Abstract
Background
Breast reconstruction is generally discouraged in women with inflammatory breast cancer (IBC). Nevertheless, reconstruction rates are increasing in this population.
Objective
We aimed to determine contemporary trends and predictors of breast reconstruction use and its impact on mortality among IBC patients.
Methods
Demographic, clinicopathologic, and follow-up data for women with non-metastatic IBC having mastectomy between 2004 and 2015 were collected from the Surveillance, Epidemiology, and End Results (SEER) 18 registries database. Rates and predictors of immediate breast reconstruction, along with survival outcomes between the breast reconstruction and no reconstruction groups were calculated. To account for selection bias, a propensity score analysis matching one reconstruction patient to three no reconstruction patients was performed.
Results
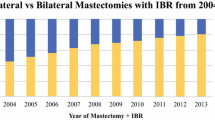
A total of 4076 women with non-metastatic IBC who underwent mastectomy (388 [9.5%] with breast reconstruction and 3688 [90.5%] without) were included. The proportion of women undergoing breast reconstruction and contralateral prophylactic mastectomy increased from 6.2 to 15.3% and 12.9 to 29.6%, respectively, between 2004 and 2015. Younger age, higher annual income, metropolitan residence, and bilateral mastectomy predicted breast reconstruction use. The 10-year breast cancer-specific survival was 62.9% for women having breast reconstruction and 47.6% for women not having breast reconstruction. After propensity-matched analysis, 10-year cancer-specific survival was similar between the reconstruction (56.6%) and no reconstruction (62.2%) groups (adjusted hazard ratio 0.96, 95% confidence interval 0.79–1.16; p = 0.65).
Conclusions
Breast reconstruction rates continue to rise among IBC patients, particularly young women and women with access to reconstruction. Breast reconstruction is not associated with inferior breast cancer-specific survival and can be an option for select patients.


Similar content being viewed by others
References
Menta A, Fouad TM, Lucci A, et al. Inflammatory breast cancer: what to know about this unique, aggressive breast cancer. Surg Clin North Am. 2018. https://doi.org/10.1016/j.suc.2018.03.009.
Palangie T, Mosseri V, Mihura J, et al. Prognostic factors in inflammatory breast cancer and therapeutic implications. Eur J Cancer. 1994. https://doi.org/10.1016/0959-8049(94)90115-5.
Yang CH, Cristofanilli M. Systemic treatments for inflammatory breast cancer. Breast Dis. 2006. https://doi.org/10.3233/bd-2006-22107.
Cristofanilli M, Valero V, Buzdar AU, et al. Inflammatory breast cancer (IBC) and patterns of recurrence: understanding the biology of a unique disease. Cancer. 2007. https://doi.org/10.1002/cncr.22927.
Thoms WW, McNeese M, Fletcher GH, Buzdar AU, Eva Singletary S, Jane OM. Multimodal treatment for inflammatory breast cancer. Int J Radiat Oncol Biol Phys. 1989. https://doi.org/10.1016/0360-3016(89)90060-6.
Baldini E, Gardin G, Evangelista G, Prochilo T, Collecchi P, Lionetto R. Long-term results of combined-modality therapy for inflammatory breast carcinoma. Clin Breast Cancer. 2004. https://doi.org/10.3816/cbc.2004.n.042.
Rehman S, Reddy CA, Tendulkar RD. Modern outcomes of inflammatory breast cancer. Int J Radiat Oncol Biol Phys. 2012. https://doi.org/10.1016/j.ijrobp.2012.01.030.
Adesoye T, Lucci A. Current surgical management of inflammatory breast cancer. Ann Surg Oncol. 2021. https://doi.org/10.1245/s10434-021-10522-z.
Chang EI, Chang EI, Ito R, et al. Challenging a traditional paradigm: 12-year experience with autologous free flap breast reconstruction for inflammatory breast cancer. Plast Reconstr Surg. 2015. https://doi.org/10.1097/prs.0000000000000900.
Santos PM, Bogen H, Taunk NK, Tchou J, Wu L, Freedman GM. Reconstruction does not impact local control or survival outcomes in inflammatory breast cancer patients treated with trimodality therapy [poster abstract]. Int J Radiat Oncol Biol Phys. 2019;103(5):E23.
Simpson AB, McCray D, Wengler C, et al. Immediate reconstruction in inflammatory breast cancer: challenging current care. Ann Surg Oncol. 2016. https://doi.org/10.1245/s10434-016-5554-z.
Mortenson MM, Schneider PD, Khatri VP, et al. Immediate breast reconstruction after mastectomy increases wound complications: however, initiation of adjuvant chemotherapy is not delayed. Arch Surg. 2004. https://doi.org/10.1001/archsurg.139.9.988.
Karadsheh MJ, Katsnelson JY, Ruth KJ, et al. Breast reconstruction in inflammatory breast cancer: an analysis of predictors, trends, and survival from the National Cancer Database. Plast Reconstrc Surg Glob Open. 2021. https://doi.org/10.1097/GOX.0000000000003528.
Chen H, Wu K, Wang M, Wang F, Zhang M, Zhang P. A standard mastectomy should not be the only recommended breast surgical treatment for non-metastatic inflammatory breast cancer: a large population-based study in the Surveillance, Epidemiology, and End Results database 18. Breast. 2017. https://doi.org/10.1016/j.breast.2017.06.002.
von Elm E, Altman DG, Egger M, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007. https://doi.org/10.1016/S0140-6736(07)61602-X.
Austin PC. Optimal caliper widths for propensity-score matching when estimating differences in means and differences in proportions in observational studies. Pharm Stat. 2011;10(2):150–61. https://doi.org/10.1002/pst.433.
Austin PC, Stuart EA. Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies. Stat Med. 2015;34(28):3661–79. https://doi.org/10.1002/sim.6607.
Droulias CA, Sewell CW, McSweeney MB, Powell RW. Inflammatory carcinoma of the breast: a correlation of clinical, radiologic and pathologic findings. Ann Surg. 1976. https://doi.org/10.1097/00000658-1976080000-00014.
Dawood S, Lei X, Dent R, et al. Survival of women with inflammatory breast cancer: a large population-based study. Ann Oncol. 2014. https://doi.org/10.1093/annonc/mdu121.
Hance KW, Anderson WF, Devesa SS, Young HA, Levine PH. Trends in inflammatory breast carcinoma incidence and survival: the surveillance, epidemiology, and end results program at the National Cancer Institute. J Natl Cancer Inst. 2005. https://doi.org/10.1093/jnci/dji172.
Anderson WF, Schairer C, Chen BE, Hance KW, Levine PH. Epidemiology of inflammatory breast cancer (IBC). Breast Dis. 2006. https://doi.org/10.3233/bd-2006-22103.
Li BD, Sicard MA, Ampil F, et al. Trimodal therapy for inflammatory breast cancer: a surgeon’s perspective. Oncology. 2010. https://doi.org/10.1159/000318529.
van Uden DJP, van Maaren MC, Bult P, et al. Pathologic complete response and overall survival in breast cancer subtypes in stage III inflammatory breast cancer. Breast Cancer Res Treat. 2019. https://doi.org/10.1007/s10549-019-05219-7.
Cortazar P, Zhang L, Untch M, et al. Pathologic complete response and long-term clinical benefit in breast cancer: the CTNeoBC pooled analysis. Lancet. 2014. https://doi.org/10.1016/S0140-6736(13)62422-8.
Juhl AA, Christensen S, Zachariae R, Damsgaard TE. Unilateral breast reconstruction after mastectomy–patient satisfaction, aesthetic outcome and quality of life. Acta Oncol. 2017. https://doi.org/10.1080/0284186X.2016.1266087.
Elder EE, Brandberg Y, Bjorklund T, et al. Quality of life and patient satisfaction in breast cancer patients after immediate breast reconstruction: a prospective study. Breast. 2005. https://doi.org/10.1016/j.breast.2004.10.008.
Lim DW, Retrouvey H, Kerrebijn I, et al. Longitudinal study of psychosocial outcomes following surgery in women with unilateral nonhereditary breast cancer. Ann Surg Oncol. 2021. https://doi.org/10.1245/s10434-021-09928-6.
Hoffman DI, Santos PM, Goldbach M, et al. Immediate breast reconstruction for inflammatory breast cancer: trends in use and clinical outcomes 2004–2016. Ann Surg Oncol. 2021. https://doi.org/10.1245/s10434-021-10404-4.
Lim DW, Metcalfe KA, Narod SA. Bilateral mastectomy in women with unilateral breast cancer: a review. JAMA Surg. 2021. https://doi.org/10.1001/jamasurg.2020.664.
Tracy MS, Rosenberg SM, Dominici L, Partridge AH. Contralateral prophylactic mastectomy in women with breast cancer: trends, predictors, and areas for future research. Breast Cancer Res Treat. 2013. https://doi.org/10.1007/s10549-013-2643-6.
Montgomery LL, Tran KN, Heelan MC, et al. Issues of regret in women with contralateral prophylactic mastectomies. Ann Surg Oncol. 1999. https://doi.org/10.1007/s10434-999-0542-1.
Patel SA, Ng M, Nardello SM, Ruth K, Bleicher RJ. Immediate breast reconstruction for women having inflammatory breast cancer in the United States. Cancer Med. 2018. https://doi.org/10.1002/cam4.1546.
Oh DD, Flitcroft K, Brennan ME, Spillane AJ. Patterns and outcomes of breast reconstruction in older women—a systematic review of the literature. Eur J Surg Oncol. 2016. https://doi.org/10.1016/j.esjo.2016.02.010.
Schumacher JR, Taylor LJ, Tucholka JL, et al. Socioeconomic factors associated with post-mastectomy immediate reconstruction in a contemporary cohort of breast cancer survivors. Ann Surg Oncol. 2017. https://doi.org/10.1245/s10434-017-5933-0.
Shippee TP, Kozhimannil KB, Rowan K, Virnig BA. Health insurance coverage and racial disparities in breast reconstruction after mastectomy. Womens Health Issues. 2014. https://doi.org/10.1016/j.whi.2014.03.001.
Chin PL, Andersen JS, Somlo G, Chu DZ, Schwarz RE, Ellenhorn JD. Esthetic reconstruction after mastectomy for inflammatory breast cancer: is it worthwhile? J Am Coll Surg. 2000. https://doi.org/10.1016/s1072-7515(99)00267-7.
Nakhlis F, Regan MM, Chun YS, et al. Patterns of breast reconstruction in patients diagnosed with inflammatory breast cancer: the Dana-Farber Cancer Institute’s Inflammatory Breast Cancer Program experience. Breast J. 2020. https://doi.org/10.1111/tbj.13509.
Mohanty S, Bilimoria KY. Comparing national cancer registries: the National Cancer Data Base (NCDB) and the Surveillance, Epidemiology, and End Results (SEER) program. J Surg Oncol. 2014. https://doi.org/10.1002/jso.23568.
Janz TA, Graboyes EM, Nguyen SA, et al. A comparison of the NCDB and SEER database for researching involving head and neck cancer. Otolaryngol Head Neck Surg. 2019. https://doi.org/10.1177/0194599818792205.
Boffa DJ, Rosen JE, Mallin K, et al. Using the National Cancer Database for outcomes research: a review. JAMA Oncol. 2017. https://doi.org/10.1001/jamaoncol.2016.6905.
Acknowledgment
This work was supported by the Peter Gilgan Center for Research on Women’s Cancers. VG is supported by a Canadian Institutes of Health Research (CIHR) Frederick Banting & Charles Best Canada Graduate Scholarship – Doctoral Research Award. DWL is supported by the CIHR Fellowship and the Canadian Cancer Society Chair in Breast Cancer Research at Women’s College Research Institute (Women’s College Hospital, Toronto, ON, Canada), and is also the recipient of a 2021 Conquer Cancer Young Investigator Award for Invasive Lobular Carcinoma Research supported by Conquer Cancer, the ASCO Foundation, and the Lobular Breast Cancer Alliance. SAN is supported by a Tier 1 Canada Research Chair in Breast Cancer.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Ananya Gopika Nair, Vasily Giannakeas, John L. Semple, Steven A. Narod, and David W. Lim declare they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was presented as a poster presentation at the 23rd Annual Meeting of the American Society of Breast Surgeons (ASBrS), 6–10 April 2022, Las Vegas, NV, USA, and was selected as one of the top 10 posters.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nair, A.G., Giannakeas, V., Semple, J.L. et al. Contemporary Trends in Breast Reconstruction Use and Impact on Survival Among Women with Inflammatory Breast Cancer. Ann Surg Oncol 29, 8072–8082 (2022). https://doi.org/10.1245/s10434-022-12408-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-12408-0