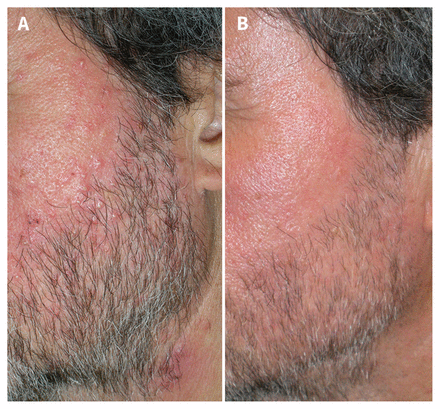
A 66-year-old man was referred by his primary care physician for assessment of a three-year history of treatment-resistant pruritic facial lesions. The patient had multiple system atrophy, treated with a combination of carbidopa/levodopa/entacapone and pramipexole. His multiple facial pustules had not responded to amoxicillin, amoxicillin/clavulanic acid, doxycycline (100 mg/d for 6 months) or topical metronidazole. He had had a partial response following treatment with isotretinoin (0.25 mg/kg daily, then 0.5 mg/kg daily for 6 months), but the pustules had relapsed immediately after treatment withdrawal. We observed multiple light-brown papules and pustules over his cheeks, chin and forehead, associated with dryness and erythema, but no comedones, telangiectasias or flushing (Figure 1A). Bacterial and fungal cultures of the pustules were negative. Skin scraping samples were negative for Malassezia (formerly known as Pityrosporum), but positive for large quantities of Demodex mites, identified as Demodex folliculorum (see Appendix 1, available at www.cmaj.ca/lookup/suppl/doi:10.1503/cmaj.161323/-/DC1). We diagnosed demodicosis. Substantial improvement was observed after two doses of oral ivermectin (200 μg/kg per dose, 2 weeks apart) with no relapse after one year (Figure 1B).
(A) Numerous papules and pustules, associated with facial erythema, over the cheeks and forehead of a 66-year-old man. (B) Substantial improvement following treatment with oral ivermectine.
Demodex folliculorum is a saprophytic parasitic mite of the pilosebaceous follicle and seborrheic glands and is found mainly on the face of adult men.1,2 The role of Demodex mites in inflammatory skin conditions remains controversial, but is suggested by the efficacy of topical or oral antiparasitic therapy. Demodex folliculorum should be considered whenever a rosacea-like or papulopustular eruption of the face fails to respond to standard therapy for rosacea, and no bacterial pathogens can be implicated.1 The condition is characterized by itchy pustules, follicular scaling and dryness, conglobata demodicosis with nodulocystic lesions, and blepharitis.1,2 Demodicosis is more frequent in immunocompromised patients with HIV, diabetes and hematopoietic malignancies. Diagnosis relies on skin surface biopsy and skin scrapings, with mite colonization greater than 5/cm2.1–3 Treatment recommendations are supported by case reports and include crotamiton cream, tetracyclines, and topical or systemic metronidazole. Topical and oral ivermectin may be effective in severe cases, although these are not readily available in Canada.1–3
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
The authors have obtained patient consent.