Abstract
The blood–brain barrier (BBB) is a constellation of cells within the neurovascular unit of the brain that perform the barrier function, being also involved in the mechanisms of neuroplasticity. The BBB permeability relies on the efficiency of making contacts between cerebrovascular endothelial cells, mechanisms of transcellular permeability, and crosstalk between endothelial and perivascular cells, specifically, pericytes and astrocytes. In addition, the BBB permeability is a derivative of the entire neurovascular unit’s activity and affects the processes of neuroplasticity, specifically, neurogenesis, which in the adult brain occurs in specialized neurogenic niches wherein the maintenance of the pool of stem and progenitor cells, their renewal, proliferation, and differentiation are controlled by the local microenvironment. The formation of this microenvironment is largely determined by the BBB permeability in microvessels that make up a vascular basis of neurogenic niches. Therefore, functional coupling of neurogenesis and neoangiogenesis is an important component of the mechanisms underlying brain plasticity. The processes of neoangiogenesis and neurogenesis are interrelated through the effects of a wide range of regulatory molecules: growth factors, cytokines, neuro- and gliotransmitters, metabolites. Modern technologies make it possible to develop new protocols for controlling the activity of cells that form a proneurogenic and/or proangiogenic microenvironment. The review summarizes current ideas on the mechanisms of neuroplasticity that involve cerebrovascular endothelial cells, as well as on the possibilities of controlling or optogenetic targeting of perivascular astroglia.

Similar content being viewed by others
Abbreviations
- Ab:
-
amyloid beta
- Ang:
-
аngiopoietin
- AVV:
-
adenovirus vector
- BBB:
-
blood–brain barrier
- BDNF:
-
brain-derived neurotrophic factor
- ChR2:
-
channelrhodopsin-2
- CXCL:
-
chemokine ligand
- Cx43:
-
сonnexin 43
- DLL4:
-
delta-like ligand 4
- EGF:
-
epidermal growth factor
- FGF2:
-
basic fibroblast growth factor 2
- FOX:
-
forkhead box
- GABA:
-
Gamma aminobutyric acid
- GFAP:
-
glial fibrillary acidic protein
- GPR81:
-
G protein-coupled receptor 81
- GSK-3:
-
glycogen synthase kinase-3
- HIF-1:
-
hypoxia-inducible factor 1
- HMGB1:
-
high-mobility group protein B1
- IGF1:
-
insulin-like growth factor 1
- IL1b:
-
interleukin-1
- JAM:
-
junctional adhesion molecule
- LIF:
-
leukemia inhibitory factor
- MCT1:
-
monocarboxylate transporter 1
- NeuroD1:
-
neurogenic differentiation factor 1
- Notch:
-
notch receptors
- NO:
-
nitrogen monoxide
- NPCs:
-
neural progenitor cells
- NSCs:
-
neural stem cells
- NT3:
-
neutrofin 3
- NVU:
-
neurovascular unit
- PCNA:
-
proliferating cell nuclear antigen
- PEDF:
-
pigment epithelium-derived factor
- PlGF-2:
-
placenta growth factor-2
- SCF:
-
stem cell factor
- SGZ:
-
subgranular zone
- Shh:
-
sonic hedgehog
- Stalk-cells:
-
cells expressing the Notch receptor
- SVZ:
-
subventricular zone
- TGF:
-
transforming growth factor
- Tip-cells:
-
cells expressing the DLL4
- VEGF:
-
vascular endothelial growth factor
- Wnt:
-
Wnt signaling protein
REFERENCES
Nikitin VP, Sherstnev VV (2009) The Concept of the Integrative Activities of Neurons and Mechanisms of Neuroplasticity. Neurochem J 3:29–34. https://doi.org/10.1134/S1819712409010048
Riguelme PA, Drapeau E, Doetsch F (2008) Brain micro-ecologies: neural stem cell niches in the adult mammalian brain. Philos Trans R Soc Lond B Biol Sci 363:123–137. https://doi.org/10.1098/rstb.2006.2016
Trentesaux C, Striediner K, Pomerants J, Klein OD (2020) From gut to glutes: The critical role of niche signals in the maintenance and renewal of adult stem cells. Curr Opin Cell Biol 63:88–101. https://doi.org/10.1016/j.ceb.2020.01.004
Abrous DN, Koehl M, Le Moal M (2005) Adult neurogenesis: From precursors to network and physiology. Physiol Rev 85:523–569. https://doi.org/10.1152/physrev.00055.2003
Altman J, Das GD (1965) Autoradiographic and histological evidence of postnatal hippocampal neurogenesis in rats. J Comp Neurol 124:319–335. https://doi.org/10.1002/cne.901240303
Altman J, Das GD (1966) Autoradiographic and histological studies of postnatal neurogenesis. I. A longitudinal investigation of the kinetics, migration and transformation of cells incorporating tritiated thymidine in neonate rats, with special reference to postnatal neurogenesis in some brain regions. J Comp Neurol 126:337–389. https://doi.org/10.1002/cne.901260302
Butti E, Cusimano M, Bacigaluppi M, Martino G (2014) Neurogenic and non-neurogenic functions of endogenous neural stem cells. Front Neurosci 8:92. https://doi.org/10.3389/fnins.2014.00092
Avarez-Buylla A, Lim DA (2004) For the long run: maintaining germinal niches in the adult brain. Neuron 41:683–686. https://doi.org/10.1016/s0896-6273(04)00111-4
Mind GL, Song H (2005) Adult neurogenesis in the mammalian central nervous system. Annu Rev Neurosci 28:223–250. https://doi.org/10.1146/annurev.neuro.28.051804.101459
Mandairon N, Sacquet J, Garcia S, Ravel N, Jourdan F, Didier A (2006) Neurogenic correlates of an olfactory discrimination task in the adult olfactory bulb. Eur J Neurosci 24:3578–3588. https://doi.org/10.1111/j.1460-9568.2006.05235.x
Shors TJ, Townsend DA, Zhao M, Kozorovitskiy Y, Gould E (2002) Neurogenesis may relate to some but not all types of hippocampal-dependent learning. Hippocampus 12:578–584. https://doi.org/10.1002/hipo.10103
Wiltrout C, Lang B, Yan Y, Dempsey RJ, Vemuganti R (2007) Repairing brain after stroke: A review on post-ischemic neurogenesis. Neurochem Int 50:1028–1041. https://pubmed.ncbi.nlm.nih.gov/17531349
Dennis CV, Suh LS, Rodriguez ML, Kril JJ, Sutherland GT (2016) Human adult neurogenesis across the ages: An immunohistochemical study. Neuropathol Appl Neurobiol 42:621–638. https://doi.org/10.1111/nan.12337
Young SZ, Taylor MM, Bordey A (2011) Neurotransmitters couple brain activity to subventricular zone neurogenesis. Eur J Neurosci 33:1123–1132. https://doi.org/10.1111/j.1460-9568.2011.07611.x
Lee JC (1971) Evolutyion in the concept of the blood–brain barrier phenomen. Prog Neuropathol 1:84–145.
Joó F (1996) Endothelial cells of the brain and other organ systems: some similarities and differences. Progress in Neurobiol 48:255–273. https://doi.org/10.1016/0301-0082(95)00046-1
Bradbury MW (1985) The blood–brain barrier. Transport across the cerebral endothelium. Circ Res 57:213–222. https://doi.org/10.1161/01.res.57.2.213
Begley DJ, Brightman MW (2003) Structural and functional aspects of the blood–brain barrier. Prog Drug Res 61:39–78. https://doi.org/10.1007/978-3-0348-8049-7_2
Pardridge WM (1999) Blood–brain barrier biology and methodology. J Neurovirol 5:556–569. https://doi.org/10.3109/13550289909021285
Roh E, Song DK, Kim MS (2016) Emerging role of the brain in the homeostatic regulation of energy and glucose metabolism. Exp Mol Med 48:e216. https://doi.org/10.1038/emm.2016.4
Hawkins BT, Davis TP (2005) The blood–brain barrier/neurovascular unit in health disease. Pharmacol Rev 57:173–185. https://doi.org/10.1124/pr.57.2.4
Rubin LL, Staddon JM (1999) The cell biology of the blood–brain barrier. Ann Rev Neurosci 22:11–28. https://doi.org/10.1146/annurev.neuro.22.1.11
Abbott NJ, Patabendige AA, Dolman DE, Yusof SR, Begley DJ. (2010) Structure and function of the blood–brain barrier. Neurobiol Dis 37(1):13–25. https://doi.org/10.1016/j.nbd.2009.07.030
Ballabh P, Braun A, Nedergaard M (2004) The blood–brain barrier: an overview: structure, regulation, and clinical implications. Neurobiol Dis 16(1):1–13. https://pubmed.ncbi.nlm.nih.gov/15207256/
Salmina AB, Morgun AV, Kuvacheva NV, Komleva YuK, Pojilenkova EA, Kutischeva IA, Trufanova LV, Taranushenko TE, Martyinova GP (2013) Intercellular communications in the development the blood–brain barrier. Pediatriya Zhurn Im GN Speranskogo 92:155–159. https://www.elibrary.ru/item.asp?id=19394048
Palmer TD, Willhoite AR, Gage FH (2000) Vascular niche for adult hippocampal neurogenesis. J Comp Neurol 425:479–494. https://doi.org/10.1002/1096-9861(20001002)425:4<479::aid-cne2>3.0.co;2-3
Apple DM, Kokovay E (2017) Vascular niche contribution to age-associate neural stem cell dysfunction. Am J Physiol August 11:896–902. https://journals.physiology.org/doi/pdf/10.1152/ajpheart.00154.2017
Alvarez-Buylla A, Garcia-Verdugo JM (2002) Neurogenesis in adult subventricular zone. J Neurosci 22:629–634. https://doi.org/10.1523/JNEUROSCI.22-03-00629.2002
Doetsch F (2003) A niche for adult neural stem cell niche. Curr Opin Genetic Develop 13:543–550. https://doi.org/10.1016/j.gde.2003.08.012
Salmina AB, Morgun AV, Kuvacheva NV, Lopatina OL, Komleva YK, Malinovskaya NA, Pozhilenkova EA (2014) Establishment of neurogenic microenvironment in the neurovascular unit: the connexin 43 story. Rev Neurosci 25:97–111. https://doi.org/10.1515/revneuro-2013-0044
Pozhilenkova EA, Lopatina OL, Komleva YK, Salmin VV, Salmina AB (2017) Blood–brain barrier-supported neurogenesis in healthy and diseased brain. Rev Neurosci 28:397–415. https://doi.org/10.1515/revneuro-2016-0071
Conover JC, Notti RQ (2008) The neural stem cell niche. Cell Tissue Res 331:211–224. https://doi.org/10.1007/s00441-007-0503-6
Jin K, Zhu Y, Sun Y, Mao XO, Xie L, Greenberg DA (2002) Vascular endothelial growth factor (VEGF) stimulates neurogenesis in vitro and in vivo. Proc Natl Acad Sci USA 99:11946–11950. https://doi.org/10.1073/pnas.182296499
Doetsch F, Petreanu L, Caille I, Garcia-Verdugo JM, Alvarez-Buylla A (2002) EGF converts transit-amplifying neurogenic precursors in the adult brain into multipotent stem cells. Neuron 36:1021–1034. https://doi.org/10.1016/s0896-6273(02)01133-9
Kilpatrick TJ, Barlett PF (1995) Cloned multipotential precursors from the mouse cerebrum require FGF-2, whereas glial restricted precursors are stimulated with either FGF-2 or EGF. J Neurosci 15:3653–3661. https://doi.org/10.1523/JNEUROSCI.15-05-03653.1995
Cheng A, Wang S, Cai J, Rao MS, Mattson MP (2003) Nitric oxide act in a positive feedback loop with BDNF to regulate neural progenitor cell proliferation and differentiation in the mammalian brain. Dev Biol 258:319–333. https://doi.org/10.1016/s0012-1606(03)00120-9
Andreu-Agulló C, Morante-Redolat JM, Delgado AC, Fariñas I (2009) Vascular niche factor PEDF modulates Notch-dependent stemness in the adult subependymal zone. Nat Neurosci 12:1514–1523. https://doi.org/10.1038/nn.2437
Ramírez-Castillejo C, Sánchez-Sánchez F, Andreu-Agulló C, Ferrón SR, Aroca-Aguilar JD, Sánchez P, Mira H, Escribano J, Fariñas I (2006) Pigment epithelium-derived factor is a niche signal for neural stem cell renewal. Nat Neuroscience 9:331–339. https://doi.org/10.1038/nn1657
Zhang J, Jiao J (2015) Molecular Biomarkers for Embryonic and Adult Neural Stem Cell and Neurogenesis. Biomed Res Int 2015:727542. https://doi.org/10.1155/2015/727542
Bátiz LF, Castro MA, Burgos PV, Velásquez ZD, Muñoz RI, Lafourcade CA, Troncoso-Escudero P, Wyneken U (2016) Exosomes as Novel Regulators of Adult Neurogenic Niches. Front Cell Neurosci 9:501. https://doi.org/10.3389/fncel.2015.00501
Delgado AC, Ferrón SR, Vicente D, Porlan E, Perez-Villalba A, Trujillo CM, D’Ocón P, Fariñas I (2014) Endothelial NT-3 Delivered by Vasculature and CSF Promotes Quiescence of Subependymal Neural Stem Cells through Nitric Oxide Induction. Neuron 83:572–585. https://doi.org/10.1016/j.neuron.2014.06.015
Gómez-Gaviro MV, Scott CE, Sesay AK, Matheu A, Booth S, Galichet C, Lovell-Badge R (2012) Betacellulin promotes cell proliferation in the neural stem cell niche and stimulates neurogenesis. Proc Natl Acad Sci U S A 109:1317–1322. https://doi.org/10.1073/pnas.1016199109
Crouch EE, Liu C, Silva-Vargas V, Doetsch F (2015) Regional and stage-specific effects of prospectively purified vascular cells on the adult V-SVZ neural stem cell lineage. J Neurosci 35:4528–4539. https://doi.org/10.1523/JNEUROSCI.1188-14.2015
Chong CM, Ai N, Ke M, Tan Y, Huang Z, Li Y, Lu JH, Ge W, Su H (2018) Roles of Nitric Oxide Synthase Isoforms in Neurogenesis. Mol Neurobiol 55:2645–2652. https://doi.org/10.1007/s12035-017-0513-7
Goldberg JS, Hirschi KK (2012) A Vascular perspective on neurogenesis. In: Bonfanti L (ed) Neural Stem Cells—New Perspectives. https://www.intechopen.com/chapters/44266
Lamus F, Martín C, Carnicero E, Moro JA, Fernández JMF, Mano A, Gato Á, Alonso MI (2020) FGF2/EGF contributes to brain neuroepithelial precursor proliferation and neurogenesis in rat embryos: the involvement of embryonic cerebrospinal fluid. Dev Dyn 249:141–153. https://doi.org/10.1002/dvdy.135
Zheng W, Nowakowski RS, Vaccarino FM (2004) Fibroblast growth factor 2 is required for maintaining the neural stem cell pool in the mouse brain subventricular zone. Dev Neurosci 26:181–196. https://doi.org/10.1159/000082136
Killer K, Le O, Beauséjour C (2021) The Intracerebroventricular Injection of Murine Mesenchymal Stromal Cells Engineered to Secrete Epidermal Growth Factor Does Not Prevent Loss of Neurogenesis in Irradiated Mice. Radiat Res 196:315–322. https://doi.org/10.1667/RADE-21-00017.1
Yang C, Qi Y, Sun Z (2021) The Role of Sonic Hedgehog Pathway in the Development of the Central Nervous System and Aging-Related Neurodegenerative Diseases. Front Mol Biosci 8:711710. https://doi.org/10.3389/fmolb.2021.711710
Kandasamy M, Lehner B, Kraus S, Sander PR, Marschallinger J, Rivera FJ, Trümbach D, Ueberham U, Reitsamer HA, Strauss O, Bogdahn U, Couillard-Despres S, Aigner L (2014) TGF-beta signalling in the adult neurogenic niche promotes stem cell quiescence as well as generation of new neurons. J Cell Mol Med 18:1444–1459. https://doi.org/10.1111/jcmm.12298
Dumont CM, Piselli JM, Kazi N, Bowman E, Li G, Linhardt RJ, Temple S, Dai G, Thompson DM (2017) Factors Released from Endothelial Cells Exposed to Flow Impact Adhesion, Proliferation, and Fate Choice in the Adult Neural Stem Cell Lineage. Stem Cells Dev 26:1199–1213. https://doi.org/10.1089/scd.2016.0350
Qiu Z, Yang J, Deng G, Li D, Zhang S (2021) Angiopoietin-like 4 promotes angiogenesis and neurogenesis in a mouse model of acute ischemic stroke. Brain Res Bull 168:156–164. https://doi.org/10.1016/j.brainresbull.2020.12.023
Obernier K, Alvarez-Buylla A (2019) Neural stem cells: origin, heterogeneity and regulation in the adult mammalian brain. Development 146:dev156059. https://doi.org/10.1242/dev.156059
Li F, Chong ZZ, Maiese K (2006) Winding through the WNT pathway during cellular development and demise. Histol Histopathol 21:103–124. https://doi.org/10.14670/HH-21.103
Young JK, Heinbockel T, Gondré-Lewis MC (2013) Astrocyte fatty acid binding protein-7 is a marker for neurogenic niches in the rat hippocampus. Hippocampus 23:1476–1483. https://doi.org/10.1002/hipo.22200
Salmina AB, Malinovskaya NA, Kuvacheva NV, Morgun AV, Khilazheva ED, Gorina YaV, Pozhilenkova EA, Frolova OV (2014) Connexin and Pannexin Transport Systems in Cells of Neurovascular Unit of the Brain. Neurochem J 31:122–133. https://doi.org/10.7868/s1027813314020095
Heneka MT, Rodríguez JJ, Verkhratsky A (2010) Neuroglia in neurodegeneration. Brain Res Rev 63:189–211. https://doi.org/10.1016/j.brainresrev.2009.11.004
Caesar K, Hashemi P, Douhou A, Bonvento G, Boutelle M, Walls AB, Lauritzen M (2008) Glutamate receptor-dependent increments in lactate, glucose and oxygen metabolism evoked in rat cerebellum in vivo. J Physiol 586(5):1337–1349. https://pubmed.ncbi.nlm.nih.gov/18187464/
Horvat A, Muhic M, Smolic T, Begic E, Zorec R, Kreft M, Vardjan N (2021) Ca2+ as the prime trigger of aerobic glycolysis in astrocytes. Cell Calcium 95: 102368. https://www.sciencedirect.com/science/article/pii/S0143416021000221
Siegenthaler JA, Sohet F, Daneman R (2013) 'Sealing off the CNS': cellular and molecular regulation of blood–brain barriergenesis. Curr Opin Neurobiol 23:1057–1064. https://doi.org/10.1016/j.conb.2013.06.006
Mizee MR, Wooldrik D, Lakeman KA, van het Hof B, Drexhage JA, Geerts D, Bugiani M, Aronica E, Mebius RE, Prat A, de Vries HE, Reijerkerk A (2013) Retinoic acid induces blood–brain barrier development. J Neurosci 33:1660–1671. https://doi.org/10.1523/JNEUROSCI.1338-12.2013
Ferrara N, Gerber HP, LeCouter J (2003) The biology of VEGF and its receptors. Nat Med 9:669–676. https://doi.org/10.1038/nm0603-669
You T, Bi Y, J Li, Zhang M, Chen X, Zhang K, Li J (2017) IL-17 induces reactive astrocytes and up-regulation of vascular endothelial growth factor (VEGF) through JAK/STAT signaling. Scient Rep7: 41779. https://www.nature.com/articles/srep41779
Choi SH, Kim HJ, Cho HJ, Park SD, Lee NE, Hwang SH, Rhim H, Kim HC, Cho IH, Nah SY (2019) Gintonin-mediated release of astrocytic vascular endothelial growth factor protect cortical astrocytes from hypoxia-induced cell damages. J Ginseng Res 43(2):305–311. https://khu.elsevierpure.com/en/publications/gintonin-mediated-release-of-astrocytic-vascular-endothelial-grow
Shen Y, Gu J, Liu Z, Xu C, Qian S, Zhang X, Zhou B, Guan Q, Sun Y, Wang Y, Jin X (2018) Inhibition of HIF-1α Reduced Blood Brain Barrier Damage by Regulating MMP-2 and VEGF During Acute Cerebral Ischemia. Front Cell Neurosci 12:288. https://www.frontiersin.org/articles/10.3389/fncel.2018.00288/full
Liu J, Li J (2022) Astrocytes Protect Human Brain Microvascular Endothelial Cells from Hypoxia Injury by Regulating VEGF Expression. J Healthcare Engineer 2022:1884959. https://www.hindawi.com/journals/jhe/2022/1884959/
Baumann J, Tsao CC, Huang SF, Gassmann M, Ogunshola OO (2021) Astrocyte-specific hypoxia-inducible factor 1 (HIF-1) does not disrupt the endothelial barrier during hypoxia in vitro. Fluids and Barriers of the CNS 18:13. https://fluidsbarrierscns.biomedcentral.com/articles/10.1186/s12987-021-00247-2
Jin K, Zhu Y, Sun Y, Mao X, Xie L, Greenberg DA (2002) Vascular endothelial growth factor (VEGF) stimulates neurogenesis in vitro and in vivo. Biol Sci 99(18):11946–11950. https://www.pnas.org/doi/10.1073/pnas.182296499
Udo H, Yoshida Y, Kino T, Ohnuki K, Mizunoya W, Mukuda T, Sugiyama H (2008) Enhanced Adult Neurogenesis and Angiogenesis and Altered Affective Behaviors in Mice Overexpressing Vascular Endothelial Growth Factor 120. J Neurosci 28(53):14522–14536. https://sci-hub.wf/10.1523/JNEUROSCI.3673-08.2008
Komleva Yu, Salmina AB, Prokopenko CV, Shestakova LA, Petrova MM, Malinovskaya NA, Lopatina OL (2013) Changes in structural and functional plasticity of the brain induced by environmental enrichment. Ann Rus Acad Med Sci 6:39–48. https://www.elibrary.ru/item.asp?id=19139669
Hummel FC, Cohen LG (2005) Drivers of brain plasticipy. Curr Opin Neurol 18:667– 674. https://doi.org/10.1097/01.wco.0000189876.37475.42
Lin R, Cai J, Nathan C, Wei X, Schleidt S, Rosenwasser R, Iacovitti L (2015) Neurogenesis is enchanced by stroke in multiple new stem cell niches along the ventricular system at sites of high BBB permeability. Neurobiol Dis 74:229–239. https://doi.org/10.1016/j.nbd.2014.11.016
Font MA, Arboix A, Krupinski J (2010) Angiogenesis, neurogenesis and neuroplasticity in ischemic stroke. Curr Cardiol Rev 6:238–244. https://doi.org/10.2174/157340310791658802
Biron KE, Dickstein DL, Gopaul R, Jefferies WA (2011) Amyloid triggers extensive cerebral angiogenesis causing blood brain barrier permeability and hypervascularity in Alzheimer’s disease. PLoS One 6:e23789. https://doi.org/10.1371/journal.pone.0023789
Palma-Tortosa S, García-Culebras A, Moraga A, Hurtado O, Ruiz-Peres A, Duran-Laforet V, Parra J, Cuartero MI, Pradillo JM, Moro MA, Lizasoain I (2017) Specific Features of SVZ Neurogenesis After Cortical Ischemia: a Longitudinal Study. Sci Rep 7: 16343. https://doi.org/10.1038/s41598-017-16109-7
Deshapande SS, Malik S, Conforti P, Lin J-di, Chu Yu-H, Nath S, Greulich F, Dumbach M-A, Uhlenhaut NH, Shachtrup C (2021) P75 neurotrophin receptor controls subventricular zone neural stem cell after stroke. Cell and Tissue Res 387: 415–431. https://link.springer.com/article/10.1007/s00441-021-03539-z
Liang H, Zhao H, Gleichman A, Carmichael ST (2019) Region-specific and activity-dependent regulation of SVZ neurogenesis and recovery after stroke. Biol Sci 116(27):13621–13630. https://doi.org/10.1073/pnas.1811825116
Mahoney ER, Dumitrescu L, Moore AM, Cambronero FE, De Jager PL, Koran MEI, Petyuk VA, Robinson RAS, Goyal S, Schneider JA, Bennett DA, Jefferson AL, Hohman TJ (2021) Brain expression of the vascular endothelial growth factor gene family in cognitive aging and alzheimer's disease. Mol Psychiatry 26:888–896. https://doi.org/10.1038/s41380-019-0458-5
Zhu H, Zhang Y, Zhong Yi, Ye Y, Hu X, Gu L, Xiong X (2021) Inflammation-Mediated Angiogenesis in Ischemic Stroke. Front Cell Neurosci 15:652647. https://www.frontiersin.org/articles/10.3389/fncel.2021.652647/full
Lin R, Cai J, Nathan C, Wei X, Schleidt S, Rosenwasser R, Iacovitti L (2015) Neurogenesis is enhanced by stroke in multiple new stem cell niches along the ventricular system at sites of high BBB permeability. Neurobiol Disease 74:229–239. https://doi.org/10.1016/j.nbd.2014.11.016
Lin R, Cai J, Kenyon L, Iozzo R, Rosenwasser R, Iacovitti L (2019) Systemic Factors Trigger Vasculature Cells to Drive Notch Signaling and Neurogenesis in Neural Stem Cells in the Adult Brain. Stem Cells 37:395–406. https://doi.org/10.1002/stem.2947
Rodrigues JJ, Jones VC, Verkhratsky A (2009) Impaired cell proliferation in the subventricular zone in an Alzheimer’s disease model. Neuroreport 20(10):907–912. https://pubmed.ncbi.nlm.nih.gov/19494789/
Demars M, Hu Y-S, Gadadhar A, Lazarov O (2010) Impaired neurogenesis is an early event in the etiology of familial Alzheimer’s disease in transgenic mice. J Neurosci Res 88(10):2103–2117. https://pubmed.ncbi.nlm.nih.gov/20209626/
Gerozissis K (2008) Brain insulin, energy and glucose homeostasis; genes, environment and metabolic pathologies. Eur J Pharmacol 585:38–49. https://doi.org/10.1016/j.ejphar.2008.01.050
Lin R, Cal J, Kenyon L, Iozzo R, Rosenwasser R, Iacovitti L (2019) Systemic Factors Trigger Vasculature Cells to Drive Notch Signaling and Neurogenesis in Neural Stem Cells in the Adult Brain. Stem Cells 37:395–406. https://doi.org/10.1002/stem.2947
Garcia-Caceres C, Quarta C, Varela L, Gao Y, Gruber T, Legutko B, Jastroch M, Johansson P, Ninkovic J, Yi C-X, Le Thuc O, Szigeti-Buck K, Cai W, Meyer CW, Pfluger PT, Fernandez A, Luquet S, Woods SC, Torres-Aleman I, Kahn CR, Gotz M, Horvanth TL, Tschop MH (2016) Astrocytic Insulin Signaling Couples Brain Glucose Uptake with Nutrient Availability. Cell 166(4):867–880. https://pubmed.ncbi.nlm.nih.gov/27518562/
Salmina AB, Yauzina NA, Kuvacheva NV, Petrova MM, Taranushenko TY, Malinovskaya NA, Lopatina OL, Morgun AV, Pozhilenkova YA, Okuneva OS, Morozova GA, Prokopenko SV (2013) Insulin and insulin resistance: new molecule markers and target molecule for the diagnosis and therapy of disease of central nervous system. Bull Siber Med 12:104–118. https://doi.org/10.20538/1682-0363-2013-5-104-118
Gorina YaV, Salmina AB, Kuvacheva NV, Komleva YuK, Fedyukovich LV, Uspenskaya YuA, Morozova GA, Demko IV, Petrova MM (2014) Neuroinflammation and insulin resistance in Alzheimer’s disease. Siber Med Rev 4:11–19. https://www.elibrary.ru/query_results.asp
Gorina YaV, Lopatina OL, Komleva YuK, Chernikh AI, Salmina AB (2018) The role neuroinflammation in cognitive functions and social interaction in mice with age-dependent neurodegeneration. Ann Clin Exp Neurol 12:27–32. https://www.elibrary.ru/item.asp?id=42236418&
Gorina YaV, Osipova ED, Morgun AV, Malinovskaya NA, Komleva YuK, Lopatina OL, Salmina AB (2020) Aberrant angiogenesis in brain tissue in experimental Alzheimer’s disease. Bull Siber Med 19:46–52. https://doi.org/10.20538/1682-0363-2020-4-46-52
Hockeimer W (2021) Non-spatial Information Encoding in Hippocampal CA1. Theses and Dissertation, Electronic (ETDs). https://jscholarship.library.jhu.edu/handle/1774.2/63959
Morgun AV, Osipova ED, Boytsova EB, Lopatina OL, Gorina YaV, Pozhilenkova EA, Salmina AB (2020) Vascular component of neuroinflammation in experimental Alzheimer’s disease in mice. Tsitologiya 62:16–23. https://doi.org/10.31857/s0041377120010058
Gorina YaV, Osipova ED, Morgun AV, Boytsova EB, Lopatina OL, Salmina AB (2021) Assessment of the RAGE in cells blood–brain barrier in experiment Alzheimer’s disease. Tsitologiya 63:176–183. https://doi.org/10.1134/S1990519X21030032
Morgun AV, Osipova ED, Boytsova EB, Shuvaev YuN, Komleva YuK, Trufanova LV, Vais EF, Salmina AB (2019) Astroglia-mediated regulation of cell development in the model of neurogenic niche in vitro treated with Aβ1-42. Biomed Khim 65:366–373. https://doi.org/10.18097/pbmc20196505366
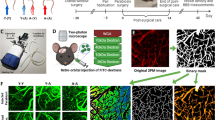
Khilazheva ED, Morgun AV, Boytsova EB, Mosiagina AI, Shuvaev AN, Malinovskaya NA, Uspenskaya YuA, Pozhilenkova EA, Salmina AB (2021) Features of the in vitro expression profile of hippocampal neurogenic niche cells during optogenetic stimulation. Biomed Khim 67:34–41. https://doi.org/10.18097/pbmc20216701034
Khilazheva ED, Pisareva NB, Morgun AV, Boytsova EB, Taranushenko TE, Frolova OV, Salmina AB (2017) Activation of lactate receptors GPR81 stimulates mitochondrial biogenesis in celebral microvessel endothelial cell. Ann Clin Exp Neurol 11:34–39. https://doi.org/10.18454/ACEN.2017.1.6155
Funding
The writing of this review was supported by the grant of the President of the Russian Federation for the state support of leading scientific schools (NSh-2547.2020.7).
Author information
Authors and Affiliations
Contributions
Analysis of literature data, writing the manuscript (E.A.T.); writing and editing the manuscript (Ya.V.G., E.D.Kh., E.B.B., A.I.M., A.V.M., A.N.Sh.); editing the manuscript, preparing the illustration (N.A.M., Yu.K.K., Yu.A.U.); conceptualization, analysis of literature data, in-process manuscript correction (A.B.S.).
Corresponding author
Ethics declarations
CONFLICT OF INTEREST
The authors declare that they have no conflict of interest related with the publication of this article.
Additional information
Translated by A. Polyanovsky
Russian Text © The Author(s), 2022, published in Rossiiskii Fiziologicheskii Zhurnal imeni I.M. Sechenova, 2022, Vol. 58, No. 3, pp. 109–115https://doi.org/10.31857/S0869813922050119.
Rights and permissions
About this article
Cite this article
Teplyashina, E.A., Gorina, Y.V., Khilazheva, E.D. et al. Cells of Cerebrovascular Endothelium and Perivascular Astroglia in the Regulation of Neurogenesis. J Evol Biochem Phys 58, 728–741 (2022). https://doi.org/10.1134/S0022093022030097
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0022093022030097