Abstract
Objective
Chorioamnionitis is associated with an increased risk of cesarean delivery and uterine atony. We hypothesized that the onset of maternal fever is temporally associated with decreased uterine contractility.
Study Design
Retrospective cohort.
Setting
Academic center.
Patients
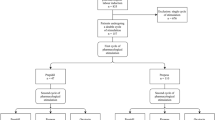
Term participants who developed a fever in the setting of an intrauterine pressure catheter.
Main Outcome Measure
Montevideo units (MVUs) and oxytocin dose at time 0 (first oral temperature ≥38°C) and in the five 1—hour blocks preceding and following T0.
Analysis
Montevideo units relative to the onset of fever. Results were adjusted for oxytocin dose and parity in a mixed-effects model.
Results
One hundred participants were included. Uterine contractility was maintained for 2 hours after the onset of maternal fever but thereafter significantly and steadily declined by an average of 6.9 ± 3.2 MVU/h (P =.03), despite the absence of a parallel decline in oxytocin exposure. Multiparas and nulliparas showed a similar pattern of waning uterine contractility. Patients who delivered vaginally maintained contractility, while those who delivered via cesarean had diminishing contractility (P =.01). The postpartum hemorrhage (PPH) rate (postpartum bleeding requiring treatment) was 32%.
Conclusions
A decline in myometrial contractility occurs 2 hours following the onset of maternal fever. Increased risk of cesarean delivery appears to be directly associated with waning uterine contractility and decreased uterine responsiveness to oxytocin. Clinically, close attention should be given to maintaining adequate uterine contractions following a diagnosis of suspected chorioamnionitis. The likelihood of successful vaginal delivery may decrease over time, and the risk of PPH is clinically significant.
Similar content being viewed by others
References
Newton ER. Chorioamnionitis and intraamniotic infection. Clin Obstet Gynecol. 1993;36(4):795.
Silver RS, Gibbs RS, Castillo M. Effect of amniotic fluid bacteria on the course of labor in nulliparous women at term. Obstet Gynecol. 1986;68(5):587–592.
Satin AJ, Maberry MC, Leveno KJ, Sherman ML, Kline DM. Chorioamnionitis: a harbinger of dystocia. Obstet Gynecol. 1992;79(6):913–915.
Mark SP, Croughan-Minihane MS, Kilpatrick SJ. Chorioamnionitis and uterine function. Obstet Gynecol. 2000;95(6 pt 1):909–912.
Duff P, Sanders R, Gibbs RS. The course of labor in term patients with chorioamnionitis. Am J Obstet Gynecol. 1983;147(4):391–395.
Cierny JT, Unal ER, Flood P, et al. Maternal inflammatory markers and term labor performance. Am J Obstet Gynecol. 2014;210(5):447.e1–e6.
Romero R, Chaemsaithong P, Docheva N, et al. Clinical chorioamnionitis IV: the maternal plasma cytokine profile. J Perinat Med. 2016;44(1):77–98.
Higgins RD, Saade G, Polin RA, et al. Evaluation and management of women and newborns with a maternal diagnosis of chorioamnionitis: summary of a workshop. Obstet Gynecol. 2016;127(3):426e36.
Yancey MK, Schuchat A, Brown LK, Ventura VL, Markenson GR. The accuracy of late antenatal screening cultures in predicting genital group B streptococcal colonization at delivery. Obstet Gynecol. 1996;88(5):811–815.
Dillon HC, Khare S, Gray BM. Group B streptococcal carriage and disease: a 6-year prospective study. J Pediatrics. 1987;110(1):31–36.
Rouse DJ, Landon M, Leveno K, et al. The Maternal-Fetal Medicine cesarean registry: chorioamnionitis at term and its duration—relationship to outcomes. Am J Obstet Gynecol. 2004;191(1):211–216.
Rouse DJ, Leindecker S, Landon M, et al. The MFMU Cesarean Registry: uterine atony after primary cesarean delivery. Am J Obstet Gynecol. 2005;193(3 pt 2):1056–1060.
Wetta LA, Szychowski JM, Seals S, Mancuso MS, Biggio JR, Tita AT. Risk factors for uterine atony/postpartum hemorrhage requiring treatment after vaginal delivery. Am J Obstet Gynecol. 2013;209(1):51.e1–e6.
Spong CY, Berghella V, Wenstrom KD, Mercer BM, Saade GR. Preventing the first cesarean delivery: summary of a joint Eunice Kennedy Shriver National Institute of Child Health and Human Development, Society for Maternal-Fetal Medicine, and American College of Obstetricians and Gynecologists Workshop. Obstet Gynecol. 2012;120(5):1181–1193.
Henry DEM, Cheng YW, Shaffer B, et al. Perinatal outcomes in the setting of active phase arrest of labor. Obstet Gynecol. 2007;112(5):1109–1115.
Arulkumaran S, Gibb DM, Lun KC, Heng SH, Ratnam SS. The effect of parity on uterine activity in labour. Br J Obstet Gynaecol. 1984;91(9):843–848.
Fairlie FM, Phillips GF, Andrews BJ, Calder AA. An analysis of uterine activity in spontaneous labour using a microcomputer. Br J Obstet Gynaecol. 1988;95(1):57–64.
Chaemsaithong P, Madan I, Romero R, et al. Characterization of the myometrial transcriptome in women with an arrest of dilatation during labor. J Perinat Med. 2013;41(6):665–681.
Leroy MJ, Dallot E, Czerkiewicz I, Schmitz T, Breuiller-Fouché M. Inflammation of choriodecidua induces tumor necrosis factor alpha-mediated apoptosis of human myometrial cells. Biol Reprod. 2007;76(5):769–776.
Rauk PN, Friebe-Hoffman U. Interleukin-1β down regulates the oxytocin receptor in cultured uterine smooth muscle cells. Am J Reprod Immunol. 2000;43(2):83–89.
Lirussi F, O’Brien M, Wendremaire M, et al. SAR150640, a selective β3-adrenoceptor agonist, prevents human myometrial remodeling and activation of matrix metalloproteinase in an in vitro model of chorioamnionitis. Br J Pharmacol. 2010;159:1354–1366.
Newton ER, Prihoda TJ, Gibbs RS. Logistic regression analysis of risk factors for intra-amniotic infection. Obstet Gynecol. 1989;73(4):571–575.22.
Soper DE, Mayhall G, Dalton HP. Risk factors for intra-amniotic infection: a prospective epidemiologic study. Am J Obstet Gynecol. 1989;161:562–568.
Lavesson T, Akerman F, Olofsson P. Effects on fetal and maternal temperatures of paracetamol administration during labour: a case-control study. Eur J Obstet Gynecol Reprod Biol. 2013;168(2):138–144.
Laughon SK, Branch DW, Beaver J, Zhang J. Changes in labor patterns over 50 years. Am J Obstet Gynecol. 2012;206(5):419.e1–e9.
Segal S. Labor epidural analgesia and maternal fever. Anesthes Anal. 2010;111(6):1467–1475.
Fusi L, Steer PJ, Maresh MJ, Beard RW. Maternal pyrexia associated with the use of epidural analgesia in labour. Lancet. 1989;1(8649):1250–1252
Goetzl L, Rivers J, Zighelboim I, Wali A, Badell M, Suresh MS. Intrapartum epidural analgesia and maternal temperature regulation. Obstet Gynecol. 2007;109(3):687–9028.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zackler, A., Flood, P., Dajao, R. et al. Suspected Chorioamnionitis and Myometrial Contractility: Mechanisms for Increased Risk of Cesarean Delivery and Postpartum Hemorrhage. Reprod. Sci. 26, 178–183 (2019). https://doi.org/10.1177/1933719118778819
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719118778819