Abstract
Background
This prospective multicenter sentinel lymph node (SLN) trial investigated whether molecular analysis would improve the detection of SLN metastases and their prognostic value. We report mammaglobin quantitative real-time polymerase chain reaction (qRT-PCR) results and clinical outcome for 547 patients (mean follow-up 7 years).
Methods
Breast cancer patients (excluding stage IV disease or palpable nodes) were enrolled from 1996 to 2005 at 16 institutional review board-approved sites. Alternate 2-mm serial sections of each SLN were examined by hematoxylin and eosin staining with or without immunohistochemistry at multiple levels or blinded and assayed by Taqman qRT-PCR according to previously established thresholds.
Results
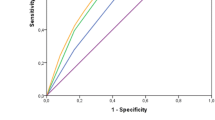
Mammaglobin remains a highly specific (99%), sensitive (97% primary tumor; 82% N1 SLN) marker for breast cancer. Mammaglobin SLN expression was associated with other prognostic factors, was detected in most patients with distant recurrence (48 of 79; 61%), and was associated with decreased recurrence-free survival (log rank P < 0.0001). Molecular analysis upstaged 13% (52 of 394) node-negative (N0) patients who exhibited a significantly lower distant recurrence-free survival compared to node-negative, PCR-negative patients (80 vs. 91%; P < 0.04). N0 patients with PCR-positive SLN were 3.4 times more likely to experience relapse than PCR-negative patients (odds ratio 3.4; 95% confidence interval 1.6–7.1; P = 0.001). However, molecular staging failed to predict most of the N0 patient recurrences (25 of 34) and was not a statistically significant independent predictor of distant recurrence.
Conclusions
To our knowledge, these data are the first to prospectively compare PCR detection of SLN metastases with long-term outcome in breast cancer patients. Molecular staging of SLN detected clinically significant disease missed by standard pathology. Further refinement and optimization of molecular staging is indicated to improve clinical utility.



Similar content being viewed by others
References
Tafra L, Lannin DR, Swanson MS, et al. Multicenter trial of sentinel node biopsy for breast cancer using both technetium sulfur colloid and isosulfan blue dye. Ann Surg. 2001;233:51–9.
Min CJ, Tafra L, Verbanac KM. Identification of superior markers for polymerase chain reaction detection of breast cancer metastases in sentinel lymph nodes. Cancer Res. 1998;58:4581–4.
Watson MA, Fleming TP. Mammaglobin, a mammary-specific member of the uteroglobin gene family, is overexpressed in human breast cancer. Cancer Res. 1996;56:860–5.
Watson MA, Dintzis S, Darrow CM, et al. Mammaglobin expression in primary, metastatic, and occult breast cancer. Cancer Res. 1999;59:3028–31.
Fleming TP, Watson MA. Mammaglobin, a breast-specific gene, and its utility as a marker for breast cancer. Ann N Y Acad Sci. 2000;923:78–89.
Verbanac KM, Min J, Mannie AE, et al. Clinical significance of PCR-detected metastases in sentinel nodes of breast cancer patients: an interim report. J Clin Oncol. 2004;22:9516
Verbanac KM, Min CJ, Mannie A, et al. Multimarker quantitative RT-PCR detects nodal metastases in recurrent patients enrolled in multicenter sentinel node trial. Breast Cancer Res Treat. 2004;88:S12–3.
Backus J, Laughlin T, Wang Y, et al. Identification and characterization of optimal gene expression markers for detection of breast cancer metastasis. J Mol Diagn. 2005;7:327–36.
Reed J, Rosman M, Verbanac KM, et al. Prognostic implications of isolated tumor cells and micrometastases in sentinel nodes of patients with invasive breast cancer: 10-year analysis of patients enrolled in the prospective East Carolina University/Anne Arundel Medical Center Sentinel Node Multicenter Study. J Am Coll Surg. 2009;208:333–40.
Verbanac KM, Mannie A, Min CJ, et al. RT-PCR detection of breast cancer metastases in sentinel lymph nodes of breast cancer patients. Breast Cancer Res Treat. 2002;76:S126.
Cote RJ, Peterson HF, Chaiwun B, et al. Role of immunohistochemical detection of lymph-node metastases in management of breast cancer. International Breast Cancer Study Group. Lancet. 1999;354:896–900.
Singletary SE, Connolly JL. Breast cancer staging: working with the sixth edition of the AJCC staging manual. CA Cancer J Clin. 2006;56:37–47.
Singletary SE, Greene FL, Sobin LH. Classification of isolated tumor cells: clarification of the 6th edition of the American Joint Committee on Cancer staging manual. Cancer. 2003;98:2740–1.
Shivers S, Jakub J, Pendas S, et al. Molecular staging for patients with malignant melanoma. Expert Rev Anticancer Ther. 2007;7:1665–74.
Gimbergues P, Dauplat MM, Cayre A, et al. Correlation between molecular metastases in sentinel lymph nodes of breast cancer patients and St Gallen risk category. Eur J Surg Oncol. 2007;33:16–22.
Bostick PJ, Huynh KT, Sarantou T, et al. Detection of metastases in sentinel lymph nodes of breast cancer patients by multiple-marker RT-PCR. Int J Cancer. 1998;79:645–51.
Masuda N, Tamaki Y, Sakita I, et al. Clinical significance of micrometastases in axillary lymph nodes assessed by reverse transcription-polymerase chain reaction in breast cancer patients. Clin Cancer Res. 2000;6:4176–85.
Viale G, Dell’Orto P, Biasi MO, et al. Comparative evaluation of an extensive histopathologic examination and a real-time reverse-transcription-polymerase chain reaction assay for mammaglobin and cytokeratin 19 on axillary sentinel lymph nodes of breast carcinoma patients. Ann Surg. 2008;247:136–42.
Sakaguchi M, Virmani A, Dudak MW, et al. Clinical relevance of reverse-transcriptase-polymerase chain reaction for the detection of axillary lymph node metastases in breast cancer. Ann Surg Oncol. 2003;10:117–25.
Mikhitarian K, Martin RH, Mitas M, et al. Molecular analysis improves sensitivity of breast sentinel lymph node biopsy: results of a multi-institutional prospective cohort study. Surgery. 2005;138:474–81.
Peppercorn J, Perou CM, Carey LA. Molecular subtypes in breast cancer evaluation and management: divide and conquer. Cancer Invest. 2008;26:1–10.
Albain KS, Paik S, van’t Veer L. Prediction of adjuvant chemotherapy benefit in endocrine responsive, early breast cancer using multigene assays. Breast. 2009;18(Suppl 3):S141–5.
Acknowledgment
This study was supported in part by a career development award (DAMD 7-98-1-8079) and a clinical translation research award from the Department of Defense Breast Cancer Research program (DAMD 17-00-1-0239). We acknowledge a research contract from Ortho Clinical Diagnostics. We acknowledge the technical and collaborative support of Drs. John Backus, Robert Belly, David Atkins, and colleagues, Veridex, LLC. We acknowledge the technical assistance of H. Keith Pittman, BS, Meagan Holcomb, MS, Rith Yim, MS, and Khalief Hamden, MD, East Carolina University. We acknowledge the database management of Kristen Sawyer, MS, CCRA, and Maryann Moreland, BA, Anne Arundel Medical Center; Diane Boyce, RN, Debra Peaden, CCRP, and Anna Broome, BA, East Carolina University. We also acknowledge the support of the East Carolina University/Anne Arundel Medical Center Sentinel Node Study Group Investigators and Sites (Eastern Virginia University/Sentara Norfolk General Hospital, Norfolk, VA; Winchester Hospital, Woburn, MA; Carteret Surgical, Morehead City, NC; Martha Jefferson Hospital, Charlottesville, VA; Alamance Regional Medical Center, Burlington, NC; Memorial Hospital, Martinsville, VA; Carolinas Medical Center, Charlotte, NC; Moore Regional Hospital, Pinehurst, NC; Mercy Hospital, Portland, ME; Breast Care Center of the Blue Ridge, Roanoke, VA; Virginia Beach General Hospital, Virginia Beach, VA; Moses Cone Hospital, Greensboro, NC; Lewis Gale Clinic, Salem, VA; Winchester Medical Center, Winchester, VA).
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
This study is conducted for the ECU/AAMC Sentinel Node Study Group.
Rights and permissions
About this article
Cite this article
Verbanac, K.M., Min, C.J., Mannie, A.E. et al. Long-Term Follow-up Study of a Prospective Multicenter Sentinel Node Trial: Molecular Detection of Breast Cancer Sentinel Node Metastases. Ann Surg Oncol 17 (Suppl 3), 368–377 (2010). https://doi.org/10.1245/s10434-010-1262-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-010-1262-2