-
PDF
- Split View
-
Views
-
Cite
Cite
WMM Verschuren, A Blokstra, HSJ Picavet, HA Smit, Cohort Profile: The Doetinchem Cohort Study, International Journal of Epidemiology, Volume 37, Issue 6, December 2008, Pages 1236–1241, https://doi.org/10.1093/ije/dym292
Close - Share Icon Share
How did the study come about?
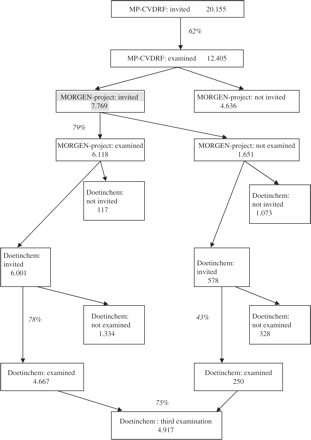
The origin of the Doetinchem Cohort Study lies within the Monitoring Project on Cardiovascular Disease Risk Factors (MP-CVDRF), which was aimed at providing prevalence estimates of cardiovascular disease risk factors, such as smoking, blood pressure and serum cholesterol levels. During 1987–91 each year an age- and sex-stratified random sample of men and women aged 20–59 years, was invited to participate. The MP-CVDRF was carried out in three towns in The Netherlands (Amsterdam in the west, Doetinchem in the east and Maastricht in the south), and from each of the three towns, about 12 000 men and women were examined. In the subsequent Monitoring Project on Chronic Disease Risk Factors (MORGEN-project), carried out from 1993–97, in Doetinchem only respondents from the MP-CVDRF were invited to participate, while in Amsterdam and Maastricht again random samples from the general population were examined. The protocol was extended, because the focus broadened from cardiovascular to other chronic diseases such as cancer, diabetes, musculoskeletal disorders and COPD. Due to extension of the protocol, with similar budget, not all 12 405 participants in the MP-CVDRF could be re-invited. Instead, a random sample of in total 7769 of the respondents at baseline was invited for re-examination. This random sample is considered the basis of the cohort (Figure 1).
Flow chart of invitations and response leading to the study population of the Doetinchem Cohort Study
What does it cover?
The aim of the Doetinchem Cohort Study is to study the impact of (changes in) lifestyle factors and biological risk factors on aspects of health, such as the incidence of chronic diseases, physical and cognitive functioning and quality of life. During the course of the study, the scope has continuously broadened. At baseline, the focus was on determinants of cardiovascular diseases. Starting from the second examination of the cohort, the scope has extended to a broad spectrum of chronic diseases that have a substantial public health impact, such as diabetes, cancer, musculoskeletal disorders, asthma and COPD. During the fourth round the social aspects were assessed and in the fifth round that will start in 2008 the focus will be more on healthy ageing and the measures will also include bone density, osteoarthritis, osteoporosis and fractures, other chronic diseases than the big five (such as diseases of bowel, liver, thyroid gland), incontinence, muscle strength and tests for physical functioning.
The study is thus aimed at a broad spectrum of hypotheses, with respect to both exposure and outcomes (Table 1). A biobank, with blood samples from each round of examination, enables us to study new hypotheses that come up during the study, when there is a biomarker that can be measured in the stored blood samples.
Overview of themes measured in Doetinchem Cohort Study
| Lifestyle factors: smoking (current and history), physical activity, dietary habits, alcohol consumption, physical load in daily activities (only in round 2) |
| Biological factors: blood pressure (incl. ankle–arm index from round 4), total and HDL-cholesterol, blood glucose (from round 2), (and several blood samples stored for future analyses), lung function (from round 2), body mass index, waist and hip circumference (from round 2), for women: reproductive history and additional characteristics on menstruation, contraception use |
| Functioning: quality of life (SF36 from round 2 onwards), cognitive functioning (for those aged >45 years, from 1995 onwards) hearing and eyesight issues (from round 4) |
| Social aspects: important social contacts (from round 2), positive and negative social experiences, between round 2 and 3 an extensive questionnaire on stress, various psychosocial aspects and life events, social functioning (number and type of social activities from round 4) |
| Chronic diseases: diabetes, cardiovascular disease (claudication, stroke, heart disease), migraine, musculoskeletal pain of back and upper extremities, cancer, asthma and COPD (including lung function tests from round 2 onwards) |
| Background characteristics: age, sex, marital status, educational level, work status and household characteristics |
| Registry links: mortality (CBS), hospital discharge by diagnosis (LMR) and pharmacy register (PHARMO). |
| Lifestyle factors: smoking (current and history), physical activity, dietary habits, alcohol consumption, physical load in daily activities (only in round 2) |
| Biological factors: blood pressure (incl. ankle–arm index from round 4), total and HDL-cholesterol, blood glucose (from round 2), (and several blood samples stored for future analyses), lung function (from round 2), body mass index, waist and hip circumference (from round 2), for women: reproductive history and additional characteristics on menstruation, contraception use |
| Functioning: quality of life (SF36 from round 2 onwards), cognitive functioning (for those aged >45 years, from 1995 onwards) hearing and eyesight issues (from round 4) |
| Social aspects: important social contacts (from round 2), positive and negative social experiences, between round 2 and 3 an extensive questionnaire on stress, various psychosocial aspects and life events, social functioning (number and type of social activities from round 4) |
| Chronic diseases: diabetes, cardiovascular disease (claudication, stroke, heart disease), migraine, musculoskeletal pain of back and upper extremities, cancer, asthma and COPD (including lung function tests from round 2 onwards) |
| Background characteristics: age, sex, marital status, educational level, work status and household characteristics |
| Registry links: mortality (CBS), hospital discharge by diagnosis (LMR) and pharmacy register (PHARMO). |
Overview of themes measured in Doetinchem Cohort Study
| Lifestyle factors: smoking (current and history), physical activity, dietary habits, alcohol consumption, physical load in daily activities (only in round 2) |
| Biological factors: blood pressure (incl. ankle–arm index from round 4), total and HDL-cholesterol, blood glucose (from round 2), (and several blood samples stored for future analyses), lung function (from round 2), body mass index, waist and hip circumference (from round 2), for women: reproductive history and additional characteristics on menstruation, contraception use |
| Functioning: quality of life (SF36 from round 2 onwards), cognitive functioning (for those aged >45 years, from 1995 onwards) hearing and eyesight issues (from round 4) |
| Social aspects: important social contacts (from round 2), positive and negative social experiences, between round 2 and 3 an extensive questionnaire on stress, various psychosocial aspects and life events, social functioning (number and type of social activities from round 4) |
| Chronic diseases: diabetes, cardiovascular disease (claudication, stroke, heart disease), migraine, musculoskeletal pain of back and upper extremities, cancer, asthma and COPD (including lung function tests from round 2 onwards) |
| Background characteristics: age, sex, marital status, educational level, work status and household characteristics |
| Registry links: mortality (CBS), hospital discharge by diagnosis (LMR) and pharmacy register (PHARMO). |
| Lifestyle factors: smoking (current and history), physical activity, dietary habits, alcohol consumption, physical load in daily activities (only in round 2) |
| Biological factors: blood pressure (incl. ankle–arm index from round 4), total and HDL-cholesterol, blood glucose (from round 2), (and several blood samples stored for future analyses), lung function (from round 2), body mass index, waist and hip circumference (from round 2), for women: reproductive history and additional characteristics on menstruation, contraception use |
| Functioning: quality of life (SF36 from round 2 onwards), cognitive functioning (for those aged >45 years, from 1995 onwards) hearing and eyesight issues (from round 4) |
| Social aspects: important social contacts (from round 2), positive and negative social experiences, between round 2 and 3 an extensive questionnaire on stress, various psychosocial aspects and life events, social functioning (number and type of social activities from round 4) |
| Chronic diseases: diabetes, cardiovascular disease (claudication, stroke, heart disease), migraine, musculoskeletal pain of back and upper extremities, cancer, asthma and COPD (including lung function tests from round 2 onwards) |
| Background characteristics: age, sex, marital status, educational level, work status and household characteristics |
| Registry links: mortality (CBS), hospital discharge by diagnosis (LMR) and pharmacy register (PHARMO). |
Who is in the sample?
The baseline measurements were carried out in 12 405 respondents from Doetinchem. This was a general population sample, drawn as an age (5-year age group) and gender stratified sample, from the municipal registers. Response rates at baseline were ∼62%. As described earlier, a sample of these respondents (N = 7769) are subsequently followed as a cohort. In Table 2, the baseline measurements of these 7769 men and women aged 20–59 years are described.
Characteristics [mean (SD)] of participants of the Doetinchem Cohort Study at baseline (1987–1991)
| . | Men . | Women . | Total . |
|---|---|---|---|
| . | N = 3641 . | N = 4128 . | N = 7769 . |
| Age, years [mean (SD)] | 40.5 (10.2) | 39.9 (10.5) | 40.2 (10.3) |
| Gender (% males) | 53 | ||
| Education, highest degree reached (%) | |||
| Primary school | 13 | 17 | 15 |
| Lower secondary/vocational school | 44 | 52 | 48 |
| Intermediate vocational/higher secondary school | 24 | 19 | 21 |
| Higher vocational/university | 19 | 12 | 15 |
| Blood pressure | |||
| Diastolic, mmHg [mean, (SD)] | 80 (10) | 76 (11) | 78 (11) |
| Systolic in mmHg [mean, (SD)] | 126 (14) | 118 (15) | 122 (15) |
| Hypertension (%)a | 24.0 | 15.4 | 19.4 |
| Blood lipids | |||
| Total cholesterol, mmol/l [mean (SD)] | 5.6 (1.12) | 5.4 (1.08) | 5.5 (1.10) |
| Hypercholesterolemia (≥6.5 mmol/l) (%) | 18.9 | 15.0 | 16.8 |
| HDL cholesterol, mmol/l [mean (SD)] | 1.1 (0.26) | 1.4 (0.31) | 1.2 (0.31) |
| Low HDL cholesterol (≤0.9 mmol/l) (%) | 19.2 | 4.6 | 11.5 |
| Body weight | |||
| BMI, kg/m2 [mean, (SD)] | 25.1 (3.2) | 24.4 (4.0) | 24.7 (3.7) |
| overweight (25 kg/m2 <BMI <30 kg/m2) (%) | 41.3 | 27.5 | 34.0 |
| obesity (BMI ≥30 kg/m2) (%) | 6.4 | 8.9 | 7.8 |
| Smoking | |||
| Smokers (%) | 37.1 | 35.3 | 36.2 |
| Ex-smokers (%) | 31.7 | 23.3 | 27.2 |
| Never smokers (%) | 31.2 | 41.3 | 36.6 |
| Mean (SD) number of cigarettes smoked per day (in smokers) | 15.7 (8.3) | 13.4 (7.1) | 14.5 (7.8) |
| Alcohol consumption | |||
| Drinkers (≥1 glass/week) (%) | 78.7 | 48.1 | 62.4 |
| Mean (SD) glasses of alcohol per day (drinkers only) | 1.9 (1.6) | 1.0 (0.84) | 1.6 (1.4) |
| . | Men . | Women . | Total . |
|---|---|---|---|
| . | N = 3641 . | N = 4128 . | N = 7769 . |
| Age, years [mean (SD)] | 40.5 (10.2) | 39.9 (10.5) | 40.2 (10.3) |
| Gender (% males) | 53 | ||
| Education, highest degree reached (%) | |||
| Primary school | 13 | 17 | 15 |
| Lower secondary/vocational school | 44 | 52 | 48 |
| Intermediate vocational/higher secondary school | 24 | 19 | 21 |
| Higher vocational/university | 19 | 12 | 15 |
| Blood pressure | |||
| Diastolic, mmHg [mean, (SD)] | 80 (10) | 76 (11) | 78 (11) |
| Systolic in mmHg [mean, (SD)] | 126 (14) | 118 (15) | 122 (15) |
| Hypertension (%)a | 24.0 | 15.4 | 19.4 |
| Blood lipids | |||
| Total cholesterol, mmol/l [mean (SD)] | 5.6 (1.12) | 5.4 (1.08) | 5.5 (1.10) |
| Hypercholesterolemia (≥6.5 mmol/l) (%) | 18.9 | 15.0 | 16.8 |
| HDL cholesterol, mmol/l [mean (SD)] | 1.1 (0.26) | 1.4 (0.31) | 1.2 (0.31) |
| Low HDL cholesterol (≤0.9 mmol/l) (%) | 19.2 | 4.6 | 11.5 |
| Body weight | |||
| BMI, kg/m2 [mean, (SD)] | 25.1 (3.2) | 24.4 (4.0) | 24.7 (3.7) |
| overweight (25 kg/m2 <BMI <30 kg/m2) (%) | 41.3 | 27.5 | 34.0 |
| obesity (BMI ≥30 kg/m2) (%) | 6.4 | 8.9 | 7.8 |
| Smoking | |||
| Smokers (%) | 37.1 | 35.3 | 36.2 |
| Ex-smokers (%) | 31.7 | 23.3 | 27.2 |
| Never smokers (%) | 31.2 | 41.3 | 36.6 |
| Mean (SD) number of cigarettes smoked per day (in smokers) | 15.7 (8.3) | 13.4 (7.1) | 14.5 (7.8) |
| Alcohol consumption | |||
| Drinkers (≥1 glass/week) (%) | 78.7 | 48.1 | 62.4 |
| Mean (SD) glasses of alcohol per day (drinkers only) | 1.9 (1.6) | 1.0 (0.84) | 1.6 (1.4) |
aSystolic ≥140 mmHg and/or diastolic ≥90 mmHg and/or anti-hypertensive medication.
Characteristics [mean (SD)] of participants of the Doetinchem Cohort Study at baseline (1987–1991)
| . | Men . | Women . | Total . |
|---|---|---|---|
| . | N = 3641 . | N = 4128 . | N = 7769 . |
| Age, years [mean (SD)] | 40.5 (10.2) | 39.9 (10.5) | 40.2 (10.3) |
| Gender (% males) | 53 | ||
| Education, highest degree reached (%) | |||
| Primary school | 13 | 17 | 15 |
| Lower secondary/vocational school | 44 | 52 | 48 |
| Intermediate vocational/higher secondary school | 24 | 19 | 21 |
| Higher vocational/university | 19 | 12 | 15 |
| Blood pressure | |||
| Diastolic, mmHg [mean, (SD)] | 80 (10) | 76 (11) | 78 (11) |
| Systolic in mmHg [mean, (SD)] | 126 (14) | 118 (15) | 122 (15) |
| Hypertension (%)a | 24.0 | 15.4 | 19.4 |
| Blood lipids | |||
| Total cholesterol, mmol/l [mean (SD)] | 5.6 (1.12) | 5.4 (1.08) | 5.5 (1.10) |
| Hypercholesterolemia (≥6.5 mmol/l) (%) | 18.9 | 15.0 | 16.8 |
| HDL cholesterol, mmol/l [mean (SD)] | 1.1 (0.26) | 1.4 (0.31) | 1.2 (0.31) |
| Low HDL cholesterol (≤0.9 mmol/l) (%) | 19.2 | 4.6 | 11.5 |
| Body weight | |||
| BMI, kg/m2 [mean, (SD)] | 25.1 (3.2) | 24.4 (4.0) | 24.7 (3.7) |
| overweight (25 kg/m2 <BMI <30 kg/m2) (%) | 41.3 | 27.5 | 34.0 |
| obesity (BMI ≥30 kg/m2) (%) | 6.4 | 8.9 | 7.8 |
| Smoking | |||
| Smokers (%) | 37.1 | 35.3 | 36.2 |
| Ex-smokers (%) | 31.7 | 23.3 | 27.2 |
| Never smokers (%) | 31.2 | 41.3 | 36.6 |
| Mean (SD) number of cigarettes smoked per day (in smokers) | 15.7 (8.3) | 13.4 (7.1) | 14.5 (7.8) |
| Alcohol consumption | |||
| Drinkers (≥1 glass/week) (%) | 78.7 | 48.1 | 62.4 |
| Mean (SD) glasses of alcohol per day (drinkers only) | 1.9 (1.6) | 1.0 (0.84) | 1.6 (1.4) |
| . | Men . | Women . | Total . |
|---|---|---|---|
| . | N = 3641 . | N = 4128 . | N = 7769 . |
| Age, years [mean (SD)] | 40.5 (10.2) | 39.9 (10.5) | 40.2 (10.3) |
| Gender (% males) | 53 | ||
| Education, highest degree reached (%) | |||
| Primary school | 13 | 17 | 15 |
| Lower secondary/vocational school | 44 | 52 | 48 |
| Intermediate vocational/higher secondary school | 24 | 19 | 21 |
| Higher vocational/university | 19 | 12 | 15 |
| Blood pressure | |||
| Diastolic, mmHg [mean, (SD)] | 80 (10) | 76 (11) | 78 (11) |
| Systolic in mmHg [mean, (SD)] | 126 (14) | 118 (15) | 122 (15) |
| Hypertension (%)a | 24.0 | 15.4 | 19.4 |
| Blood lipids | |||
| Total cholesterol, mmol/l [mean (SD)] | 5.6 (1.12) | 5.4 (1.08) | 5.5 (1.10) |
| Hypercholesterolemia (≥6.5 mmol/l) (%) | 18.9 | 15.0 | 16.8 |
| HDL cholesterol, mmol/l [mean (SD)] | 1.1 (0.26) | 1.4 (0.31) | 1.2 (0.31) |
| Low HDL cholesterol (≤0.9 mmol/l) (%) | 19.2 | 4.6 | 11.5 |
| Body weight | |||
| BMI, kg/m2 [mean, (SD)] | 25.1 (3.2) | 24.4 (4.0) | 24.7 (3.7) |
| overweight (25 kg/m2 <BMI <30 kg/m2) (%) | 41.3 | 27.5 | 34.0 |
| obesity (BMI ≥30 kg/m2) (%) | 6.4 | 8.9 | 7.8 |
| Smoking | |||
| Smokers (%) | 37.1 | 35.3 | 36.2 |
| Ex-smokers (%) | 31.7 | 23.3 | 27.2 |
| Never smokers (%) | 31.2 | 41.3 | 36.6 |
| Mean (SD) number of cigarettes smoked per day (in smokers) | 15.7 (8.3) | 13.4 (7.1) | 14.5 (7.8) |
| Alcohol consumption | |||
| Drinkers (≥1 glass/week) (%) | 78.7 | 48.1 | 62.4 |
| Mean (SD) glasses of alcohol per day (drinkers only) | 1.9 (1.6) | 1.0 (0.84) | 1.6 (1.4) |
aSystolic ≥140 mmHg and/or diastolic ≥90 mmHg and/or anti-hypertensive medication.
How often have they been followed?
The cohort is re-examined every 5 years. Only between the first and second round is 6 years, because a pilot year was necessary to test new elements of the study. The fourth round has been completed in 2007, and the fifth round has started in 2008, with funding from the Dutch Ministry of Public Health, Welfare and Sports. Respondents are also followed through linkage to several registers. All respondents are flagged in the national population register: if a respondent dies we are informed about the date of death. Regular linkage with the mortality register of Statistics Netherlands provides the cause of death of all respondents that have died. Incidence of cancer is based on linkage with the national cancer register (LKR), incidence of a broad range of diseases is based on linkage to the national hospital discharge register (LMR). From 1991 onwards, every prescribed medicine that has been collected at the pharmacist by a respondent is available through linkage with the pharmacy register (PHARMO). All these linkages are done for those respondents that have agreed on that in their informed consent (which is the case for over 95% of the respondents).
What has been measured?
Biological risk factors
Blood pressure was measured in each round, with the subject in sitting position. Systolic pressure was recorded at the appearance of sounds (first-phase Korotkoff) and diastolic blood pressure was recorded at the disappearance of sounds (fifth-phase Korotkoff). Blood pressure was measured twice, after the first measurement heart rate was measured for 30 s, followed by the second measurement.1,Total and HDL cholesterol were measured in each round (until 1998 in non-fasting EDTA-plasma, from 1998 onwards in serum) at the Lipid Reference Laboratory (LRL) of the university Hospital Dijkzigt in Rotterdam, using standardized enzymatic methods. Performance for enzymatic total and HDL cholesterol measurements fulfilled National Cholesterol Education Program (NCEP) recommendations throughout the entire study period.2,Body weight and height were measured by trained staff in each round with participants wearing light indoor clothing without shoes, with emptied pockets. Body weight was measured to the nearest 100 g on calibrated scales. From round two onwards, waist and hip circumference have also been measured. Lung function has been measured from 1994 onwards. Lung function is measured with a heated pneumotachometer (Jaeger, Germany). Calibration takes place twice a day. Subjects are seated in upright position with a fixed mouthpiece, adjusted for the height of the individual, and a nose clip. Forced expiratory volume in 1 s is measured (FEV1) as well as forced vital capacity (FVC) according to criteria of the European Respiratory Society (ERS).3 From 1995 onwards, all participants aged 45 years and older were invited to take part in a cognitive function test, consisting of several subtests: the 15 Words Learning Test, the Stroop Test, Word Fluency test and the Letter Digit Substitution Test.4–7 Between 1995 and 2005 cognitive function has been measured twice in 1964 respondents. The neuropsychological test battery that was used measures specific cognitive domains, i.e. memory function, speed of cognitive processes, cognitive flexibility, i.e. higher order information processing, and global cognitive function. The used tests are sensitive to calendar age, have no ceiling effect and are robust in detecting age-related impairment, even at middle age.8 They have also been used in other large-scale studies on cognitive function.9,10
Lifestyle factors
Smoking was assessed at every round of examination with several questions. Ever smokers were identified based on the question ‘did you ever smoke regularly’. For ever smokers, information on age at which the respondent started smoking, as well as the total number of years of smoking and average amount of cigarettes smoked was assessed, followed by a question on current smoking (‘do you smoke at present’). At baseline, dietary intake was assessed with a short (70 food items) self-administered semi-quantitative food frequency questionnaire. From 1993 onwards, a 178-item semi-quantitative food frequency questionnaire was administered. This questionnaire was developed for the EPIC-Study, a prospective study into nutrition and cancer and has been validated.11,12Physical activity was assessed at baseline with two simple questions on physical activity at work and during leisure time. Starting from 1994, an extensive physical activity self-administered questionnaire, developed for the EPIC-Study, was used to assess level of physical activity over the past year. This extensive questionnaire includes physical activity at work, during leisure time, during household activities and during transportation (e.g. bicycling to work). In addition, questions on sports activities and other strenuous activities are included. For each activity, average hours spent on that activity are recorded, separately for summer and winter.13Alcohol intake has been assessed at every round of examination, as number of glasses consumed per week, distinguishing beer, wine, port wines and strong liquor.
Demographic information
Level of education was measured as the highest level reached in seven answering categories ranging from primary school only to completed university education. Marital status has been assessed at every round, as well as household composition starting from round two onwards.
Health: in all rounds, information has been collected on self perceived health, and on history of several chronic diseases for the respondents as well as family history of several chronic diseases.
What is the attrition rate?
Response rate at baseline was 62% on average, with higher response rates among women and the elderly than in men and the younger age groups. At follow-up response rates have been 75–80% (Table 3).
Response rates in the Doetinchem Cohort Study
| . | Round 1 . | Round 2 . | Round 3 . | Round 4 . |
|---|---|---|---|---|
| Name | Monitoring Project on Cardiovascular Disease Risk Factors (MP-CVDRF) | Monitoring Project on Chronic Disease Risk Factors (MORGEN-Project) | Doetinchem cohort study | Doetinchem cohort study |
| Years | 1987–91 | 1993–97 | 1998–2002 | 2003–07 |
| Age | 20–59 yrs | 26–65 yrs | 31–70 yrs | 36–75 yrs |
| Numbers participated | 12.405 | 6.118 | 4.917 | 4.523 |
| Response | 62% | 79% | 75% | 78% |
| Numbers invited | 20.155 | 7.769 | 6.579 | 5.784 |
| Who were invited | Age and sex stratified random sample of population | A random two-third of those measured in round one | Those who were invited in round 2 excluding those who emigrated, actively withdrew from the study or died | Those who were invited in round 3 excluding those who emigrated, actively withdrew from the study or died |
| . | Round 1 . | Round 2 . | Round 3 . | Round 4 . |
|---|---|---|---|---|
| Name | Monitoring Project on Cardiovascular Disease Risk Factors (MP-CVDRF) | Monitoring Project on Chronic Disease Risk Factors (MORGEN-Project) | Doetinchem cohort study | Doetinchem cohort study |
| Years | 1987–91 | 1993–97 | 1998–2002 | 2003–07 |
| Age | 20–59 yrs | 26–65 yrs | 31–70 yrs | 36–75 yrs |
| Numbers participated | 12.405 | 6.118 | 4.917 | 4.523 |
| Response | 62% | 79% | 75% | 78% |
| Numbers invited | 20.155 | 7.769 | 6.579 | 5.784 |
| Who were invited | Age and sex stratified random sample of population | A random two-third of those measured in round one | Those who were invited in round 2 excluding those who emigrated, actively withdrew from the study or died | Those who were invited in round 3 excluding those who emigrated, actively withdrew from the study or died |
Response rates in the Doetinchem Cohort Study
| . | Round 1 . | Round 2 . | Round 3 . | Round 4 . |
|---|---|---|---|---|
| Name | Monitoring Project on Cardiovascular Disease Risk Factors (MP-CVDRF) | Monitoring Project on Chronic Disease Risk Factors (MORGEN-Project) | Doetinchem cohort study | Doetinchem cohort study |
| Years | 1987–91 | 1993–97 | 1998–2002 | 2003–07 |
| Age | 20–59 yrs | 26–65 yrs | 31–70 yrs | 36–75 yrs |
| Numbers participated | 12.405 | 6.118 | 4.917 | 4.523 |
| Response | 62% | 79% | 75% | 78% |
| Numbers invited | 20.155 | 7.769 | 6.579 | 5.784 |
| Who were invited | Age and sex stratified random sample of population | A random two-third of those measured in round one | Those who were invited in round 2 excluding those who emigrated, actively withdrew from the study or died | Those who were invited in round 3 excluding those who emigrated, actively withdrew from the study or died |
| . | Round 1 . | Round 2 . | Round 3 . | Round 4 . |
|---|---|---|---|---|
| Name | Monitoring Project on Cardiovascular Disease Risk Factors (MP-CVDRF) | Monitoring Project on Chronic Disease Risk Factors (MORGEN-Project) | Doetinchem cohort study | Doetinchem cohort study |
| Years | 1987–91 | 1993–97 | 1998–2002 | 2003–07 |
| Age | 20–59 yrs | 26–65 yrs | 31–70 yrs | 36–75 yrs |
| Numbers participated | 12.405 | 6.118 | 4.917 | 4.523 |
| Response | 62% | 79% | 75% | 78% |
| Numbers invited | 20.155 | 7.769 | 6.579 | 5.784 |
| Who were invited | Age and sex stratified random sample of population | A random two-third of those measured in round one | Those who were invited in round 2 excluding those who emigrated, actively withdrew from the study or died | Those who were invited in round 3 excluding those who emigrated, actively withdrew from the study or died |
What has been found
Baseline data of the Doetinchem Cohort Study, in combination with the data from the two other towns in which a random population sample was examined, have been used to describe levels and trends in cardiovascular risk factors in The Netherlands.14,15 Based on our data on cardiovascular risk factors in combination with questions on treatment for risk factors, we showed an increase in the treatment of hypercholesterolaemia over the period 1987–2002, but also observed that in 2002, still one-third of all those eligible for treatment are still not being treated.16,17 With respect to cognitive functioning, we showed that smoking was associated with worse cognitive functioning, while intake of n-3 and unsaturated fatty acids and moderate alcohol consumption were associated with better cognitive functioning.18,19 We also showed longitudinally that retirement was associated with an increase in weight and waist circumference among those with former active jobs, but not among those with former sedentary jobs, showing that retirement may bring opportunities for healthy changes in diet and physical activity, which could be used in health promotion programmes.20 At present, a number of research projects have started on the impact of lifestyle (smoking, diet, physical activity) and risk factors (body weight, blood pressure, serum cholesterol) on the incidence of several chronic diseases (cardiovascular diseases, diabetes, COPD and musculoskeletal disorders), and on determinants of cognitive decline and healthy ageing.
Main strengths and weaknesses
Strengths
One of the strengths of the present cohort is that extensive measurements on lifestyle have been collected, starting at a relatively young age: the entire cohort was aged less than 60 years at the start, and half of the cohort was aged 40 years or younger. Having followed this cohort now during four rounds of examinations, 5 years apart, the cohort is well-suited to study the impact of lifestyle at young/middle-age on the occurrence of chronic diseases and quality of life at middle/old age. Our lifestyle measurements are quite extensive, with three repeated measurements of an extensive dietary questionnaire, and extensive measurements of physical activity. Also our repeated measurement of cognitive function, starting at age 45 is an early measure. An advantage of conducting this study in a rural area in the east of The Netherlands is that migration rate is low in this area, which benefits the stability of the cohort.
Weaknesses
Since Doetinchem is a rural area in the eastern part of The Netherlands, the sample may not be entirely representative for The Netherlands, however this will almost always be the case with a single-site study. Response rates are always an issue. At baseline response rate was on average 62%, which is quite reasonable for a general survey in The Netherlands, but we know that e.g. the lower educated and smokers are underrepresented in our cohort. Response rates at follow-up have been stable at 75–80% over the entire study. However, both response rates as well as representativeness of the study population are mainly a problem for prevalence estimates, but much less for estimating the magnitude of associations between exposure and disease.
How can I collaborate?
We welcome collaborative research on the data of the Doetinchem Cohort Study. For more information, contact the National Institute for Public Health and the Environment, Division Public Health, Centre for Prevention and Health Services Research, Dr W.M.M. Verschuren, principal investigator (wmm.verschuren@rivm.nl). Project leader for the fifth round of examination is Dr H.S.J. Picavet (susan.picavet@rivm.nl).
Conflict of interest: None declared.
References
- physical activity
- smoking
- high density lipoprotein cholesterol
- cardiovascular diseases
- diabetes mellitus
- chronic obstructive airway disease
- heart disease risk factors
- diabetes mellitus, type 2
- blood pressure
- cancer
- diet
- alcohol drinking
- chronic disease
- demography
- life style
- mental processes
- musculoskeletal diseases
- netherlands
- public health medicine
- quality of life
- frequency of responses
- cognitive ability
- experimental attrition