Abstract
Synthetic antigen-presenting cells (APCs) are used to mediate scalable ex vivo T-cell expansion for adoptive cell therapy. Recently, we developed APC-mimetic scaffolds (APC-ms), which present signals to T cells in a physiological manner to mediate rapid and controlled T-cell expansion. APC-ms are composed of individual high-aspect-ratio silica microrods loaded with soluble mitogenic cues and coated with liposomes of defined compositions, to form supported lipid bilayers. Membrane-bound ligands for stimulation and co-stimulation of T-cell receptors are presented via the fluid, synthetic membranes, while mitogenic cues are released slowly from the microrods. In culture, interacting T cells assemble the individual APC-ms microrods into a biodegradable 3D matrix. Compared to conventional methods, APC-ms facilitates several-fold greater polyclonal T-cell expansion and improved antigen-specific enrichment of rare T-cell subpopulations. Here we provide a detailed protocol for APC-ms synthesis and use for human T-cell activation, and discuss important considerations for material design and T-cell co-culture. This protocol describes the facile assembly of APC-ms in ~4 h and rapid expansion or enrichment of relevant T-cell clones in <2 weeks, and is applicable for T-cell manufacturing and assay development.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
Data for this study are available from the corresponding author upon reasonable request.
Change history
24 January 2020
Fig. 1 as initially published had labels that were too small to be legible. The figure was replaced, and the legend text adapted accordingly, on 24 January 2020.
References
Rosenberg, S. A. & Restifo, N. P. Adoptive cell transfer as personalized immunotherapy for human cancer. Science 348, 62–68 (2015).
June, C. H., Riddell, S. R. & Schumacher, T. N. Adoptive cellular therapy: a race to the finish line. Sci. Transl. Med. 7, 280ps7 (2015).
Tran, E. et al. T-cell transfer therapy targeting mutant KRAS in cancer. N. Engl. J. Med. 375, 2255–2262 (2016).
Zacharakis, N. et al. Immune recognition of somatic mutations leading to complete durable regression in metastatic breast cancer. Nat. Med. 24, 724–730 (2018).
Strønen, E. et al. Targeting of cancer neoantigens with donor-derived T cell receptor repertoires. Science 352, 1337–1341 (2016).
Veatch, J. R. et al. Tumor-infiltrating BRAFV600E-specific CD4+ T cells correlated with complete clinical response in melanoma. J. Clin. Invest. 128, 1563–1568
Tzannou, I. et al. Off-the-shelf virus-specific T cells to treat BK virus, human Herpesvirus 6, Cytomegalovirus, Epstein-Barr virus, and adenovirus infections after allogeneic hematopoietic stem-cell transplantation. J. Clin. Oncol. J. Am. Soc. Clin. Oncol. 35, 3547–3557 (2017).
Chapuis, A. G. et al. Regression of metastatic Merkel cell carcinoma following transfer of polyomavirus-specific T cells and therapies capable of reinducing HLA Class-I. Cancer Immunol. Res. 2, 27–36 (2014).
Papadopoulou, A. et al. Activity of broad-spectrum T cells as treatment for AdV, EBV, CMV, BKV, and HHV6 infections after HSCT. Sci. Transl. Med. 6, 242ra83 (2014).
Balduzzi, A. et al. Polyomavirus JC-targeted T-cell therapy for progressive multiple leukoencephalopathy in a hematopoietic cell transplantation recipient. Bone Marrow Transplant. 46, 987–992 (2011).
Neelapu, S. S. et al. Axicabtagene Ciloleucel CAR T-cell therapy in refractory large B-cell lymphoma. N. Engl. J. Med. 377, 2531–2544 (2017).
Maude, S. L. et al. Tisagenlecleucel in children and young adults with B-cell lymphoblastic leukemia. N. Engl. J. Med. 378, 439–448 (2018).
Kochenderfer, J. N. et al. Long-duration complete remissions of diffuse large B cell lymphoma after anti-CD19 chimeric antigen receptor T cell therapy. Mol. Ther. 25, 2245–2253 (2017).
Park, J. H. et al. Long-term follow-up of CD19 CAR therapy in acute lymphoblastic leukemia. N. Engl. J. Med. 378, 449–459 (2018).
Morgan, R. A. et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science 314, 126–129 (2006).
Robbins, P. F. et al. A pilot trial using lymphocytes genetically engineered with an NY-ESO-1-reactive T-cell receptor: long-term follow-up and correlates with response. Clin. Cancer Res. J. Am. Assoc. Cancer Res. 21, 1019–1027 (2015).
Rapoport, A. P. et al. NY-ESO-1-specific TCR-engineered T cells mediate sustained antigen-specific antitumor effects in myeloma. Nat. Med. 21, 914–921 (2015).
Kageyama, S. et al. Adoptive transfer of MAGE-A4 T-cell receptor gene-transduced lymphocytes in patients with recurrent esophageal cancer. Clin. Cancer Res. 21, 2268–2277 (2015).
Baeuerle, P. A. et al. Synthetic TruC receptors engaging the complete T cell receptor for potent anti-tumor response. Nat. Commun. 10, 2087 (2019).
Tang, J., Hubbard-Lucey, V. M., Pearce, L., O’Donnell-Tormey, J. & Shalabi, A. The global landscape of cancer cell therapy. Nat. Rev. Drug Discov. 17, 465–466 (2018).
Levine, B. L., Miskin, J., Wonnacott, K. & Keir, C. Global manufacturing of CAR T cell therapy. Mol. Ther. Methods Clin. Dev. 4, 92–101 (2017).
Iyer, R. K., Bowles, P. A., Kim, H. & Dulgar-Tulloch, A. Industrializing autologous adoptive immunotherapies: manufacturing advances and challenges. Front. Med. 5, 150 (2018).
Wang, X. et al. Phase 1 studies of central memory-derived CD19 CAR T-cell therapy following autologous HSCT in patients with B-cell NHL. Blood 127, 2980–2990 (2016).
Sade-Feldman, M. et al. Defining T cell states associated with response to checkpoint immunotherapy in melanoma. Cell 175, 998–1013.e20 (2018).
Fraietta, J. A. et al. Determinants of response and resistance to CD19 chimeric antigen receptor (CAR) T cell therapy of chronic lymphocytic leukemia. Nat. Med. 24, 563–571 (2018).
Turtle, C. J. et al. CD19 CAR–T cells of defined CD4+:CD8+ composition in adult B cell ALL patients. J. Clin. Invest 126, 2123–2138 (2016).
Dustin, M. L. T-cell activation through immunological synapses and kinapses. Immunol. Rev. 221, 77–89 (2008).
Comrie, W. A., Li, S., Boyle, S. & Burkhardt, J. K. The dendritic cell cytoskeleton promotes T cell adhesion and activation by constraining ICAM-1 mobility. J. Cell Biol. 208, 457–473 (2015).
Comrie, W. A., Babich, A. & Burkhardt, J. K. F-actin flow drives affinity maturation and spatial organization of LFA-1 at the immunological synapse. J. Cell Biol. 208, 475–491 (2015).
Appel, H., Seth, N. P., Gauthier, L. & Wucherpfennig, K. W. Anergy induction by dimeric TCR ligands. J. Immunol. 166, 5279–5285 (2001).
Lee, K.-H. et al. The immunological synapse balances T cell receptor signaling and degradation. Science 302, 1218–1222 (2003).
Obst, R. The timing of T cell priming and cycling. Front. Immunol. 6, 563 (2015).
Chang, J. T., Wherry, E. J. & Goldrath, A. W. Molecular regulation of effector and memory T cell differentiation. Nat. Immunol. 15, 1104–1115 (2014).
Cheung, A. S., Zhang, D. K. Y., Koshy, S. T. & Mooney, D. J. Scaffolds that mimic antigen-presenting cells enable ex vivo expansion of primary T cells. Nat. Biotechnol. 36, 160–169 (2018).
Croissant, J. G., Fatieiev, Y. & Khashab, N. M. Degradability and clearance of silicon, organosilica, silsesquioxane, silica mixed oxide, and mesoporous silica nanoparticles. Adv. Mater. 29, 1604634 (2017).
Nguyen, T. L., Choi, Y. & Kim, J. Mesoporous silica as a versatile platform for cancer immunotherapy. Adv. Mater. 31, 1803953
GRAS Notices. https://www.accessdata.fda.gov/scripts/fdcc/index.cfm?set=GrASNotices&id=321. Accessed 16 May 2019.
Polonsky, M. et al. Induction of CD4 T cell memory by local cellular collectivity. Science 360, 1201 (2018).
Borsa, M. et al. Modulation of asymmetric cell division as a mechanism to boost CD8+ T cell memory. Sci. Immunol. 4, eaav1730 (2019).
Richter, R. P., Bérat, R. & Brisson, A. R. Formation of solid-supported lipid bilayers: an integrated view. Langmuir 22, 3497–3505 (2006).
Milone, M. C. & Levine, B. L. Powered and controlled T-cell production. Nat. Biomed. Eng. 2, 148–150 (2018).
Houghtelin, A. & Bollard, C. M. Virus-specific T cells for the immunocompromised patient. Front. Immunol. 8, 1272 (2017).
Han, J. et al. CAR-engineered NK cells targeting wild-type EGFR and EGFRvIII enhance killing of glioblastoma and patient-derived glioblastoma stem cells. Sci. Rep. 5, 11483 (2015).
Heczey, A. et al. Invariant NKT cells with chimeric antigen receptor provide a novel platform for safe and effective cancer immunotherapy. Blood 124, 2824–2833 (2014).
Kim, Y. C. et al. Engineered antigen-specific human regulatory T cells: immunosuppression of FVIII-specific T- and B-cell responses. Blood 125, 1107–1115 (2015).
Dolnikov, A., Sylvie, S., Xu, N. & O’Brien, T. Stem cell approach to generate chimeric antigen receptor modified immune effector cells to treat cancer. Blood 124, 2437–2437 (2014).
Satthaporn, S. et al. Dendritic cells are dysfunctional in patients with operable breast cancer. Cancer Immunol. Immunother. 53, 510–518 (2004).
Shinde, P., Fernandes, S., Melinkeri, S., Kale, V. & Limaye, L. Compromised functionality of monocyte-derived dendritic cells in multiple myeloma patients may limit their use in cancer immunotherapy. Sci. Rep. 8, 5705 (2018).
Wölfl, M. & Greenberg, P. D. Antigen-specific activation and cytokine-facilitated expansion of naive, human CD8+ T cells. Nat. Protoc. 9, 950–966 (2014).
Suhoski, M. M. et al. Engineering artificial antigen-presenting cells to express a diverse array of co-stimulatory molecules. Mol. Ther. 15, 981–988 (2007).
Ye, Q. et al. Engineered artificial antigen presenting cells facilitate direct and efficient expansion of tumor infiltrating lymphocytes. J. Transl. Med. 9, 131 (2011).
Eggermont, L. J., Paulis, L. E., Tel, J. & Figdor, C. G. Towards efficient cancer immunotherapy: advances in developing artificial antigen-presenting cells. Trends Biotechnol. 32, 456–465 (2014).
Turtle, C. J. & Riddell, S. R. Artificial antigen-presenting cells for use in adoptive immunotherapy. Cancer J. 16, 374–381 (2010).
Huang, X. et al. DNA-scaffolded biomaterials enable modular and tunable control of cell-based cancer immunotherapies. Preprint at bioRxiv https://www.biorxiv.org/content/10.1101/587105v1 (2019).
Zappasodi, R. et al. The effect of artificial antigen-presenting cells with preclustered anti-CD28/-CD3/-LFA-1 monoclonal antibodies on the induction of ex vivo expansion of functional human antitumor T cells. Haematologica 93, 1523–1534 (2008).
Trickett, A. & Kwan, Y. L. T cell stimulation and expansion using anti-CD3/CD28 beads. J. Immunol. Methods 275, 251–255 (2003).
Mock, U. et al. Automated manufacturing of chimeric antigen receptor T cells for adoptive immunotherapy using CliniMACS prodigy. Cytotherapy 18, 1002–1011 (2016).
Li, Y. & Kurlander, R. J. Comparison of anti-CD3 and anti-CD28-coated beads with soluble anti-CD3 for expanding human T cells: differing impact on CD8 T cell phenotype and responsiveness to restimulation. J. Transl. Med. 8, 104 (2010).
STEMCELL Technologies. Optimization of human t cell expansion protocol: effects of early cell dilution. https://cdn.stemcell.com/media/files/techbulletin/TB27143-Optimization_of_Human_T_Cell_Expansion_Protocol.pdf (2018).
Hickey, J. W. et al. Engineering an artificial T‐cell stimulating matrix for immunotherapy. Adv. Mater. 31, 1807359 (2019).
Sunshine, J. C., Perica, K., Schneck, J. P. & Green, J. J. Particle shape dependence of CD8+ T cell activation by artificial antigen presenting cells. Biomaterials 35, 269–277 (2014).
Ding, Q. et al. RAFTsomes containing epitope-MHC-II complexes mediated CD4+ T cell activation and antigen-specific immune responses. Pharm. Res. 30, 60–69 (2013).
Goldstein, S. A. & Mescher, M. F. Cell-sized, supported artificial membranes (pseudocytes): response of precursor cytotoxic T lymphocytes to class I MHC proteins. J. Immunol. 137, 3383–3392 (1986).
Giannoni, F. et al. Clustering of T cell ligands on artificial APC membranes influences T cell activation and protein kinase C θ translocation to the T cell plasma membrane. J. Immunol. 174, 3204–3211 (2005).
Steenblock, E. R., Fadel, T., Labowsky, M., Pober, J. S. & Fahmy, T. M. An artificial antigen-presenting cell with paracrine delivery of IL-2 impacts the magnitude and direction of the T cell response. J. Biol. Chem. 286, 34883–34892 (2011).
Xie, A. W. & Murphy, W. L. Engineered biomaterials to mitigate growth factor cost in cell biomanufacturing. Curr. Opin. Biomed. Eng. 10, 1–10 (2019).
Bajgain, P. et al. Optimizing the production of suspension cells using the G-Rex “M” series. Mol. Ther. Methods Clin. Dev. 1, 14015 (2014).
Brunauer, S., Emmett, P. H. & Teller, E. Absorption of gases in multimolecular layers. J. Am. Chem. Soc. 60, 309–319 (1938).
Barrett, E. P., Joyner, L. G. & Halenda, P. P. The determination of pore volume and area distributions in porous substances. i. Computations from nitrogen isotherms. J. Am. Chem. Soc. 73, 373–380 (1951).
De Lange, M. F., Vlugt, T. J. H., Gascon, J. & Kapteijn, F. Adsorptive characterization of porous solids: error analysis guides the way. Microporous Mesoporous Mater. 200, 199–215 (2014).
Zamora, C. et al. Binding of platelets to lymphocytes: a potential anti-inflammatory therapy in rheumatoid arthritis. J. Immunol. 198, 3099–3108 (2017).
Acknowledgements
We thank O. Ali, A. Najibi, M. Sobral, and H. Wang for critical reading of the protocol. We are grateful to G. Cuneo, T. Ferrante, H. Ijaz, and C. Johnson for their technical expertise and help. This work was partially supported by the Wyss Institute at Harvard University (D.J.M.), the National Institutes of Health (NIH 1R01EB015498 and U01CA214369 to D.J.M.), the Food and Drug Administration (FDA, RFA-FD-18-023), and a fellowship from the Canadian Institutes of Health Research (CIHR, D.K.Y.Z.). Part of this work was performed at the Center for Nanoscale Systems (CNS) at Harvard University, which is supported by the National Science Foundation (NSF; 1541979).
Author information
Authors and Affiliations
Contributions
A.C.S. conceived the protocol. D.K.Y.Z. and A.S.C. collected and analyzed the experimental data. D.K.Y.Z. designed the figures. D.K.Y.Z., A.S.C., and D.J.M. wrote the paper.
Corresponding author
Ethics declarations
Competing interests
An international patent application (WO2018013797A1) describes APC-ms compositions. A.S.C. is a co-founder of Immulus, Inc. D.J.M. is a co-founder, advisor, and chair of Immulus’ scientific advisory board. D.K.Y.Z. declares no competing interests.
Additional information
Peer review information Nature Protocols thanks Zhen Gu and Christopher Jewell for their contribution to the peer review of this work.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related link
Key reference using this protocol
Cheung, A. S. et al. Nat. Biotechnol. 36, 160–169 (2018): https://www.nature.com/articles/nbt.4047
Integrated supplementary information
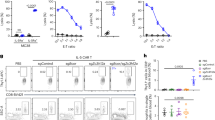
Supplementary Figure 1 Flow cytometry analysis of various T cell subpopulations.
Cell populations should be gated using appropriate fluorescence-minus-one controls. Gating strategy for live CD3+CD8+ T-cell subpopulations is shown; the same approach may be applied for CD3+CD4+ T cells. N: naïve T cell; SCM: stem memory T cell; CM: central memory T cell; EM: effector memory T cell; E: effector T cell.
Supplementary information
Supplementary Information
Supplementary Fig. 1.
Rights and permissions
About this article
Cite this article
Zhang, D.K.Y., Cheung, A.S. & Mooney, D.J. Activation and expansion of human T cells using artificial antigen-presenting cell scaffolds. Nat Protoc 15, 773–798 (2020). https://doi.org/10.1038/s41596-019-0249-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41596-019-0249-0
This article is cited by
-
Subcutaneous biodegradable scaffolds for restimulating the antitumour activity of pre-administered CAR-T cells
Nature Biomedical Engineering (2024)
-
Optimizing the manufacturing and antitumour response of CAR T therapy
Nature Reviews Bioengineering (2023)
-
Enhancing CAR-T cell functionality in a patient-specific manner
Nature Communications (2023)
-
Nanoparticle-mediated cancer cell therapy: basic science to clinical applications
Cancer and Metastasis Reviews (2023)
-
Targeting tumor extracellular matrix activates the tumor-draining lymph nodes
Cancer Immunology, Immunotherapy (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.