowing intense narcosis with a rapid and reliable offset of action, and the potential neuroprotective action of dexmedetomidine is worthy of further study.
References
Brain Trauma Foundation. Management and prognosis of severe traumatic brain injury [online]. Available from URL: http://www.braintrauma.org [Accessed 2003 Dec 17]
Jacobi J, Fraser GL, Coursin DB, et al.ai] Clinical practice guidelines for the sustained use of sedatives and analgesics in the critically ill adult. Crit Care Med 2002; 30: 119–42
Menon DK. Cerebral protection in severe brain injury: physiological determinants of outcome and their optimisation. Br Med Bull 1999; 55: 226–58
Mayer ML, Miller RJ. Excitatory amino acid receptors, second messengers, and regulation of intracellular Ca2+ in mammalian neurones. Trends Pharmacol Sci 1990; 11: 254–60
Smith WL, Borgeat P, Fitzpatrick FA. The ecosaoids: cyclooxygenase, lipoxygenase, and epoxygenase pathways. In: Vance DE, Vance J, editors. Biochemistry of lipids, lipoproteins and membranes: new comprehensive biochemistry. Amsterdam: Elsevier Science Publishers, 1991: 297–325
McCord JM. Oxygen-derived free radicals in post-ischemic tissue injury. N Engl J Med 1985; 312: 159–63
Martin NA, Patwardhan RV, Alexander MJ, et al. Characterization of cerebral hemodynamic phases following severe head trauma: hypoperfusion, hyperaemia and vasospasm. J Neurosurg 1997; 87: 9–19
Bullock R. Injury and cell function. In: Reilly P, Bullock R, editors. Head injury: pathophysiology and management of severe closed injury. Ch. 7. London; Chapman & Hall Medical, 1997: 120–44
Menon DK. Cerebral circulation. In: Priebe HJ, Skarvan K, editors. Fundamentals of anaesthesia and acute medicine. 2nd ed. London; BMJ Publications, 2000
Miller JD, Becker DP, Ward JD, et al. Significance of intracranial hypertension in severe head injury. J Neurosurg 1977; 47: 503–16
Bowers SA, Marshall LF. Outcome in 200 consecutive cases of severe head injury in San Diego County: a prospective analysis. Neurosurgery 1980; 6: 237–42
Levati A, Farina ML, Vecchi G, et al. Prognosis of severe head injuries. J Neurosurg 1982; 57: 779–83
Chan K, Dearden NM, Miller JD, et al. Multimodality monitoring as a guide to treatment of intracranial hypertension after severe brain injury. Neurosurgery 1993; 32: 547–53
Andrews PJD. What is the optimal perfusion pressure after brain injury — a review of the evidence with an emphasis on arterial pressure. Acta Anaesthesiol Scand 1995; 39Suppl. 105: 112–4
Chan KH, Miller JD, Dearden NM, et al. The effect of changes in cerebral perfusion upon middle cerebral artery blood flow velocity and jugular bulb venous oxygen saturation after severe brain injury. J Neurosurg 1991; 77: 55–61
Robertson CS, Valadka AB, Hannay HJ, et al. Prevention of secondary insults after severe head injury. Crit Care Med 1999; 27: 2086–95
Bouma GJ, Muizelaar JP, Choi SC, et al. Cerebral circulation and metabolism after severe traumatic brain injury: the elusive role of ischemia. J Neurosurg 1991; 75: 685–93
Bouma GJ, Muizelaar JP. Cerebral blood flow, cerebral blood volume, and cerebrovascular reactivity after severe head injury. J Neurosurg 1992; 09: S333–48
Marion DW, Darby J, Yonas H. Acute regional cerebral blood flow changes caused by severe head injuries. J Neurosurg 1991; 74: 407–14
Coles JP, Minhas PS, Fryer TD, et al. Effect of hyperventilation on cerebral blood flow in traumatic head injury: clinical relevance and monitoring correlates. Crit Care Med 2002; 30: 1950–9
Piek J, Chestnut RM, Marshall LF, et al. Extracranial complications of severe head injury. J Neurosurg 1992; 77: 901–7
Schulte am Esch J, Murday H, Pfeifer G. Haemodynamic changes in patients with severe head injury. Acta Neurochir (Wien) 1980; 54: 243–50
Brown RS, Mohr PA, Carey JS, et al. Cardiovascular changes after cranial cerebral injury and increased intracranial pressure. Surg Gynecol Obstet 1967; 125: 1205–11
Cruickshank JM, Neil-Dwyer G, Hayes H, et al. Reduction of stress/catecholamine-induced cardiac necrosis by beta-selective blockade. Lancet 1987; II: 585–9
Evans DE, Alter III WA, Shatsky SA, et al. Cardiac arrhythmias resulting from experimental head injury. J Neurosurg 1976; 45: 609–16
Clifton GL, Robertson CS, Kyper K, et al. Cardiovascular response to severe head injury. J Neurosurg 1983; 59: 447–54
King ML, Lichtman SW, Seliger G, et al. Heart-rate variability in chronic traumatic brain injury. Brain Inj 1997; 11: 445–53
Goldstein B, Toweill D, Lai S, et al. Uncoupling of the autonomic and cardiovascular systems in acute brain injury. Am J Physiol 1998; 275: R1287–92
Simmons RL, Martin Jr AM, Heistercamp III CA, et al. Respiratory insufficiency in combat casualties: pulmonary oedema following head injury. Ann Surg 1969; 170: 39–44
Graf CJ, Rossi NP. Pulmonary oedema and the CNS: a clinico-pathological study. Surg Neurol 1975; 3: 319–25
Van der Zee H, Malik AB, Lee BC, et al. Lung fluid and protein exchange during intracranial hypertension and the role of sympathetic mechanisms. J Appl Physiol 1980; 48: 273–80
Singbartl G. Permeability pulmonary oedema following isolated head and brain injury. Anaesthetist 1983; 32: 417–26
Ott L, Young B, Phillips R, et al. Altered gastric emptying in the head-injured patient: relationship to feed intolerance. J Neurosurg 1991; 74: 738–42
McArthur CJ, Gin T, McLaren IM, et al. Gastric emptying following brain injury: effects of choice of sedation and intracranial pressure. Intensive Care Med 1995; 21: 573–6
Norton JA, Ott LG, McLain C, et al. Intolerance to enteral feeding in the head-injured patient. J Neurosurg 1988; 68: 62–6
Garrick T, Mulvihill S, Buack S, et al. Intracerebroventricular pressure inhibits gastric antral and duodenal contractility but not acid secretion in conscious rabbits. Gastroenterology 1988; 95: 26–31
Matta B, Menon D. Severe head injury in the United Kingdom and Ireland: a survey of practice and implications for management. Crit Care Med 1996; 24: 1743–8
Shafer SL. Advances in propofol pharmacokinetics and pharmacodynamics. J Clin Anesth 5; 6Suppl 1: 15S
Westmoreland CL, Hoke JF, Sebel PS, et al. Pharmacokinetics of remifentanil (GI87084B) and its major metabolite (GI90291) in patients undergoing elective inpatient surgery. Anesthesiology 1993; 79(5): 893–903
Wilkins IA, Menon DK, Matta BF. Management of comatose patients: are we getting any better? Anaesthesia 2001; 56: 350–69
Rhoney DH, Parker D. Use of sedative and analgesic agents in neurotrauma patients: effects on cerebral physiology. Neurol Res 2001; 23: 237–59
Osborne RJ, Joel JP, Slevin ML. Morphine intoxication in renal failure: the role of morphine-6-glucuronide. BMJ 1986; 292: 1548–9
Scholz J, Steinfath M, Schulz M. Clinical pharmacokinetics of alfentanil, fentanyl and sufentanil: an update. Clin Pharmocokinet 1996; 31: 275–92
Norgaard M, Pineda EA, McGlinch BP, et al. Pharmacokinetics of fentanyl in congestive heart failure. Anesthesiology 1991; 75: A325
Greenblatt DJ, Hamatz JS, Friedman H, et al. A large-sample study of diazepam pharmacokinetics. Ther Drug Monit 1989; 11: 652–7
Greenblatt DJ, Ehrenberg BL, Gunderman J, et al. Kinetic and dynamic study of IV lorazepam: comparison with IV diazepam. J Pharmacol Exp Ther 1989; 250: 134–40
Allonen H, Ziegler G, Klotz U. Midazolam kinetics. Clin Pharmacol Ther 1981; 30: 653–61
McCollam JS, O’Neil MG, Norcross ED, et al. Continuous infusions of lorazepam, midazolam, and propofol for sedation of the critically ill surgery trauma patient: a prospective, randomised comparison. Crit Care Med 1999 Nov; 27: 2584–8
Bauer TM, Titz R, Haberthur C, et al. Prolonged sedation due to accumulation of conjugated metabolites of midazolam. Lancet 1995; 346: 145–7
Shelly MP, Mendel L, Park JR. Failure of critically ill patients to metabolise midazolam. Anaesthesia 1987; 42: 619–26
Byatt CM, Lewis LD, Dawling S, et al. Accumulation of midazolam after repeated dosage in patients receiving mechanical ventilation in an intensive care unit. BMJ 1984; 289: 799–800
Harper KW, Collier PS, Dundee JW, et al. Age and nature of operation influence the pharmacokinetics of midazolam. Br J Anaesth 1985; 57: 866–71
Maitre PO, Funk B, Crevoisier C, et al. Pharmacokinetics of midazolam in patients recovering from cardiac surgery. Eur J Clin Pharmacol 1989; 37: 161–6
Boucher BA, Kuhl DA, Fabian TC, et al. Effect of neurotrauma on hepatic drug clearance. Clin Pharmacol Ther 1991; 50: 487–97
Wagner BK, O’Hara DA. Pharmacokinetics and pharmacodynamics of sedatives and analgesics in the treatment of agitated critically ill patients. Clin Pharmacokinet 1997; 33: 426–53
Kumar A, Bleck TP. Intravenous midazolam for the treatment of status epilepticus. Crit Care Med 1992; 20: 483–8
Treiman DM, Meyers PD, Walton NY, et al. A comparison of four treatments for generalised convulsive status epilepticus. N Engl J Med 1998; 339: 792–8
Breimer LT, Hennis PJ, Burn AG, et al. Quantification of the EEG effect of midazolam by aperiodic analysis in volunteers: Pharmacokinetic/pharmacodynamic modelling. Clin Pharmacokinet 1990; 18: 245–53
Hotz MA, Ritz R, Linder L, et al. Auditory and electroencephalographic effects of midazolam and alpha-hydroxy-midazolam in healthy subjects. Br J Clin Pharmacol 2000; 49: 72–9
Schwart-Bloom RD, Miller KA, Evenson DA, et al. Benzodiazepines protect hippocampal neurons from degeneration after transient cerebral ischemia. Neuroscience 2000; 98: 471–84
de Jong RH, Bonin JD. Benzodiazepines protect mice from local anesthetic convulsions and deaths. Anesth Analg 1981; 60: 385–9
Fleischer JE, Milde JH, Moyer TP, et al. Cerebral effects of high dose midazolam and subsequent reversal with Ro15-1788 in dogs. Anesthesiology 1988; 68: 234–42
Cotev S, Shalit MN. Effects of diazepam on cerebral blood flow and oxygen uptake after head injury. Anesthesiology 1975; 43: 117–22
Tateishi A, Maekawa T, Takeshita H, et al. Diazepam and intracranial pressure. Anesthesiology 1981; 54: 335–7
Hoffman WE, Albrecht RF, Miletich DJ, et al. Cerebrovascular and cerebral metabolic effects of physostigmine, midazolam and a benzodiazepine antagonist. Anesth Analg 1986; 65: 639–44
Forster A, Juge O, Morel TP, et al. Effects of midazolam on cerebral blood flow on human volunteers. Anesthesiology 1982; 56: 453–5
Knudsen L, Cold GE, Holdgard HO, et al. The effects of midazolam on cerebral blood flow and oxygen consumption. Anaesthesia 1990; 45: 1016–9
Papazian L, Albanese J, Thirion X, et al. Effect of bolus doses of midazolam on intracranial pressure and cerebral perfusion pressure in patients with severe head injury. Br J Anaesth 1993; 71: 267–71
Shelly MP, Sultan MA, Bodenham A, et al. Midazolam infusions in critically ill patients. Eur J Anaesthesiol 1991; 8: 21–7
Nishiyama T. Sedation during artificial ventilation by continuous intravenous infusion of midazolam: effects of hepatocellular or renal damage. J Intensive Care Med 1997; 12: 40–4
Finley PR, Nolan PE. Precipitation of benzodiazepine withdrawal following sudden discontinuation of midazolam: DICP. Ann Pharmacother 1989; 23: 151–2
Sunzel M, Paalzow L, Berggren L, et al. Respiratory and cardiovascular effects in relation to plasma levels of midazolam and diazepam. Br J Clin Pharmacol 1988; 25: 561–9
Ronan KP, Gallagher TJ, George B, et al. Comparison of propofol and midazolam for sedation in intensive care unit patients. Crit Care Med 1995; 23: 286–93
Reves JG, Kissin I, Fournier S. Negative inotropic effects of midazolam. Anesthesiology 1984; 60: 517–8
Marty J, Gauzit R, Lefevre P, et al. Effects of diazepam and midazolam on baroreflex control of heart rate and on sympathetic activity in humans. Anesth Analg 1986; 65: 113–9
Chiolero RL, Ravussin P, Anderes JP, et al. The effects of midazolam reversal by RO15-1788 on cerebral perfusion pressure in patients with severe head injury. Intensive Care Med 1988; 14: 196–200
Chiolero RL, de Tribolet N. Sedatives and antagonists in the management of severely head-injured patients. Acta Neurochir Suppl (Wien) 1992; 55: 43–6
Harris CE, Grounds RM, Murray AM, et al. Propofol for long-term sedation in the ICU. Anaesthesia 1990; 45: 366–72
Bailey JM. Technique for quantifying the duration of intravenous anesthetic effect. Anesthesiology 1995 Nov; 83(5): 1095–103
Gepts E. Pharmacokinetic concepts for TCI anaesthesia. Anaesthesia 1998; 53Suppl. 1: 4–12
Bailey JM. Pharmacokinetic-pharmacodynamic modeling and ICU sedation: unexplored territories. Anesthesiology 2001; 95: 281–2
Leslie K, Sessler DI, Bjorksten AR, et al. Mild hypothermia alters propofol pharmacokinetics and increases the duration of action of atracurium. Anesth Analg 1995; 80: 1007–14
Myburgh JA, Upton RN, Grant C, et al. Epinephrine, norepinephrine and dopamine infusions decrease propofol concentrations during continuous propofol infusion in an ovine model. Intensive Care Med 2001; 27: 276–82
Buckley PM. Propofol in patients needing long-term sedation in intensive care: an assessment of the development of tolerance: a pilot study. Intensive Care Med 1997; 23: 969–74
Pinaud M, Lelausque J-N, Chetanneau A, et al. Effects of propofol on cerebral haemodynamics and metabolism in patients with head trauma. Anesthesiology 1990; 73: 404–9
Farling PA, Johnston JR, Coppel DL. Propofol infusion for sedation of patients with head injury in intensive care. Anaesthesia 1989; 44: 222–6
Kelly DF, Goodale DB, Williams J, et al. Propofol in the treatment of moderate and severe head injury: a randomised, prospective double-blinded pilot trial. J Neurosurg 1999; 90: 1042–52
Stewart L, Bullock R, Rafferty C, et al. Propofol sedation in severe head injury fails to control high ICP but reduces brain metabolism. Acta Neurochir 1994; 60: S544–6
Herregods L, Verbeke J, Rolly G, et al. Effect of propofol on elevated intracranial pressure. Anaesthesia 1988; 43: S107–9
Carrasco G, Molina R, Costa J, et al. Propofol versus midazolam in short-, medium-, and long-term sedation of critically ill patients: a cost-benefit analysis. Chest 1993; 103: 557–64
Ronan KP, Gallagher TJ, George B, et al. Comparison of propofol and midazolam for sedation in intensive care unit patients. Crit Care Med 1995; 23: 286–93
Barrientos-Vega R, Sanchez-Soria MM, Moralez-Garcia C, et al. Prolonged sedation of critically ill patients with midazolam or propofol: impact on weaning and costs. Crit Care Med 1997; 25: 33–40
Wood PR, Browne GPR, Pugh S. Propofol infusion for the treatment of status epilepticus. Lancet 1988; I: 480–1
Yanny HF, Christmas D. Propofol infusions for status epilepticus [letter]. Anaesthesia 1988; 43: 514
Thomas DG, Morgan P. Propofol infusions for the treatment of status epilepticus. Todays Anaesthetist 1989; 4: 106–7
Mackenzie SJ, Kapadia F, Grant IS. Propofol infusion for control of status epilepticus. Anaesthesia 1990; 45: 1043–5
United Kingdom Committee on Safety of Medicines. Current problems No. 20, 1987 Aug
Hodginson BP, Frith RW, Mee EDW. Propofol and the electroencephalogram. Lancet 1987; II: 1518
Harrigan PW, Browne SM, Quail AW. Multiple seizures following re-exposure to propofol. Anaesth Intensive Care 1996; 24: 261–4
Mirakhur RK. Induction characteristics of propofol in children: Comparison with thiopentone. Anaesthesia 1988; 43: 593–8
Illievich UM, Petriek W, Schramm W. Electroencephalographic burst suppression by propofol infusion in humans: hemodynamic consequences. Anesth Analg 1993; 77: 155–60
Stephan H, Sonntag H, Schenek HD, et al. Effects of Disoprivan on cerebral blood flow, cerebral oxygen consumption and cerebral vascular reactivity. Anaesthetist 1989; 36: 60–5
Ori C, Cavallini l, Freo U, et al. The effect of propofol on cerebral high energy metabolites, lactate, and glucose in normoxic and severely hypoxic rats. Life Sci 1997; 60: 1349–57
Gelb AW, Zhang C, Henderson SM. A comparison of the cerebral protective effects of propofol, thiopental and halothane in temporary feline focal cerebral ischemia [abstract]. Anesth Analg 1993; 76: S115
Young Y, Menon DK, Tisavipat N, et al. Propofol neuroprotection in a rat model of ischaemia reperfusion injury. Eur J Anaesthesiol 1997; 14: 320–6
Siani C, Zattoni J, Verardo T, et al. Response of intracranial pressure and systemic haemodynamics to 0.35, 0.80 and 2.5 mg/kg i.v. ‘Diprivan’ in conscious and normoventilated neurosurgical patients. 3rd Italian/French Meeting of Neuroanaesthesia. Capri: SIAARTI, 1986 May
Zattoni J, Siani C, Rossi A, et al. Effects of 0.8mg/kg of ‘Diprivan’ and 1.6 mg/kg of thiopentone on intracranial pressure and systemic blood pressure in neurosurgical patients. 3rd Italian-French Meeting of Neuroanaesthesia. Capri: CIAART, 1986 May
Mateu J, Barrachino F. Hypertriglyceridaemia associated with propofol sedation in critically ill patients. Intensive Care Med 1996; 22: 834–5
Laxenaire MC, Mata-Bermejo E, Moneret-Vautrin DA, et al. Life-threatening anaphylactoid reactions to propofol infusion. Neurology 1993; 77: 275–80
McHale SP, Konieczko K. Anaphylactoid reaction to propofol. Anaesthesia 1989; 47: 864–5
Possidente CJ, Rogers FB, Osler TM, et al. Elevated pancreatic enzymes after extended propofol therapy. Pharmacotherapy 1998; 18: 653–5
Wingfield TW. Pancreatitis after propofol administration: is there a relationship? Anesthesiology 1996; 84: 236–7
Leisure GS, O’Flaherty J, Green L, et al. Propofol and postoperative pancreatitis. Anesthesiology 1996; 84: 224–7
Donmez A, Sener M, Candan S, et al. Can we blame propofol for pancreatitis? Pharmacotherapy 1999; 19: 1181–2
Arduino MJ, Bland LA, McAllister SK, et al. Microbial growth and endotoxin production in the intravenous anesthetic propofol. Infect Control Hosp Epidemiol 1992; 12: 535–9
Langevin PB, Gravenstein N, Doyle TJ, et al. Growth of S. aureus in diprivan and intralipid: implications for the pathogenesis of infections. Anesthesiology 1999; 91: 1394–400
Hart B. ‘Diprivan’: a change of formulation. Eur J Anaesthesiol 2000; 17: 71–3
Zaloga GP, Teres D. The safety and efficacy of propofol containing EDTA: a randomised clinical trial programme focusing on cation and trace metal homeostasis in critically ill patients. Intensive Care Med 2000; 26Suppl. 4: S398–9
Higgins TL, Murray M, Kett DH, et al. Trace element homeostasis during continuous sedation with propofol containing EDTA versus other sedatives in critically ill patients. Intensive Care Med 2000; 26Suppl. 4: S413–21
Herr DL, Kelly K, Hall JB, et al. Safety and efficacy of propofol with EDTA when used for sedation of surgical intensive care unit patients. Intensive Care Med 2000; 26Suppl. 4: S452–62
Strickland RA, Murray MJ. Fatal metabolic acidosis in a pediatric patient receiving an infusion of propofol in the ICU: is there a relationship? Crit Care Med 1995; 23: 405–9
Parke TJ, Stevens JE, Rice ASC, et al. Metabolic acidosis and fatal myocardial failure after propofol infusion in children: five case reports. BMJ 1992; 305: 613–6
Bray RJ. Propofol infusion syndrome in children. Paediatr Anaesth 1998; 8: 491–9
Cannon ML, Glazier SS, Bauman LA. Metabolic acidosis, rhabdomyolysis, and cardiovascular collapse after prolonged propofol infusion. J Neurosurg 2001; 95: 1053–6
Cremer OL, Moons KGM, Bouman EAC, et al. Long-term propofol infusion and cardiac failure in adult head-injured patients. Lancet 2001; 357: 117–8
Menon DK, Matta BF, Gupta AK, et al. Propofol use in headinjury patients. Lancet 2001; 357: 1708–9
Kelly DF. Propofol infusion syndrome. J Neurosurg 2001; 95: 925–6
Cairns CJ, Thomas B, Fletcher S, et al. Life-threatening hyperkalaemia following therapeutic barbiturate coma. Intensive Care Med 2002; 28: 1357–60
Wolf A, Weir P, Segar P, et al. Impaired fatty acid oxidation in propofol infusion syndrome. Lancet 2001; 357: 606–7
Menon DK, Young Y, Tew DN, et al. New horizons in ICU sedation: exploring non-sedative effects of ICU sedation. Clin Intensive Care 1994; 5: 22–6
Egan TD, Lemmens HJM, Fiset P, et al. The pharmacokinetics of the new short-acting opioid remifentanil (GI8704B) in healthy adult male volunteers. Anesthesiology 1993; 79: 881–92
Thorpe DH. Opiate structure and activity: a guide to understanding the receptor. Anesth Analg 1984; 63: 143–51
Ling GSF, Spiegel K, Lockart SH, et al. Separation of opioid analgesia from respiratory depression. J Pharmacol Exp Ther 1985; 232: 149–56
Stanski DR. Pharmacokinetics and dynamics: the basis of infusion applications. Anaesth Intensive Care 1987; 15: 23–6
Davies G, Kingswood C, Street M. Pharmacokinetics of opioids in renal dysfunction. Clin Pharmacokinet 1996; 31: 410–22
Bodenham A, Park GR. Alfentanil infusion in patients requiring intensive care. Clin Pharmocokinet 1988; 15: 216–26
Ferrier C, Marty J, Bouffard Y, et al. Alfentanil pharmacokinetics in patients with cirrhosis. Anesthesiology 1985; 62: 480–4
Kapila A, Glass PS, Jacobs JR, et al. Measured contextsensitive half-times of remifentanil and alfentanil. Anesthesiology 1995; 83: 968–75
Warner DS. Experience with remifentanil in neurosurgical patients. Anesth Analg 1999; 89Suppl. 4: S33–9
Warner DS, Hindman BJ, Todd MM, et al. Intracranial pressure and hemodynamic effects of remifentanil versus alfentanil in patients undergoing supratentorial craniotomy. Anesth Analg 1996; 32: 348–53
Sneyd JR, Whaley A, Dimpel HL, et al. An open, randomised comparison of alfentanil, remifentanil and alfentanil followed by remifentanil in anesthesia for craniotomy. Br J Anaesth 1998; 81: 361–4
Coles JP, Leary TS, Monteiro JN, et al. Propofol anesthesia for craniotomy: a double-blind comparison of remifentanil, alfentanil, and fentanyl. J Neurosurg Anesthesiol 2000; 12: 15–20
Gesztesi Z, Mootz BL, White PF. The use of remifentanil infusion for hemodynamic control during intracranial surgery. Anesth Analg 1999; 89: 1282–7
Ostapkovich ND, Baker KZ, Fogarty-Mack P, et al. Cerebral blood flow and CO2 reactivity is similar during remifentanil/N2O and fentanyl/N2O anesthesia. Anesthesiology 1998; 89: 358–63
Lorenz HI, Kolbitsch C, Hormann C, et al. the effects of remifentanil on cerebral capacity in awake volunteers. Anesth Analg 2000; 90: 609–13
Bowler I, Djaiani G, Abel R, et al. A combination of intrathecal morphine and remifentanil anesthesia for fast-track cardiac anesthesia and surgery. J Cardiothorac Vasc Anesth 2002; 16: 709–14
Chinachoti T, Kessler P, Kirkham A, et al. Remifentanil vs morphine for patients in intensive care unit who need short-term mechanical ventilation. J Med Assoc Thai 2002; 85Suppl. 3: S848–57
Maze M, Scarfini C, Cavaliere F. New agents for sedation in the intensive care unit. Crit Care Clin 2001; 17: 881–97
Soltesz S, Biedler A, Silomon M, et al. Recovery after remifentanil and sufentanil for analgesia and sedation of mechanically ventilated patients after trauma or major surgery. Br J Anaesth 2001; 86: 763–8
Cohen J, Royston D. Remifentanil. Curr Opin Crit Care 2001; 7: 227–31
Olivier P, Sirieix D, Dassier P, et al. Continuous infusion of remifentanil and target-controlled infusion of propofol for patients undergoing cardiac surgery: a new approach for scheduled early extubation. J Cardiothorac Vasc Anesth 2000; 14: 29–35
Tipps LB, Coplin WM, Murry KR, et al. Safety and feasibility of continuous infusion of remifentanil in the neurosurgical intensive care unit. Neurosurgery 2000; 46: 596–602
Karabinis A, Hantson P, Speelberg B, et al. A remifentanilbased technique for analgesia and sedation in ICU patients with neurotrauma: preliminary data [abstract]. Intensive Care Med 2001; 27Suppl. 2: S275
Breen D, Wilmer A, Bodenham A, et al. The offset of pharmacodynamic effects of remifentanil in ICU patients is not affected by renal impairment [abstract]. Intensive Care Med 2001; 27Suppl. 2: S207
Russell D, Royston D, Rees PH, et al. Effect of temperature and cardiopulmonary bypass on the pharmacokinetics of remifentanil. Br J Anaesth 1997; 79: 456–9
Herrick IA, Gelb AW, Manninen PH, et al. Effects of fentanyl, sufentanil and alfentanil on brain retractor pressure. Anesth Analg 1991; 72: 359–63
From RP, Warner DS, Todd MM, et al. Anesthesia for craniotomy: a double-blind comparison of alfentanil, fentanyl and sufentanil. Anesthesiology 1990; 73: 896–904
de Nadal M, Munar F, Poca MA, et al. Cerebral haemodynamic effects of morphine and fentanyl in patients with severe head injury. Anesthesiology 2000; 92: 11–9
Albanese J, Viviand X, Potie F, et al. Sufentanil, fentanyl and alfentanil in head trauma patients: a study on cerebral hemodynamics. Crit Care Med 1999; 27(2): 407–11
Werner C, Kochs E, Bause H, et al. Effects of sufentanyl on cerebral hemodynamics and intracranial pressure in patients with brain injury. Anesthesiology 1995; 83: 721–6
Albanese J, Durbec O, Viviand X, et al. Sufentanil increases intracranial pressure in patients with head trauma. Anesthesiology 1993; 79: 493–7
Sperry RJ, Bailey PL, Reichman MV, et al. Fentanyl and sufentanil increase intracranial pressure in head trauma patients. Anesthesiology 1991; 77: 416–20
Brian Jr JE, Seifen AB. Tonic-clonic activity after sufentanil. Anesth Analg 1987; 66: 481–3
Goroszeniuk T, Malgosia A, Jones RM. Generalised grand mal seizure after recovery from uncomplicated fentanyl-etomidate anesthesia. Anesth Analg 1986; 65: 979–81
Hoisen AO. Another case of grand mal seizure after fentanyl administration. Anesthesiology 1984; 60: 387–8
Scott JC, Sarnquist FH. Seizure-like movements during fentanyl infusion with absence of seizure activity in a simultaneous EEG recording. Anesthesiology 1985; 62: 812–4
Flacke JW, Davis LJ, Flacke WE, et al. Effects of fentanyl and diazepam in dogs deprived of autonomic tone. Anesth Analg 1985; 64: 1053–9
Sebel PS, Bovill JG, Boekhorst RA, et al. Cardiovascular effects of high-dose fentanyl anaesthesia. Acta Anaesthesiol Scand 1982; 26: 308–15
Tammisto T, Takki S, Toikka P. A comparison of the circulatory effects in man of the analgesics fentanyl, pentazocine and pethidine. Br J Anaesth 1970; 42: 317–24
Flacke JW, Flacke WE, Bloor BC, et al. Histamine by four narcotics: a double-blind study in humans. Anesth Analg 1987; 66: 723–30
Rosow CE, Moss J, Philbin DM, et al. Histamine release during morphine and fentanyl anesthesia. Anesthesiology 1982; 56: 93–6
Moss J, Rosow CE. Histamine release by narcotics and muscle relaxants in humans. Anesthesiology 1983; 59: 330–59
Fahmy NR. Hemodynamics, plasma histamine, and catecholamine concentrations during anaphylactoid reaction to morphine. Anesthesiology 1981; 55: 329–31
Bowdle TA. Adverse effects of opioid agonists and agonist-antagonists in anaesthesia. Drug Saf 1998; 19: 173–89
Burks TF, Fox DA, Hirning LD, et al. Regulation of gastrointestinal function by multiple opioid receptors. Life Sci 1988; 43: 2177–81
Heyland DK, Tougas G, King D, et al. Impaired gastric emptying in mechanically ventilated, critically ill patients. Intensive Care Med 1996; 22: 1339–44
Morimoto Y, Morimoto Y, Bart RD, et al. High-dose fentanyl does not adversely affect outcome from forebrain ischemia in the rat. J Neurosurg Anesthesiol 1997; 9: 316–23
Soonthon V, Patel P, Drummond J, et al. Effect of fentanyl on cerebral injury after focal ischemia in rats. Anesth Analg 1998; 86: S357
Jeevaratnam DR, Menon DK. Survey of intensive care of severely head injured patients in the United Kingdom. BMJ 1996; 312: 944–7
Leeb-Lundberg F, Snowman A, Olsen RW. Barbiturate receptor sites are coupled to benzodiazepine receptors. Proc Natl Acad Sci U S A 1980; 77: 7468–72
Hudson RJ, Stanski DR, Burch PG. Pharmacokinetics of methohexital and thiopental in surgical patients. Anesthesiology 1983; 59: 215–9
Russo H, Simon N, Duboin MP, et al. Population pharmacokinetics of high-dose thiopental in patients with cerebral injuries. Clin Pharmacol Ther 1997; 62: 15–20
Russo H, Bressolle F, Duboin MP. Pharmacokinetics of high-dose thiopental in pediatric patients with increased intracranial pressure. Ther Drug Monit 1997; 19: 63–70
Le Corre P, Malledant Y, Tanguy M, et al. Non linear disposition of thiopentone following long-term infusion. Eur J Drug Metab Pharmacokinet 1993; 18: 255–9
Turcant A, Delhumeau A, Premel-Cabic A, et al. Thiopental pharmacokinetics under conditions of long-term infusion. Anesthesiology 1985; 63: 50–4
Nussmeier NA, Arlund C, Slogoff S, et al. Neuropsychiatric complications after cardiopulmonary bypass: cerebral protection by a barbiturate. Anesthesiology 1986; 64: 165–72
Cordato DJ, Herkes GK, Mather LE, et al. Prolonged thiopentone infusion for neurosurgical emergencies: usefulness of therapeutic drug monitoring. Anaesth Intensive Care 2001; 29: 339–48
Bayliff CD, Schwartz ML, Hardy BG. Pharmocokinetics of high-dose pentobarbital in severe head injury. Clin Pharmacol Ther 1985; 38: 457–61
Schickendantz J, Funk W, Ittner K-P, et al. Elimination of methohexitone after long-term, high-dose infusion in patients with critically elevated intracranial pressure. Crit Care Med 1999; 27: 1570–6
Smith AL, Wollman H. Cerebral blood flow and metabolism: effects of anesthetic drugs and techniques. Anesthesiology 1972; 36: 378–400
Shapiro MH, Wyte SR, Loesler J. Barbiturate augmented hypothermia for reduction of persistent intracranial hypertension. J Neurosurg 1979; 40: 90–100
Kassell NF, Hitchon PW, Gerk MK, et al. Alterations in cerebral blood flow, oxygen metabolism, and electrical activity produced by high-dose thiopental. Neurosurgery 1980; 7: 598–603
Marsh ML, Marshall LF, Shapiro HM. Neurosurgical intensive care. Anesthesiology 1977; 47: 149–63
Marshall LF, Smith RW, Shapiro HM. The outcome with aggressive treatment in severe head injuries: Part II. Acute and chronic barbiturate administration in the management of head injury. J Neurosurg 1979; 50: 26–30
Rockoff MA, Marshall LF, Shapiro HM. High-dose barbiturate therapy in humans: a clinical review of 60 patients. Ann Neurol 1979; 6: 194–9
Eisenberg HM, Frankowski RF, Contant CF, et al. High-dose barbiturate control of elevated intracranial pressure in patients with severe head injury. J Neurosurg 1988; 69: 15–23
Roberts I. Barbiturates for acute traumatic brain injury (Cochrane Review). Available in The Cochrane Library [database on disk and CD ROM]. Updated quarterly. The Cochrane Collaboration; issue 4. Oxford: Update Software, 2001
Nordstrom C-H, Messeter K, Sundbarg G, et al. Cerebral blood flow, vasoreactivity and oxygen consumption during barbiturate therapy in severe traumatic brain lesions. J Neurosurg 1988; 68: 424–31
Schwartz M, Tator C, Towed D, et al. The University of Toronto Head Injury Treatment Study: a prospective randomised comparison of pentobarbital and mannitol. Can J Neurol Sci 1984; 11: 434–40
Ward JD, Becker DP, Miller JD, et al. Failure of prophylactic barbiturate coma in the treatment of severe head injury. J Neurosurg 1985; 62: 383–8
Menon DK, Summors AJ. Neuroprotection. Curr Opin Anaesthesiol 1998; 11: 485–96
Shapiro HM. Barbiturates in brain ischaemia. Br J Anaesth 1985; 57: 82–95
Hobbs W, Rall T, Verdoorn T. Hypnotics and sedatives; ethanol. In: Gilman AG, Goodman LS, Gillman A, editors. Goodman and Gilman’s the pharmacological basis of therapeutics. 9th ed. New York: Macmillan, 1980: 373–7
Magnuson B, Hatton J, Zweng TN, et al. Pentobarbital coma in neurosurgical patients: nutrition considerations. Nutr Clin Pract 1994; 9: 146–50
Moudgil GC. Effects of premedicants, intravenous anaesthetic agents and local anaesthetics on phagocytosis in vitro. Can Anaesth Soc J 1981; 28: 597–602
Stover JF, Stocker R. Pharmacodynamics: barbiturate coma may promote reversible bone marrow suppression in patients with severe isolated brain injury. Eur J Clin Pharmacol 1998; 54: 529–34
Friederich P, Urban BW. Interaction of intravenous anesthetics with human neuronal potassium currents in relation to clinical concentrations. Anesthesiology 1999; 91: 1853–60
Chang T, Glazko AJ. Biotransformation and disposition of ketamine. Int Anesthesiol Clin 1974; 12: 157–77
Kolenda H, Gremmelt A, Rading S, et al. Ketamine for analgosedative therapy in intensive care treatment of head-injured patients. Acta Neurochir (Wien) 1996; 138: 1193–9
Bond AC, Davie CK. Ketamine and pancuronium for the shocked patient. Anaesthesia 1974; 29: 59–62
Johnstone M. The cardiovascular effects of ketamine in man. Anaesthesia 1976; 31: 873–82
Thomson AM, West DC, Lodge D. An N-methyl-aspartate-mediated synapse in rat cerebral cortex: a site of action of ketamine? Nature 1985; 313: 479–81
Eng C, Shapira Y, Lam AM. Ketamine is protective when given 2 but not 4 hours following closed cranial impact in rats. J Neurosurg Anesth 1992; 4: 305–8
Hoffman WE, Pllegrino D, Werner C, et al. Ketamine decreases plasma catecholamines and improves outcome from incomplete cerebral ischemia in rats. Anesthesiology 1992; 76: 755–62
Shapira Y, Artru AA, Lam WM. Ketamine decreases cerebral infarct volume and improves neurologicaloutcome following experimental head trauma in rats. J Neurosurg Anesthesiol 1991; 4: 231–40
Shapiro HM, Wyte SR, Harris AB. Ketamine anaesthesia in patients with intracranial pathology. Br J Anaesth 1972; 44: 1200–4
Albanese J, Arnaud S, Rey M, et al. Ketamine decreases intracranial pressure and electroencephalographic activity in traumatic brain injury patients during propofol sedation. Anesthesiology 1997; 87: 1328–34
Whyte SR, Shapiro HM, Turner P, et al. Ketamine-induced intracranial hypertension. Anesthesiology 1972; 36: 174–6
Gardner AE, Dannemeiller FJ, Dean D. Intracranial cerebrospinal fluid pressure in man during ketamine anaesthesia. Anesth Analg 1972; 51: 741–5
Schwedler M, Miletich DJ, Albrecht RF. Cerebral blood flow and metabolism following ketamine administration. Can Anaesth Soc J 1982; 29: 222–6
Domino EF, Chodoff P, Corssen G. Pharmacologic effects of Cl-581, a new dissociative anesthetic in man. Clin Pharmacol Ther 1965; 6: 279
Ferrer-Allado T, Brechner VL, Dymond A, et al. Ketamine induced electroconvulsive phenomena in the human limbic and thalamic regions. Anesthesiology 1973; 38: 333–4
Bennet DR, Madsen JA, Jordan WS, et al. Ketamine anesthesia in brain-damaged epileptics. Neurology 1973; 23: 449–60
Seth RD, Gidal BE. Refractory status epilepticus: response to ketamine. Neurology 1998; 51: 1765–6
Van Hamme MJ, Ghoneim MM, Ambre JJ. Pharmacokinetics of etomidate. Anesthesiology 1978; 49: 274–7
Cunitz G, Danhauser I, Wickbold J. Comparative investigations on the influence of etomidate, thiopentone and methohexitone on the intracranial pressure of the patient. Anaesthetist 1978; 27: 64–70
Moss E, Powell D, Gibson RM, et al. Effect of etomidate on intracranial pressure and cerebral perfusion pressure. Br J Anaesth 1979; 51: 347–52
Renou AM, Vernhiet J, Macrez P, et al. Cerebral blood flow and metabolism during etomidate anaesthesia in man. Br J Anaesth 1978; 50: 1047–51
Dearden NM, McDowell DG. Comparison of etomidate and althesin in the reduction of increased intracranial pressure after head injury. Br J Anaesth 1985 Apr; 57: 361–8
Modica PA, Tempelhoff R. Intracranial pressure during induction of anaesthesia and tracheal intubation with etomidateinduced EEG burst suppression. Can J Anaesth 1992; 39: 236–41
Gooding JH, Weng J-T, Smith RA, et al. Cardiovascular and pulmonary responses following etomidate induction of anaesthesia in patients with demonstrated cardiac disease. Anaesth Analg 1979; 58: 40–1
Holdcroft A, Morgan M, Whitwam JG, et al. Effect of dose and premedication on induction complications with etomidate. Br J Anaesth 1976; 48: 199–205
Kay B. A dose-response relationship for etomidate, with some observations on cumulation. Br J Anaesth 1976; 48: 213–6
Cohn BF, Rejger V, Hagenouw-Taal JC, et al. Results of a feasibility trial to achieve total immobilisation of patients in a neurosurgical intensive care unit with etomidate. Anesthesia 1983 Jul; 38Suppl.: 47–50
Prior JGL, Hinds J, Prior PF. The use of etomidate in the management of severe head injury. Intensive Care Med 1983; 9: 313–20
Bingham RM, Procaccio F, Prior PF, et al. Cerebral electrical activity influences the effects on cerebral perfusion pressure in traumatic coma. Br J Anaesth 1985 Sep; 57: 843–8
Fragen RJ, Weiss HW, Molteni A. The effect of propofol on adrenocortical steroidogenesis: a comparative study with etomidate and thiopental. Anesthesiology 1987; 66: 839–42
Weber MM, Lang J, Abedinopur F, et al. Different inhibitory effect of etomidate and ketoconazole on human adrenal steroid biosynthesis. Clin Invest 1993; 71: 933–8
Wagner RL, White PF. Etomidate inhibits adrenocortical function in surgical patients. Anesthesiology 1984; 60: 647–51
Absalom A, Pledger D, Kong A. Adrenocortical function in critically ill patients 24 hr after a single dose of etomidate. Anaesthesia 1999; 54: 861–7
Wyatt I, Ledingham IM. Mortality amongst multiple trauma patients admitted to an intensive therapy unit. Anaesthesia 1984; 39: 973–81
Varon J, Marik P. Etomidate and propylene glycol toxicity. J Emerg Med 1998; 16: 485
Doenicke A, Roizen MF, Hoernecke R, et al. Haemolysis after etomidate: comparison of propylene glycol and lipid formulations. Br J Anaesth 1997; 79: 386–8
McConnel JR, Ong CS, McAllister JL, et al. Propylene glycol toxicity following continuous etomidate infusion for the control of refractory cerebral edema. Neurosurgery 1996; 38: 232–3
Van de Wiele B, Rubinstein E, Peacock W, et al. Propylene glycol toxicity caused by prolonged infusion of etomidate. J Neurosurg Anesthesiol 1995; 7: 259–62
Levy ML, Aranda M, Zelman V, et al. Propylene glycol toxicity following continuous etomidate infusion for the control of refractory cerebral edema. Neurosurgery 1995; 37: 363–9
Segal IS, Vickery RG, Walton JK, et al. Dexmedetomidine diminishes halothane anesthetic requirements in rats through postsynaptic alpha-2 adrenergic receptor. Anesthesiology 1988; 69: 818–23
Coughlan MG, Lee JG, Bosnjak ZJ, et al. Direct coronary and cerebral vascular responses to dexmedetomidine: significance of endogenous nitric oxide synthesis. Anesthesiology 1992; 77: 998–1006
Scheinin H, Karhuvaara S, Olkkola KT, et al. Pharmacodynamics and pharmacokinetics of intramuscular dexmedetomidine. Clin Pharmacol Ther 1992; 52: 537–46
Rodrigues AD, Roberts EM. The in vitro interaction of dexmedetomidine with human liver microsomal cytochtome P4502D6 (CYP2D6). Drug Metab Dispos 1997; 25: 651–5
Scarby T. Pharmacological properties of prejunctional alpha-adrenoceptors in isolated feline middle cerebral arteries: comparison with the postjunctional alpha-adrenoceptors. Acta Physiol Scand 1984; 122: 165–74
Fale A, Kirsch JR, McPherson RW. α2-Adrenergic agonist effects on normocapnic and hypercapnic cerebral blood flow in the dog are anesthetic dependent. Anesth Analg 1994; 79: 892–8
Zornow MH, Scheller MS, Sheehan PB, et al. Intracranial pressure effects of dexmedetomidine in rabbits. Anesth Analg 1992; 75: 232–7
Hoffman WE, Kochs E, Werner C, et al. Dexmedetomidine improves neurological outcome from incomplete ischemia in the rat. Anesthesiology 1991; 75: 328–32
Talke P, Tong C, Lee HW, et al. Effect of dexmedetomidine on lumbar cerebrospinal fluid pressure in humans. Anesth Analg 1997; 85: 358–64
Khan ZP, Ferguson CN, Jones RM. Alpha-2 and imidazoline receptor agonists: their pharmacology and therapeutic role. Anaesthesia 1999; 54: 146–65
Payen D, Quintin L, Plaisance P, et al. Head injury: clonidine decreases plasma catecholamines. Crit Care Med 1991; 18: 392–5
Asgeirsson B, Grände P-O, Nordstrom C-H, et al. Effects of hypotensive treatment with β2-agonist and β1-agonist on cerebral haemodynamics in severely head injured patients. Acta Anaesthesiol Scand 1995; 39: 347–51
Asgeirsson B, Grände P-O, Nordstrom C-H. A new therapy of post-trauma edema based on haemodynamics principles for brain volume regulation. Crit Care Med 1994; 20: 260–4
Eker C, Asgeirsson B, Grande P-O, et al. Improved outcome after severe head injury with a new therapy based on principles for brain volume regulation and preserved microcirculation. Crit Care Med 1998; 26: 1881–6
Minassian AT, Beydon L, Decq P, et al. Changes in cerebral haemodynamics after a single dose of clonidine in severely head-injured patients. Anesth Analg 1997; 84: 127–32
Brook AD, Ahrens TS, Schaiff R, et al. Effect of a nursingimplemented sedation protocol on the duration of mechanical ventilation. Crit Care Med 1999; 27: 2609–15
Fischler M, Bonnet F, Trang H, et al. The pharmacokinetics of droperidol in anesthetised patients. Anesthesiology 1986; 64: 486–9
Stanley TH. Cardiovascular effects of droperidol during enflurane and enflurane-nitrous oxide anesthesia in man. Can J Anaesth 1978; 25: 26–9
Levante A, Raggueneau JL, Trawale JM, et al. Neuroleptics and continuous measurement of intracranial pressure. Ann Anesthesiol Fr 1976; 17: 1189–92
Michenfelder JD, Theyn RA. Effects of fentanyl, droperidol and Innovar on canine cerebral metabolism and blood flow. Br J Anaesth 1971; 43: 630–5
Rao N, Jellinek HM, Wollston DC. Agitation in closed head injury: haloperidol effects on rehabilitation outcome. Arch Phys Med Rehabil 1985; 66: 30–4
Harvey M. Managing agitation in critically ill patients. Am J Crit Care 1996; 5: 7–15
Carroll K, Magruder K. The role of analgesics and sedatives in the management of pain and agitation during weaning from mechanical ventilation. Crit Care Nurs Q 1993; 15: 68–77
Lund N, Papadakos PJ. Barbiturates, neuroleptics, and propofol for sedation. Crit Care Med 1995; 11: 875–86
Hunt N, Stern TA. The association between IV haloperidol and torsades de pointes. Psychosomatics 1995; 36: 541–9
Baldessarini RJ. Drugs and the treatment of psychiatric disorders. In: Golman AG, Rall TW, Nies AS, et al., editors. The pharmacological basis of therapeutics. New York: Pergamon Press, 1990
Elovic EP, Lansang R, Li Y, et al. The use of atypical antipsychotics in traumatic brain injury. J Head Traurna Rehabil 2003; 19: 177–95
Temple MT. Use of atypical anti-psychoties in the management of post-traumatic confusional, states in traumatic brain injury. J R Army Med Corps. 2003; 149: 54–5
Cohen IL, editor. The management of the agitated ICU patient. Crit Care Med 2002; 30 Suppl.: S97–S123
Acknowledgements
The authors have provided no information on sources of funding or on conflicts of interest directly relevant to the content of this review.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Urwin, S.C., Menon, D.K. Comparative Tolerability of Sedative Agents in Head-Injured Adults. Drug-Safety 27, 107–133 (2004). https://doi.org/10.2165/00002018-200427020-00003
Published:
Issue Date:
DOI: https://doi.org/10.2165/00002018-200427020-00003