Abstract
Background/Purpose
Malignant small bowel obstruction (mSBO) is a common consequence of advanced malignancies. Surgical consultation is common, however data on the outcomes following an operation are lacking. We investigated a specific operative approach—intestinal bypass—to determine the outcomes associated with this intervention.
Methods
Patients with a preoperative diagnosis of mSBO who underwent intestinal bypass between 2015 and 2021 were included. Isolated colonic obstruction was excluded as was gastric outlet obstruction. Perioperative and postoperative outcomes were measured, including complications, overall survival, return to oral intake, and return to intended oncologic therapy. Patients were additionally grouped as to whether the operation was performed as elective or as inpatient.
Results
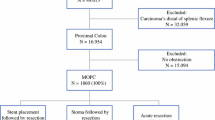
Overall, 55 patients were identified, with a mean age of 61.2 ± 14 years. The most common primary malignancy was colorectal cancer (65.5%) and 80% of patients had a preoperative diagnosis of metastatic disease. Small bowel to colon was the most common bypass procedure (51%). Severe complications occurred in 25.5% of patients with three in-hospital mortalities (5.5%). Survival rates at 30, 90, and 180 days were 91%, 80%, and 62%, respectively. The majority of patients were discharged to home (85.5%) and were tolerating an oral diet (74.6%). Twenty-seven patients (49.1%) returned to some form of oncologic treatment.
Conclusions
Patients with mSBO face a potentially terminal condition. In this study, approximately 75% of patients who underwent intestinal bypass were able to regain the ability to eat, and 49% returned to oncologic therapy. Although retrospective, these data suggest the approach is efficacious for palliation of this difficult sequela of advanced cancer.


Similar content being viewed by others
References
Banting SP, Waters PS, Peacock O, et al. Management of primary and metastatic malignant small bowel obstruction, operate or palliate. A systematic review. ANZ J Surg. 2021;91(3):282–90.
Franke AJ, Iqbal A, Starr JS, Nair RM, George TJ Jr. Management of malignant bowel obstruction associated with GI cancers. J Oncol Pract. 2017;13(7):426–34.
Song Y, Metzger DA, Bruce AN, et al. Surgical outcomes in patients with malignant small bowel obstruction: a national cohort study. Ann Surg. 2022;275(1):e198–205.
Badgwell BD, Smith K, Liu P, Bruera E, Curley SA, Cormier JN. Indicators of surgery and survival in oncology inpatients requiring surgical evaluation for palliation. Support Care Cancer. 2009;17(6):727–34.
Williams LA, Bruera E, Badgwell B. In search of the optimal outcome measure for patients with advanced cancer and gastrointestinal obstruction: a qualitative research study. Ann Surg Oncol. 2020;27(8):2646–52.
Alese OB, Kim S, Chen Z, Owonikoko TK, El-Rayes BF. Management patterns and predictors of mortality among US patients with cancer hospitalized for malignant bowel obstruction. Cancer. 2015;121(11):1772–8.
Badgwell BD, Contreras C, Askew R, Krouse R, Feig B, Cormier JN. Radiographic and clinical factors associated with improved outcomes in advanced cancer patients with bowel obstruction. J Palliat Med. 2011;14(9):990–6.
Tuca A, Guell E, Martinez-Losada E, Codorniu N. Malignant bowel obstruction in advanced cancer patients: epidemiology, management, and factors influencing spontaneous resolution. Cancer Manag Res. 2012;4:159–69.
Chicago Consensus Working G. The Chicago consensus on peritoneal surface malignancies: palliative care considerations. Ann Surg Oncol. 2020;27(6):1798-1804.
Miller P, John PR, Ganai S. How should surgical palliative success be defined? AMA J Ethics. 2021;23(10):E778-782.
Lee KC, Sokas CM, Streid J, et al. Quality indicators in surgical palliative care: a systematic review. J Pain Symptom Manage. 2021;62(3):545–58.
Stacey CL, Pai M, Novisky MA, Radwany SM. Revisiting “awareness contexts” in the 21st century hospital: How fragmented and specialized care shape patients’ Awareness of Dying. Soc Sci Med. 2019;220:212–8.
Groff AC, Colla CH, Lee TH. Days spent at home: a patient-centered goal and outcome. New Eng J Med. 2016;375(17):1610–2.
Shen E, Rozema EJ, Haupt EC, et al. Assessing the concurrent validity of days alive and at home metric. J Am Geriatr Soc. 2021. https://doi.org/10.1111/jgs.17506.
Suskind AM, Zhao S, Boscardin WJ, Smith A, Finlayson E. Time spent away from home in the year following high-risk cancer surgery in older adults. J Am Geriatr Soc. 2020;68(3):505–10.
Chesney TR, Haas B, Coburn NG, et al. Patient-centered time-at-home outcomes in older adults after surgical cancer treatment. JAMA Surg. 2020;155(11):e203754.
Lilley EJ, Scott JW, Goldberg JE, et al. Survival, healthcare utilization, and end-of-life care among older adults with malignancy-associated bowel obstruction: comparative study of surgery, venting gastrostomy, or medical management. Ann Surg. 2018;267(4):692–9.
Pujara D, Chiang YJ, Cormier JN, Bruera E, Badgwell B. Selective approach for patients with advanced malignancy and gastrointestinal obstruction. J Am Coll Surg. 2017;225(1):53–9.
Shaw C, Bassett RL, Fox PS, et al. Palliative venting gastrostomy in patients with malignant bowel obstruction and ascites. Ann Surg Oncol. 2013;20(2):497–505.
Francescutti V, Miller A, Satchidanand Y, Alvarez-Perez A, Dunn KB. Management of bowel obstruction in patients with stage IV cancer: predictors of outcome after surgery. Ann Surg Oncol. 2013;20(3):707–14.
Paul Olson TJ, Pinkerton C, Brasel KJ, Schwarze ML. Palliative surgery for malignant bowel obstruction from carcinomatosis: a systematic review. JAMA Surg. 2014;149(4):383–92.
Wancata LM, Abdelsattar ZM, Suwanabol PA, Campbell DA Jr, Hendren S. Outcomes after surgery for benign and malignant small bowel obstruction. J Gastrointest Surg. 2017;21(2):363–71.
Legendre H, Vanhuyse F, Caroli-Bosc FX, Pector JC. Survival and quality of life after palliative surgery for neoplastic gastrointestinal obstruction. Eur J Surg Oncol. 2001;27(4):364–7.
Englert ZP, White MA, Fitzgerald TL, Vadlamudi A, Zervoudakis G, Zervos EE. Surgical management of malignant bowel obstruction: at what price palliation? Am Surg. 2012;78(6):647–52.
Shariat-Madar B, Jayakrishnan TT, Gamblin TC, Turaga KK. Surgical management of bowel obstruction in patients with peritoneal carcinomatosis. J Surg Oncol. 2014;110(6):666–9.
Ito Y, Fujitani K, Sakamaki K, et al. QOL assessment after palliative surgery for malignant bowel obstruction caused by peritoneal dissemination of gastric cancer: a prospective multicenter observational study. Gastric Cancer. 2021;24(5):1131–9.
Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250(2):187–96.
Lis CG, Gupta D, Lammersfeld CA, Markman M, Vashi PG. Role of nutritional status in predicting quality of life outcomes in cancer: a systematic review of the epidemiological literature. Nutr J. 2012;11:27.
Prost ADJ, Douard R, Malamut G, Mecheri F, Wind P. Small bowel obstruction in patients with a prior history of cancer: predictive findings of malignant origins. World J Surg. 2014;38(2):363–9.
Helyer LK, Law CH, Butler M, Last LD, Smith AJ, Wright FC. Surgery as a bridge to palliative chemotherapy in patients with malignant bowel obstruction from colorectal cancer. Ann Surg Oncol. 2007;14(4):1264–71.
McNiff KK, Caligiuri MA, Davidson NE, et al. Improving goal concordant care among 10 leading academic U.S. Cancer Hospitals: a collaboration of the alliance of dedicated cancer centers. Oncologist. 2021;26(7):533–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Meagan Read, Benjamin D. Powers, Jose M. Pimiento, Danielle Laskowitz, Erin Mihelic, Iman Imanirad, Sophie Dessureault, Seth Felder, and Sean P. Dineen declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Read, M., Powers, B.D., Pimiento, J.M. et al. Management of Malignant Small Bowel Obstruction: Is Intestinal Bypass Effective Palliation?. Ann Surg Oncol 29, 6980–6987 (2022). https://doi.org/10.1245/s10434-022-12204-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-12204-w