Abstract
OBJECTIVE: To describe the medical care use and costs associated with migraine.
DESIGN: Retrospective case-control design in which migraine case status was ascertained via validated telephone interview and linked with comprehensive claims data. Unadjusted and adjusted use and cost differences by migraine status were evaluated using exponential score tests and generalized estimating equations.
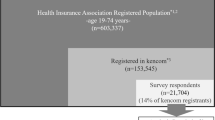
SETTING AND PATIENTS: We interviewed 8,579 individuals to identify migraine cases (N=1,265) and a random sample of nonmigraine controls (N=1,178) among eligible health plan enrollees aged 18 to 55.
MEASURES: Survey responses were used to categorize individuals meeting the International Headache Society’s diagnostic criteria for migraine with or without aura as migraine cases and to collect information on comorbid psychiatric symptoms. Claims data were used to compile annual medical and pharmaceutical use and costs, presence of migraine diagnosis, and other diagnosed comorbidities.
RESULTS: Interview-ascertained migraine cases used more outpatient visits (9.1 vs 6.8; P<.01), were more likely to be seen in the emergency department (20.7% vs 17.6%; P<.05), and were admitted to the hospital more (4.5% vs 2.8%; P<.05) compared to nonmigraine controls. Cases incurred significantly higher medical care costs ($2,761 vs $2,064; P<.01). Multivariable model results indicate that much of this increase in costs is due to the presence of major depressive symptoms as well as other diagnosed comorbidities that are more common among those with migraine.
CONCLUSIONS: By combining validated telephone survey information to identify migraine cases and controls with comprehensive claims data, we found migraine cases incur higher medical care costs compared to controls. These increased costs are associated with the presence of psychiatric symptoms and other comorbidities.
Similar content being viewed by others
References
Stewart WF, Lipton RB, Liberman J. Variation in migraine prevalence by race. Neurology. 1996;47:52–9.
Lipton RB, Stewart WF, Diamond S, Diamond ML, Reed M. Prevalence and burden of migraine in the United States: data from the American Migraine Study II. Headache. 2001;41:646–57.
Lipton RB, Stewart WF, Kolodner KB, Liberman JN. Epidemiology and patterns of health care use for migraine in the United States. Headache. 1999;39:65–6.
Hu XH, Markson LE, Lipton RB, Stewart WF, Berger ML. Burden of migraine in the United States: disability and economic costs. Arch Intern Med. 1999;159:813–8.
Stang PE, Osterhaus JT, Celentano DD. Migraine. Patterns of healthcare use. Neurology. 1994;44(6 suppl 4):S47-S55.
Kolodner K, Lipton RB, Elston Lafata J, et al. Pharmacy and medical claims data identified migraine sufferers with high specificity but modest sensitivity. J Clin Epidemiol. 2004. In press.
Lipton RB, Diamond S, Reed M, Diamond ML, Stewart WF. Migraine diagnosis and treatment: results from the American Migraine Study II. Headache. 2001;47:638–45.
Celentano DD, Stewart WF, Lipton RB, Reed ML. Medication use and disability among migraineurs: a national probability sample survey. Headache. 1992;32:223–8.
Stewart WF, Lipton RB, Whyte J, et al. An international study to assess reliability of the Migraine Disability Assessment (MIDAS) score. Neurology. 1999;53:988–94.
Headache Classification Committee of the International Headache Society. Classification and diagnostic criteria for headache disorders: cranial neuralgias and facial pain. Cephalalgia. 1998;8:19–28.
Stewart WF, Lipton RB, Kolodner KB, Sawyer J, Lee C, Liberman JN. Validity of the Migraine Disability Assessment (MIDAS) score in comparison to a diary-based measure in a population sample of migraine sufferers. Pain. 2000;88:41–52.
Stewart WF, Lipton RB, Sawyer J. A multi-national study to assess the reliability of the migraine disability assessment (MIDAS) score. Headache. 1998;38:407.
Ware JE, Gandek B. The SF-36 health survey: development and use in mental health and the IQOLA Project. Int J Ment Health. 1994;23:49–73.
Spitzer RL, Kroenke K, Williams JB. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA. 1999;282:1737–44.
Melfi CA, Croghan TW. Use of claims data for research on treatment and outcomes of depression care. Med Care. 1999;374(4 suppl):AS77-AS80.
Simon G, Ormel J, VonKorff M, Barlow W. Health care costs associated with depressive and anxiety disorders in primary care. Am J Psychiatry. 1995;152:352–7.
Harman JS, Rollman BL, Hanusa BH, Lenze EJ, Shear MK. Physician office visits of adults for anxiety disorders in the United States, 1985–1998. J Gen Intern Med. 2002;17:165–72.
Deyo RA, Taylor VM, Diehr P, et al. Analysis of automated administrative and survey databases to study patterns and outcomes of care. Spine. 1994;19(suppl 18):2083S-2091S.
Schneeweiss S, Seeger JD, Maclure M, Wang PS, Avorn J, Glynn RJ. Performance of comorbidity scores to control for confounding in epidemiologic studies using claims data. Am J Epidemiol. 2001;154:854–64.
Savage IR. Contributions to the theory of rank order statistics—the two sample case. Ann Math Stat. 1956;27:590–615.
Duan N, Manning WG, Morris CN, Newhouse JP. A comparison of alternative models for the demand for medical care. J Bus Econ Stat. 1983;1:115–26.
Manning WG, Mullahy J. Estimating log models: to transform or not to transform? J Health Econ. 2001;20:461–94.
Breslau N, Schultz LR, Stewart WF, Lipton RB, Lucia VC, Welch KM. Headache and major depression: is the association specific to migraine? Neurology. 2000;54:308–13.
Breslau N. Migraine comorbidity with stroke, epilepsy and major depression. In Olesen J, Steiner TJ, Lipton RB, eds. Reducing the Burden of Headache. Oxford: Oxford University Press; 2003:164–72.
Clouse JC, Osterhaus JT. Healthcare resource use and costs associated with migraine in a managed healthcare setting. Ann Pharmacother. 1994;28:659–64.
Edmeads J, Mackell JA. The economic impact of migraine: an analysis of direct and indirect costs. Headache. 2002;42:501–9.
Linet MS, Celentano DD, Stewart WF. Headache characteristics associated with physician consultation: a population-based survey. Am J Prev Med. 1991;7:40–6.
Lipton RB, Stewart WF, Sawyer J, Edmeads JG. Clinical utility of an instrument assessing migraine disability: the Migraine Disability Assessment (MIDAS) questionnaire. Headache. 2001;41:854–61.
Lipton RB, Stewart WF, Celentano DD, Reed ML. Undiagnosed migraine headaches. A comparison of symptom-based and reported physician diagnosis. Arch Intern Med. 1992;152:1273–8.
Von Korff M, Wagner EH, Dworkin SF, Saunders KW. Chronic pain and use of ambulatory health care. Psychosom Med. 1991;53:61–79.
Stewart WF, Lipton RB. Migraine headache: epidemiology and health care utilization. Cephalalgia. 1993;13(suppl 12):41–6.
Rasmussen BK, Olesen J. Migraine with aura and migraine without aura: an epidemiological study. Cephalalgia. 1992;12:221–8.
Lipton RB, Stewart WF, Von Korff M. The burden of migraine. A review of cost to society. Pharmacoeconomics. 1994;6:215–21.
Von Korff M, Stewart WF, Lipton RB. Assessing headache severity. New directions. Neurology. 1994;44(6 suppl 4):S40-S46.
Ramadan NM, Silberstein S, Freitag F, Gilbert TT, Frishberg BM. Evidence based guidelines for migraine headache in the primary care setting: pharmacological management for prevention of migraine. Available at: http://www.neurology.org. Accessed March 1, 2003.
Lipton RB, Silberstein S. Why study the comorbidity of migraine? Neurology. 1994;44:28–32.
Silberstein S, Lipton RB. Chronic daily headache, including transformed migraine, chronic tension type headache and medication overuse. In: Silberstein S, Lipton RB, Dalessio DJ, eds. Wolff’s Headache and other Head Pain. New York, NY: Oxford University Press; 2001:247–82.
Centers for Disease Control and Prevention. Colorectal cancer test use among persons aged ≥ 50 years—United States, 2001. MMWR. 2003;52:193–6.
Davies GM, Santanello N, Lipton R. Determinants of patient satisfaction with migraine therapy. Cephalalgia. 2000;20:554–60.
Dasbach EJ, Carides GW, Gerth WC, Santanello NC, Pigeon JG, Kramer M. Work and productivity loss in the rizatriptan multiple attack study. Cephalalgia. 2000;29:830–4.
Cady RK, Sheftell F, Lipton RB, Kwong WJ, O’Quinn S. Economic implications of early treatment of migraine with sumatriptan tablets. Clin Ther. 2001;23:284–91.
Stang P, Cady R, Batenhorst A, Hoffman L. Workplace productivity. A review of the impact of migraine and its treatment. Pharmacoeconomics. 2001;19:231–44.
Author information
Authors and Affiliations
Corresponding author
Additional information
This research was supported by AstraZeneca Pharmaceuticals.
Rights and permissions
About this article
Cite this article
Lafata, J.E., Moon, C., Leotta, C. et al. The medical care utilization and costs associated with migraine headache. J GEN INTERN MED 19, 1005–1012 (2004). https://doi.org/10.1111/j.1525-1497.2004.30021.x
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2004.30021.x