Abstract
Background
The understanding of epidermal growth factor receptor (EGFR) deregulation in carcinogenesis remains incomplete. We investigated the implications of EGFR gene status and EGFR nuclear translocation in gallbladder carcinoma (GBCA).
Methods
Subcellular localization of EGFR and phosphorylated EGFR (pEGFR) was analyzed by fractional immunoblotting and confocal immunofluorescence in GBCA cell lines. pEGFR binding to iNOS promoter was assessed by chromatin immunoprecipitation with iNOS promoter activity evaluated by luciferase assay. EGFR, pEGFR, and iNOS were immunohistochemically assessable for localization and level in the training set of 104 GBCAs on tissue microarrays, with 76 cases analyzed for EGFR gene by chromogenic in situ hybridization (CISH) and mutant-enriched PCR targeting exons 19 and 21. The prognostic impact of nuclear pEGFR (N-pEGFR) immunoexpression was reaffirmed on whole sections of 58 GBCAs in the test set.
Results
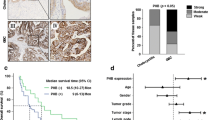
Nuclear expression of EGFR and pEGFR was substantiated in vitro with augmented activity of iNOS promoter elicited by pEGFR binding upon EGF treatment. Despite no mutation, EGFR amplification, identified in 11 cases (15%) by CISH, strongly correlated with cytoplasmic EGFR expression (P < 0.001) but not with disease-specific survival (DSS). Immunoexpression of nuclear EGFR (N-EGFR), cytoplasmic pEGFR, and N-pEGFR was strongly related to that of iNOS (all ≤0.005). N-pEGFR independently predicted worse DSS in both training (P = 0.0468, HR = 2.024) and test sets (P = 0.0223, HR = 5.573).
Conclusions
N-EGFR and N-pEGFR express in GBCA, conferring clinical aggressiveness partly through iNOS transactivation. Lacking response-predicting mutation, EGFR gene status, albeit amplified in 15% of GBCA, is neither related to nuclear EGFR translocation nor prognostically useful.




Similar content being viewed by others
References
Lo HW, Hung MC. Nuclear EGFR signaling network in cancers: linking EGFR pathway to cell cycle progression, nitric oxide pathway and patient survival. Br J Cancer. 2006;94(2):184–8.
Wang SC, Hung MC. Nuclear translocation of the epidermal growth factor receptor family membrane tyrosine kinase receptors. Clin Cancer Res. 2009;15(21):6484–9.
Lo HW, Xia W, Wei Y, Ali-Seyed M, Huang SF, Hung MC. Novel prognostic value of nuclear epidermal growth factor receptor in breast cancer. Cancer Res. 2005;65(1):338–48.
Hadzisejdic I, Mustac E, Jonjic N, Petkovic M, Grahovac B. Nuclear EGFR in ductal invasive breast cancer: correlation with cyclin-D1 and prognosis. Mod Pathol. 2010;23(3):392–403.
Psyrri A, Yu Z, Weinberger PM, et al. Quantitative determination of nuclear and cytoplasmic epidermal growth factor receptor expression in oropharyngeal squamous cell cancer by using automated quantitative analysis. Clin Cancer Res. 2005;11(16):5856–62.
Xia W, Wei Y, Du Y, et al. Nuclear expression of epidermal growth factor receptor is a novel prognostic value in patients with ovarian cancer. Mol Carcinog. 2009;48(7):610–7.
Wang JM, Ko CY, Chen LC, Wang WL, Chang WC. Functional role of NF-IL6beta and its sumoylation and acetylation modifications in promoter activation of cyclooxygenase 2 gene. Nucl Acids Res. 2006;34(1):217–31.
Lo HW, Hsu SC, Ali-Seyed M, et al. Nuclear interaction of EGFR and STAT3 in the activation of the iNOS/NO pathway. Cancer Cell. 2005;7(6):575–89.
Li SH, Li CF, Sung MT, et al. Skp2 is an independent prognosticator of gallbladder carcinoma among p27(Kip1)-interacting cell cycle regulators: an immunohistochemical study of 62 cases by tissue microarray. Mod Pathol. 2007;20(4):497–507.
Reis-Filho JS, Milanezi F, Carvalho S, et al. Metaplastic breast carcinomas exhibit EGFR, but not HER2, gene amplification and overexpression: immunohistochemical and chromogenic in situ hybridization analysis. Breast Cancer Res. 2005;7(6):R1028–35.
Chang JW, Liu HP, Hsieh MH, et al. Increased epidermal growth factor receptor (EGFR) gene copy number is strongly associated with EGFR mutations and adenocarcinoma in non-small cell lung cancers: a chromogenic in situ hybridization study of 182 patients. Lung Cancer. 2008;61(3):328–39.
Asano H, Toyooka S, Tokumo M, et al. Detection of EGFR gene mutation in lung cancer by mutant-enriched polymerase chain reaction assay. Clin Cancer Res. 2006;12(1):43–8.
Fong Y, Lin YS, Liou CP, Li CF, Tzeng CC. Chromosomal imbalances in lung adenocarcinomas with or without mutations in the epidermal growth factor receptor gene. Respirology. 2010;15:700–5.
Wang SC, Hung MC. Cytoplasmic/nuclear shuttling and tumor progression. Ann NY Acad Sci. 2005;1059:11–5.
Hanada N, Lo HW, Day CP, Pan Y, Nakajima Y, Hung MC. Co-regulation of B-Myb expression by E2F1 and EGF receptor. Mol Carcinog. 2006;45(1):10–7.
Hung LY, Tseng JT, Lee YC, et al. Nuclear epidermal growth factor receptor (EGFR) interacts with signal transducer and activator of transcription 5 (STAT5) in activating Aurora-A gene expression. Nucl Acids Res. 2008;36(13):4337–51.
Leone F, Cavalloni G, Pignochino Y, et al. Somatic mutations of epidermal growth factor receptor in bile duct and gallbladder carcinoma. Clin Cancer Res. 2006;12(6):1680–5.
Nakazawa K, Dobashi Y, Suzuki S, Fujii H, Takeda Y, Ooi A. Amplification and overexpression of c-erbB-2, epidermal growth factor receptor, and c-met in biliary tract cancers. J Pathol. 2005;206(3):356–65.
Ooi A, Suzuki S, Nakazawa K, Itakura J, Imoto I, Nakamura H, Dobashi Y. Gene amplification of Myc and its coamplification with ERBB2 and EGFR in gallbladder adenocarcinoma. Anticancer Res. 2009;29(1):19–26.
Pao W, Miller V, Zakowski M, et al. EGF receptor gene mutations are common in lung cancers from “never smokers” and are associated with sensitivity of tumors to gefitinib and erlotinib. Proc Natl Acad Sci U S A. 2004;101(36):13306–11.
Dittmann K, Mayer C, Rodemann HP. Nuclear EGFR as novel therapeutic target: insights into nuclear translocation and function. Strahlenther Onkol. 2010;186(1):1–6.
Kim HP, Yoon YK, Kim JW, et al. Lapatinib, a dual EGFR and HER2 tyrosine kinase inhibitor, downregulates thymidylate synthase by inhibiting the nuclear translocation of EGFR and HER2. PLoS One. 2009;4(6):e5933.
Li C, Iida M, Dunn EF, Ghia AJ, Wheeler DL. Nuclear EGFR contributes to acquired resistance to cetuximab. Oncogene. 2009;28(43):3801–13.
Acknowledgment
This study was supported in part by grants from National Science Council, Taiwan (NSC96-2321-B-182A-001-MY2), Chang Gung Memorial Hospital (CMRPG870753), Chi-Mei Medical Center (CMFHR9935), and Department of Health, Taiwan (DOH99-TD-C-111-004). The authors are grateful to genomic core laboratory (CZRPG880253) and tissue bank (CMRPG870461) of Chang Gung Memorial Hospital-Kaohsiung Medical Center. Immense gratitude is given to Dr. Shiu-Feng F. Huang and Dr. Marc Ladanyi for providing critical technical assistance in EGFR chromogenic in situ hybridization.
Conflicts of interest
The authors have no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Chien-Feng Li, Fu-Ming Fang, and Ju-Ming Wang contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, CF., Fang, FM., Wang, JM. et al. EGFR Nuclear Import in Gallbladder Carcinoma: Nuclear Phosphorylated EGFR Upregulates iNOS Expression and Confers Independent Prognostic Impact. Ann Surg Oncol 19, 443–454 (2012). https://doi.org/10.1245/s10434-011-1942-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-011-1942-6