-
PDF
- Split View
-
Views
-
Cite
Cite
N.M. van Mello, F. Mol, B.C. Opmeer, W.M. Ankum, K. Barnhart, A. Coomarasamy, B.W. Mol, F. van der Veen, P.J. Hajenius, Diagnostic value of serum hCG on the outcome of pregnancy of unknown location: a systematic review and meta-analysis, Human Reproduction Update, Volume 18, Issue 6, November/December 2012, Pages 603–617, https://doi.org/10.1093/humupd/dms035
Close - Share Icon Share
Abstract
The term ‘pregnancy of unknown location’ (PUL) refers to cases where a pregnancy test is positive but the pregnancy cannot be visualized by transvaginal sonography (TVS). Various strategies integrating TVS and serum hCG measures are used to follow-up until the location and/or viability of the pregnancy becomes clear; however, the optimal strategy to predict the outcome of pregnancy in women with PUL is unknown. Therefore, we performed a systematic review and meta-analysis to determine the diagnostic accuracy of the various serum hCG strategies in women with PUL.
We searched Medline and EMBASE for articles which were published (in any language) from 1980 to January 2012 on strategies using serum hCG in women with PUL and reporting on the final outcome of pregnancy.
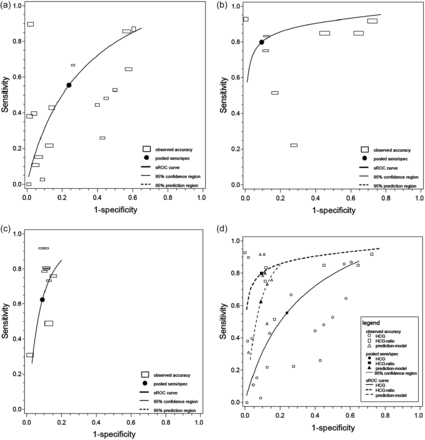
From 980 selected titles, 23 articles, all cohort studies, were included. There were 10 studies on a single serum hCG cut-off level, 4 on serum hCG ratio (hCG 48 h/hCG 0 h) and 6 on logistic regression modelling. Three other strategies were reported using serum hCG, serum progesterone and/or uterine curettage findings; each of these strategies comprised a single study. Comparative diagnostic studies have not been performed on the diagnostic value of serum hCG in women with PUL. Included studies showed substantial clinical heterogeneity in the definition of the outcome, and only data for the pregnancy outcome ectopic pregnancy (EP) were suitable for meta-analysis. The receiver operating characteristic curves showed that the serum hCG ratios and logistic regression models had a better performance as compared with an absolute single serum hCG level (as the curve was considerably closer to the diagonal, indicating no diagnostic value).
Overall the study was limited by the high clinical heterogeneity of the data but in women with PUL diagnostic strategies using serum hCG ratios, either alone or in logistic regression models, have the best diagnostic performance in the case of EP. Well defined prospective comparative studies using standardized diagnostics and clinical application plus agreed definitions of outcome are required to identify the best strategy to diagnose pregnancy outcome in women with PUL.
Background
‘Pregnancy of unknown location’ (PUL) is the term used to define a pregnancy which cannot be visualized by transvaginal sonography (TVS). PUL occurs in 7–30% of women who present with complaints in early pregnancy, e.g. abdominal discomfort and/or vaginal bleeding (Kirk et al., 2009).
The majority of women with PUL (50–70%) have a spontaneously resolving pregnancy with serum hCG levels declining to undetectable levels, the so-called failed PUL. Such a pregnancy can either be a failed intrauterine pregnancy (IUP) or a resolved ectopic pregnancy (EP), as the location of the pregnancy remains undetermined. In some women the pregnancy duration is simply too short to allow its visualization on the initial scan. Follow-up scans in combination with rising serum hCG levels will eventually demonstrate an IUP. In 7–20% of women with a PUL, an EP is eventually diagnosed and these women are eligible for laparoscopic surgery or medical therapy with systemic methotrexate (MTX). Only a minority of women will have a persisting PUL, defined as an inconclusive TVS in combination with a rise or plateau in serial serum hCG levels. The optimal management for persisting PUL is not known. Systemic MTX as well as expectant management are reported to be successful (Condous et al., 2003).
There is worldwide consensus that TVS and quantitative serum hCG measurement are useful and should be applied to diagnose the pregnancy location, i.e. the pregnancy outcome in women with PUL (Dutch Society of Obstetrics and Gynaecology, 2001; American College of Obstetricians and Gynaecologists, 2008; Barnhart, 2009; Royal College of Obstetricians and Gynaecologists, 2010). A variety of algorithms have been proposed, integrating clinical examination, TVS and (repeated) serum hCG measurements, to predict the final location and viability of the pregnancy (Cacciatore et al., 1990; Stovall et al., 1992; Ankum et al., 1995; Hajenius et al., 1995; Gracia and Barnhart, 2001; Mertz and Yalcinkaya, 2001; Kohn et al., 2003; Condous et al., 2004, 2005a; Timmerman, 2004). However, no evidence exists on the optimal strategy to predict the outcome of pregnancy in women with PUL. We therefore performed a systematic review and meta-analysis to determine the diagnostic accuracy of the various serum hCG strategies in women with PUL.
Methods
Identification of studies
We performed a literature search using a structured predefined search string on Ovid MEDLINE and EMBASE from 1980 to January 2012. An information specialist performed the electronic search using the terms: ‘unknown/unidentified/undetermined/uncertain pregnancy’ or ‘ectopic pregnancy’, ‘chorionic gonadotrophin’, ‘diagnosis/prognosis/prediction’. We checked cross-references of eligible papers to identify papers not captured by electronic searches. There was a restriction concerning publication year because the introduction of TVS was around the mid-1980s. No restrictions were made based on language.
Selection of studies and data extraction
Two reviewers (N.M. and F.M.) evaluated potentially eligible papers in a two-stage process. First, papers identified in the search were screened for eligibility by reading the title and abstract. If there were any doubts about eligibility, the full text was screened to make sure that no papers were missed. We then obtained full-text versions of all papers which were selected by at least one of the reviewers in the first stage.
Papers were included if the studies reported on women with PUL, serum hCG levels and the final outcome of the pregnancy (IUP, EP, treated persistent PUL or failed PUL). All studies were scored on methodological quality according to the standard for reporting of diagnostic accuracy guideline and the quality assessment tool of diagnostic accuracy studies (QUADAS) and entered on a data extraction form (Khan et al., 2004; Whiting et al., 2006). We scored each study on the following characteristics: study design, data collection (prospective or retrospective), sampling (consecutive women or other) and reported TVS findings. The index test was serum hCG. The reference test differed per pregnancy outcome. To evaluate potential verification bias, we assessed the predefined reference standard as a composite of IUP, EP or other outcomes, as defined by the authors for the QUADAS scoring. Item number 4 of the QUADAS tool, concerning disease progression bias, was removed from the scoring list because the actual pregnancy outcome can only be determined when the pregnancy progresses in women with PUL. We also removed item number 10 from the QUADAS tool because time is an indispensable factor in the diagnosis of women with a PUL and the reference standard was, by definition, performed after the index test.
Studies were included when data were available, either directly or retractable, in which absolute serum hCG levels were expressed for the final pregnancy outcome and/or two-by-two tables for specified strategies were provided.
Statistical analysis
We calculated sensitivity and specificity with 95% confidence intervals (CIs) for each study individually, created forest plots to explore heterogeneity for sensitivity and specificity and plotted their combined results in receiver operating characteristic (ROC) space (sensitivity versus 1 − specificity). To obtain summary estimates of sensitivity and specificity and their 95% CIs and to construct summary ROC (sROC) curves bivariate regression analysis was used (Reitsma et al., 2005; Hamza et al., 2008). The bivariate regression model statistically incorporates the negative correlation that might exist between sensitivity and specificity, because sensitivity and specificity within a study are often negatively correlated, owing to implicit variation of threshold values (Leeflang et al., 2008). To determine the variation or statistical heterogeneity between the results of the studies the random-effects approach was applied. The random-effects approach estimates and incorporates the amount of between-study variability in both sensitivity and specificity. The included studies often reported a different threshold value to define a positive pregnancy test result. To evaluate accuracy measures over the whole range of reported hCG thresholds in all studies, we did not limit our analysis to a single threshold value but estimated accuracy measures for all reported threshold values by assuming that the shift in accuracy (higher sensitivity and lower specificity) due to different thresholds is accounted for by the correlation term, as specified in the bivariate model.
The recommended bivariate modelling approach cannot appropriately account for covariates (such as threshold) with multiple observations from the same study (Leeflang et al., 2008). In order to avoid results being biased towards studies reporting on many different thresholds, we used a stratified bootstrap approach to statistically incorporate different thresholds from the same study in the model. We estimated each model in 50 stratified bootstrap samples, in which only one accuracy estimate from each study was randomly selected. The average overall estimates from 50 bootstrap samples is used to estimate sROC curves, where the increase in sensitivity and decrease in specificity reflect the shift in the threshold value of serum hCG in the model. As the data points represent different thresholds defining a positive test result, the sROC points for these models only reflect the average operating point but have no evident clinical meaning. For the analysis the statistical software package SAS 9.3 (SAS Institute, Cary, NC) was used. A value of P < 0.05 was considered statistically significant.
Results
Number of retrieved papers
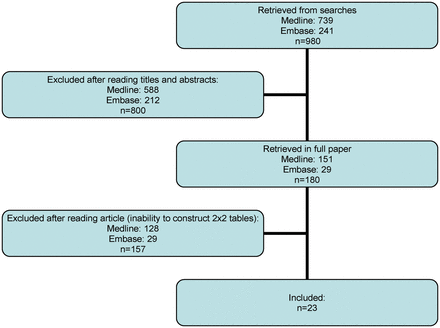
Our search retrieved 980 citations from MEDLINE and EMBASE. The process of selection of papers is summarized in Fig. 1. We retrieved no papers from cross-references. After screening titles, abstracts and cross-references, 180 papers were selected for full text review. Of these, 23 studies were included for the meta-analysis.
Flow chart of literature search and article selection for a systematic review and meta-analysis of studies on women with pregnancy of unknown location, diagnostic strategies using serum hCG levels and the final outcome of the pregnancy.
Characteristics of included studies
The characteristics of the 23 included studies are presented in Table I. Different types of diagnostic strategy using serum hCG were identified. Studies from 1995 to 2011 used a single absolute serum hCG cut-off level (n = 10), studies from 1995 to 2008 used serial serum hCG levels over 48 h, thereby focusing on the hCG ratio (hCG 48 h/hCG 0 h) (n = 4), while more recently (2006–2010) logistic regression modelling strategies were described (n = 6). These six logistic regression models all used serum hCG ratios but combined with different variables: clinical symptoms (n = 2), TVS findings (n = 4), maternal age (n = 2), gestational age (n = 2), risk factors for EP (n = 1) and progesterone levels (n = 4). One study used the prediction by the nurse practitioner combined with hCG ratios, and another the logarithm of the hCG average, the hCG ratio and its quadratic effect. Three other strategies were reported using serum hCG, serum progesterone and/or uterine curettage findings; each of these strategies comprised a single study.
Characteristics of the 23 included studies in a systematic review of the diagnostic value of serum hCG on the outcome of pregnancy of unknown location (PUL).
| First author (year) . | Serum hCG test . | PUL population . | Study type . | Outcome definitions and reference tests . |
|---|---|---|---|---|
| Single serum hCG cut-off level | ||||
| Hajenius et al. (1995) | hCG >1000 IU/l | Clinical suspicion of EP, i.e. vaginal bleeding with/without abdominal pain and/or risk factors and patients without symptoms or risk factors. Without clinical symptoms of shock No visible pregnancy on TVS Serum hCG <1500 IU/L | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and uneventful decrease of hCG |
| Kaplan et al. (1996) | hCG <1000 mIU/ml | Inconclusive diagnosis by TVS and abdominal ultrasound: no evidence of IUP or EP | Prospective cohort | IUP: confirmed by TVS or villi after D&C EP: confirmed at laparoscopy or laparotomy |
| Dart et al. (1997) | hCG >3000 mIU/ml Menstrual days >38 | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | Normal IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS and villi at pathology, no villi after D&C with hCG falling to zero or hCG falling to zero without intervention |
| Dart and Howard (1998) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Dart et al. (1999a) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: empty endometrial cavity and no adnexal or cul-de-sac findings. Exclusion: lost to follow-up, endometrial stripe thickness not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Mol et al. (1998) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No IUP at TVS and no ectopic mass or fluid in pouch of Douglas | Prospective cohort study | IUP: TVS confirmation at 12 weeks EP: laparoscopy Nonviable pregnancy: non viable IUP and chemical pregnancies, resolved without treatment |
| Dart et al. (2002) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: prior TVS showed IUP, passed definitive product of conception, status post-D&C, recent delivery or lost to follow-up | Prospective observational cohort study | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after D&C or systemic MTX or negative D&C |
| Condous et al. (2005a) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational study | IUP: presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| El Bishry and Ganta (2008) | P <16 nmol/l and hCG >25 IU/l P = 16–80 nmol/l and hCG >25 IU/l P >80 nmol/l and hCG <1000 IU/l P >80 nmol/l and hCG >1000 IU/l | Inconclusive scan | Retrospective cohort study | Viable IUP Criterion standard diagnosis of IUP, EP or miscarriage, not further specified |
| Shaunik et al. (2011) | hCG <2000 mIU/ml | Non-viable PUL: clinically stable, initial hCG >2000 mIU/ml and non-diagnostic ultrasound or abnormal rise/fall/plateau with initial hCG <2000 mIU/ml | Cohort study | IUP = non-viable IUP: histopathology after curettage or resolution of hCG after curettage EP: histopathology at surgery or TVS ectopic gestational sac or rise in hCG after curettage without villi at pathology |
| Serum hCG ratio | ||||
| Ankum et al. (1995) | Initial hCG <1500, hCG ratio | No pregnancy detectable at TVS and hCG <1500 IU/l | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and decrease of hCG with the disappearance of symptoms |
| Dart et al. (1999b) | hCG increase <66% hCG decrease <50% | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate. Second serum hCG performed within 7 days of first visit and before D&C or laparoscopy or MTX. Exclusion: lost to follow-up | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after negative D&C or treated with systemic MTX or EP visualized on TVS Abnormal IUP: (1) hCG >3000 mIU/ml with an empty uterus, decreasing hCG or progesterone <5.0 ng/ml before D&C and villi after D&C. (2) Villi after D&C and hCG falling to zero without intervention and (3) hCG values falling to zero without intervention |
| Condous et al. (2004) | Logistic regression model M1 (hCG ratio >0.21) | Women with abdominal pain, vaginal blood loss or to determine gestational age. No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational cohort study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: initial progesterone <20 nmol/l and spontaneous resolution of pregnancy: decrease of hCG <5 with the disappearance of symptoms |
| Bignardi et al. (2008) | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective observational cohort | IUP: gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Logistic regression model | ||||
| Gevaert et al. (2006) | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | PUL not further specified | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| Kirk et al. (2006) | Logistic regression model based on hCG ratio, prediction by nurse practitioner and costs | No evidence of an IUP or EP on TVS. Exclusion criteria: visualization of an intrauterine gestational sac with or without a fetal pole, adnexal mass thought to be an EP, heterogeneous tissue in endometrial cavity and hemodynamic instability or pain, or hemoperitoneum on TVS | Prospective non-interventional observational study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later, the presence of gestational sac eccentrically placed in the endometrial cavity or heterogeneous tissue in the cavity. EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/L with the disappearance of pregnancy symptoms |
| Condous et al. (2007a) | Logistic regression model M4 hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | No signs of an IUP, an EP or retained products of conception at TVS | Prospective cohort study | IUP: intrauterine gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Kirk et al. (2007) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No evidence of an IUP or EP on TVS, hCG level <10 000 IU/l, clinically stable and no signs of hemoperitoneum on TVS | Prospective interventional study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/l with the disappearance of pregnancy symptoms |
| Condous et al. (2007b) | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity, TVS 2 weeks later to confirm viability EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Barnhart et al. (2010) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | Women with lower abdominal pain, vaginal bleeding, maternal anxiety or confirmation of gestational age. PUL if there was no evidence of an IUP or EP on TVS | Retrospective cohort study | IUP: rise hCG in 48 h >66% and TVS 2 weeks later: the presence of gestational sac eccentrically placed in the endometrial cavity EP: histological confirmation of villi in the tube or echogenicity consistent with an EP Spontaneous miscarriage/failing PUL: spontaneous resolution of pregnancy with the decrease of hCG level <5 U/l |
| Other strategies | ||||
| Condous et al. (2005b) | Single visit protocol: high-risk PUL Prog 5–81 nmol/l or hCG >50 IU/l | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test | Retrospective protocol development, followed by prospective trial | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL Failing PUL: persistent PUL and falling hCG levels |
| Condous et al. (2006) | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test. Clinically stable women | Prospective observational cohort study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL |
| Rivera et al. (2009) | hCG decrease <50% after manual vacuum aspiration | Hemodynamically stable women and serum hCG level >2000 mIU/ml or if <2000 mIU/ml with abnormally rising levels <66% in 48 h and no evidence of IUP or EP on TVS by the Radiology Department. Exclusion: sonographic evidence of EP or IUP including a gestational sac, heavy vaginal bleeding suggestive of passage of ‘tissue,’ or inability to tolerate an outpatient MVA | Prospective cohort | IUP: villi at histology EP: nr |
| First author (year) . | Serum hCG test . | PUL population . | Study type . | Outcome definitions and reference tests . |
|---|---|---|---|---|
| Single serum hCG cut-off level | ||||
| Hajenius et al. (1995) | hCG >1000 IU/l | Clinical suspicion of EP, i.e. vaginal bleeding with/without abdominal pain and/or risk factors and patients without symptoms or risk factors. Without clinical symptoms of shock No visible pregnancy on TVS Serum hCG <1500 IU/L | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and uneventful decrease of hCG |
| Kaplan et al. (1996) | hCG <1000 mIU/ml | Inconclusive diagnosis by TVS and abdominal ultrasound: no evidence of IUP or EP | Prospective cohort | IUP: confirmed by TVS or villi after D&C EP: confirmed at laparoscopy or laparotomy |
| Dart et al. (1997) | hCG >3000 mIU/ml Menstrual days >38 | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | Normal IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS and villi at pathology, no villi after D&C with hCG falling to zero or hCG falling to zero without intervention |
| Dart and Howard (1998) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Dart et al. (1999a) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: empty endometrial cavity and no adnexal or cul-de-sac findings. Exclusion: lost to follow-up, endometrial stripe thickness not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Mol et al. (1998) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No IUP at TVS and no ectopic mass or fluid in pouch of Douglas | Prospective cohort study | IUP: TVS confirmation at 12 weeks EP: laparoscopy Nonviable pregnancy: non viable IUP and chemical pregnancies, resolved without treatment |
| Dart et al. (2002) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: prior TVS showed IUP, passed definitive product of conception, status post-D&C, recent delivery or lost to follow-up | Prospective observational cohort study | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after D&C or systemic MTX or negative D&C |
| Condous et al. (2005a) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational study | IUP: presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| El Bishry and Ganta (2008) | P <16 nmol/l and hCG >25 IU/l P = 16–80 nmol/l and hCG >25 IU/l P >80 nmol/l and hCG <1000 IU/l P >80 nmol/l and hCG >1000 IU/l | Inconclusive scan | Retrospective cohort study | Viable IUP Criterion standard diagnosis of IUP, EP or miscarriage, not further specified |
| Shaunik et al. (2011) | hCG <2000 mIU/ml | Non-viable PUL: clinically stable, initial hCG >2000 mIU/ml and non-diagnostic ultrasound or abnormal rise/fall/plateau with initial hCG <2000 mIU/ml | Cohort study | IUP = non-viable IUP: histopathology after curettage or resolution of hCG after curettage EP: histopathology at surgery or TVS ectopic gestational sac or rise in hCG after curettage without villi at pathology |
| Serum hCG ratio | ||||
| Ankum et al. (1995) | Initial hCG <1500, hCG ratio | No pregnancy detectable at TVS and hCG <1500 IU/l | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and decrease of hCG with the disappearance of symptoms |
| Dart et al. (1999b) | hCG increase <66% hCG decrease <50% | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate. Second serum hCG performed within 7 days of first visit and before D&C or laparoscopy or MTX. Exclusion: lost to follow-up | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after negative D&C or treated with systemic MTX or EP visualized on TVS Abnormal IUP: (1) hCG >3000 mIU/ml with an empty uterus, decreasing hCG or progesterone <5.0 ng/ml before D&C and villi after D&C. (2) Villi after D&C and hCG falling to zero without intervention and (3) hCG values falling to zero without intervention |
| Condous et al. (2004) | Logistic regression model M1 (hCG ratio >0.21) | Women with abdominal pain, vaginal blood loss or to determine gestational age. No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational cohort study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: initial progesterone <20 nmol/l and spontaneous resolution of pregnancy: decrease of hCG <5 with the disappearance of symptoms |
| Bignardi et al. (2008) | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective observational cohort | IUP: gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Logistic regression model | ||||
| Gevaert et al. (2006) | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | PUL not further specified | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| Kirk et al. (2006) | Logistic regression model based on hCG ratio, prediction by nurse practitioner and costs | No evidence of an IUP or EP on TVS. Exclusion criteria: visualization of an intrauterine gestational sac with or without a fetal pole, adnexal mass thought to be an EP, heterogeneous tissue in endometrial cavity and hemodynamic instability or pain, or hemoperitoneum on TVS | Prospective non-interventional observational study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later, the presence of gestational sac eccentrically placed in the endometrial cavity or heterogeneous tissue in the cavity. EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/L with the disappearance of pregnancy symptoms |
| Condous et al. (2007a) | Logistic regression model M4 hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | No signs of an IUP, an EP or retained products of conception at TVS | Prospective cohort study | IUP: intrauterine gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Kirk et al. (2007) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No evidence of an IUP or EP on TVS, hCG level <10 000 IU/l, clinically stable and no signs of hemoperitoneum on TVS | Prospective interventional study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/l with the disappearance of pregnancy symptoms |
| Condous et al. (2007b) | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity, TVS 2 weeks later to confirm viability EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Barnhart et al. (2010) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | Women with lower abdominal pain, vaginal bleeding, maternal anxiety or confirmation of gestational age. PUL if there was no evidence of an IUP or EP on TVS | Retrospective cohort study | IUP: rise hCG in 48 h >66% and TVS 2 weeks later: the presence of gestational sac eccentrically placed in the endometrial cavity EP: histological confirmation of villi in the tube or echogenicity consistent with an EP Spontaneous miscarriage/failing PUL: spontaneous resolution of pregnancy with the decrease of hCG level <5 U/l |
| Other strategies | ||||
| Condous et al. (2005b) | Single visit protocol: high-risk PUL Prog 5–81 nmol/l or hCG >50 IU/l | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test | Retrospective protocol development, followed by prospective trial | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL Failing PUL: persistent PUL and falling hCG levels |
| Condous et al. (2006) | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test. Clinically stable women | Prospective observational cohort study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL |
| Rivera et al. (2009) | hCG decrease <50% after manual vacuum aspiration | Hemodynamically stable women and serum hCG level >2000 mIU/ml or if <2000 mIU/ml with abnormally rising levels <66% in 48 h and no evidence of IUP or EP on TVS by the Radiology Department. Exclusion: sonographic evidence of EP or IUP including a gestational sac, heavy vaginal bleeding suggestive of passage of ‘tissue,’ or inability to tolerate an outpatient MVA | Prospective cohort | IUP: villi at histology EP: nr |
IUP, intrauterine pregnancy; TVS, transvaginal sonography; EP, ectopic pregnancy; PUL, pregnancy of unknown location; TIR, trophoblast in regression; D&C, dilatation and curettage; MTX, methotrexate; na, not applicable; nr, not reported.
Characteristics of the 23 included studies in a systematic review of the diagnostic value of serum hCG on the outcome of pregnancy of unknown location (PUL).
| First author (year) . | Serum hCG test . | PUL population . | Study type . | Outcome definitions and reference tests . |
|---|---|---|---|---|
| Single serum hCG cut-off level | ||||
| Hajenius et al. (1995) | hCG >1000 IU/l | Clinical suspicion of EP, i.e. vaginal bleeding with/without abdominal pain and/or risk factors and patients without symptoms or risk factors. Without clinical symptoms of shock No visible pregnancy on TVS Serum hCG <1500 IU/L | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and uneventful decrease of hCG |
| Kaplan et al. (1996) | hCG <1000 mIU/ml | Inconclusive diagnosis by TVS and abdominal ultrasound: no evidence of IUP or EP | Prospective cohort | IUP: confirmed by TVS or villi after D&C EP: confirmed at laparoscopy or laparotomy |
| Dart et al. (1997) | hCG >3000 mIU/ml Menstrual days >38 | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | Normal IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS and villi at pathology, no villi after D&C with hCG falling to zero or hCG falling to zero without intervention |
| Dart and Howard (1998) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Dart et al. (1999a) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: empty endometrial cavity and no adnexal or cul-de-sac findings. Exclusion: lost to follow-up, endometrial stripe thickness not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Mol et al. (1998) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No IUP at TVS and no ectopic mass or fluid in pouch of Douglas | Prospective cohort study | IUP: TVS confirmation at 12 weeks EP: laparoscopy Nonviable pregnancy: non viable IUP and chemical pregnancies, resolved without treatment |
| Dart et al. (2002) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: prior TVS showed IUP, passed definitive product of conception, status post-D&C, recent delivery or lost to follow-up | Prospective observational cohort study | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after D&C or systemic MTX or negative D&C |
| Condous et al. (2005a) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational study | IUP: presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| El Bishry and Ganta (2008) | P <16 nmol/l and hCG >25 IU/l P = 16–80 nmol/l and hCG >25 IU/l P >80 nmol/l and hCG <1000 IU/l P >80 nmol/l and hCG >1000 IU/l | Inconclusive scan | Retrospective cohort study | Viable IUP Criterion standard diagnosis of IUP, EP or miscarriage, not further specified |
| Shaunik et al. (2011) | hCG <2000 mIU/ml | Non-viable PUL: clinically stable, initial hCG >2000 mIU/ml and non-diagnostic ultrasound or abnormal rise/fall/plateau with initial hCG <2000 mIU/ml | Cohort study | IUP = non-viable IUP: histopathology after curettage or resolution of hCG after curettage EP: histopathology at surgery or TVS ectopic gestational sac or rise in hCG after curettage without villi at pathology |
| Serum hCG ratio | ||||
| Ankum et al. (1995) | Initial hCG <1500, hCG ratio | No pregnancy detectable at TVS and hCG <1500 IU/l | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and decrease of hCG with the disappearance of symptoms |
| Dart et al. (1999b) | hCG increase <66% hCG decrease <50% | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate. Second serum hCG performed within 7 days of first visit and before D&C or laparoscopy or MTX. Exclusion: lost to follow-up | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after negative D&C or treated with systemic MTX or EP visualized on TVS Abnormal IUP: (1) hCG >3000 mIU/ml with an empty uterus, decreasing hCG or progesterone <5.0 ng/ml before D&C and villi after D&C. (2) Villi after D&C and hCG falling to zero without intervention and (3) hCG values falling to zero without intervention |
| Condous et al. (2004) | Logistic regression model M1 (hCG ratio >0.21) | Women with abdominal pain, vaginal blood loss or to determine gestational age. No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational cohort study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: initial progesterone <20 nmol/l and spontaneous resolution of pregnancy: decrease of hCG <5 with the disappearance of symptoms |
| Bignardi et al. (2008) | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective observational cohort | IUP: gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Logistic regression model | ||||
| Gevaert et al. (2006) | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | PUL not further specified | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| Kirk et al. (2006) | Logistic regression model based on hCG ratio, prediction by nurse practitioner and costs | No evidence of an IUP or EP on TVS. Exclusion criteria: visualization of an intrauterine gestational sac with or without a fetal pole, adnexal mass thought to be an EP, heterogeneous tissue in endometrial cavity and hemodynamic instability or pain, or hemoperitoneum on TVS | Prospective non-interventional observational study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later, the presence of gestational sac eccentrically placed in the endometrial cavity or heterogeneous tissue in the cavity. EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/L with the disappearance of pregnancy symptoms |
| Condous et al. (2007a) | Logistic regression model M4 hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | No signs of an IUP, an EP or retained products of conception at TVS | Prospective cohort study | IUP: intrauterine gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Kirk et al. (2007) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No evidence of an IUP or EP on TVS, hCG level <10 000 IU/l, clinically stable and no signs of hemoperitoneum on TVS | Prospective interventional study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/l with the disappearance of pregnancy symptoms |
| Condous et al. (2007b) | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity, TVS 2 weeks later to confirm viability EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Barnhart et al. (2010) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | Women with lower abdominal pain, vaginal bleeding, maternal anxiety or confirmation of gestational age. PUL if there was no evidence of an IUP or EP on TVS | Retrospective cohort study | IUP: rise hCG in 48 h >66% and TVS 2 weeks later: the presence of gestational sac eccentrically placed in the endometrial cavity EP: histological confirmation of villi in the tube or echogenicity consistent with an EP Spontaneous miscarriage/failing PUL: spontaneous resolution of pregnancy with the decrease of hCG level <5 U/l |
| Other strategies | ||||
| Condous et al. (2005b) | Single visit protocol: high-risk PUL Prog 5–81 nmol/l or hCG >50 IU/l | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test | Retrospective protocol development, followed by prospective trial | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL Failing PUL: persistent PUL and falling hCG levels |
| Condous et al. (2006) | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test. Clinically stable women | Prospective observational cohort study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL |
| Rivera et al. (2009) | hCG decrease <50% after manual vacuum aspiration | Hemodynamically stable women and serum hCG level >2000 mIU/ml or if <2000 mIU/ml with abnormally rising levels <66% in 48 h and no evidence of IUP or EP on TVS by the Radiology Department. Exclusion: sonographic evidence of EP or IUP including a gestational sac, heavy vaginal bleeding suggestive of passage of ‘tissue,’ or inability to tolerate an outpatient MVA | Prospective cohort | IUP: villi at histology EP: nr |
| First author (year) . | Serum hCG test . | PUL population . | Study type . | Outcome definitions and reference tests . |
|---|---|---|---|---|
| Single serum hCG cut-off level | ||||
| Hajenius et al. (1995) | hCG >1000 IU/l | Clinical suspicion of EP, i.e. vaginal bleeding with/without abdominal pain and/or risk factors and patients without symptoms or risk factors. Without clinical symptoms of shock No visible pregnancy on TVS Serum hCG <1500 IU/L | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and uneventful decrease of hCG |
| Kaplan et al. (1996) | hCG <1000 mIU/ml | Inconclusive diagnosis by TVS and abdominal ultrasound: no evidence of IUP or EP | Prospective cohort | IUP: confirmed by TVS or villi after D&C EP: confirmed at laparoscopy or laparotomy |
| Dart et al. (1997) | hCG >3000 mIU/ml Menstrual days >38 | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | Normal IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS and villi at pathology, no villi after D&C with hCG falling to zero or hCG falling to zero without intervention |
| Dart and Howard (1998) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: status post-D&C, recent delivery, definitive diagnosis not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Dart et al. (1999a) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: empty endometrial cavity and no adnexal or cul-de-sac findings. Exclusion: lost to follow-up, endometrial stripe thickness not determined | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy and confirmed by histology Abnormal IUP: abnormal sac on TVS or hCG >3000 mIU/ml without an intrauterine sac or villi after D&C or hCG falling to zero without intervention |
| Mol et al. (1998) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No IUP at TVS and no ectopic mass or fluid in pouch of Douglas | Prospective cohort study | IUP: TVS confirmation at 12 weeks EP: laparoscopy Nonviable pregnancy: non viable IUP and chemical pregnancies, resolved without treatment |
| Dart et al. (2002) | hCG <1000 mIU/ml | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate: no evidence of IUP or EP Exclusion: prior TVS showed IUP, passed definitive product of conception, status post-D&C, recent delivery or lost to follow-up | Prospective observational cohort study | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after D&C or systemic MTX or negative D&C |
| Condous et al. (2005a) | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational study | IUP: presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| El Bishry and Ganta (2008) | P <16 nmol/l and hCG >25 IU/l P = 16–80 nmol/l and hCG >25 IU/l P >80 nmol/l and hCG <1000 IU/l P >80 nmol/l and hCG >1000 IU/l | Inconclusive scan | Retrospective cohort study | Viable IUP Criterion standard diagnosis of IUP, EP or miscarriage, not further specified |
| Shaunik et al. (2011) | hCG <2000 mIU/ml | Non-viable PUL: clinically stable, initial hCG >2000 mIU/ml and non-diagnostic ultrasound or abnormal rise/fall/plateau with initial hCG <2000 mIU/ml | Cohort study | IUP = non-viable IUP: histopathology after curettage or resolution of hCG after curettage EP: histopathology at surgery or TVS ectopic gestational sac or rise in hCG after curettage without villi at pathology |
| Serum hCG ratio | ||||
| Ankum et al. (1995) | Initial hCG <1500, hCG ratio | No pregnancy detectable at TVS and hCG <1500 IU/l | Prospective cohort | IUP: confirmed on TVS EP: laparoscopy or laparotomy TIR: PUL and decrease of hCG with the disappearance of symptoms |
| Dart et al. (1999b) | hCG increase <66% hCG decrease <50% | Abdominal pain or vaginal bleeding and positive serum hCG. TVS indeterminate. Second serum hCG performed within 7 days of first visit and before D&C or laparoscopy or MTX. Exclusion: lost to follow-up | Retrospective cohort | IUP: positive heartbeat on TVS or delivery child EP: laparoscopy or hCG increases or plateau after negative D&C or treated with systemic MTX or EP visualized on TVS Abnormal IUP: (1) hCG >3000 mIU/ml with an empty uterus, decreasing hCG or progesterone <5.0 ng/ml before D&C and villi after D&C. (2) Villi after D&C and hCG falling to zero without intervention and (3) hCG values falling to zero without intervention |
| Condous et al. (2004) | Logistic regression model M1 (hCG ratio >0.21) | Women with abdominal pain, vaginal blood loss or to determine gestational age. No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or hemoperitoneum | Prospective observational cohort study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: initial progesterone <20 nmol/l and spontaneous resolution of pregnancy: decrease of hCG <5 with the disappearance of symptoms |
| Bignardi et al. (2008) | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective observational cohort | IUP: gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Logistic regression model | ||||
| Gevaert et al. (2006) | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | PUL not further specified | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: persistent PUL and falling hCG levels |
| Kirk et al. (2006) | Logistic regression model based on hCG ratio, prediction by nurse practitioner and costs | No evidence of an IUP or EP on TVS. Exclusion criteria: visualization of an intrauterine gestational sac with or without a fetal pole, adnexal mass thought to be an EP, heterogeneous tissue in endometrial cavity and hemodynamic instability or pain, or hemoperitoneum on TVS | Prospective non-interventional observational study | IUP: hCG ratio over 48 h >66% and TVS 2 weeks later, the presence of gestational sac eccentrically placed in the endometrial cavity or heterogeneous tissue in the cavity. EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/L with the disappearance of pregnancy symptoms |
| Condous et al. (2007a) | Logistic regression model M4 hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | No signs of an IUP, an EP or retained products of conception at TVS | Prospective cohort study | IUP: intrauterine gestational sac confirmed at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Kirk et al. (2007) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No evidence of an IUP or EP on TVS, hCG level <10 000 IU/l, clinically stable and no signs of hemoperitoneum on TVS | Prospective interventional study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with histology of chorionic villi or persistent PUL Failing PUL: spontaneous decrease of hCG level <5 U/l with the disappearance of pregnancy symptoms |
| Condous et al. (2007b) | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | No signs of an IUP, an EP or retained products of conception at TVS. Exclusion: clinically unstable or acute abdomen or blood in pouch of Douglas according to TVS | Prospective cohort study | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity, TVS 2 weeks later to confirm viability EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi Failing PUL: progesterone <20 nmol/l at presentation + fall in serum hCG <5 IU/L |
| Barnhart et al. (2010) | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | Women with lower abdominal pain, vaginal bleeding, maternal anxiety or confirmation of gestational age. PUL if there was no evidence of an IUP or EP on TVS | Retrospective cohort study | IUP: rise hCG in 48 h >66% and TVS 2 weeks later: the presence of gestational sac eccentrically placed in the endometrial cavity EP: histological confirmation of villi in the tube or echogenicity consistent with an EP Spontaneous miscarriage/failing PUL: spontaneous resolution of pregnancy with the decrease of hCG level <5 U/l |
| Other strategies | ||||
| Condous et al. (2005b) | Single visit protocol: high-risk PUL Prog 5–81 nmol/l or hCG >50 IU/l | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test | Retrospective protocol development, followed by prospective trial | IUP: the presence of gestational sac eccentrically placed in the endometrial cavity EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL Failing PUL: persistent PUL and falling hCG levels |
| Condous et al. (2006) | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | No signs of an IUP, an EP or retained products of conception at TVS in women with a positive urinary pregnancy test. Clinically stable women | Prospective observational cohort study | IUP: intrauterine gestational sac ± fetal pole ± cardiac activity, or heterogeneous tissue within endometrial cavity suggestive of retained products of conception at TVS EP: TVS blob sign, bagel sign, ectopic gestational sac with/without cardiac activity and/or laparoscopy with the histology of chorionic villi or persistent PUL |
| Rivera et al. (2009) | hCG decrease <50% after manual vacuum aspiration | Hemodynamically stable women and serum hCG level >2000 mIU/ml or if <2000 mIU/ml with abnormally rising levels <66% in 48 h and no evidence of IUP or EP on TVS by the Radiology Department. Exclusion: sonographic evidence of EP or IUP including a gestational sac, heavy vaginal bleeding suggestive of passage of ‘tissue,’ or inability to tolerate an outpatient MVA | Prospective cohort | IUP: villi at histology EP: nr |
IUP, intrauterine pregnancy; TVS, transvaginal sonography; EP, ectopic pregnancy; PUL, pregnancy of unknown location; TIR, trophoblast in regression; D&C, dilatation and curettage; MTX, methotrexate; na, not applicable; nr, not reported.
In all studies the definition of PUL was at least a positive pregnancy test and an inconclusive TVS in hemodynamically stable women. Five studies strictly specified the inclusion criteria to women with vaginal blood loss and/or abdominal pain. The other studies included women with PUL, either with vaginal blood loss and/or abdominal pain and/or risk factors for EP and women who came in for first trimester screening without symptoms or risk factors but with an uncertain gestational age. Further specific inclusion criteria among studies were serum hCG cut-off levels varying between 1500 and 10 000 IU/l and an abnormal rise/fall/plateau of serum hCG with an with initial hCG <2000 IU/l.
Of the 23 included studies, 15 were prospective cohort studies and eight were retrospective cohort studies. Not all studies reported on all pregnancy outcomes as the reference test. IUP was variously described as an intrauterine gestational sac, an abnormal sac on TVS, histological confirmation of villi after uterine curettage, spontaneously declining serum hCG without intervention (biochemical pregnancies), fetal heartbeat upon TVS or delivery of a child. Only four studies (from the same author) reported both viable and non-viable IUP separately in the same cohort (Dart et al., 1997, 1999a, b; Dart and Howard, 1998).
For the outcome EP, a composite reference test was used, i.e. confirmation by laparoscopy and additional histology or an ultrasound diagnosis or specific serum hCG cut-off levels. Ultrasound diagnosis ranged from some free fluid in the pouch of Douglas, an inhomogeneous mass adjacent to the ovary, and moving separately from the ovary (blob sign), a mass with a hyper-echoic ring around the gestational sac (bagel sign) (Condous et al., 2005c) to an ectopic gestational sac with or without fetal cardiac activity. Other criteria used to define the outcome as EP were rising or plateauing serum hCG levels after uterine curettage, negative histopathology after uterine curettage, or plateauing serum hCG levels for which systemic MTX was used.
Some studies reported other pregnancy outcomes, such as trophoblast in regression (TIR), failing PUL or miscarriage.
The quality assessment tool (QUADAS) for the included studies is shown in Table II, and from this table it becomes clear that all studies were prone to potential bias. All studies used diagnostic strategies that include the outcome of the serum hCG to determine the type of reference test, e.g. laparoscopy in case of certain serum hCG cut-offs. Thus, the reference standard was not the same for all patients regardless of the index test (differential verification bias) and the reference standard was not independent of the index test (incorporation bias). For the same reason the results of the reference standard were not interpreted without knowledge of the results of the index test (blinding or review bias).
QUADAS for the included studies.
| . | Was the spectrum of patients' representative of patients in practice? Spectrum bias . | Were selection criteria clearly described? . | Is the reference standard likely to correctly classify the target condition? . | Did the whole study population receive verification of diagnosis? Selection bias . | Did patients receive the same reference standard regardless of the index test result? Differential verification bias . | Was the reference standard independent of the index test? (e.g. not measured in same test/session) Incorporation bias . | Was the execution of the index test described in sufficient detail to permit replication of the test? . | Was the execution of the reference standard described in sufficient detail to permit its replication? . | Were the reference standard results interpreted without knowledge of the results of the index test? Blinding or review bias . | Were the same clinical data available when test results were interpreted as would be available when the test is used in practice? . | Were uninterpretable/intermediate test results reported? . | Were withdrawals from the study explained? . |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Hajenius et al. (1995) | Y | Y | Y | Y | N | Y | Y | Y | N | Y | Y | Y |
| Kaplan et al. (1996) | Y | Y | Y | Y | U | Y | Y | Y | U | Y | Y | Y |
| Dart et al. (1997) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart and Howard (1998) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart et al. (1999a) | Y | Y | Y | Y | N | Y | Y | Y | U | Y | Y | Y |
| Mol et al. (1998) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (2002) | Y | Y | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Condous et al. (2005a) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| El Bishry and Ganta (2008) | Y | Y | Y | Y | U | N | Y | Y | U | Y | Y | N |
| Shaunik et al. (2011) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | N |
| Ankum et al. (1995) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (1999b) | Y | Y | Y | Y | U | U | Y | Y | Y | Y | Y | Y |
| Condous et al. (2004) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Bignardi et al. (2008) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Gevaert et al. (2006) | Y | N | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | U | Y | Y | Y |
| Condous et al. (2007a) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2007) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2007b) | Y | Y | Y | Y | N | N | Y | Y | N | U | Y | Y |
| Barnhart et al. (2010) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2005b) | Y | Y | Y | Y | N | U | Y | Y | N | Y | Y | Y |
| Condous et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Rivera et al. (2009) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | Y |
| . | Was the spectrum of patients' representative of patients in practice? Spectrum bias . | Were selection criteria clearly described? . | Is the reference standard likely to correctly classify the target condition? . | Did the whole study population receive verification of diagnosis? Selection bias . | Did patients receive the same reference standard regardless of the index test result? Differential verification bias . | Was the reference standard independent of the index test? (e.g. not measured in same test/session) Incorporation bias . | Was the execution of the index test described in sufficient detail to permit replication of the test? . | Was the execution of the reference standard described in sufficient detail to permit its replication? . | Were the reference standard results interpreted without knowledge of the results of the index test? Blinding or review bias . | Were the same clinical data available when test results were interpreted as would be available when the test is used in practice? . | Were uninterpretable/intermediate test results reported? . | Were withdrawals from the study explained? . |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Hajenius et al. (1995) | Y | Y | Y | Y | N | Y | Y | Y | N | Y | Y | Y |
| Kaplan et al. (1996) | Y | Y | Y | Y | U | Y | Y | Y | U | Y | Y | Y |
| Dart et al. (1997) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart and Howard (1998) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart et al. (1999a) | Y | Y | Y | Y | N | Y | Y | Y | U | Y | Y | Y |
| Mol et al. (1998) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (2002) | Y | Y | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Condous et al. (2005a) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| El Bishry and Ganta (2008) | Y | Y | Y | Y | U | N | Y | Y | U | Y | Y | N |
| Shaunik et al. (2011) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | N |
| Ankum et al. (1995) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (1999b) | Y | Y | Y | Y | U | U | Y | Y | Y | Y | Y | Y |
| Condous et al. (2004) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Bignardi et al. (2008) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Gevaert et al. (2006) | Y | N | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | U | Y | Y | Y |
| Condous et al. (2007a) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2007) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2007b) | Y | Y | Y | Y | N | N | Y | Y | N | U | Y | Y |
| Barnhart et al. (2010) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2005b) | Y | Y | Y | Y | N | U | Y | Y | N | Y | Y | Y |
| Condous et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Rivera et al. (2009) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | Y |
Y, yes; N, no; U, unclear.
QUADAS for the included studies.
| . | Was the spectrum of patients' representative of patients in practice? Spectrum bias . | Were selection criteria clearly described? . | Is the reference standard likely to correctly classify the target condition? . | Did the whole study population receive verification of diagnosis? Selection bias . | Did patients receive the same reference standard regardless of the index test result? Differential verification bias . | Was the reference standard independent of the index test? (e.g. not measured in same test/session) Incorporation bias . | Was the execution of the index test described in sufficient detail to permit replication of the test? . | Was the execution of the reference standard described in sufficient detail to permit its replication? . | Were the reference standard results interpreted without knowledge of the results of the index test? Blinding or review bias . | Were the same clinical data available when test results were interpreted as would be available when the test is used in practice? . | Were uninterpretable/intermediate test results reported? . | Were withdrawals from the study explained? . |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Hajenius et al. (1995) | Y | Y | Y | Y | N | Y | Y | Y | N | Y | Y | Y |
| Kaplan et al. (1996) | Y | Y | Y | Y | U | Y | Y | Y | U | Y | Y | Y |
| Dart et al. (1997) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart and Howard (1998) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart et al. (1999a) | Y | Y | Y | Y | N | Y | Y | Y | U | Y | Y | Y |
| Mol et al. (1998) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (2002) | Y | Y | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Condous et al. (2005a) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| El Bishry and Ganta (2008) | Y | Y | Y | Y | U | N | Y | Y | U | Y | Y | N |
| Shaunik et al. (2011) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | N |
| Ankum et al. (1995) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (1999b) | Y | Y | Y | Y | U | U | Y | Y | Y | Y | Y | Y |
| Condous et al. (2004) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Bignardi et al. (2008) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Gevaert et al. (2006) | Y | N | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | U | Y | Y | Y |
| Condous et al. (2007a) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2007) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2007b) | Y | Y | Y | Y | N | N | Y | Y | N | U | Y | Y |
| Barnhart et al. (2010) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2005b) | Y | Y | Y | Y | N | U | Y | Y | N | Y | Y | Y |
| Condous et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Rivera et al. (2009) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | Y |
| . | Was the spectrum of patients' representative of patients in practice? Spectrum bias . | Were selection criteria clearly described? . | Is the reference standard likely to correctly classify the target condition? . | Did the whole study population receive verification of diagnosis? Selection bias . | Did patients receive the same reference standard regardless of the index test result? Differential verification bias . | Was the reference standard independent of the index test? (e.g. not measured in same test/session) Incorporation bias . | Was the execution of the index test described in sufficient detail to permit replication of the test? . | Was the execution of the reference standard described in sufficient detail to permit its replication? . | Were the reference standard results interpreted without knowledge of the results of the index test? Blinding or review bias . | Were the same clinical data available when test results were interpreted as would be available when the test is used in practice? . | Were uninterpretable/intermediate test results reported? . | Were withdrawals from the study explained? . |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Hajenius et al. (1995) | Y | Y | Y | Y | N | Y | Y | Y | N | Y | Y | Y |
| Kaplan et al. (1996) | Y | Y | Y | Y | U | Y | Y | Y | U | Y | Y | Y |
| Dart et al. (1997) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart and Howard (1998) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Dart et al. (1999a) | Y | Y | Y | Y | N | Y | Y | Y | U | Y | Y | Y |
| Mol et al. (1998) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (2002) | Y | Y | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Condous et al. (2005a) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| El Bishry and Ganta (2008) | Y | Y | Y | Y | U | N | Y | Y | U | Y | Y | N |
| Shaunik et al. (2011) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | N |
| Ankum et al. (1995) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Dart et al. (1999b) | Y | Y | Y | Y | U | U | Y | Y | Y | Y | Y | Y |
| Condous et al. (2004) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Bignardi et al. (2008) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Gevaert et al. (2006) | Y | N | Y | Y | N | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | U | Y | Y | Y |
| Condous et al. (2007a) | Y | Y | Y | Y | U | U | Y | Y | U | Y | Y | Y |
| Kirk et al. (2007) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2007b) | Y | Y | Y | Y | N | N | Y | Y | N | U | Y | Y |
| Barnhart et al. (2010) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Condous et al. (2005b) | Y | Y | Y | Y | N | U | Y | Y | N | Y | Y | Y |
| Condous et al. (2006) | Y | Y | Y | Y | N | N | Y | Y | N | Y | Y | Y |
| Rivera et al. (2009) | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | Y |
Y, yes; N, no; U, unclear.
Diagnostic performance of serum hCG in PUL
Sensitivities and specificities, as calculated from each study reporting on serum hCG, are reported for each pregnancy outcome in Table III. We intended to perform a meta-analysis if the same diagnostic serum hCG strategy and the same outcome definition was reported per pregnancy outcome. For the outcome IUP there was sufficient clinical heterogeneity between studies (being either any form of IUP at TVS or specific viable or non-viable IUP) that forest plots or sROC plots would not be informative. Other pregnancy outcomes, such as TIR or failing PUL, were only reported in a few studies and, when reported, the studies did not perform the same diagnostic test. Only the pregnancy outcome EP was reported more consistently, in terms of outcome definition, the reference test and reported data (2 × 2 tables) to allow meta-analysis.
The performance of serum hCG in diagnosing pregnancy outcome in women with PUL.
| First author (year) . | n . | Serum hCG strategy . | Pregnancy outcomes . | ||
|---|---|---|---|---|---|
| IUP (sensitivity/specificity) . | EP (sensitivity/specificity) . | Other (sensitivity/specificity) . | |||
| Single serum hCG cut-off level | |||||
| Hajenius et al. (1995) | 265 | hCG >1000 IU/l | 0.95/0.33 | 0.90/0.98 | 0.58/1.0 |
| Kaplan et al. (1996) | 72 | hCG <1000 mIU/ml | 0.27/0.64 | 0.67/0.74 | nr |
| Dart et al. (1997) | 194 | hCG >3000 mIU/ml Menstrual days >38 | 0.00/0.55 0.29/0.13 | 0.26/0.57 0.70/0.16 | 0.48/0.84 0.90/0.44 |
| Dart and Howard (1998) | 147 | hCG <1000 mIU/ml | nr | 0.48/0.55 | nr |
| Dart et al. (1999a) | 224 | hCG <1000 mIU/ml | 0.91/0.41 | 0.64/0.40 | 0.52/0.41 |
| Mol et al. (1998) | 262 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | 0.20/0.80 0.00/0.83 0.00/0.86 | 0.43/0.86 0.40/0.96 0.38/0.98 | 0.11/0.69 0.06/0.81 0.02/0.81 |
| Dart et al. (2002) | 420 | hCG <1000 mIU/ml | nr | 0.86/0.43 | nr |
| Condous et al. (2005a) | 569 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | nr | 0.22/0.87 0.15/0.93 0.11/0.95 | nr |
| El Bishry and Ganta (2008) | 126 | Progesterone <16 nmol/l and hCG >25 IU/l Progesterone 16–80 nmol/l and hCG >25 IU/l Progesterone >80 nmol/l and hCG <1000 IU/l Progesterone >80 nmol/l and hCG >1000 IU/l | 0.03/0.44 0.71/0.57 0.03/1.0 0.23/0.99 | 0.44/0.60 0.53/0.50 Na/0.99 0.03/0.91 | nr |
| Shaunik et al. (2011) | 173 | hCG <2000 mIU/ml | 0.61/0.13 | 0.87/0.39 | na |
| Serum hCG ratio | |||||
| Ankum et al. (1995) | 85 | Initial hCG <1500, hCG ratio | Nr | 1.0/0.97 | nr |
| Dart et al. (1999b) | 307 | hCG increase <66% hCG decrease <50% | 0.25/0.80 0.00/0.67 | 0.74/0.50 0.80/0.59 | 0.15/0.65 0.34/0.91 |
| Condous et al. (2004) | 388 | Logistic regression model M1 (cut-off hCG ratio of 0.21 for EP; cut-off hCG ratio of 0.72 for failing PUL) | Training set: 0.86/0.98 Test set: 0.81/0.98 | Training set: 0.75/0.89 Test set: 0.83/0.88 | Training set: 0.89/0.95 Test set: 0.90/0.98 |
| Bignardi et al. (2008) | 940 | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | 1.0/0.73 0.07/0.09 0.23/0.05 | 0.85/0.55 0.85/0.36 0.92/0.28 | 0.11/0.03 0.98/0.76 0.98/0.58 |
| Logistic regression model | |||||
| Gevaert et al. (2006) | 856 | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | nr | 0.77/0.83 0.77/0.80 | nr |
| Kirk et al. (2006) | 357 | Logistic regression model based on hCG ratio and prediction by nurse practitioner | 0.89/0.78 | 0.76/0.84 | 0.78/0.87 |
| Condous et al. (2007a) | 376 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | 0.86/0.96 Training set: 0.73/0.97 Test set: 0.86/0.97 | 0.80/0.89 Training set: 0.92/0.94 Test set: 0.79/0.90 | 0.87/0.98 Training set: 0.97/0.98 Test set: 0.90/0.97 |
| Kirk et al. (2007) | 363 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.95/0.90 | 0.31/0.98 | 0.99/0.94 |
| Condous et al. (2007b) | 376 | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.86/0.95 Training set: 0.79/0.98 Test set: 0.86/0.96 | 0.73/0.87 Training set: 0.92/0.91 Test set: 0.80/0.89 | 0.86/0.99 Training set: 0.97/0.98 Test set: 0.87/0.98 |
| Barnhart et al. (2010) | 1035 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | UK cohort: 0.88/0.97 US cohort: 0.84/0.93 | UK cohort: 0.81/0.89 US cohort: 0.49/0.87 | UK cohort: 0.88/0.99 US cohort: 0.81/0.83 |
| Other strategies | |||||
| Condous et al. (2005b) | 518 | Single visit protocol: High-risk PUL progesterone 5–81 nmol/l or hCG >50 IU/l | nr | Training set 0.77/0.81 Test set 0.84/0.33 | nr |
| Condous et al. (2006) | 1003 | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | nr | 0.52/nr | nr |
| Rivera et al. (2009) | 22 | hCG decrease <50% after manual vacuum aspiration | na | 1.0/0.92 | na |
| First author (year) . | n . | Serum hCG strategy . | Pregnancy outcomes . | ||
|---|---|---|---|---|---|
| IUP (sensitivity/specificity) . | EP (sensitivity/specificity) . | Other (sensitivity/specificity) . | |||
| Single serum hCG cut-off level | |||||
| Hajenius et al. (1995) | 265 | hCG >1000 IU/l | 0.95/0.33 | 0.90/0.98 | 0.58/1.0 |
| Kaplan et al. (1996) | 72 | hCG <1000 mIU/ml | 0.27/0.64 | 0.67/0.74 | nr |
| Dart et al. (1997) | 194 | hCG >3000 mIU/ml Menstrual days >38 | 0.00/0.55 0.29/0.13 | 0.26/0.57 0.70/0.16 | 0.48/0.84 0.90/0.44 |
| Dart and Howard (1998) | 147 | hCG <1000 mIU/ml | nr | 0.48/0.55 | nr |
| Dart et al. (1999a) | 224 | hCG <1000 mIU/ml | 0.91/0.41 | 0.64/0.40 | 0.52/0.41 |
| Mol et al. (1998) | 262 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | 0.20/0.80 0.00/0.83 0.00/0.86 | 0.43/0.86 0.40/0.96 0.38/0.98 | 0.11/0.69 0.06/0.81 0.02/0.81 |
| Dart et al. (2002) | 420 | hCG <1000 mIU/ml | nr | 0.86/0.43 | nr |
| Condous et al. (2005a) | 569 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | nr | 0.22/0.87 0.15/0.93 0.11/0.95 | nr |
| El Bishry and Ganta (2008) | 126 | Progesterone <16 nmol/l and hCG >25 IU/l Progesterone 16–80 nmol/l and hCG >25 IU/l Progesterone >80 nmol/l and hCG <1000 IU/l Progesterone >80 nmol/l and hCG >1000 IU/l | 0.03/0.44 0.71/0.57 0.03/1.0 0.23/0.99 | 0.44/0.60 0.53/0.50 Na/0.99 0.03/0.91 | nr |
| Shaunik et al. (2011) | 173 | hCG <2000 mIU/ml | 0.61/0.13 | 0.87/0.39 | na |
| Serum hCG ratio | |||||
| Ankum et al. (1995) | 85 | Initial hCG <1500, hCG ratio | Nr | 1.0/0.97 | nr |
| Dart et al. (1999b) | 307 | hCG increase <66% hCG decrease <50% | 0.25/0.80 0.00/0.67 | 0.74/0.50 0.80/0.59 | 0.15/0.65 0.34/0.91 |
| Condous et al. (2004) | 388 | Logistic regression model M1 (cut-off hCG ratio of 0.21 for EP; cut-off hCG ratio of 0.72 for failing PUL) | Training set: 0.86/0.98 Test set: 0.81/0.98 | Training set: 0.75/0.89 Test set: 0.83/0.88 | Training set: 0.89/0.95 Test set: 0.90/0.98 |
| Bignardi et al. (2008) | 940 | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | 1.0/0.73 0.07/0.09 0.23/0.05 | 0.85/0.55 0.85/0.36 0.92/0.28 | 0.11/0.03 0.98/0.76 0.98/0.58 |
| Logistic regression model | |||||
| Gevaert et al. (2006) | 856 | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | nr | 0.77/0.83 0.77/0.80 | nr |
| Kirk et al. (2006) | 357 | Logistic regression model based on hCG ratio and prediction by nurse practitioner | 0.89/0.78 | 0.76/0.84 | 0.78/0.87 |
| Condous et al. (2007a) | 376 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | 0.86/0.96 Training set: 0.73/0.97 Test set: 0.86/0.97 | 0.80/0.89 Training set: 0.92/0.94 Test set: 0.79/0.90 | 0.87/0.98 Training set: 0.97/0.98 Test set: 0.90/0.97 |
| Kirk et al. (2007) | 363 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.95/0.90 | 0.31/0.98 | 0.99/0.94 |
| Condous et al. (2007b) | 376 | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.86/0.95 Training set: 0.79/0.98 Test set: 0.86/0.96 | 0.73/0.87 Training set: 0.92/0.91 Test set: 0.80/0.89 | 0.86/0.99 Training set: 0.97/0.98 Test set: 0.87/0.98 |
| Barnhart et al. (2010) | 1035 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | UK cohort: 0.88/0.97 US cohort: 0.84/0.93 | UK cohort: 0.81/0.89 US cohort: 0.49/0.87 | UK cohort: 0.88/0.99 US cohort: 0.81/0.83 |
| Other strategies | |||||
| Condous et al. (2005b) | 518 | Single visit protocol: High-risk PUL progesterone 5–81 nmol/l or hCG >50 IU/l | nr | Training set 0.77/0.81 Test set 0.84/0.33 | nr |
| Condous et al. (2006) | 1003 | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | nr | 0.52/nr | nr |
| Rivera et al. (2009) | 22 | hCG decrease <50% after manual vacuum aspiration | na | 1.0/0.92 | na |
The performance of serum hCG in diagnosing pregnancy outcome in women with PUL.
| First author (year) . | n . | Serum hCG strategy . | Pregnancy outcomes . | ||
|---|---|---|---|---|---|
| IUP (sensitivity/specificity) . | EP (sensitivity/specificity) . | Other (sensitivity/specificity) . | |||
| Single serum hCG cut-off level | |||||
| Hajenius et al. (1995) | 265 | hCG >1000 IU/l | 0.95/0.33 | 0.90/0.98 | 0.58/1.0 |
| Kaplan et al. (1996) | 72 | hCG <1000 mIU/ml | 0.27/0.64 | 0.67/0.74 | nr |
| Dart et al. (1997) | 194 | hCG >3000 mIU/ml Menstrual days >38 | 0.00/0.55 0.29/0.13 | 0.26/0.57 0.70/0.16 | 0.48/0.84 0.90/0.44 |
| Dart and Howard (1998) | 147 | hCG <1000 mIU/ml | nr | 0.48/0.55 | nr |
| Dart et al. (1999a) | 224 | hCG <1000 mIU/ml | 0.91/0.41 | 0.64/0.40 | 0.52/0.41 |
| Mol et al. (1998) | 262 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | 0.20/0.80 0.00/0.83 0.00/0.86 | 0.43/0.86 0.40/0.96 0.38/0.98 | 0.11/0.69 0.06/0.81 0.02/0.81 |
| Dart et al. (2002) | 420 | hCG <1000 mIU/ml | nr | 0.86/0.43 | nr |
| Condous et al. (2005a) | 569 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | nr | 0.22/0.87 0.15/0.93 0.11/0.95 | nr |
| El Bishry and Ganta (2008) | 126 | Progesterone <16 nmol/l and hCG >25 IU/l Progesterone 16–80 nmol/l and hCG >25 IU/l Progesterone >80 nmol/l and hCG <1000 IU/l Progesterone >80 nmol/l and hCG >1000 IU/l | 0.03/0.44 0.71/0.57 0.03/1.0 0.23/0.99 | 0.44/0.60 0.53/0.50 Na/0.99 0.03/0.91 | nr |
| Shaunik et al. (2011) | 173 | hCG <2000 mIU/ml | 0.61/0.13 | 0.87/0.39 | na |
| Serum hCG ratio | |||||
| Ankum et al. (1995) | 85 | Initial hCG <1500, hCG ratio | Nr | 1.0/0.97 | nr |
| Dart et al. (1999b) | 307 | hCG increase <66% hCG decrease <50% | 0.25/0.80 0.00/0.67 | 0.74/0.50 0.80/0.59 | 0.15/0.65 0.34/0.91 |
| Condous et al. (2004) | 388 | Logistic regression model M1 (cut-off hCG ratio of 0.21 for EP; cut-off hCG ratio of 0.72 for failing PUL) | Training set: 0.86/0.98 Test set: 0.81/0.98 | Training set: 0.75/0.89 Test set: 0.83/0.88 | Training set: 0.89/0.95 Test set: 0.90/0.98 |
| Bignardi et al. (2008) | 940 | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | 1.0/0.73 0.07/0.09 0.23/0.05 | 0.85/0.55 0.85/0.36 0.92/0.28 | 0.11/0.03 0.98/0.76 0.98/0.58 |
| Logistic regression model | |||||
| Gevaert et al. (2006) | 856 | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | nr | 0.77/0.83 0.77/0.80 | nr |
| Kirk et al. (2006) | 357 | Logistic regression model based on hCG ratio and prediction by nurse practitioner | 0.89/0.78 | 0.76/0.84 | 0.78/0.87 |
| Condous et al. (2007a) | 376 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | 0.86/0.96 Training set: 0.73/0.97 Test set: 0.86/0.97 | 0.80/0.89 Training set: 0.92/0.94 Test set: 0.79/0.90 | 0.87/0.98 Training set: 0.97/0.98 Test set: 0.90/0.97 |
| Kirk et al. (2007) | 363 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.95/0.90 | 0.31/0.98 | 0.99/0.94 |
| Condous et al. (2007b) | 376 | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.86/0.95 Training set: 0.79/0.98 Test set: 0.86/0.96 | 0.73/0.87 Training set: 0.92/0.91 Test set: 0.80/0.89 | 0.86/0.99 Training set: 0.97/0.98 Test set: 0.87/0.98 |
| Barnhart et al. (2010) | 1035 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | UK cohort: 0.88/0.97 US cohort: 0.84/0.93 | UK cohort: 0.81/0.89 US cohort: 0.49/0.87 | UK cohort: 0.88/0.99 US cohort: 0.81/0.83 |
| Other strategies | |||||
| Condous et al. (2005b) | 518 | Single visit protocol: High-risk PUL progesterone 5–81 nmol/l or hCG >50 IU/l | nr | Training set 0.77/0.81 Test set 0.84/0.33 | nr |
| Condous et al. (2006) | 1003 | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | nr | 0.52/nr | nr |
| Rivera et al. (2009) | 22 | hCG decrease <50% after manual vacuum aspiration | na | 1.0/0.92 | na |
| First author (year) . | n . | Serum hCG strategy . | Pregnancy outcomes . | ||
|---|---|---|---|---|---|
| IUP (sensitivity/specificity) . | EP (sensitivity/specificity) . | Other (sensitivity/specificity) . | |||
| Single serum hCG cut-off level | |||||
| Hajenius et al. (1995) | 265 | hCG >1000 IU/l | 0.95/0.33 | 0.90/0.98 | 0.58/1.0 |
| Kaplan et al. (1996) | 72 | hCG <1000 mIU/ml | 0.27/0.64 | 0.67/0.74 | nr |
| Dart et al. (1997) | 194 | hCG >3000 mIU/ml Menstrual days >38 | 0.00/0.55 0.29/0.13 | 0.26/0.57 0.70/0.16 | 0.48/0.84 0.90/0.44 |
| Dart and Howard (1998) | 147 | hCG <1000 mIU/ml | nr | 0.48/0.55 | nr |
| Dart et al. (1999a) | 224 | hCG <1000 mIU/ml | 0.91/0.41 | 0.64/0.40 | 0.52/0.41 |
| Mol et al. (1998) | 262 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | 0.20/0.80 0.00/0.83 0.00/0.86 | 0.43/0.86 0.40/0.96 0.38/0.98 | 0.11/0.69 0.06/0.81 0.02/0.81 |
| Dart et al. (2002) | 420 | hCG <1000 mIU/ml | nr | 0.86/0.43 | nr |
| Condous et al. (2005a) | 569 | hCG >1000 IU/l hCG >1500 IU/l hCG >2000 IU/l | nr | 0.22/0.87 0.15/0.93 0.11/0.95 | nr |
| El Bishry and Ganta (2008) | 126 | Progesterone <16 nmol/l and hCG >25 IU/l Progesterone 16–80 nmol/l and hCG >25 IU/l Progesterone >80 nmol/l and hCG <1000 IU/l Progesterone >80 nmol/l and hCG >1000 IU/l | 0.03/0.44 0.71/0.57 0.03/1.0 0.23/0.99 | 0.44/0.60 0.53/0.50 Na/0.99 0.03/0.91 | nr |
| Shaunik et al. (2011) | 173 | hCG <2000 mIU/ml | 0.61/0.13 | 0.87/0.39 | na |
| Serum hCG ratio | |||||
| Ankum et al. (1995) | 85 | Initial hCG <1500, hCG ratio | Nr | 1.0/0.97 | nr |
| Dart et al. (1999b) | 307 | hCG increase <66% hCG decrease <50% | 0.25/0.80 0.00/0.67 | 0.74/0.50 0.80/0.59 | 0.15/0.65 0.34/0.91 |
| Condous et al. (2004) | 388 | Logistic regression model M1 (cut-off hCG ratio of 0.21 for EP; cut-off hCG ratio of 0.72 for failing PUL) | Training set: 0.86/0.98 Test set: 0.81/0.98 | Training set: 0.75/0.89 Test set: 0.83/0.88 | Training set: 0.89/0.95 Test set: 0.90/0.98 |
| Bignardi et al. (2008) | 940 | hCG ratio >0.87 hCG ratio <1.66 hCG ratio <2 | 1.0/0.73 0.07/0.09 0.23/0.05 | 0.85/0.55 0.85/0.36 0.92/0.28 | 0.11/0.03 0.98/0.76 0.98/0.58 |
| Logistic regression model | |||||
| Gevaert et al. (2006) | 856 | Bayesian network Parameter prior model >0.13 Structure an parameter prior model >0.06 | nr | 0.77/0.83 0.77/0.80 | nr |
| Kirk et al. (2006) | 357 | Logistic regression model based on hCG ratio and prediction by nurse practitioner | 0.89/0.78 | 0.76/0.84 | 0.78/0.87 |
| Condous et al. (2007a) | 376 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) Multinomial logistic regression model with clinical information M5 | 0.86/0.96 Training set: 0.73/0.97 Test set: 0.86/0.97 | 0.80/0.89 Training set: 0.92/0.94 Test set: 0.79/0.90 | 0.87/0.98 Training set: 0.97/0.98 Test set: 0.90/0.97 |
| Kirk et al. (2007) | 363 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.95/0.90 | 0.31/0.98 | 0.99/0.94 |
| Condous et al. (2007b) | 376 | Logistic regression model M1 (hCG ratio [hCG 48 h/hCG 0 h]) logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | 0.86/0.95 Training set: 0.79/0.98 Test set: 0.86/0.96 | 0.73/0.87 Training set: 0.92/0.91 Test set: 0.80/0.89 | 0.86/0.99 Training set: 0.97/0.98 Test set: 0.87/0.98 |
| Barnhart et al. (2010) | 1035 | Logistic regression model M4 (hCG ratio [hCG 48 h/hCG 0 h], [log] of hCG average, quadratic effect of the hCG ratio {[hCG ratio of 1.17] × [hCG ratio of 1.17]}) | UK cohort: 0.88/0.97 US cohort: 0.84/0.93 | UK cohort: 0.81/0.89 US cohort: 0.49/0.87 | UK cohort: 0.88/0.99 US cohort: 0.81/0.83 |
| Other strategies | |||||
| Condous et al. (2005b) | 518 | Single visit protocol: High-risk PUL progesterone 5–81 nmol/l or hCG >50 IU/l | nr | Training set 0.77/0.81 Test set 0.84/0.33 | nr |
| Condous et al. (2006) | 1003 | Uterine curettage if hCG (0 h) ≥2000 U/l and progesterone (0 h) <45 nmol/l or hCG (0 h) <2000 U/l and hCG ratio <1.16 | nr | 0.52/nr | nr |
| Rivera et al. (2009) | 22 | hCG decrease <50% after manual vacuum aspiration | na | 1.0/0.92 | na |
Nonetheless, the accuracy reported for different strategies showed considerable heterogeneity owing to the use of different hCG thresholds (cut-off) to define a positive pregnancy test. We therefore compared the sROC curves rather than the pooled estimates for sensitivity and specificity, as this summary point estimate does not reflect the accuracy for a particular operating point of the test. The pooled data for the pregnancy outcome EP are shown per strategy, i.e. an absolute single serum hCG level, serum hCG ratios and logistic regression models, in ROC plots in Fig. 2. These curves show that an absolute single serum hCG level had a poor performance in diagnosing EP in women with PUL, compared with the serum hCG ratios and logistic regression models, as the sROC curve is considerably closer to the diagonal, indicating no diagnostic value.
ROC plots with pooled data for the pregnancy outcome EP in women with pregnancy of unknown location by strategy. (a) An absolute single serum hCG level; (b) serum hCG ratios; (c) logistic regression models and (d) all strategies in one plot. Each small cube within a plot represents the sample size of each study, with the vertical length of the cube presenting the number EPs, and the horizontal the number women without EP. sROC, summary ROC curve.
Discussion
We performed a systematic review of various serum hCG-based strategies to diagnose the pregnancy outcome in women with PUL. For most pregnancy outcomes, the data were clinically very heterogeneous, and only the outcome EP was suitable for meta-analysis. An absolute single serum hCG level had the lowest diagnostic value, while strategies using serum hCG ratios, either alone or incorporated in logistic regression models, showed reasonable diagnostic performance for EP.
Worldwide, different diagnostic strategies using serum hCG in women with a PUL have been introduced and optimized within the same population for more accurate and earlier diagnosis. Differences in definitions of populations (e.g. very strict ultrasound definitions of PUL versus any form of inconclusive scanning as defined by the clinician) and final pregnancy outcomes (e.g. IUP solely based on location therefore a combination of viable and non-viable pregnancies, or very strictly defined as a pregnancy leading to the delivery of a child), have made the interpretation of current literature difficult and a meta-analysis of the data nearly impossible. It is important to realize that geographic differences in the prevalence of, for example EP and the a priori risk of the women enrolled, may affect the performance of a particular strategy. This is illustrated by the validation of a logistic regression model developed in the UK on a US population (Barnhart et al., 2010). Whereas this model had 80% sensitivity for EP in the UK, this decreased to 49% when applied in the US PUL population, with a similar specificity of ∼88% in both populations. A first step in improving the objective comparison of research outcomes in the diagnosis of PUL and in reducing clinical heterogeneity is the international consensus statement which has recently become available (Barnhart et al., 2011). This consensus statement proposes uniformity in definitions of population, target disease and final outcome of women with a PUL to allow the objective interpretation of research, objective assessment of future reproductive prognosis and hopefully lead to improved clinical care.
The results of the pooled data need to be interpreted with caution. First, all included studies were cohort studies evaluating one diagnostic test for the diagnosis EP. To date, no randomised controlled trials have been published comparing different diagnostic strategies for EP in women with PUL. Second, there was clinical heterogeneity between the studied populations. Most studies originating from the USA reported the evaluation of women who presented to emergency departments, where the ultrasound distinction between PUL and probable EP is not always made. In studies from European countries, women are directly evaluated by a specialized team in an early pregnancy unit, which may have resulted in a stricter ultrasound definition of PUL. Third, the reference test for the diagnosis EP was not uniform in all studies. The gold standard in the diagnosis of EP is laparoscopic confirmation but the PUL population is mostly asymptomatic and also a candidate for non-surgical management. Also, laparoscopy has some limitations; early ongoing EPs are sometimes too small to be seen at the time of laparoscopy. In addition to laparoscopy, alternative ultrasound reference tests for EP were used: an ectopic gestational sac with the visualization of a yolk sac or embryo, an inhomogeneous mass (blob sign) or an empty gestational sac (bagel sign). This alternative reference test using ultrasound for the diagnosis of EP is also not without limitations. However, the diagnostic performance of TVS can achieve a sensitivity of between 93.2 and 94.4% (Condous et al., 2005c; Kirk et al., 2008). Another reference test for EP was an increasing serum hCG after uterine curettage with absent chorionic villi (Barnhart et al., 2002).
In general, the pregnancy outcome EP alone is not the most patient-centred outcome. Owing to the earlier diagnosis of EP, the field is moving from the clinically important EP that requires surgery because of a real risk to woman's health, to those EPs where health practitioners act preventatively (e.g. with MTX) despite the fact that spontaneous resolution is possible. Current literature on the diagnostic accuracy of serum hCG strategies in women with PUL did not provide enough data to inform us about diagnostic criteria needed to distinguish between pregnancies that will lead to a viable IUP, those that do not require any intervention because the pregnancy is failing and those where we need to intervene as failure does put the woman's health at risk. Properly conducted prospective studies are needed to provide this relevant data.
Some diagnostic strategies in single studies had rather low sensitivity and/or specificity. The natural history of PUL may be such that more time is needed (i.e. testing later in the pregnancy) to distinguish the pregnancy outcomes. Rendering a prediction on only a single, or two, serum hCG measurement may lead to an inherent misclassification.
The sROC curves based on the pooled data show a higher sensitivity for the serum hCG ratio strategy but the regression models apparently have a better performance regarding specificity. In clinical practice these models are complex and often need computer analyses. Since most women with PUL are followed up by at least two serum hCG measurements, the serum hCG ratio strategy seems easier to implement.
In conclusion, in women with PUL the diagnostic strategies using serum hCG ratios, either alone or incorporated in logistic regression models, seem to have the best diagnostic performance in case of EP. Overall, the data were very heterogeneous and comparative diagnostic studies have not been performed on the diagnostic value of serum hCG in women with PUL. Studies directly comparing the efficacy of serum hCG strategies are warranted in order to identify the best strategy to diagnose pregnancy outcome in women with PUL.
Authors' roles
W.M.A., K.B., B.W.M. and F.v.d.V. all contributed substantially to the conception and design of this review. NvM and FM screened all titles, abstracts, articles and extracted data for meta-analyses. B.W.M. and P.J.H. were third reviewers in case consensus could not be reached directly. B.C.O. supervised the analysis and interpretation of data. N.v.M. drafted the article, all other authors critically revised multiple versions of the manuscript. All authors gave their final approval of the version to be published.
Funding
F.M. and P.J.H. are supported by grants from The Netherlands Organisation for Health Research and Development (Agiko stipendium 920-03-328 and Clinical Fellow 40-00703-97-05-154). No other funding was either sought or obtained for this study.
Conflict of interest
None declared.
Acknowledgements
We thank C.E.J.M. Limpens, clinical librarian, for her help with the literature search.