Abstract
Background
An integrated approach to skin sparing mastectomy with tissue expander placement followed by radiotherapy and delayed reconstruction was initiated in our institution in 2002. The purpose of this study was to assess the surgical outcomes of this strategy.
Methods
Between September 2002 and August 2013, a total of 384 reconstructions had a tissue expander placed at the time of mastectomy and subsequently underwent radiotherapy. Rates and causes of tissue expander explantation before, during, and after radiotherapy, as well as tumor specific outcomes and reconstruction approaches, were collected.
Results
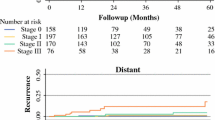
Median follow-up after diagnosis was 5.6 (range 1.3–13.4) years. In the study cohort, 364 patients (94.8%) had stage II–III breast cancer, and 7 patients (1.8%) had locally recurrent disease. The 5-year rates of actuarial locoregional control, disease-free survival, and overall survival were 99.2, 86.1, and 92.4%, respectively. The intended delayed-immediate reconstruction was subsequently completed in 325 of 384 mastectomies (84.6% of the study cohort). Of the remaining 59 tissue expanders, 1 was explanted before radiotherapy, 1 during radiotherapy, and 7 patients (1.8%) were lost to follow-up. Fifty patients (13.0%) required tissue expander explantation after radiation and before their planned final reconstruction, primarily due to cellulitis. Nonetheless, the cumulative rate of completed reconstructions was 89.6%. The median time from placement of the tissue expander until reconstruction was 12 (interquartile range 9–15) months.
Conclusions
Tissue expander placement at skin-sparing mastectomy in patients who require radiotherapy appears to be a viable strategy for combining reconstruction and radiotherapy.



Similar content being viewed by others
References
Cordeiro PG, Pusic AL, Disa JJ, McCormick B, VanZee K. Irradiation after immediate tissue expander/implant breast reconstruction: outcomes, complications aesthetic results, and satisfaction among 156 patients. Plast Reconstr Surg. 2004;113(3):877–81.
Tran NV, Chang DW, Gupta A, Kroll SS, Robb GL. Comparison of immediate and delayed free TRAM flap breast reconstruction in patients receiving postmastectomy radiation therapy. Plast Reconstr Surg. 2001;108:78–82.
Benediktsson K, Perbeck L. Capsular contracture around saline-filled and textured subcutaneously-placed implants in irradiated and non-irradiated breast cancer patients: five years of monitoring of a prospective trial. J Plast Reconstr Aesthet Surg. 2006;59:27–34.
Kronowitz SJ, Hunt KK, Kuerer HM, et al. Delayed-immediate breast reconstruction. Plast Reconstr Surg. 2004;113:1617–28.
Stovall M, Smith SA, Langholz BM, et al. Dose to the contralateral breast from radiotherapy and risk of second primary breast cancer in the Wecare Study. Int J Radiat Oncol Biol Phys. 2008;72:1021–30.
Schechter NR, Strom EA, Perkins GH, et al. Immediate breast reconstruction can impact postmastectomy irradiation. Int J Radiat Oncol Biol Phys. 2005;28:485–94.
Kroll SS, Coffee JA, Jr., Winn RJ, Schusterman MA. A comparison of factors affecting aesthetic outcomes of tram flap breast reconstructions. Plast Reconstr Surg 1995;96:860–4.
Al-Ghazal SK, Sully L, Fallowfield L, Blamey RW. The psychological impact of immediate rather than delayed breast reconstruction. Eur J Surg Oncol 2000;26:17–9.
Rozen WM, Ashton MW, Taylor GI. Defining the role for autologous breast reconstruction after mastectomy: social and oncological implications. Clin Breast Cancer. 2008;8:134–42.
Atisha D, Alderman AK, Lowery JC, Kuhn LE, Davis J, Wilkins EG. Prospective analysis of long-term psychosocial outcomes in breast reconstruction: two-year postoperative results from the Michigan Breast Reconstruction Outcomes Study. Ann Surg. 2008;247:1019–28.
Motwani SB, Strom EA, Schechter NR, et al. The impact of immediate breast reconstruction on the technical delivery of postmastectomy radiotherapy. Int J Radiat Oncol Biol Phys. 2006;66:76–82.
Nahabedian MY, Momen B. The impact of breast reconstruction on the oncologic efficacy of radiation therapy: a retrospective analysis. Ann Plast Surg. 2008;60:244–50.
Buchholz TA, Strom EA, Perkins GH, McNeese MD. Controversies regarding the use of radiation after mastectomy in breast cancer. Oncologist. 2002;7:539–46.
Hughes K, Brown C, Perez V, Ting JW, Rozen WM, Whitaker IS, Korentager R. The effect of radiotherapy on implant-based breast reconstruction in the setting of skin-sparing mastectomy: clinical series and review of complications. Anticancer Res. 2012;32(2):553–7.
Ho A, Cordeiro P, Disa J, et al. Long-term outcomes in breast cancer patients undergoing immediate 2-stage expander/implant reconstruction and postmastectomy radiation. Cancer. 2012;118:2552–9.
Nava MB, Cortinovis U, Ottolenghi J, et al. Skin reducing mastectomy. Plast Reconstr Surg. 2006;118:603–10.
Georgiade GS, Riefkohl R, Cox E, McCarty KS, Seigler HF, Georgiade NG, Snowhite JC. Long-term clinical outcome of immediate reconstruction after mastectomy. Plast Reconstr Surg. 1985;76:415–420.
Rudolph R, Arganese T, Woodward M. The ultrastructure and etiology of chronic radiotherapy damage in human skin. Ann Plast Surg. 1982;9:282–92.
Spear SL, Onyewu C. Staged breast reconstruction with saline-filled implants in the irradiated breast: recent trends and therapeutic implications. Plast Reconstr Surg. 2000;105:930–42.
Ayoub Z, Strom EA, Ovalle V, et al. Radiotherapy after skin-sparing mastectomy and placement of a tissue expander: effectiveness of a coordinated, multidisciplinary approach. American Radium Society 99th Annual Meeting. 2017 May 6–9. Int J Radiat Oncol Biol Phys. 2017:98:E19. Abstract P015.
Cordeiro PG, McCarthy CM. A single surgeon’s 12-year experience with tissue expander/implant breast reconstruction: part I. A prospective analysis of early complications. Plast Reconstr Surg. 2006;118:825–31.
Nahabedian MY, Tsangaris T, Momen B, Manson PN. Infectious complications following breast reconstruction with expanders and implants. Plast Reconstr Surg. 2003;112:467–76.
Armstrong RW, Berkowitz L, Bolding F. Infection following breast reconstruction. Ann Plast Surg. 1989;23:284–8.
Viola GM, Selber JC, Crosby M, et al. Salvaging the infected breast tissue expander: a standardized multidisciplinary approach. Plast Reconstr Surg Glob Open. 2016;4:e732.
Selber JC, Wren JH, Garvey PB, Zhang H, Erickson C, Clemens MW, Butler CE. Critical evaluation of risk factors and early complications in 564 consecutive two-stage implant-based breast reconstructions using acellular dermal matrix at a single center. Plast Reconstr Surg. 2015;136:10–20.
Ho AY, Patel N, Ohri N, et al. Bilateral implant reconstruction does not affect the quality of postmastectomy radiation therapy. Med Dosimetry. 2014;39(1):18–22.
Cordeiro PG, Albornoz CR, McCormick B, Hu Q, VanZee K. The impact of postmastectomy radiotherapy on two-stage implant breast reconstruction: an analysis of long-term surgical outcomes, aesthetic results, and satisfaction over 13 years. Plast Reconstr Surg. 2014;134:588–95.
Cordeiro PG, Albornoz CR, McCormick B, Hudis CA, Hu Q, Heerdt A, Matros E. What is the optimum timing of post-mastectomy radiotherapy in two-stage prosthetic reconstruction: radiation to the tissue expander or permanent implant? Plast Reconstr Surg. 2015;135:1509.
Acknowledgement
Supported in part by Cancer Center Support (Core) Grant CA016672 from the National Institute of Cancer, National Institutes of Health, to The University of Texas MD Anderson Cancer Center.
Disclosure
None of the authors has any commercial interest or conflict to disclose related to the present work.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ayoub, Z., Strom, E.A., Ovalle, V. et al. A 10-Year Experience with Mastectomy and Tissue Expander Placement to Facilitate Subsequent Radiation and Reconstruction. Ann Surg Oncol 24, 2965–2971 (2017). https://doi.org/10.1245/s10434-017-5956-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-017-5956-6