Abstract
Background: The choice of bearing articulation for total hip arthroplasty in younger patients is amenable to debate. We compared mid-term patient-reported outcomes and survivorship across 2 different bearing articulations in a young patient cohort.
Methods: We reviewed patients with cobalt-chrome or oxidized zirconium on highly crosslinked polyethylene who were followed prospectively between 2004 and 2012. Kaplan–Meier analysis was used to determine predicted cumulative survivorship at 5 years with all-cause and aseptic revisions as the outcome. We compared patient-reported outcomes, including the Harris hip score (HHS), Western Ontario and McMaster University Osteoarthritis Index (WOMAC) and Short-form 12 (SF-12) scores.
Results: A total of 622 patients were followed during the study period. Mean follow-up was 8.2 (range 2.0–10.6) years for cobalt-chrome and 7.8 (range 2.1–10.7) years for oxidized zirconium. Mean age was 54.9 ± 10.6 years for cobalt-chrome and 54.8 ± 10.7 years for oxidized zirconium. Implant survivorship was 96.0% (95% confidence interval [CI] 94.9%–97.1%) for cobalt-chrome and 98.7% (95% CI 98.0%–99.4%) for oxidized zirconium on highly crosslinked polyethylene for all-cause revisions, and 97.2% (95% CI 96.2%–98.2%) for cobalt-chrome and 99.0% (95% CI 98.4%–99.6%) for oxidized zirconium for aseptic revisions. An age-, sex- and diagnosis-matched comparison of the HHS, WOMAC and SF-12 scores demonstrated no significant changes in clinical outcomes across the groups.
Conclusion: Both bearing surface couples demonstrated excellent mid-term survivorship and outcomes in young patient cohorts. Future analyses on wear and costs are warranted to elicit differences between the groups at long-term follow-up.
The use of total hip arthroplasty in younger patient populations is becoming more common in clinical practice.1–3 Basic science and clinical research has provided an understanding of implant survivorship, patient satisfaction and complication rates in traditional bearing surfaces.4 Patient factors, implant-specific wear properties and survivorship influence implant selection.1 Concerns remain regarding polyethylene wear in younger, higher-demand patients, resulting in osteolysis secondary to localized phagocytosis.1,4 The introduction of highly crosslinked polyethylene has resulted in lower wear rates with at least intermediate follow-up than conventional polyethylene.5–11 The improved wear rates are also maintained across various manufacturers of highly crosslinked polyethylene. However, there is a variety of femoral heads to select and pair with this improved polyethylene surface.
Cobalt-chrome on polyethylene is a long-standing bearing couple that has the advantage of modularity and avoids the risk of fracture seen with ceramic articulations.12 However, both simulator and clinical studies demonstrate the potential for oxidative wear and damage, resulting in a roughened surface and accelerated polyethylene wear.1,12,13 Oxidized zirconium is a metallic alloy centre with an oxidized zirconium surface 5–10 μm thick that offers reduced wear rates on a polyethylene bearing surface.1,14 It was introduced to improve scratch resistance over traditional cobalt-chromium heads and to lower the risk of femoral head fracture reported with ceramic implants.15,16 Tribiological testing has shown that oxidized zirconium has better wettability and less surface adhesion on polyethylene than cobalt-chrome.17
Although the advantages and disadvantages of these bearing surface couples are well described, few studies have directly compared the bearing surface couples with respect to implant survivorship and clinical outcomes. Therefore, the purpose of this study was to directly compare age-, sex-and body mass index (BMI)–matched cohorts of patients who received cobalt-chrome or oxidized zirconium on highly crosslinked polyethylene. Our hypothesis was that implant survivorship and clinical outcomes would not differ significantly between the groups at mid-term follow-up.
Methods
We completed a retrospective review of our prospective institutional arthroplasty database for the period 2004–2012 to identify all patients undergoing primary total hip arthroplasty procedures using highly crosslinked polyethylene. Seven different surgeons within our institution performed the procedures. To be included in the analysis, patients had to be English-speaking and older than 19 years, and they had to have undergone primary total hip procedures performed using a cobalt-chrome or oxidized zirconium femoral head and a highly crosslinked polyethylene liner. Procedures were then stratified based on the femoral head bearing surface. We collected data, including patient age, sex, BMI and primary diagnosis at the time of the index procedure. The time to latest follow-up was also recorded.
We identified the patients in whom a cobalt-chrome femoral head was used, and these patients were matched with those who received an oxidized zirconium (Oxinium TM, Smith and Nephew) femoral head and compared based on sex, age and BMI. We included patients with a minimum 2-year follow-up and with complete clinical and radiographic data.
Implant survivorship data were collected, including the time to revision in years. We also documented the cause of revision. Clinical outcome measures, including the Harris Hip Score (HHS),18 Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC)19 and the Short-Form 12 (SF-12)20 questionnaire were reviewed. The pre- and postoperative scores for each questionnaire were recorded and used to calculate change scores at latest follow-up. We also compared the absolute value of each questionnaire at latest follow-up. Patients had routine follow-up at 6 weeks, 3 months and 1 year, and then annually or biannually depending on clinical progress.
Plain radiographs were obtained at routine follow-up visits. Views included an anterior–posterior (AP) pelvis as well as an AP and lateral view of the involved hip. Images were reviewed via the web-based image viewer Centricity Enterprise Web (GE Medical Systems) under 2× magnification. One of the operating surgeons (S.M.P.) interpreted the radiographs along with a fellowship-trained arthroplasty surgeon who did not operate on any of the included patients. The images were analyzed for areas of osteolysis within the femoral Gruen zones and acetabular DeLee–Charnley zones.21,22 Any cases revised during the study period were excluded from radiographic analysis. Institutional review board approval was obtained for completion of this study.
Statistical analysis
We assessed demographic variables using descriptive statistics. Kaplan–Meier analysis was used to generate survivorship curves with 95% confidence intervals (CIs) and to determine predicted cumulative survivorship at 5 years with revision for any cause as the end point. We also calculated the 5-year survivorship for aseptic revisions. All of the outcome measures (WOMAC, SF-12, HHS) and continuous variables were evaluated preoperatively and from the most recent postoperative visit using a 2-sided t test. Nominal data were compared using a Pearson χ2 analysis. A 2-sided p < 0.05 indicated statistical significance. We used SPSS software version 20 (SPSS Inc) for all analyses.
Results
A total of 622 patients were included in our analysis; 311 received a cobalt-chrome femoral head and 311 received an oxidized zirconium femoral head. Patient demographic and clinical characteristics for each group are outlined in Table 1. The mean time to latest follow-up was 8.1 (range 2.0–10.6) years for the cobalt-chrome group and 7.8 (range 2.1–10.7) years for the oxidized zirconium group. The most common primary diagnosis at the time of the index procedure in both groups was osteoarthritis (Table 1). The types and sizes of femoral heads as well as highly crosslinked polyethylene liners are listed in Table 2.
Patient demographic and clinical characteristics at the time of surgery
Distribution of femoral head implants and highly crosslinked polyethylene liners
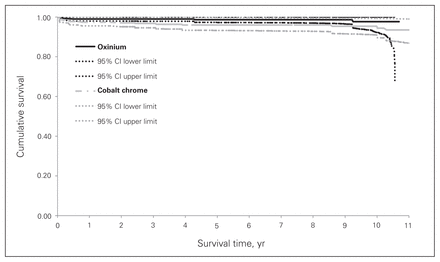
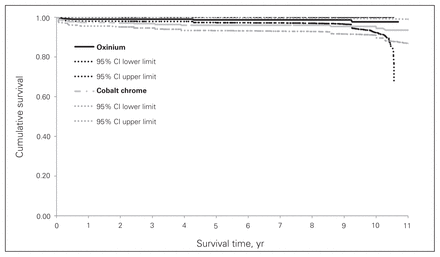
Implant survivorship was 96.0% (95% CI 94.9%–97.1%) for cobalt-chrome and 98.7% (95% CI 98.0%–99.4%) for oxidized zirconium on highly crosslinked polyethylene for all-cause revisions (Fig. 1). Implant survivorship was 97.2% (95% CI 96.2%–98.2%) for cobalt-chrome and 99.0% (95% CI 98.4%–99.6%) for oxidized zirconium for aseptic revisions (Fig. 2).
Kaplan–Meier analysis for all-cause revisions with 95% confidence intervals (CIs).
Kaplan–Meier analysis for aseptic revisions with 95% confidence intervals (CIs).
There were no statistically significant differences between the groups in the outcome measure change scores for age-, sex- and diagnosis-matched comparisons. There were also no statistically significant differences in the absolute SF-12, WOMAC or HHS scores at latest follow-up (Table 3).
Clinical outcome change score and score at latest follow-up
There were a total of 19 complications requiring revision during the study period (Table 4). All cases revised for periprosthetic infection were managed with a 2-stage revision, as they were classified as chronic periprosthetic infections.23 The patient in the cobalt-chrome group whose case was revised for aseptic loosening had a loose femoral stem, the patient in the oxidized zirconium cohort whose case was revised for that reason had a loose acetabular component. One of the patients in the cobalt-chrome cohort who underwent revision for a dislocation had an acetabular revision with head and liner exchange. The remaining patients with dislocations were managed with closed reduction. One of the patients in the cobalt-chrome group with a periprosthetic fracture was revised to a long, extensively coated stem. The remaining patients with periprosthetic fractures had Vancouver AG fractures managed nonoperatively with protected weight bearing.24 No patients underwent revision for polyethylene wear.
Etiology of revision cases
Discussion
This study reports survivorship and clinical outcomes across 2 different femoral head options on a highly crosslinked polyethylene liner from a large, prospectively collected cohort. Survivorship was 96.0% for cobalt-chrome and 98.7% for oxidized zirconium for all-cause revisions at 5 years. Both bearing articulations demonstrated improvement in clinical outcome measures and had no statistically significant differences in change scores for age-, sex- and diagnosis-matched comparisons. The mean change scores all surpassed the minimally important difference reported in the literature for all outcome measures except the mental component summary score on the SF-12.25,26 The difference in number of instability revision cases may be attributable to reduced use of 32 mm and 36 mm femoral heads in the cobalt-chrome group.
Total hip arthroplasty is a procedure being performed in progressively younger patients, with increasing physical demands being placed on the implants. Highly crosslinked polyethylene was introduced in an effort to decrease wear rates and reduce the risk of osteolysis and aseptic loosening secondary to polyethylene wear.5,6,9,27,28 Previously, cobalt-chrome has been reported to have increased adhesive wear compared with oxidized zirconium on ultra-high molecular weight polyethylene.17 More recently, cobalt-chrome has demonstrated reduced wear rates using this bearing surface, and highly crosslinked polyethylene has been recommended for younger patients undergoing total hip arthroplasty.29–32 Our study demonstrates that excellent clinical outcomes are achievable with cobalt-chrome and oxidized zirconium femoral head articulations on a highly crosslinked polyethylene liner.
A study by Lewis and colleagues2 examined clinical outcomes with oxidized zirconium as a bearing articulation in 100 young patients undergoing total hip arthroplasty randomized to either cobalt-chrome or oxidized zirconium femoral heads. Both groups demonstrated excellent results and comparable improvements across the HHS, WOMAC and SF-12 outcome measures. Limitations to that study were that both groups received either conventional or highly crosslinked polyethylene, and the results were reported after only 2 years.2 That group’s findings are now supported by our findings at mid-term follow-up, as we found no significant differences between the groups across any of the outcome measures.
Periprosthetic dislocation was the most common complication and warrants further discussion. Implant retrieval studies have identified that although oxidized zirconium may be more scratch-resistant than cobalt-chrome,1 it is still vulnerable to in situ damage that may compromise long-term survivorship. One case report33 of an early anterior hip dislocation demonstrated surface damage to an oxidized zirconium head, exposing the zirconium-based undersurface. Electron microscopy demonstrated delamination of the oxidized layer. Another case report34 discussed an immediate revision for leg-length discrepancy using an oxidized zirconium head. Stereomicroscopy revealed evidence of metal transfer, likely from the acetabular component, deep scratches and cracks in the oxidized surface. Wear analysis of oxidized zirconium heads showed that the wear rates of those damaged clinically through attempted closed reductions or damaged through simulation were up to 50 times faster than wear rates in undamaged heads.35 These studies emphasize that great care needs to be taken when any closed reduction is attempted with an oxidized zirconium femoral head — a principle that should be applied to all bearing articulations.
Limitations
Our study is not without limitations. Owing to the improved wear properties of oxidized zirconium on highly crosslinked polyethylene reported in the literature, there is a selection bias to a younger or more active patient population. This cannot be accounted for using a retrospective study design. A randomized controlled trial would account for this limitation. As a result of this selection bias, the use of clinical questionnaires in this population may succumb to a ceiling effect, thus a detectable difference in clinical performance may not be possible.36 Furthermore, with the exception of the oxidized zirconium heads (which were from only 1 manufacturer), there was some heterogeneity with respect to the design and manufacturer of the femoral heads, highly crosslinked polyethylene liners and femoral stem and acetabular cup design. This heterogeneity is largely owing to surgeon preference. Our radiographic analysis was limited to a determination of osteolysis in either cohort; however, it would be unlikely that there would be any detectable differences in polyethylene wear between the groups given the mid-term follow-up period examined in this study.
Conclusion
Our results demonstrate excellent mid-term clinical outcomes and survivorship for both bearing surfaces. The cobalt-chrome and oxidized zirconium on highly crosslinked polyethylene articulations are both excellent considerations in young patients undergoing total hip arthroplasty. Further long-term clinical and radiographic follow-up of these cohorts is required to determine whether there is a detectable difference in polyethylene wear that may result in discernible differences in survivorship. Advanced techniques in wear analysis should also be used to delineate these differences in a matched bearing surface cohort. Finally, a cost-effectiveness analysis would be warranted given similar short- and mid-term clinical outcomes between the bearing articulations and differing costs among femoral head designs.
Footnotes
Competing interests: R. McCalden is paid consultant for Smith and Nephew. J. Howard is paid consultant for Smith and Nephew, Stryker, and DePuy. D. Naudie is a paid consultant for Smith and Nephew, Stryker, and Zimmer. E. Vasarhelyi is paid consultant for DePuy. No other competing interests declared.
Contributors: All authors designed the study. S. Petis and L. Somerville acquired the data, which all authors analyzed. S. Petis and L. Somerville wrote the article, which all authors reviewed and approved for publication.
- Accepted December 7, 2015.