Abstract
The association between health-related role limitations in the mental and physical subdomains and clinical status (i.e., chronic disease and comorbid depressive symptoms) is mediated by health-promoting behaviors. To enhance health-promoting behaviors in adults with chronic disease, it is necessary to identify item-level associations among targets of health-related monitoring and management. Therefore, the current study used a network approach to examine associations among health-related role limitations, depressive symptoms, existential well-being, socioeconomic position, and health-promoting behavior in adults with chronic disease. A total of 535 adults (mean ± SD age = 62.9 ± 11.9 years; males, n = 231, females, n = 304) who were regularly visiting an outpatient clinic for chronic disease treatment participated in this cross-sectional study. Data on participant demographics, chronic disease diagnoses, socioeconomic status, health-related role limitations (12-item short form survey scores), depressive symptoms (patient health questionnaire-9 scores), existential well-being (scores for four items of the McGill quality of life questionnaire-Revised), and health-promoting behavior (Healthy Habits Questionnaire scores) were acquired. “Undirected regularized partial correlations” and “directional joint probability distributions” among these variables were calculated using a mixed graphical model (MGM) and directed acyclic graph (DAG). In the MGM, the most influential nodes were emotional well-being, feelings of failure, and health-related limitations affecting usual role and physical activities. According to both the MGM and DAG, the relationship between emotional well-being and feelings of failure mediated the relationships of health-related role limitations with concentration difficulty and suicidal ideation. A positive mindset was dependent on the probability distributions of suicidal ideation, controllability of life, and positive self-image. Both the meaning of life and a positive mindset had direct associations with proactive living. Specifically, proactive living was associated with a balanced diet, regular exercise, volunteering in the community, and nurturing intimacy in social interactions. The meaning and controllability of life in individuals with chronic diseases could mediate the relationships of health-promoting behavior with health-related limitations related to usual role activities, physical activities, and depressive symptoms. Thus, interventions targeting health-promoting behaviors should aim to enhance the meaning and controllability of life (as it pertains to limitations in usual role and physical activities), as well as promote proactive screening and timely psychiatric treatment of depressive symptoms including feelings of failure, concentration difficulties, and suicidal ideation.
Similar content being viewed by others
Introduction
Importance of health-promoting behavior in the treatment of chronic disease patients
Chronic disease can be defined as a medical condition lasting ≥ 1 year that requires ongoing medical attention and/or limits activities of daily living1. Cardiovascular diseases (such as heart attacks and stroke), cancers, chronic respiratory diseases (such as chronic obstructive pulmonary disease and asthma), diabetes, and chronic renal diseases account for > 80% of all chronic disease-related deaths that occur before the age of 70 years1,2. Additionally, chronic diseases such as hypertension, dyslipidemia (high low-density lipoprotein cholesterol), and diabetes are major risk factors for cardiovascular diseases1. Regarding health-related role limitations, chronic arthritis is a leading cause of work disability in the United States and a common cause of chronic pain1. Chronic arthritis affects about one in four adults in the United States and is more prevalent among those diagnosed with diabetes and/or cardiovascular disease compared with adults without chronic diseases3. Osteoporosis is a major risk factor for all-cause mortality in adults aged ≥ 60 years4, and is associated with substantial health-related role limitations even in the absence of frailty fractures5. Globally, 30–60% of adults have multiple chronic conditions that can negatively affect health, function, and quality of life6,7. For instance, hypertension, diabetes, dyslipidemia, chronic pulmonary disease, chronic renal disease, chronic arthritis, and osteoporosis are frequently comorbid and associated with higher risks of all-cause mortality and health-related role limitations.
The likelihood of chronic diseases might depend on the combined effects of genetic, physiological, environmental, and behavioral factors2. For instance, lower socioeconomic status is associated with a higher risk of developing chronic diseases such as cardiovascular disease8,9. Moreover, in adults with multiple chronic diseases, lower educational achievement and monthly household income are associated with worse clinical status at follow-up assessments10. Accordingly, comorbid depressive symptoms and poor health-related behaviors, such as non-adherence to pharmacotherapy, reportedly mediated the relationship between lower socioeconomic status and uncontrolled blood pressure in middle-aged and older adults with hypertension11. To improve patient outcomes and potentially prevent chronic diseases, health-promoting behaviors such as maintaining a healthy diet, engaging in regular exercise and physical activity, getting enough sleep, quitting smoking, limiting alcohol intake, going for regular health screenings, making time for leisure activities, talking with friends about personal concerns and feelings, and participating in social activities within community- or faith-based organizations are crucial12,13. However, the vast majority of individuals newly diagnosed with a chronic disease do not adopt health-promoting behaviors and thus fail to achieve long-term improvements in health14.
Health-related role limitations and health-promoting behaviors in chronic disease patients
Health-related role limitations are a major element of disease-related burden15. Chronic non-communicable diseases (i.e., diseases that are typically caused by unhealthy behaviors rather than being spread through infection) are an important cause of health-related disability and role limitation in developed countries16. The 12-item Short Form Survey (SF-12)17 can be used to measure limitations in physical health (i.e., general health, physical activities, and usual role activities [in association with physical health problems or bodily pain]) and mental health (i.e., vitality, emotional well-being, and usual role or social activities [in association with emotional problems]).
Health-related role limitations might be associated with decreased adherence to health-promoting behaviors in patients with chronic disease. Among adults with hypertension, dyslipidemia, and/or diabetes, those with fewer health-related role limitations in physical and mental health subdomains engaged in more health-promoting behaviors, specifically adequate fruit/vegetable intake and abstaining from smoking (which influenced mental health), and adequate physical activity (which influenced physical health, regardless of clinical status)18. Also, ego resilience had a stronger mediating effect on the association between emotional outlook and positive emotion at baseline versus after a health-promoting intervention aimed at increasing physical activity among adults in the workplace19. In contrast, in adults with hypertension, greater health-related role limitations in the mental health subdomain were associated with difficulty adhering to a healthy diet and engaging in regular exercise, as well as current smoking status20. Furthermore, the presence of psychological distress might decrease adherence to recommended preventive care, such as influenza vaccinations and annual dental check-ups21. Currently, the mechanisms underlying the association between health-related functional status and behavioral outcomes (i.e., health-promoting behaviors) are not well understood.
Comorbid depressive symptoms and health-promoting behaviors in chronic disease patients
Chronic diseases such as hypertension22, diabetes mellitus23, pulmonary hypertension24, chronic kidney disease25, and rheumatoid arthritis26 are associated with increased rates of psychological distress, depressive symptoms, anxiety, and cognitive disturbance27,28,29. Furthermore, more severe comorbid depressive symptoms are associated with a higher number of chronic disease diagnosese30. Disease-related physical limitations and psychological distress, clinical deterioration, maladaptive health-related behaviors, and depressive symptoms are often mutually reinforcing31,32. Furthermore, comorbid depressive symptoms may affect health-related behaviors such as self-care behavior, physical activity, sleep time, eating habits, and compliance with treatment31,33,34, and were associated with adverse health and social outcomes in patients with chronic disease27. For example, depression negatively affects blood sugar control in diabetics because of lowered compliance to behaviors such as following a specific diet, taking medications on time, assessing metabolic parameters, and maintaining a consistent sleep cycle35. Furthermore, adults with comorbid depression are less likely to quit smoking after being diagnosed with acute coronary syndrome36. To date, few studies have examined the associations between health-promoting behaviors and depressive symptoms in patients with chronic disease37,38,39.
Existential well-being and health-promoting behaviors in chronic disease patients
Existential well-being depends on an individual’s perspective on the meaning and purpose of life, satisfaction regarding their own life, and feelings regarding death and suffering40. The meaningful existence subdomain40,41,42 of the McGill quality of life questionnaire-revised (MQOL-R)43,44 measures existential well-being in terms of the meaning/purpose of life, progress/fulfillment of life goals, feeling of having control over one’s own life, and positive self-image. Existential well-being and health-promoting behaviors might have a bidirectional relationship. For instance, middle-aged adults with a greater sense of purpose in life are more likely to be physically active and less likely to experience sleep problems compared with those with less sense of purpose45. Furthermore, health-promoting behaviors, such as regular physical activity, at baseline were associated with a stronger purpose of life 4 years later46. Greater existential well-being has been linked with a lower rate of depression and better-preserved health. In patients with chronic renal disease undergoing peritoneal dialysis, fewer health-related role limitations in the physical and mental subdomains, as well as milder depressive symptoms, were correlated with a stronger sense of meaning and purpose in life47. Conversely, a diagnosis of stroke and/or depression at baseline appeared to contribute to a weaker sense of purpose 4 years later46. Existential well-being, i.e., a sense of control in life, is associated with emotional well-being (positive affect and optimism), less severe depressive symptoms, and health-promoting behaviors including physical activity, good sleep hygiene, and social involvement48. However, few studies have examined the item-level associations among health-related role limitations, depressive symptoms, facets of existential well-being, and diverse health-promoting behaviors in people with chronic diseases.
Study aim and hypothesis
Physical and mental limitations (i.e., limitations in physical activities [due to health problems], role activities [due to physical health problems or bodily pain], vitality, emotional well-being, and usual or social activities [due to emotional problems])49,50,51, depressive symptoms52,53, existential well-being (meaning/purpose of life, progress/fulfillment of life goals, having control over one’s own life, and positive self-image)40,41,42, and socioeconomic status (educational attainment, employment, and monthly household income)52,53,54 are all associated with health-promoting behaviors (maintaining a healthy diet, engaging in regular exercise and physical activity, getting enough sleep, abstaining from smoking, limiting alcohol intake, going for regular health screenings, making time for leisure activities, talking with friends about concerns and feelings, and participating in social activities within community- or faith-based organizations)12,13 in adults with chronic diseases. Moreover, health-related role limitations in the mental and physical subdomains are associated with chronic disease and comorbid depressive symptoms in adults with chronic disease, where these relationships are mediated by health-promoting behaviors51. Adults with chronic diseases who had more severe depressive symptoms experienced greater enhancement of self-efficacy after an intervention targeting health-promoting behaviors55.
It can be difficult to capture the multiple mechanisms underlying health-promoting behaviors in adults with chronic disease, which include health status (health-related role limitations), cognitions (existential well-being), emotions (depressive symptoms), and behaviors (i.e., health-promoting behaviors)56,57,58, using correlation and regression analyses. Furthermore, it can be difficult to determine the variance in item-level responses among participants with similar summary scores59,60. To identify factors that should be targeted by interventions aimed at enhancing health-promoting behaviors in adults with chronic diseases, the relationships among assessment items must be examined61,62. To identify item-level associations among health-related role limitations, depressive symptoms, existential well-being, socioeconomic position, and health-promoting behaviors in adults with chronic disease, we used a network approach38,59,63,64. A mixed graphical model (MGM)65 comprised of continuous, categorical, and/or ordinal variables can be used to “regularize” partial correlations. In addition, directed acyclic graphs (DAGs)63 displaying probability distributions among variables, and the magnitude and direction of their relationships, can reveal conditional dependence. In the current study, we tested our hypothesis that there may be associations among health-related role limitations in physical and mental subdomains, vitality, emotional well-being, depressive symptoms, existential well-being, socioeconomic position, and health-promoting behaviors using a network approach. We also examined regularized partial correlations (MGMs) and “regularized directional independent associations” (DAGs) among assessment items. We expected to identify factors mediating the relationships of health-promoting behaviors with health-related role limitations, depressive symptoms, existential well-being, and socioeconomic status.
Methods
Participants and data collection
In this cross-sectional study, we recruited chronic disease patients who had been diagnosed at Seoul National University Hospital between October 2016 and February 2017. The inclusion criteria were as follows: aged ≥ 19 years, diagnosed with ≥ 1 chronic disease (hypertension4,66, hyperlipidemia66, diabetes4,66, chronic pulmonary disease67,68, chronic renal disease69,70, chronic arthritis67,71, or osteoporosis4,5), visited the outpatient clinic at Seoul National University Hospital between October 2016 and February 2017 for treatment of chronic diseases, fluent in Korean, and willing to participate in this study. A total of 535 adults regularly visited the outpatient clinic for treatment of chronic diseases and completed self-report questionnaires between October 5, 2016 and February 28, 2017. All participants received sufficient information about the study and provided written informed consent. The survey was anonymous and confidential. This study was approved by the clinical research ethics committee of Seoul National University Hospital College of Medicine (IRB number 1601-075-734). All procedures were performed in accordance with relevant guidelines and regulations.
Measures
Demographic information (age, sex, marital status, residential area) and chronic disease diagnoses (hypertension, hyperlipidemia, diabetes mellitus, chronic pulmonary disease, chronic renal disease, chronic arthritis, and osteoporosis) were confirmed by a physician at the outpatient clinic. Information about socioeconomic status (educational attainment, monthly household income, employment status), health-related role limitations (assessed by the 12-item Short Form Survey [SF-12])72, depressive symptoms (assessed by the Patient Health Questionnaire-9 [PHQ-9]73,74, existential well-being (assessed by four items of the MQOL-R)43,44, and health-promoting behavior (assessed by the Healthy Habits Questionnaire [HHQ]75) was acquired; no clinical evaluations were conducted by psychiatrists.
Health-related role limitations: SF-12
The SF-12 was developed to measure health-related quality of life17. It consists of 12 items distributed among eight subdomains of physical and mental health49: including general health (item 1), vitality (item 10), emotional well-being (items 9 and 11), limitations in physical activities (moderate activities and climbing several stairs) due to health problems (items 2 and 3), limitations in usual role activities due to physical health problems (items 4 and 5), limitations in usual role activities due to bodily pain (item 8), limitations in usual role activities due to emotional problems (items 6 and 7), and limitations in social activities due to physical or emotional problems (item 12)49,50. The 5- and 3-point Likert scale scores for the items were averaged within each subdomain49,50 to be used as nodes in the MGM (Fig. 1) and DAG (Fig. 2).
(A) Mixed graphical model comprised of health-related role limitation, depressive symptoms, existential well-being, and health behaviors in chronic disease. The “node predictability value” (variance in a given node’s value explained by the nodes with which it is connected) is indicated by the shadowed parts of rings surrounding each node. (B) Betweenness centrality values (the proportion of the shortest paths in the network containing a given node) of health-related role limitation, depressive symptoms, existential well-being, and health behaviors calculated from (A). The x-axis represents z-scores.
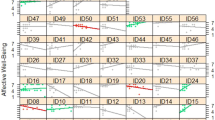
Directed acyclic graph of health-related role limitation, depressive symptoms, existential well-being, and health behaviors in chronic disease. The magnitude of association between two items is displayed by the thickness of an edge; the thicker the edge, the stronger the association between the two items connected.
Depressive symptoms: PHQ-9
The PHQ-973,74 evaluates depressive symptoms including hopelessness, anhedonia, sleep disturbance, fatigue, changes in appetite, guilt, concentration difficulties, psychomotor agitation/retardation, and suicidal ideation via nine self-report items. The total scores on the PHQ-9 reflect the severity of depression, which is classified as no depression (score of 0–4), mild depressive symptoms (score of 5–9), moderate depressive symptoms (score of 10–19), or severe depressive symptoms (score of 20–27)76. The 4-point Likert scale scores (none, 3–4 days, 8–10 days, or 12–14 days) for the nine depressive symptoms were used as nodes in the MGM (Fig. 1) and DAG (Fig. 2).
Existential well-being: MQOL-R
The MQOL-R43,44 comprises 14 items and is used to measure the level of subjective well-being throughout the lifespan in terms of physical symptoms (3 items), psychological symptoms (4 items), social support (3 items), and meaningful existence (4 items)40,41,42. In the current study, the 10-point Likert scale scores for four items related to existential well-being (meaningfulness and purposefulness of life, progress/fulfillment of life goals, having control over one’s own life, and positive self-image as a person) were used as nodes in the MGM (Fig. 1) and DAG (Fig. 2).
Health-promoting behavior: HHQ
The HHQ75 examines the practice of 12 important health-promoting behaviors: positive mindset, regular exercise, balanced diet, proactive attitude, regular medical checkups, volunteering in the community, religious and existential activities, nonsmoking, controlled drinking, work-life balance, nurturing intimacy in social interactions, and consistently taking prescribed medications. Five-point Likert scale scores (no intention, intention of performing within the next six months, intention of performing within the next month, have been practicing for < 6 months, have been practicing for ≥ 6 months) were translated into binary data (have been practicing for any duration = 1, not practicing yet = 0) to be used as nodes in the MGM (Fig. 1) and DAG (Fig. 2).
Statistical analysis
We used network analyses to elucidate the associations among the scores for the eight subdomains of the SF-12, nine PHQ-9 depressive symptoms (including suicidal ideation), four (MQOL-R) existential well-being items, 12 HHQ health-related habits, and three variables related to socioeconomic status (educational attainment, monthly household income, and employment status). “Undirected” and “directional conditional dependencies”77 among the variables were estimated using MGMs (undirected networks comprising nodes showing conditional dependencies or regularized partial correlations) and a DAG (a Bayesian network showing the conditional probability distributions and directional dependencies of nodes with parent nodes)78,79, respectively. In these networks, variables served as nodes (n = 36) and edges between nodes represented conditional dependence59.
MGM
This study included categorical, ordinal, and continuous data80, and we estimated “undirected conditional dependencies”77 between variables using MGMs with the R package mgm65. MGMs represent edge weights by generating node-wise regression coefficients81. To prevent potentially spurious associations, mgm employs the least absolute shrinkage and selection operator (LASSO) approach82. LASSO reduces all edge weights so that they approach zero and sets small weights to exactly zero82. To derive MGM networks, we optimized the edge weights during LASSO regularization (controlled by parameter λ) using a pairwise model (interaction order k = 2) and the extended Bayesian information criterion (tuning parameter γ = 0)59. Two variables were considered independent if they were not connected when conditioned on other variables83. The thickness of each edge in the network represents the strength of the association, with thicker edges representing stronger associations84. To identify the principal nodes within the MGM networks, we calculated the betweenness centrality (proportion of paths in the network that contain a given node)85; four items (nodes) within the top 12% were defined as hubs38. Similar to R2 regression coefficients, “node predictability values” were estimated, i.e., values reflecting how accurately a node could be predicted by the other nodes it shared an edge with59,62,86. Node predictability values were visualized using pie charts62. The MGM network structure was visualized using the Fruchterman − Reingold algorithm, which was performed using the R package qgraph84.
DAG
The DAG is a Bayesian approach for modeling networks with edges that are directed and noncircular, with the goal of discerning relationships among nodes based on cross-sectional data63. Using the R package bnlearn, we applied the ‘hill-climbing’ greedy search algorithm to our dataset87. The DAG added and removed edges (connecting variables or nodes), and reversed their direction, until the goodness of fit satisfied the BIC88. An iterative bootstrapping procedure with 10,000 iterations was used to determine whether an edge existed between two symptom nodes88,89. In the second step, we generated an averaged network by retaining edges that were consistently present in the 10,000 bootstrapped networks. The cut-off point for consistently present nodes was set using a statistical method with high sensitivity and specificity88,90. Finally, a BIC value was computed for each edge, with higher values (depicted by thicker edges) signifying greater importance within the network structure88.
Results
Sample characteristics
A total of 535 adults [mean ± SD age = 62.9 ± 11.9 years; males, n = 231; females, n = 304) participated in the current study. Table 1 provides the demographic, chronic disease diagnosis, socioeconomic status, health-related role limitation (SF-12 scores), depressive symptom (PHQ-9 scores), existential well-being (scores on four MQOL-R items), and health-promoting behavior (HHQ scores) data of the participants. The mean number of diagnosed chronic diseases per participant was 2.1 ± 0.9 and the most common diagnoses were hypertension (n = 284, 53.1%), hyperlipidemia (n = 279, 52.1%), and diabetes (n = 249, 46.5%). Regarding educational attainment, 230 (43.0%) participants had an education level of college or higher level, and another 183 (34.2%) were high school graduates. A total of 197 (36.8%) participants were employed (n = 96; 17.9%) or self-employed (n = 101, 18.9%), and another 338 (63.2%) were unemployed or retired. Only 196 (36.6%) of the participants had a monthly household income ≥ 3000 US dollars (third quintile of the monthly average income of households with one or more family members in the Republic of Korea during 2016 and 2017 [https://kosis.kr/]).
According to the SF-12 scores, the general health, physical functioning and role limitations due to physical health, and role limitation due to pain was fair, good, and very good, respectively. Vitality and emotional well-being were also good, and role limitations due to emotional problems and social functioning were very good. The severity of depressive symptoms, as evaluated using the PHQ-9, was mild (mean total PHQ-9 score = 4.4 ± 5.0). Regarding existential well-being, the median MQOL-R satisfaction (meaning/purpose of life, progress/fulfillment of life goals, feeling of having control over one’s own life, and self-image) score was 8 out of 10. Finally, the mean performance of health behavior (regardless of duration) score was 9.4 ± 2.8. The most commonly practiced health-promoting behaviors were consistently taking prescribed medications (n = 506, 94.6%) and abstaining from smoking (n = 485, 90.7%). The least frequently practiced health-promoting behaviors were volunteering in the community (n = 279, 52.1%) and religious and existential activities (n = 325, 60.7%).
Network analyses: MGM and DAG
Overview
The MGM network for physical and mental quality of life (8 SF-12 domains), depressive symptoms (nine PHQ-9 items including suicidal ideation), existential well-being (four MQOL-R items), health-promoting behavior (12 HHQ items), and socioeconomic status (educational attainment, monthly household income, and employment status) is presented in Fig. 1A and Table 2. Although 636 edges were possible, only 42 (6.6%) were evident in the final MGM. According to the betweenness centrality data displayed in Fig. 1B, four items (nodes) within the top 12% of all 36 nodes comprising the MGM functioned as hubs in the MGM: emotional well-being (calm/peaceful and downhearted/sad; z-score = 3.25), limitations in usual role activities due to emotional problems (z-score = 1.92), physical health problems (z-score = 1.70), and feeling like a failure (z-score = 2.11). Furthermore, the degree to which each node could be predicted by the other nodes with which it shared an edge was estimated; the results are shown in Fig. 1A. In the DAG analysis (Fig. 2, Table 3), the strength of the association between two items is denoted by the thickness of the edge, as stated above91. Table 3 lists the edge weights (from strongest to weakest). The directions of the edge weights indicate the increase or decrease in a given score that would be expected if the arc were removed from the DAG92. If two items are strongly related, the edge weight will be negative and its absolute value will be large91.
Perceived meaning, achievement of life goals, control of life and health-promoting behavior
Perceived meaning, achievement of life goals and control of one’s life were directly influenced by emotional problem-related limitations in usual role activities, emotional well-being (calm/peaceful and not sad), and concentration difficulties, respectively (Fig. 2, Table 3). There was a partial correlation between perceived achievement of life goals (existential well-being) and emotional well-being (calm/peaceful and not sad; r = 0.02), which contributed to the high predictive value (61.8%) for the achievement of life goals item (Fig. 1A, Table 2).
Positive mindset, as the hub node for health-promoting behavior in the DAG, was influenced by the joint probability distributions of suicidal ideation, perceived control of one’s life, and positive self-image. Positive mindset and perceived meaning of life (existential well-being) were both parent nodes of proactive living (health-promoting behavior). Furthermore, positive mindset, proactive living, and perceived controllability of one’s life were directly associated with the fostering of intimate interpersonal relationships (health-promoting behavior) (Fig. 2, Table 3).
The types of health-promoting behavior with the highest node predictability values in the MGM were proactive living (43.3%; via partial correlations with positive mindset [r = 0.09], balanced diet [r = 0.05], and nurturing intimacy in social interactions [r = 0.02]), positive mindset (40.0%; via partial correlations with proactive living [r = 0.09] and nurturing intimacy in social interactions [r = 0.02]), and nonsmoking (38.4%; via a partial correlation with controlled drinking [r = 0.12]) (Fig. 1A, Table 2). In the DAG, positive mindset had a direction influence on proactive living, nurturing intimacy in social interactions, regular medical checkups, regular exercise, and eating a balanced diet. Proactive living, which was influenced by the joint probability distributions of positive mindset and the meaning and purpose of life, also had direct associations with a balanced diet, volunteering in the community, nurturing intimacy in social interactions, and regular exercise (Fig. 2, Table 3).
Associations between health-related role limitations and depressive symptoms
Among the physical and mental health subdomains, node predictability values in the MGM were highest for emotional well-being (calm/peaceful and not sad; 80.3%) and vitality (71.4%), and lowest for general health (34.8%) and limitations in physical activities due to health problems (39.5%) (Fig. 1A, Table 2). In the DAG, limitations in physical activities due to health problems emerged was the most pivotal node, and had direct associations with limitations in usual role activities due to physical health problems and pain, monthly household income, and vitality. In turn, limitations in physical activities due to health problems had a direct influence on role limitations due to emotional problems and pain, limitations in social activities due to physical or emotional problems, and fatigue (Fig. 2, Table 3). Among the health-related role limitation items, the strongest partial correlations in the MGM were between limitations in usual role activities due to physical health problems and limitations in physical activities due to health problems; limitations in usual role activities due to physical health problems and those due to emotional problems; and emotional well-being (calm/peaceful and not sad) and vitality (r = 0.30 for all three relationships; Fig. 1A, Table 2).
Health-related role limitations and depressive symptoms were connected in the MGM through the regularized partial correlation between emotional well-being and feeling like a failure (r = 0.20; Fig. 1A, Table 2). In the DAG, feeling like a failure was affected by the joint probability distributions of emotional well-being, vitality, hopelessness, and anhedonia. The emergence of depressive symptoms in the DAG was related to anhedonia through the joint probability distributions of emotional well-being and educational attainment. Anhedonia had direct associations with other depressive symptoms (feelings of hopelessness), psychomotor retardation/agitation, concentration difficulties, fatigue, and feeling like a failure (Fig. 2, Table 3).
The predictability of depressive symptoms in the MGM included both low values, i.e., 27.7% (psychomotor agitation/retardation) and 29.9% (changed appetite and eating behaviors), and relatively high values, i.e., 45.0% (fatigue) and 52.0% (hopelessness). The strongest partial correlations among the depressive symptoms in the MGM were between hopelessness and anhedonia (r = 0.43), and psychomotor agitation/retardation and concentration difficulty (r = 0.39). Notably, the node predictability value of suicidal ideation was 38.5% due to its partial correlations with hopelessness (r = 0.27), feeling like a failure (r = 0.22), and psychomotor agitation/retardation (r = 0.15) (Fig. 1A, Table 2). Likewise, in the DAG, suicidal ideation was influenced by the joint probability distributions of feeling like a failure and hopelessness (Fig. 2, Table 3).
Discussion
The relationship between emotional well-being and the feeling of failure in individuals with chronic disease mediates the relationships of limitations in usual role activities due to emotional problems with concentration difficulties and suicidal ideation
In the current study, the most influential nodes in the MGM (indicated by the betweenness centrality values) in terms of the regularized partial correlations among items were emotional well-being (calm/peaceful and downhearted/sad), feeling like a failure, limitations in usual role activities due to emotional problems (low mood and anxiety), and limitations in physical activities due to health problems. Likewise, the DAG in the current study revealed direct associations of limitations in physical activities due to health problems with limitations in usual role activities due to physical health problems and/or bodily pain, monthly household income, and vitality. The prevalence of chronic disease is a significant predictor of depressive symptoms93. Physical symptoms such as pain, dyspnea, gait and balance problems, and frailty, in addition to low ability to accept illness and long illness duration, may contribute to reduced physical activity, impaired activities of daily living, limited role functioning in occupational and social settings, depressive symptoms, anxiety, and lower life satisfaction94,95,96,97,98,99. Medication for chronic disease combined with antidepressants22, behavioral inerventions100, cognitive-behavioral therapy101, and face-to-face social support102 could be helpful for improving the physical health status and decreasing the depressive symptoms of patients with chronic disease.
Our findings emphasize the importance of preserving the usual role activities and social functioning of patients with chronic disease. In both the MGM and DAG, regularized partial associations (MGM) and the joint probability distribution of “directional conditional dependencies” (DAG) between emotional well-being (calm/peaceful and downhearted/sad) and feeling like a failure mediated the relationships of limitations in usual role activities due to emotional problems with concentration difficulties and suicidal ideation. In the MGM, the predictability of suicidal ideation was 38.5% due to partial correlations with hopelessness, feeling like a failure, and psychomotor change. Previous studies have also suggested that factors potentially exacerbating suicidal ideation include hopelessness (pessimism about the future), concentration difficulties, low motivation levels, and distress related to serious medical illnesses103,104,105. In our DAG, suicidal ideation was dependent on the joint probability distributions of feeling like a failure and hopelessness. Additionally, suicidal ideation had direct associations with psychomotor changes, concentration difficulties, and a positive mindset. Combining health education106 (delivered using electronic mobile devices) with motivational interviewing107 could improve depressive symptoms and self-efficacy.
Associations between the meaning/controllability of life and health-promoting behaviors
The current findings emphasize the importance of existential well-being to health-promoting behaviors. In the DAG, a positive mindset and proactive living mediated the relationships of existential well-being with health-promoting behaviors. Specifically, the health-promoting behavior of maintaining a positive mindset was influenced by the joint probability distributions of suicidal ideation, positive self-image, and feelings of control over one’s life. Perceived loss of control over one’s life was significantly associated with perceived unaffordability of long-term life projects108. In a life crisis, such as a new cancer diagnosis, people desire agency in daily life and interpersonal connections109. Therefore, improving the knowledge, skills, attitudes, and self-awareness necessary for good health behaviors could reduce anxiety and depressive symptoms in adults with chronic disease110.
In this study, both a positive mindset and strong sense of purpose in life had direct associations with other health-promoting behaviors of proactive living. Proactive living had direct associations with a balanced diet, regular exercise, volunteering in the community, and nurturing intimacy in social interactions. The importance of the meaning and purpose of life has been emphasized with respect to treatment adherence in people with newly diagnosed cancer111. Good health behaviors, such as adherence to prescribed medication, are difficult to achieve and maintain, especially in patients with chronic disease112. Conversely, for people faced with a life crisis, loss of meaning is strongly connected with suicidal ideation104. As the search for and presence of meaning in life are highly correlated in patients with chronic disease or pain, finding meaning in life must be a focus during the management of chronic disease patients113. People with physical illness and pain might find meaning and hope through personal activities and interpersonal relationships111,113. Regular assessments of interpersonal communication and social connections109, combined with cognitive-behavioral therapy114 and behavioral modification115, could enhance emotional well-being and life meaning116 in patients with chronic disease.
Limitations
The current study had several limitations. First, as we used a cross-sectional design, establishing causality in the associations between the different variables was not possible. Second, we used self-report measures to examine health-promoting behavior. Real-time tracking of daily behaviors using wearable devices, such as smart watches, might provide more detailed and accurate measurements of health-promoting behavior. Third, we did not perform subgroup analyses or construct MGMs and DAGs for individual physical illnesses. However, the seven chronic diseases examined in this study (hypertension, diabetes, dyslipidemia, chronic pulmonary disease, chronic renal disease, chronic arthritis, and osteoporosis) are frequently comorbid, and 30–60% of adults have multiple chronic conditions6,7. Future studies with more participants are needed to compare network-level associations among different chronic diseases.
Conclusions
We applied network analysis to identify factors that could be targeted by interventions to enhance health-promoting behaviors in adults with chronic diseases. The meaning and controllability of life of individuals with chronic disease mediated the associations of health-related limitations in usual role activities, physical activities, and depressive symptoms. Interventions targeting health-promoting behaviors, the meaning and controllability of life, limitations of usual role activities, and physical activities, as well as proactive screening and timely psychiatric consultations to address depressive symptoms (such as feelings of failure, concentration difficulties, and suicidal ideation) are needed.
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
(NCCDPHP), N. C. F. C. D. P. A. H. P. About Chronic Diseases. https://www.cdc.gov/chronicdisease/about/index.htm (2022).
(WHO), W. H. O. Noncommunicable Diseases. https://www.who.int/news-room/fact-sheets/detail/noncommunicable-diseases (2020).
Barbour, K. E., Helmick, C. G., Boring, M. & Brady, T. J. Vital signs: Prevalence of doctor-diagnosed arthritis and arthritis-attributable activity limitation—United States, 2013–2015. Morb. Mortal Wkly. Rep. 66, 246–253. https://doi.org/10.15585/mmwr.mm6609e1 (2017).
Gutzwiller, J. P. et al. Osteoporosis, diabetes, and hypertension are major risk factors for mortality in older adults: An intermediate report on a prospective survey of 1467 community-dwelling elderly healthy pensioners in Switzerland. BMC Geriatr. 18, 115. https://doi.org/10.1186/s12877-018-0809-0 (2018).
Hopman, W. M. et al. Longitudinal assessment of health-related quality of life in osteoporosis: Data from the population-based Canadian Multicentre Osteoporosis Study. Osteoporos Int. 30, 1635–1644. https://doi.org/10.1007/s00198-019-05000-y (2019).
Vetrano, D. L. et al. Frailty and multimorbidity: A systematic review and meta-analysis. J. Gerontol. A Biol. Sci. Med. Sci. 74, 659–666. https://doi.org/10.1093/gerona/gly110 (2019).
Griffith, L. E. et al. Multimorbidity frameworks impact prevalence and relationships with patient-important outcomes. J. Am. Geriatr. Soc. 67, 1632–1640. https://doi.org/10.1111/jgs.15921 (2019).
Lee, M., Park, S. & Lee, K. S. Relationship between morbidity and health behavior in chronic diseases. J. Clin. Med. 9, 010121. https://doi.org/10.3390/jcm9010121 (2020).
Vadini, F. et al. Homocysteine and education but not lipoprotein (a) predict estimated 10-year risk of cardiovascular disease in blood donors: A community based cross-sectional study. BMC Cardiovasc. Disord. 19, 177. https://doi.org/10.1186/s12872-019-1157-5 (2019).
Mira, R., Newton, T. & Sabbah, W. Inequalities in the progress of multiple chronic conditions: A systematic review of longitudinal studies. PLoS ONE 17, e0263357. https://doi.org/10.1371/journal.pone.0263357 (2022).
Qin, W. & Xu, L. Pathways linking relative deprivation to blood pressure control: the mediating role of depression and medication adherence among Chinese middle-aged and older hypertensive patients. BMC Geriatr. 23, 57. https://doi.org/10.1186/s12877-023-03769-6 (2023).
(NCCDPHP), N. C. F. C. D. P. A. H. P. How You Can Prevent Chronic Diseases. https://www.cdc.gov/chronicdisease/about/prevent/index.htm (2023).
(NCCDPHP), N. C. F. C. D. P. A. H. P. Promoting Health for Adults. https://www.cdc.gov/chronicdisease/resources/publications/factsheets/promoting-health-for-adults.htm (2022).
Newsom, J. T. et al. Health behavior change following chronic illness in middle and later life. J. Gerontol. B Psychol. Sci. Soc. Sci. 67, 279–288. https://doi.org/10.1093/geronb/gbr103 (2012).
Murray, C. J. et al. Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: A systematic analysis for the Global Burden of Disease Study 2010. Lancet 380, 2197–2223. https://doi.org/10.1016/s0140-6736(12)61689-4 (2012).
World Health Organization. World Report on Disability 2011 (World Health Organization, 2011).
Clause-Verdreau, A. C., Audureau, É., Leplège, A. & Coste, J. Contrasted trends in health-related quality of life across gender, age categories and work status in France, 1995–2016: Repeated population-based cross-sectional surveys using the SF-36. J. Epidemiol. Community Health 73, 65–72. https://doi.org/10.1136/jech-2018-210941 (2019).
González-Chica, D. A. et al. Are we reducing the risk of cardiovascular disease and improving the quality of life through preventive health care? Results of a population-based study in South Australia. Prev. Med. 99, 164–170. https://doi.org/10.1016/j.ypmed.2017.02.007 (2017).
Seaton, C. L., Bottorff, J. L., Jones-Bricker, M. & Lamont, S. The role of positive emotion and ego-resilience in determining men’s physical activity following a workplace health intervention. Am. J. Mens Health 12, 1916–1928. https://doi.org/10.1177/1557988318803744 (2018).
Trivedi, R. B., Ayotte, B., Edelman, D. & Bosworth, H. B. The association of emotional well-being and marital status with treatment adherence among patients with hypertension. J. Behav. Med. 31, 489–497. https://doi.org/10.1007/s10865-008-9173-4 (2008).
Thorpe, J. M., Kalinowski, C. T., Patterson, M. E. & Sleath, B. L. Psychological distress as a barrier to preventive care in community-dwelling elderly in the United States. Med. Care 44, 187–191. https://doi.org/10.1097/01.mlr.0000196965.54871.d5 (2006).
Wang, L. et al. Effects of combination treatment in hypertensive patients with depression: A systematic review and meta-analysis of 27 randomized controlled trials. Ther. Clin. Risk Manag. 18, 197–211. https://doi.org/10.2147/tcrm.S347622 (2022).
Liu, X. et al. A systematic review and meta-analysis of the prevalence and risk factors of depression in type 2 diabetes patients in China. Front. Med. 9, 759499. https://doi.org/10.3389/fmed.2022.759499 (2022).
Rawlings, G. H., Beail, N., Armstrong, I. & Thompson, A. R. Self-help cognitive behavioural therapy for anxiety in pulmonary hypertension: Pilot randomised controlled trial. ERJ Open Res. 8, 1. https://doi.org/10.1183/23120541.00526-2021 (2022).
de Donato, A., Buonincontri, V., Borriello, G., Martinelli, G. & Mone, P. The dopamine system: Insights between kidney and brain. Kidney Blood Press. Res. https://doi.org/10.1159/000522132 (2022).
Hill, J. et al. The prevalence of comorbidity in rheumatoid arthritis: A systematic review and meta-analysis. Br. J. Community Nurs. 27, 232–241. https://doi.org/10.12968/bjcn.2022.27.5.232 (2022).
Kayser, J., Hu, R. X., Rosenscruggs, D., Li, L. & Xiang, X. A systematic review of the impact of select mindfulness interventions on psychological outcomes among older adults with chronic health conditions. Clin. Gerontol. https://doi.org/10.1080/07317115.2022.2076636 (2022).
Araya, R. et al. Effect of a digital intervention on depressive symptoms in patients with comorbid hypertension or diabetes in Brazil and Peru: Two randomized clinical trials. JAMA 325, 1852–1862. https://doi.org/10.1001/jama.2021.4348 (2021).
Dingwall, K. M. et al. Effectiveness of wellbeing intervention for chronic kidney disease (WICKD): Results of a randomised controlled trial. BMC Nephrol. 22, 136. https://doi.org/10.1186/s12882-021-02344-8 (2021).
Gabriel, A. et al. Evaluating depressive symptoms among low-socioeconomic-status African American women aged 40 to 75 years with uncontrolled hypertension: A secondary analysis of a randomized clinical trial. JAMA Psychiatry 78, 426–432. https://doi.org/10.1001/jamapsychiatry.2020.4622 (2021).
Shapiro, M. S. Special psychosocial issues in diabetes management: Diabetes distress, disordered eating, and depression. Prim. Care 49, 363–374. https://doi.org/10.1016/j.pop.2021.11.007 (2022).
Køpfli, M. L. et al. Effect of telemonitoring on quality of life for patients with chronic obstructive pulmonary disease—A randomized controlled trial. Chron. Respir. Dis. 20, 14799731231157772. https://doi.org/10.1177/14799731231157771 (2023).
Uphoff, E. et al. Behavioural activation therapy for depression in adults with non-communicable diseases. Cochrane Database Syst. Rev. 8, 013461. https://doi.org/10.1002/14651858.CD013461.pub2 (2020).
García-Lara, R. A. et al. Prevalence of depression and related factors among patients with chronic disease during the COVID-19 pandemic: A systematic review and meta-analysis. Diagnostics 12, 123094. https://doi.org/10.3390/diagnostics12123094 (2022).
Sridhar, G. R. Can the management of depression in type 2 diabetes be democratized? World J. Diabetes 13, 203–212. https://doi.org/10.4239/wjd.v13.i3.203 (2022).
Lovatt, S. et al. Smoking cessation after acute coronary syndrome: A systematic review and meta-analysis. Int. J. Clin. Pract. 75, e14894. https://doi.org/10.1111/ijcp.14894 (2021).
Yun, J. Y. & Kim, Y. K. Phenotype network and brain structural covariance network of major depression. Adv. Exp. Med. Biol. 1305, 3–18. https://doi.org/10.1007/978-981-33-6044-0_1 (2021).
Suh, W. Y., Lee, J., Yun, J. Y., Sim, J. A. & Yun, Y. H. A network analysis of suicidal ideation, depressive symptoms, and subjective well-being in a community population. J. Psychiatr. Res. 142, 263–271. https://doi.org/10.1016/j.jpsychires.2021.08.008 (2021).
Yun, J. Y. et al. Impact of COVID-19 on lifestyle, personal attitudes, and mental health among Korean medical students: Network analysis of associated patterns. Front. Psychiatry 12, 702092. https://doi.org/10.3389/fpsyt.2021.702092 (2021).
Cohen, S. R., Mount, B. M., Tomas, J. J. & Mount, L. F. Existential well-being is an important determinant of quality of life. Evidence from the McGill quality of life questionnaire. Cancer 77, 576–586 (1996).
Albers, G. et al. Evaluation of quality-of-life measures for use in palliative care: A systematic review. Palliat. Med. 24, 17–37. https://doi.org/10.1177/0269216309346593 (2010).
Cohen, S. R. et al. Validity of the McGill quality of life questionnaire in the palliative care setting: A multi-centre Canadian study demonstrating the importance of the existential domain. Palliat. Med. 11, 3–20. https://doi.org/10.1177/026921639701100102 (1997).
Hyun Kim, S. et al. Validation study of the Korean version of the McGill quality of life questionnaire. Palliat. Med. 21, 441–447. https://doi.org/10.1177/0269216307079816 (2007).
Cohen, S. R. et al. Measuring the quality of life of people at the end of life: The McGill quality of life questionnaire-revised. Palliat. Med. 31, 120–129. https://doi.org/10.1177/0269216316659603 (2017).
Kim, E. S., Shiba, K., Boehm, J. K. & Kubzansky, L. D. Sense of purpose in life and five health behaviors in older adults. Prev. Med. 139, 106172. https://doi.org/10.1016/j.ypmed.2020.106172 (2020).
Nakamura, J. S., Chen, Y., VanderWeele, T. J. & Kim, E. S. What makes life purposeful? Identifying the antecedents of a sense of purpose in life using a lagged exposure-wide approach. SSM Popul. Health 19, 101235. https://doi.org/10.1016/j.ssmph.2022.101235 (2022).
Cheawchanwattana, A. et al. Spiritual well-being and its relationship with patient characteristics and other patient-reported outcomes in peritoneal dialysis patients: Findings from the PDOPPS. Nephrology (Carlton) 27, 621–631. https://doi.org/10.1111/nep.14034 (2022).
Hong, J. H. et al. The positive influence of sense of control on physical, behavioral, and psychosocial health in older adults: An outcome-wide approach. Prev. Med. 149, 106612. https://doi.org/10.1016/j.ypmed.2021.106612 (2021).
Ware, J. Jr., Kosinski, M. & Keller, S. D. A 12-item short-form health survey: Construction of scales and preliminary tests of reliability and validity. Med. Care 34, 220–233. https://doi.org/10.1097/00005650-199603000-00003 (1996).
Gandek, B. et al. Cross-validation of item selection and scoring for the SF-12 health survey in nine countries: Results from the IQOLA project. International quality of life assessment. J. Clin. Epidemiol. 51, 1171–1178. https://doi.org/10.1016/s0895-4356(98)00109-7 (1998).
Auld, J. P., Mudd, J. O., Gelow, J. M., Hiatt, S. O. & Lee, C. S. Self-care moderates the relationship between symptoms and health-related quality of life in heart failure. J. Cardiovasc. Nurs. 33, 217–224. https://doi.org/10.1097/jcn.0000000000000447 (2018).
Cramm, J. M. & Nieboer, A. P. Self-management abilities, physical health and depressive symptoms among patients with cardiovascular diseases, chronic obstructive pulmonary disease, and diabetes. Patient Educ. Couns. 87, 411–415. https://doi.org/10.1016/j.pec.2011.12.006 (2012).
Guo, J. et al. Diabetes self-management, depressive symptoms, quality of life and metabolic control in youth with type 1 diabetes in China. J. Clin. Nurs. 22, 69–79. https://doi.org/10.1111/j.1365-2702.2012.04299.x (2013).
Yun, J. Y., Sim, J. A., Lee, S. & Yun, Y. H. Stronger association of perceived health with socio-economic inequality during COVID-19 pandemic than pre-pandemic era. BMC Public Health 22, 1757. https://doi.org/10.1186/s12889-022-14176-8 (2022).
Jerant, A., Kravitz, R., Moore-Hill, M. & Franks, P. Depressive symptoms moderated the effect of chronic illness self-management training on self-efficacy. Med. Care 46, 523–531. https://doi.org/10.1097/MLR.0b013e31815f53a4 (2008).
Lightfoot, C. J. et al. The codevelopment of “my kidneys & me”: A digital self-management program for people with chronic kidney disease. J. Med. Internet Res. 24, e39657. https://doi.org/10.2196/39657 (2022).
Wei, X. et al. Effects of different interventions on smoking cessation in chronic obstructive pulmonary disease patients: A systematic review and network meta-analysis. Int. J. Nurs. Stud. 136, 104362. https://doi.org/10.1016/j.ijnurstu.2022.104362 (2022).
Salmoirago-Blotcher, E. et al. Mind your heart: Exploring feasibility, acceptability, and preliminary effects of phone-delivered mindfulness training on medication adherence in outpatients with chronic heart failure. J. Cardiovasc. Nurs. 37, 595–602. https://doi.org/10.1097/jcn.0000000000000891 (2022).
Fried, E. I. et al. Using network analysis to examine links between individual depressive symptoms, inflammatory markers, and covariates. Psychol. Med. 50, 2682–2690. https://doi.org/10.1017/s0033291719002770 (2020).
Elovainio, M. et al. Is moderate depression associated with sleep stage architecture in adolescence? Testing the stage type associations using network and transition probability approaches. Psychol. Med. 51, 426–434. https://doi.org/10.1017/s0033291719003453 (2021).
Fischer, R. et al. Association of burnout with depression and anxiety in critical care clinicians in Brazil. JAMA Netw. Open 3, e2030898. https://doi.org/10.1001/jamanetworkopen.2020.30898 (2020).
Zavlis, O. et al. How does the COVID-19 pandemic impact on population mental health? A network analysis of COVID influences on depression, anxiety and traumatic stress in the UK population. Psychol. Med. https://doi.org/10.1017/s0033291721000635 (2021).
Briganti, G., Scutari, M. & McNally, R. J. A tutorial on Bayesian networks for psychopathology researchers. Psychol. Methods https://doi.org/10.1037/met0000479 (2022).
Yun, J. Y., Shim, G. & Jeong, B. Verbal abuse related to self-esteem damage and unjust blame harms mental health and social interaction in college population. Sci. Rep. 9, 5655. https://doi.org/10.1038/s41598-019-42199-6 (2019).
Haslbeck, J. M. B. & Waldorp, L. J. mgm: Estimating time-varying mixed graphical models in high-dimensional data. J. Stat. Softw. 93, 1–46. https://doi.org/10.18637/jss.v093.i08 (2020).
Otieno, P. et al. Multimorbidity of cardiometabolic diseases: A cross-sectional study of patterns, clusters and associated risk factors in sub-Saharan Africa. BMJ Open 13, e064275. https://doi.org/10.1136/bmjopen-2022-064275 (2023).
Schiltz, N. K. Prevalence of multimorbidity combinations and their association with medical costs and poor health: A population-based study of US adults. Front. Public Health 10, 953886. https://doi.org/10.3389/fpubh.2022.953886 (2022).
Alter, P. et al. Disease progression and age as factors underlying multimorbidity in patients with COPD: Results from COSYCONET. Int. J. Chron. Obstruct. Pulmon. Dis. 17, 1703–1713. https://doi.org/10.2147/copd.S364812 (2022).
Sullivan, M. K. et al. The presence and impact of multimorbidity clusters on adverse outcomes across the spectrum of kidney function. BMC Med. 20, 420. https://doi.org/10.1186/s12916-022-02628-2 (2022).
Kuan, V. et al. Identifying and visualising multimorbidity and comorbidity patterns in patients in the English National Health Service: A population-based study. Lancet Digit. Health 5, e16–e27. https://doi.org/10.1016/s2589-7500(22)00187-x (2023).
Tran, T. N., Lee, S., Oh, C. M. & Cho, H. Multimorbidity patterns by health-related quality of life status in older adults: An association rules and network analysis utilizing Korean National Health and Nutrition Examination Survey. Epidemiol. Health. https://doi.org/10.4178/epih.e2022113 (2022).
Kim, S.-H. et al. Assessment of psychometric properties of the Korean SF-12 v2 in the general population. BMC Public Health 14, 1086–1086. https://doi.org/10.1186/1471-2458-14-1086 (2014).
Kroenke, K., Spitzer, R. L. & Williams, J. B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 16, 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x (2001).
Park, S. J., Choi, H. R., Choi, J. H., Kim, K. & Hong, J. P. Reliability and validity of the Korean version of the patient health questionnaire-9 (PHQ-9). Anxiety Mood 6, 119–124. https://doi.org/10.35144/ghn.2017.7.2.71 (2010).
Kang, E., Kim, S., Rhee, Y. E. & Yun, Y. H. Development and validation of the highly effective health behavior pattern inventory—Short form. Chronic Illn. 17, 81–94. https://doi.org/10.1177/1742395319843166 (2021).
Park, S. J., Choi, H. R., Choi, J. H., Kim, K. & Hong, J. P. Reliability and validity of the Korean version of the patient health questionnaire-9 [PHQ-9]. Anxiety Mood 6, 119–124 (2010).
Epskamp, S. & Fried, E. I. A tutorial on regularized partial correlation networks. Psychol. Methods 23, 617–634. https://doi.org/10.1037/met0000167 (2018).
Tu, Y. K. Commentary: Is structural equation modelling a step forward for epidemiologists? Int. J. Epidemiol. 38, 549–551. https://doi.org/10.1093/ije/dyn346 (2009).
Kaplan, D. & Lee, C. Bayesian model averaging over directed acyclic graphs with implications for the predictive performance of structural equation models. Struct. Equ. Model. 23, 343–353. https://doi.org/10.1080/10705511.2015.1092088 (2016).
Haslbeck, J. M. B. & Waldorp, L. J. How well do network models predict observations? On the importance of predictability in network models. Behav. Res. Methods 50, 853–861. https://doi.org/10.3758/s13428-017-0910-x (2018).
Wang, E., Reardon, B., Cherian, B., George, W. T. & Xavier, R. M. Disorder agnostic network structure of psychopathology symptoms in youth. J. Psychiatr. Res. 143, 246–253. https://doi.org/10.1016/j.jpsychires.2021.09.026 (2021).
Tibshirani, R. Regression shrinkage and selection via the lasso. J. R. Stat. Soc. Ser. B (Methodol.) 58, 267–288 (1996).
Epskamp, S., Borsboom, D. & Fried, E. I. Estimating psychological networks and their accuracy: A tutorial paper. Behav. Res. Methods 50, 195–212. https://doi.org/10.3758/s13428-017-0862-1 (2018).
Epskamp, S., Cramer, A. O. J., Waldorp, L. J., Schmittmann, V. D. & Borsboom, D. qgraph: Network visualizations of relationships in psychometric data. J. Stat. Softw. 48, 1–18. https://doi.org/10.18637/jss.v048.i04 (2012).
Rubinov, M. & Sporns, O. Complex network measures of brain connectivity: Uses and interpretations. Neuroimage 52, 1059–1069. https://doi.org/10.1016/j.neuroimage.2009.10.003 (2010).
Haslbeck, J. M. B. & Fried, E. I. How predictable are symptoms in psychopathological networks? A reanalysis of 18 published datasets. Psychol. Med. 47, 2767–2776. https://doi.org/10.1017/s0033291717001258 (2017).
Scutari, M. Learning Bayesian networks with the bnlearn R package. J. Stat. Softw. 35(22), 2010. https://doi.org/10.18637/jss.v035.i03 (2010).
Lazarov, A. et al. Symptom structure of PTSD and co-morbid depressive symptoms—A network analysis of combat veteran patients. Psychol. Med. 50, 2154–2170. https://doi.org/10.1017/s0033291719002034 (2020).
McNally, R. J., Heeren, A. & Robinaugh, D. J. A Bayesian network analysis of posttraumatic stress disorder symptoms in adults reporting childhood sexual abuse. Eur. J. Psychotraumatol. 8, 1341276. https://doi.org/10.1080/20008198.2017.1341276 (2017).
Scutari, M. & Nagarajan, R. Identifying significant edges in graphical models of molecular networks. Artif. Intell. Med. 57, 207–217. https://doi.org/10.1016/j.artmed.2012.12.006 (2013).
Moradi, S. et al. Network modeling of major depressive disorder symptoms in adult women. Psychol. Med. https://doi.org/10.1017/s0033291722002604 (2022).
Scutari, M. Learning Bayesian networks with the bnlearn R package. J. Stat. Softw. 35, 1–22. https://doi.org/10.18637/jss.v035.i03 (2010).
Khidri, F. F. et al. Physical activity, dietary habits and factors associated with depression among medical students of Sindh, Pakistan, during the COVID-19 pandemic. Psychol. Res. Behav. Manag. 15, 1311–1323. https://doi.org/10.2147/prbm.S364540 (2022).
Grabich, S., Farrelly, E., Ortmann, R., Pollack, M. & Wu, S. S. Real-world burden of systemic lupus erythematosus in the USA: A comparative cohort study from the Medical Expenditure Panel Survey (MEPS) 2016–2018. Lupus Sci. Med. 9, 640. https://doi.org/10.1136/lupus-2021-000640 (2022).
Kochovska, S. et al. Persisting breathlessness and activities reduced or ceased: A population study in older men. BMJ Open Respir. Res. 9, 1168. https://doi.org/10.1136/bmjresp-2021-001168 (2022).
Yohannes, A. M. et al. Depressive and anxiety symptoms in patients with COPD: A network analysis. Respir. Med. 198, 106865. https://doi.org/10.1016/j.rmed.2022.106865 (2022).
Badura-Brzoza, K. et al. Comparative assessment of the relationship between emotional factors and quality of life in a group of patients with type 1 and type 2 diabetes—Preliminary report. Psychiatr. Pol. 56, 123–135. https://doi.org/10.12740/PP/OnlineFirst/122461 (2022).
Santos, D. et al. Association between frailty and depression among hemodialysis patients: A cross-sectional study. Sao Paulo Med. J. 140, 406–411. https://doi.org/10.1590/1516-3180.2021.0556.R1.14092021 (2022).
Tanaka, T., Okita, M., Jenkins, S. & Kozu, R. Clinical and psychological impact of chronic pain in people with chronic obstructive pulmonary disease. Int. J. Chron. Obstruct. Pulmon. Dis. 17, 893–903. https://doi.org/10.2147/copd.S359223 (2022).
Gulley, L. D. et al. Examining cognitive-behavioral therapy change mechanisms for decreasing depression, weight, and insulin resistance in adolescent girls at risk for type 2 diabetes. J. Psychosom. Res. 157, 110781. https://doi.org/10.1016/j.jpsychores.2022.110781 (2022).
Vlachou, E. et al. Effectiveness of cognitive behavioral therapy-based interventions on psychological symptoms in adults with type 2 diabetes mellitus: An update review of randomized controlled trials. J. Diabetes Complic. 36, 108185. https://doi.org/10.1016/j.jdiacomp.2022.108185 (2022).
Ng, L., Amatya, B. & Khan, F. Outcomes of a peer support program in multiple sclerosis in an Australian community cohort: A prospective study. J. Neurodegener. Dis. 2013, 429171. https://doi.org/10.1155/2013/429171 (2013).
McPherson, P., Sall, S., Santos, A., Thompson, W. & Dwyer, D. S. Catalytic reaction model of suicide. Front. Psychiatry 13, 817224. https://doi.org/10.3389/fpsyt.2022.817224 (2022).
Bobevski, I. et al. Demoralisation and its link with depression, psychological adjustment and suicidality among cancer patients: A network psychometrics approach. Cancer Med. 11, 815–825. https://doi.org/10.1002/cam4.4406 (2022).
McNally, R. J., Robinaugh, D. J., Deckersbach, T., Sylvia, L. G. & Nierenberg, A. A. Estimating the symptom structure of bipolar disorder via network analysis: Energy dysregulation as a central symptom. J. Psychopathol. Clin. Sci. 131, 86–97. https://doi.org/10.1037/abn0000715 (2022).
Wu, V. X. et al. Development of a community-based e-health program for older adults with chronic diseases: Pilot pre-post study. JMIR Aging 5, e33118. https://doi.org/10.2196/33118 (2022).
Bilgin, A., Muz, G. & Yuce, G. E. The effect of motivational interviewing on metabolic control and psychosocial variables in individuals diagnosed with diabetes: Systematic review and meta-analysis. Patient Educ. Couns. https://doi.org/10.1016/j.pec.2022.04.008 (2022).
Chirumbolo, A., Callea, A. & Urbini, F. The effect of job insecurity and life uncertainty on everyday consumptions and broader life projects during COVID-19 pandemic. Int. J. Environ. Res. Public Health 18, 105363. https://doi.org/10.3390/ijerph18105363 (2021).
Lynch, K. A. et al. Navigating a newly diagnosed cancer through clinician-facilitated discussions of health-related patient values: A qualitative analysis. BMC Palliat. Care 21, 29. https://doi.org/10.1186/s12904-022-00914-7 (2022).
Duarte-Díaz, A. et al. Increased patient empowerment is associated with improvement in anxiety and depression symptoms in type 2 diabetes mellitus: Findings from the INDICA study. Int. J. Environ. Res. Public Health 19, 084818. https://doi.org/10.3390/ijerph19084818 (2022).
Leão, D. et al. The importance of spirituality for women facing breast cancer diagnosis: A qualitative study. Int. J. Environ. Res. Public Health 18, 126415. https://doi.org/10.3390/ijerph18126415 (2021).
Nakata, C. et al. Narrative arcs and shaping influences in long-term medication adherence. Soc. Sci. Med. 285, 114264. https://doi.org/10.1016/j.socscimed.2021.114264 (2021).
Costanza, A. et al. Meaning in life among patients with chronic pain and suicidal ideation: Mixed methods study. JMIR Form. Res. 5, e29365. https://doi.org/10.2196/29365 (2021).
Donatti, L., Malvezzi, H., Azevedo, B. C., Baracat, E. C. & Podgaec, S. Cognitive behavioral therapy in endometriosis, psychological based intervention: A systematic review. Rev. Bras. Ginecol. Obstet. 44, 295–303. https://doi.org/10.1055/s-0042-1742406 (2022).
Cuenca-Martínez, F. et al. Behavior modification techniques on patients with chronic pain in the context of COVID-19 telerehabilitation: An umbrella review. Int. J. Environ. Res. Public Health 19, 095260. https://doi.org/10.3390/ijerph19095260 (2022).
Gagnon, P. et al. A cognitive-existential intervention to improve existential and global quality of life in cancer patients: A pilot study. Palliat. Support Care 13, 981–990. https://doi.org/10.1017/s147895151400073x (2015).
Funding
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIT) (2023R1A2C1006783) and by the Korea Health Technology R&D Project through the Korea Health Industry Development Institute, funded by the Ministry of Health & Welfare, Republic of Korea (HI16C0455).
Author information
Authors and Affiliations
Contributions
Y.H.Y. and J.Y.Y. performed study conceptualization. J.Y.Y. wrote the main manuscript text and prepared all figures. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yun, JY., Yun, Y.H. Health-promoting behavior to enhance perceived meaning and control of life in chronic disease patients with role limitations and depressive symptoms: a network approach. Sci Rep 13, 4848 (2023). https://doi.org/10.1038/s41598-023-31867-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-31867-3
This article is cited by
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.