Abstract
Background
This study aimed to review the oncologic outcomes of nerve-sparing radical hysterectomy (NSRH) in cervical cancer and to compare them with those of standard conventional radical hysterectomy (CRH).
Methods
A search of the MEDLINE (Ovid), EMBASE (Ovid), and Cochrane Central Register of Controlled Trials (CENTRAL) databases for studies published to March 3, 2014 was performed using the search term “nerve sparing or radical hysterectomy and cervical cancer.” The main outcome measure was the recurrence rate after NSRH. The hazard ratio for recurrence was used to compare NSRH and CRH.
Results
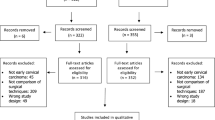
A total of 21 studies reported data on oncologic outcomes of NSRH. The recurrence rate after NSRH was reported to be 0 to 19.6 %. Of the 21 studies, 10 comparing outcomes between NSRH and CRH were assessed for their eligibility to be included in a meta-analysis. However, the scarcity and heterogeneity of effect estimates in these comparison trials precluded performance of a meta-analysis.
Conclusions
The results showed that the evidence addressing the oncologic safety of NSRH over that of CRH in cervical cancer is neither adequate nor statistically relevant. A properly designed, prospective randomized noninferiority trial is needed to assess the oncologic outcomes of NSRH before this surgical approach is adopted as the standard of care for patients with tumors that have unfavorable prognostic features. Until then, NSRH should be considered primarily for patients with small tumors due to the very low risk of parametrial and lymph node involvement, with maximum benefit conferred to the patient from autonomic nerve preservation without any requirement for adjuvant treatment.

Similar content being viewed by others
References
de Kroon CD, Gaarenstroom KN, van Poelgeest MI, Peters AA, Trimbos JB. Nerve sparing in radical surgery for early-stage cervical cancer: yes we should! Int J Gynecol Cancer. 2010;20(11 Suppl 2):S39–41.
Fujii S, Takakura K, Matsumura N, et al. Anatomic identification and functional outcomes of the nerve-sparing Okabayashi radical hysterectomy. Gynecol Oncol. 2007;107:4–13.
Espino-Strebel EE, Luna JT, Domingo EJ. A comparison of the feasibility and safety of nerve-sparing radical hysterectomy with the conventional radical hysterectomy. Int J Gynecol Cancer. 2010;20:1274–83.
Possover M, Stober S, Plaul K, Schneider A. Identification and preservation of the motoric innervation of the bladder in radical hysterectomy type III. Gynecol Oncol. 2000;79:154–7.
Pieterse QD, Ter Kuile MM, Deruiter MC, Trimbos JB, Kenter GG, Maas CP. Vaginal blood flow after radical hysterectomy with and without nerve sparing: a preliminary report. Int J Gynecol Cancer. 2008;18:576–83.
Cibula D, Velechovska P, Slama J, et al. Late morbidity following nerve-sparing radical hysterectomy. Gynecol Oncol. 2010;116:506–11.
Long Y, Yao DS, Pan XW, Ou TY. Clinical efficacy and safety of nerve-sparing radical hysterectomy for cervical cancer: a systematic review and meta-analysis. PLoS One. 2014;9:e94116.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6:e1000100.
Barbic M, Rakar S, Levicnik A, Di Stefano AB. Comparison of nerve content in removed parametrial tissue after classic radical hysterectomy and nerve-sparing radical hysterectomy-histologic evaluation. Eur J Gynaecol Oncol. 2012;33:21–4.
Ceccaroni M, Roviglione G, Spagnolo E, et al. Pelvic dysfunctions and quality of life after nerve-sparing radical hysterectomy: a multicenter comparative study. Anticancer Res. 2012;32:581–8.
Chen C, Li W, Li F, et al. Classical and nerve-sparing radical hysterectomy: an evaluation of the nerve trauma in cardinal ligament. Gynecol Oncol. 2012;125:245–51.
Cibula D, Pinkavova I, Dusek L, et al. Local control after tailored surgical treatment of early cervical cancer. Int J Gynecol Cancer. 2011;21:690–8.
Ditto A, Martinelli F, Mattana F, et al. Class III nerve-sparing radical hysterectomy versus standard class III radical hysterectomy: an observational study. Ann Surg Oncol. 2011;18:3469–78.
Gallotta V, Fanfani F, Scambia G. Minilaparoscopic nerve sparing radical hysterectomy in locally advanced cervical cancer after neoadjuvant radiochemotherapy. Gynecol Oncol. 2014;132(3):758–9.
Hockel M, Horn LC, Hentschel B, Hockel S, Naumann G. Total mesometrial resection: high resolution nerve-sparing radical hysterectomy based on developmentally defined surgical anatomy. Int J Gynecol Cancer. 2003;13:791–803.
Horn LC, Fischer U, Hockel M. Occult tumor cells in surgical specimens from cases of early cervical cancer treated by liposuction-assisted nerve-sparing radical hysterectomy. Int J Gynecol Cancer. 2001;11:159–63.
Lee YS, Chong GO, Lee YH, Hong DG, Cho YL, Park IS. Robot-assisted total preservation of the pelvic autonomic nerve with extended systematic lymphadenectomy as part of nerve-sparing radical hysterectomy for cervical cancer. Int J Gynecol Cancer. 2013;23:1133–8.
Liang Z, Chen Y, Xu H, Li Y, Wang D. Laparoscopic nerve-sparing radical hysterectomy with fascia space dissection technique for cervical cancer: description of technique and outcomes. Gynecol Oncol. 2010;119:202–7.
Magrina JF, Pawlina W, Kho RM, Magtibay PM. Robotic nerve-sparing radical hysterectomy: feasibility and technique. Gynecol Oncol. 2011;121:605–9.
Maneschi F, Ianiri P, Sarno M, Gagliardi F, Panici PB. Nerve-sparing class III-IV radical hysterectomy: urodynamic study and surgical technique. Int J Gynecol Cancer. 2012;22:675–80.
Narducci F, Collinet P, Merlot B, et al. Benefit of robot-assisted laparoscopy in nerve-sparing radical hysterectomy: urinary morbidity in early cervical cancer. Surg Endosc. 2013;27:1237–42.
Papp Z, Csapo Z, Hupuczi P, Mayer A. Nerve-sparing radical hysterectomy for stage IA2-IIB cervical cancer: 5-year survival of 501 consecutive cases. Eur J Gynaecol Oncol. 2006;27:553–60.
Park NY, Chong GO, Hong DG, Cho YL, Park IS, Lee YS. Oncologic results and surgical morbidity of laparoscopic nerve-sparing radical hysterectomy in the treatment of FIGO stage IB cervical cancer: long-term follow-up. Int J Gynecol Cancer. 2011;21:355–62.
Puntambekar SP, Patil A, Joshi SN, Rayate NV, Puntambekar SS, Agarwal GA. Preservation of autonomic nerves in laparoscopic total radical hysterectomy. J Laparoendosc Adv Surg Tech A. 2010;20:813–9.
Sakuragi N, Todo Y, Kudo M, Yamamoto R, Sato T. A systematic nerve-sparing radical hysterectomy technique in invasive cervical cancer for preserving postsurgical bladder function. Int J Gynecol Cancer. 2005;15:389–97.
Tseng CJ, Shen HP, Lin YH, Lee CY, Wei-Cheng Chiu W. A prospective study of nerve-sparing radical hysterectomy for uterine cervical carcinoma in Taiwan. Taiwan J Obstet Gynecol. 2012;51:55–9.
van den Tillaart SA, Kenter GG, Peters AA, Dekker FW, Gaarenstroom KN, Fleuren GJ, Trimbos JB. Nerve-sparing radical hysterectomy: local recurrence rate, feasibility, and safety in cervical cancer patients stage IA to IIA. Int J Gynecol Cancer. 2009;19:39–45.
Wu J, Liu X, Hua K, Hu C, Chen X, Lu X. Effect of nerve-sparing radical hysterectomy on bladder function recovery and quality of life in patients with cervical carcinoma. Int J Gynecol Cancer. 2010;20:905–9.
Gil-Ibanez B, Diaz-Feijoo B, Perez-Benavente A, et al. Nerve sparing technique in robotic-assisted radical hysterectomy: results. Int J Med Robot. 2013;9:339–44.
Ditto A, Martinelli F, Borreani C, et al. Quality of life and sexual, bladder, and intestinal dysfunctions after class III nerve-sparing and class II radical hysterectomies: a questionnaire-based study. Int J Gynecol Cancer. 2009;19:953–7.
Pieterse QD, Kenter GG, Maas CP, de Kroon CD, Creutzberg CL, Trimbos JB, Ter Kuile MM. Self-reported sexual, bowel and bladder function in cervical cancer patients following different treatment modalities: longitudinal prospective cohort study. Int J Gynecol Cancer. 2013;23:1717–25.
Jensen PT, Groenvold M, Klee MC, Thranov I, Petersen MA, Machin D. Longitudinal study of sexual function and vaginal changes after radiotherapy for cervical cancer. Int J Radiat Oncol Biol Phys. 2003;56:937–49.
Frumovitz M, Sun CC, Schover LR, et al. Quality of life and sexual functioning in cervical cancer survivors. J Clin Oncol. 2005;23:7428–36.
Querleu D, Morrow CP. Classification of radical hysterectomy. Lancet Oncol. 2008;9:297–303.
Cibula D, Abu-Rustum NR, Benedetti-Panici P, Kohler C, Raspagliesi F, Querleu D, Morrow CP. New classification system of radical hysterectomy: emphasis on a three-dimensional anatomic template for parametrial resection. Gynecol Oncol. 2011;122:264–8.
Verleye L, Vergote I, Reed N, Ottevanger PB. Quality assurance for radical hysterectomy for cervical cancer: the view of the European Organization for Research and Treatment of Cancer–Gynecological Cancer Group (EORTC-GCG). Ann Oncol. 2009;20:1631–8.
Hintze J. PASS 13. NCSS, LLC, Kaysville, Utah, USA. www.ncss.com. 2014.
Reade CJ, Eiriksson LR, Covens A. Surgery for early-stage cervical cancer: how radical should it be? Gynecol Oncol. 2013;131:222–30.
Acknowledgments
This work was supported by the grant from the Ministry of Health of the Czech Republic (RVO VFN64165), and by Charles University in Prague (UNCE 204024 and PRVOUK-P27/LF1/1).
Conflict of interest
There is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Basaran, D., Dusek, L., Majek, O. et al. Oncological Outcomes of Nerve-Sparing Radical Hysterectomy for Cervical Cancer: A Systematic Review. Ann Surg Oncol 22, 3033–3040 (2015). https://doi.org/10.1245/s10434-015-4377-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-015-4377-7