Abstract
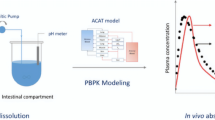
There is an overgrowing emphasis on supersaturating drug delivery systems (SDDS) with increase in number of poorly water-soluble compounds. However, biopharmaceutical performance from these formulations is limited by phase transformation to stable crystalline form due to their high-energy physical form. In the present study, in vitro kinetic solubility in water and dissolution in biorelevant medium integrated with in silico physiologically based pharmacokinetic (PBPK) modeling was used to predict biopharmaceutical performance of SDDS of poorly water-soluble compound, carbamazepine (CBZ). GastroPlus™ with advanced compartmental absorption and transit model was used as a simulation tool for the study. Wherein, the model was developed using physicochemical properties of CBZ and disposition parameters obtained after intravenous administration of CBZ (20 mg/kg) into Sprague-Dawley (SD) rats. Biorelevant medium was selected by screening different dissolution media for their capability to predict oral plasma concentration-time profile of marketed formulation of CBZ. In vivo performance of SDDS was predicted with the developed model and compared to observed plasma concentration-time profile obtained after oral administration of SDDS into SD rats (20 mg/kg). The predictions, with strategy of using kinetic solubility and dissolution in the selected biorelevant medium, were consistent with observed biopharmaceutical performance of SDDS. Additionally, phase transformation of CBZ during gastrointestinal transit of formulations was evaluated and correlated with in vivo dissolution deconvoluted by Loo-Reigelman analysis.








Similar content being viewed by others
Abbreviations
- CBZ:
-
Carbamazepine
- BCS:
-
Biopharmaceutics Classification System
- CBZ-DH:
-
Carbamazepine dihydrate
- GIT:
-
Gastrointestinal tract
- SDDS:
-
Supersaturating drug delivery systems
- CoC:
-
Cocrystal
- ASD:
-
Amorphous solid dispersion
- G+:
-
GastroPlusTM
- PBPK:
-
Physiologically based pharmacokinetic modeling
- ACAT:
-
Advanced compartmental absorption and transit
- LR:
-
Loo-Reigelman
- SAC:
-
Saccharin
- HPMCAS:
-
Hydroxypropyl methylcellulose acetate succinate
- DSC:
-
Differential scanning calorimetry
- PXRD:
-
Powder X-ray diffraction
- CPCSEA:
-
Committee for the Purpose of Control and Supervision of Experiments on Animals
- %PE:
-
% prediction error
- EHC:
-
Enterohepatic circulation
- SEM:
-
Scanning electron microscopy
References
Jones HM, Gardner IB, Watson KJ. Modelling and PBPK simulation in drug discovery. AAPS J. 2009;11(1):155–66.
Kesisoglou F, Chung J, van Asperen J, Heimbach T. Physiologically based absorption modeling to impact biopharmaceutics and formulation strategies in drug development—industry case studies. J Pharm Sci. 2016;105(9):2723–34.
Brouwers J, Brewster ME, Augustijns P. Supersaturating drug delivery systems: the answer to solubility-limited oral bioavailability? J Pharm Sci. 2009;98(8):2549–72.
Raw AS, Furness MS, Gill DS, Adams RC, Holcombe FO, Lawrence XY. Regulatory considerations of pharmaceutical solid polymorphism in abbreviated new drug applications (ANDAs). Adv Drug Deliv Rev. 2004;56(3):397–414.
Bertilsson L. Clinical pharmacokinetics of carbamazepine. Clin Pharmacokinet. 1978;3(2):128–43.
Wilding I, Davis S, Hardy J, Robertson C, John V, Powell M, et al. Relationship between systemic drug absorption and gastrointestinal transit after the simultaneous oral administration of carbamazepine as a controlled-release system and as a suspension of 15N-labelled drug to healthy volunteers. Br J Clin Pharmacol. 1991;32(5):573–9.
Riad LE, Sawchuk RJ. Absorptive clearance of carbamazepine and selected metabolites in rabbit intestine. Pharm Res. 1991;8(8):1050–5.
Kahela P, Aaltonen R, Lewing E, Anttila M, Kristoffersson E. Pharmacokinetics and dissolution of two crystalline forms of carbamazepine. Int J Pharm. 1983;14(1):103–12.
Murphy D, Rodrıguez-Cintrón F, Langevin B, Kelly R, Rodrıguez-Hornedo N. Solution-mediated phase transformation of anhydrous to dihydrate carbamazepine and the effect of lattice disorder. Int J Pharm. 2002;246(1):121–34.
Yates I, Bi V, Farzana I, Deal S, Durig T. Selection of polymeric carriers for carbamazepine amorphous solid dispersions 2014. Available from: http://www.ashland.com/Ashland/Static/Documents/ASI/Pharmaceutical/aaps2014/2014AAPS_Carbamazepine.pdf.
Alshahrani SM, Lu W, Park J-B, Morott JT, Alsulays BB, Majumdar S, et al. Stability-enhanced hot-melt extruded amorphous solid dispersions via combinations of Soluplus® and HPMCAS-HF. AAPS PharmSciTech. 2015;16(4):824–34.
Hickey MB, Peterson ML, Scoppettuolo LA, Morrisette SL, Vetter A, Guzmán H, et al. Performance comparison of a co-crystal of carbamazepine with marketed product. Eur J Pharm Biopharm. 2007;67(1):112–9.
Friščić T, Fábián L, Burley JC, Jones W, Motherwell WS. Exploring cocrystal–cocrystal reactivity via liquid-assisted grinding: the assembling of racemic and dismantling of enantiomeric cocrystals. ChCom. 2006;(48):5009–11.
Vasconcelos T, Sarmento B, Costa P. Solid dispersions as strategy to improve oral bioavailability of poor water soluble drugs. Drug Discov Today. 2007;12(23):1068–75.
Patil SR, Kumar L, Kohli G, Bansal AK. Validated HPLC method for concurrent determination of antipyrine, carbamazepine, furosemide and phenytoin and its application in assessment of drug permeability through Caco-2 cell monolayers. Sci Pharm. 2012;80(1):89–100.
Otsuka K, Shono Y, Dressman J. Coupling biorelevant dissolution methods with physiologically based pharmacokinetic modelling to forecast in-vivo performance of solid oral dosage forms. J Pharm Pharmacol. 2013;65(7):937–52.
Avdeef A. Solubility of sparingly-soluble ionizable drugs. Adv Drug Deliv Rev. 2007;59(7):568–90.
Lee H, Park S-A, Sah H. Surfactant effects upon dissolution patterns of carbamazepine immediate release tablet. Arch Pharm Res. 2005;28(1):120–6.
Kovacevic I, Parojcic J, Homšek I, Tubic-Grozdanis M, Langguth P. Justification of biowaiver for carbamazepine, a low soluble high permeable compound, in solid dosage forms based on IVIVC and gastrointestinal simulation. Mol Pharm. 2008;6(1):40–7.
Madden S, Maggs JL, Park BK. Bioactivation of carbamazepine in the rat in vivo. Evidence for the formation of reactive arene oxide (s). Drug Metab Dispos. 1996;24(4):469–79.
Šehić S, Betz G, Hadžidedić Š, El-Arini SK, Leuenberger H. Investigation of intrinsic dissolution behavior of different carbamazepine samples. Int J Pharm. 2010;386(1):77–90.
Remmel RP, Sinz MW, Cloyd JC. Dose-dependent pharmacokinetics of carbamazepine in rats: determination of the formation clearance of carbamazepine-10, 11-epoxide. Pharm Res. 1990;7(5):513–7.
Wagner C, Jantratid E, Kesisoglou F, Vertzoni M, Reppas C, Dressman JB. Predicting the oral absorption of a poorly soluble, poorly permeable weak base using biorelevant dissolution and transfer model tests coupled with a physiologically based pharmacokinetic model. Eur J Pharm Biopharm. 2012;82(1):127–38.
Loo J, Riegelman S. New method for calculating the intrinsic absorption rate of drugs. J Pharm Sci. 1968;57(6):918–28.
Rodríguez-Hornedo N, Murphy D. Surfactant-facilitated crystallization of dihydrate carbamazepine during dissolution of anhydrous polymorph. J Pharm Sci. 2004;93(2):449–60.
Tian F, Zeitler J, Strachan C, Saville D, Gordon K, Rades T. Characterizing the conversion kinetics of carbamazepine polymorphs to the dihydrate in aqueous suspension using Raman spectroscopy. J Pharm Biomed Anal. 2006;40(2):271–80.
Grzesiak AL, Lang M, Kim K, Matzger AJ. Comparison of the four anhydrous polymorphs of carbamazepine and the crystal structure of form I. J Pharm Sci. 2003;92(11):2260–71.
Alhalaweh A, Roy L, Rodríguez-Hornedo N, Velaga SP. pH-dependent solubility of indomethacin–saccharin and carbamazepine–saccharin cocrystals in aqueous media. Mol Pharm. 2012;9(9):2605–12.
Porter Iii WW, Elie SC, Matzger AJ. Polymorphism in carbamazepine cocrystals. Cryst Growth Des. 2008;8(1):14–6.
Sigma-Aldrich. Product comparision guide: Sodium dodecyl sulfate 2016. Available from: http://www.sigmaaldrich.com/catalog/substance/sodiumdodecylsulfate2883815121311?lang=en®ion=IN&attrlist=Critical micelle concentration.
Gabrielsson J, Weiner D. Non-compartmental analysis. Computational toxicology: Springer; 2012. p. 377–89.
Qureshi SA. Developing discriminatory drug dissolution tests and profiles: some thoughts for consideration on the concept and its interpretation. Dissolut Technol. 2006;13(4):18–23.
Ueda K, Higashi K, Yamamoto K, Moribe K. The effect of HPMCAS functional groups on drug crystallization from the supersaturated state and dissolution improvement. Int J Pharm. 2014;464(1–2):205–13.
AquaSolve™ hypromellose acetate succinate 2015. Available from: https://www.ashland.com/industries/pharmaceutical/oral-solid-dose/aquasolve-hypromellose-acetate-succinate.
Tajarobi F, Larsson A, Matic H, Abrahmsén-Alami S. The influence of crystallization inhibition of HPMC and HPMCAS on model substance dissolution and release in swellable matrix tablets. Eur J Pharm Biopharm. 2011;78(1):125–33.
Homayouni A, Sadeghi F, Varshosaz J, Garekani HA, Nokhodchi A. Promising dissolution enhancement effect of soluplus on crystallized celecoxib obtained through antisolvent precipitation and high pressure homogenization techniques. Colloids Surf B: Biointerfaces. 2014;122:591–600.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(DOC 1315 kb)
Rights and permissions
About this article
Cite this article
Thakore, S.D., Thakur, P.S., Shete, G. et al. Assessment of Biopharmaceutical Performance of Supersaturating Formulations of Carbamazepine in Rats Using Physiologically Based Pharmacokinetic Modeling. AAPS PharmSciTech 20, 179 (2019). https://doi.org/10.1208/s12249-019-1386-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-019-1386-z