Abstract
Limited data is available on factors impacting the outcomes of second hematopoietic cell transplantation (HCT2) in patients with secondary acute myeloid leukemia (sAML). This study aimed to assess HCT2 outcome for sAML comparing reduced-intensity (RIC) to myeloablative (MAC) conditioning. Two hundred and fifteen patients were included: RIC (n = 134), MAC (n = 81). The median follow-up was 41.1 (95% CI: 26.7–69.3) and 28.5 (95% CI: 23.9–75.4) months, respectively. At two years, the relapse incidence (RI) was 58.3% versus 51.1% in RIC and MAC, respectively. The 2-year leukemia free survival (LFS) was 26.6% versus 26%, and the graft-versus-host disease (GVHD)-free, relapse-free survival (GRFS) was 16.4% versus 12.1%, while OS was 31.4% and 39.7%, for RIC and MAC respectively. MVA showed a significantly lower RI [hazard ratio (HR) = 0.46 (95% CI, 0.26–0.8, p = 0.006)] and improved LFS [HR = 0.62 (95% CI, 0.39–0.98, p = 0.042)] with MAC versus RIC. The choice of conditioning regimen did not impact non-relapse mortality [HR = 1.14 (95% CI, 0.52–2.5, p = 0.74)], overall survival (OS) [HR = 0.72 (95% CI, 0.44–1.17, p = 0.18)] or GRFS [HR = 0.89 (95% CI, 0.59–1.36, p = 0.6)]. In conclusion, MAC was associated with a lower RI and superior LFS. These results support the use of MAC for eligible patients with sAML who are being considered for HCT2.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Requests for the raw data used in this study should be sent to CP.
Change history
07 October 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41409-022-01834-z
References
Granfeldt Ostgard LS, Medeiros BC, Sengelov H, Norgaard M, Andersen MK, Dufva IH, et al. Epidemiology and clinical significance of secondary and therapy-related acute myeloid leukemia: a National population-based cohort study. J Clin Oncol. 2015;33:3641–9. https://doi.org/10.1200/jco.2014.60.0890.
Hulegårdh E, Nilsson C, Lazarevic V, Garelius H, Antunovic P, Rangert Derolf Å, et al. Characterization and prognostic features of secondary acute myeloid leukemia in a population-based setting: a report from the Swedish Acute Leukemia Registry. Am J Hematol. 2015;90:208–14. https://doi.org/10.1002/ajh.23908.
Della Porta MG. Prognosis of secondary acute myeloid leukemia. Leuk Res. 2013;37:857–8. https://doi.org/10.1016/j.leukres.2013.04.016.
Park SH, Chi H-S, Cho Y-U, Jang S, Park C-J. Evaluation of prognostic factors in patients with therapy-related acute myeloid leukemia. Blood Res. 2013;48:185 https://doi.org/10.5045/br.2013.48.3.185.
Christiansen DH, Andersen MK, Pedersen-Bjergaard J. Mutations with loss of heterozygosity of p53 are common in therapy-related myelodysplasia and acute myeloid leukemia after exposure to alkylating agents and significantly associated with deletion or loss of 5q, a complex karyotype, and a poor prognosis. J Clin Oncol. 2001;19:1405–13. https://doi.org/10.1200/jco.2001.19.5.1405.
Kayser S, Döhner K, Krauter J, Köhne C-H, Horst HA, Held G, et al. The impact of therapy-related acute myeloid leukemia (AML) on outcome in 2853 adult patients with newly diagnosed AML. Blood. 2011;117:2137–45. https://doi.org/10.1182/blood-2010-08-301713.
Zeichner SB, Arellano ML. Secondary adult acute myeloid leukemia: a review of our evolving understanding of a complex disease process. Curr Treatment Options in Oncol. 2015;16. https://doi.org/10.1007/s11864-015-0355-3.
Litzow MR, Tarima S, Perez WS, Bolwell BJ, Cairo MS, Camitta BM, et al. Allogeneic transplantation for therapy-related myelodysplastic syndrome and acute myeloid leukemia. Blood. 2010;115:1850–7. https://doi.org/10.1182/blood-2009-10-249128.
Sengsayadeth S, Labopin M, Boumendil A, Finke J, Ganser A, Stelljes M, et al. Transplant Outcomes for Secondary Acute Myeloid Leukemia: Acute Leukemia Working Party of the European Society for Blood and Bone Marrow Transplantation Study. Biol Blood Marrow Transpl. 2018;24:1406–14. https://doi.org/10.1016/j.bbmt.2018.04.008.
Schmaelter A-K, Labopin M, Socié G, Itälä-Remes M, Blaise D, Yakoub-Agha I, et al. Inferior outcome of allogeneic stem cell transplantation for secondary acute myeloid leukemia in first complete remission as compared to de novo acute myeloid leukemia. Blood Cancer Journal. 2020;10. https://doi.org/10.1038/s41408-020-0296-3.
Yoshizato T, Nannya Y, Atsuta Y, Shiozawa Y, Iijima-Yamashita Y, Yoshida K, et al. Genetic abnormalities in myelodysplasia and secondary acute myeloid leukemia: impact on outcome of stem cell transplantation. Blood. 2017;129:2347–58. https://doi.org/10.1182/blood-2016-12-754796.
Bazarbachi A, Schmid C, Labopin M, Beelen D, Wolfgang Blau I, Potter V, et al. Evaluation of trends and prognosis over time in patients with AML relapsing after allogeneic hematopoietic cell transplant reveals improved survival for young patients in recent years. Clin Cancer Res. 2020;26:6475–82. https://doi.org/10.1158/1078-0432.ccr-20-3134.
Kharfan-Dabaja MA, Labopin M, Polge E, Nishihori T, Bazarbachi A, Finke J, et al. Association of second allogeneic hematopoietic cell transplant vs donor lymphocyte infusion with overall survival in patients with acute myeloid leukemia relapse. JAMA Oncol. 2018;4:1245–53. https://doi.org/10.1001/jamaoncol.2018.2091.
Shimoni A, Labopin M, Finke J, Ciceri F, Deconinck E, Kröger N, et al. Donor selection for a second allogeneic stem cell transplantation in AML patients relapsing after a first transplant: a study of the Acute Leukemia Working Party of EBMT. Blood Cancer Journal. 2019;9. https://doi.org/10.1038/s41408-019-0251-3.
Schmid C, De Wreede LC, Van Biezen A, Finke J, Ehninger G, Ganser A, et al. Outcome after relapse of myelodysplastic syndrome and secondary acute myeloid leukemia following allogeneic stem cell transplantation: a retrospective registry analysis on 698 patients by the Chronic Malignancies Working Party of the European Society of B. Haematologica. 2018;103:237–45. https://doi.org/10.3324/haematol.2017.168716.
Saraceni F, Scortechini I, Fiorentini A, Dubbini MV, Mancini G, Federici I, et al. Conditioning regimens for frail patients with acute leukemia undergoing allogeneic stem cell transplant: how to strike gently. Clin Hematol Int. 2021. https://doi.org/10.2991/chi.k.210731.001.
Potdar RR, Gupta S, Giebel S, Savani BN, Varadi G, Nagler A, et al. Current status and perspectives of irradiation-based conditioning regimens for patients with acute leukemia undergoing hematopoietic stem cell transplantation. Clin Hematol Int. 2019;1:19–27. https://doi.org/10.2991/chi.d.190218.002.
Sengsayadeth S, Gatwood KS, Boumendil A, Labopin M, Finke J, Ganser A, et al. Conditioning intensity in secondary AML with prior myelodysplastic syndrome/myeloproliferative disorders: an EBMT ALWP study. Blood Adv. 2018;2:2127–35. https://doi.org/10.1182/bloodadvances.2018019976.
Kröger N, Iacobelli S, Franke G-N, Platzbecker U, Uddin R, Hübel K, et al. Dose-reduced versus standard conditioning followed by allogeneic stem-cell transplantation for patients with myelodysplastic syndrome: a prospective randomized phase III study of the EBMT (RICMAC Trial). J Clin Oncol. 2017;35:2157–64. https://doi.org/10.1200/jco.2016.70.7349.
Bacigalupo A, Ballen K, Rizzo D, Giralt S, Lazarus H, Ho V, et al. Defining the intensity of conditioning regimens: working definitions. Biol Blood Marrow Transpl. 2009;15:1628–33. https://doi.org/10.1016/j.bbmt.2009.07.004.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J, et al. 1994 consensus conference on acute GVHD grading. Bone Marrow Transpl. 1995;15:825–8.
Shulman HM, Sullivan KM, Weiden PL, McDonald GB, Striker GE, Sale GE, et al. Chronic graft-versus-host syndrome in man. A long-term clinicopathologic study of 20 Seattle patients. Am J Med. 1980;69:204–17. https://doi.org/10.1016/0002-9343(80)90380-0.
Ruggeri A, Labopin M, Ciceri F, Mohty M, Nagler A Definition of GvHD-free, relapse-free survival for registry-based studies: an ALWP-EBMT analysis on patients with AML in remission. In: Bone Marrow Transplant, vol. 51: England, 2016, 610-1.
Kanate AS, Nagler A, Savani B. Summary of scientific and statistical methods, study endpoints and definitions for observational and registry-based studies in hematopoietic cell transplantation. Clin Hematol Int. 2019;2:2–4. https://doi.org/10.2991/chi.d.191207.001.
R: A language and environment for statistical computing. In. https://www.R-project.org/. R Core Team: R Foundation for Statistical Computing, Vienna, Austria., 2020.
Vrhovac R, Labopin M, Ciceri F, Finke J, Holler E, Tischer J, et al. Second reduced intensity conditioning allogeneic transplant as a rescue strategy for acute leukaemia patients who relapse after an initial RIC allogeneic transplantation: analysis of risk factors and treatment outcomes. Bone Marrow Transpl. 2016;51:186–93. https://doi.org/10.1038/bmt.2015.221.
Ruggeri A, Battipaglia G, Labopin M, Ehninger G, Beelen D, Tischer J, et al. Unrelated donor versus matched sibling donor in adults with acute myeloid leukemia in first relapse: an ALWP-EBMT study. J Hematol Oncol. 2016;9:89 https://doi.org/10.1186/s13045-016-0321-y.
Kharfan‐Dabaja MA, Labopin M, Brissot E, Kroger N, Finke J, Ciceri F, et al. Second allogeneic haematopoietic cell transplantation using HLA‐matched unrelated versus T‐cell replete haploidentical donor and survival in relapsed acute myeloid leukaemia. Br J Haematol. 2021;193:592–601. https://doi.org/10.1111/bjh.17426.
Kantarjian H, Kadia T, Dinardo C, Daver N, Borthakur G, Jabbour E, et al. Acute myeloid leukemia: current progress and future directions. Blood Cancer Journal. 2021;11. https://doi.org/10.1038/s41408-021-00425-3.
Schmid C, Labopin M, Schaap N, Veelken H, Schleuning M, Stadler M, et al. Prophylactic donor lymphocyte infusion after allogeneic stem cell transplantation in acute leukaemia - a matched pair analysis by the Acute Leukaemia Working Party of EBMT. Br J Haematol. 2018. https://doi.org/10.1111/bjh.15691.
Nagler A, Labopin M, Dholaria B, Finke J, Brecht A, Schanz U, et al. Second allogeneic stem cell transplantation in patients with acute lymphoblastic leukaemia: a study on behalf of the Acute Leukaemia Working Party of the European Society for Blood and Marrow Transplantation. Br J Haematol. 2019;186:767–76. https://doi.org/10.1111/bjh.15973.
Andreola G, Labopin M, Beelen D, Chevallier P, Tabrizi R, Bosi A, et al. Long-term outcome and prognostic factors of second allogeneic hematopoietic stem cell transplant for acute leukemia in patients with a median follow-up of 10 years. Bone Marrow Transpl. 2015;50:1508–12. https://doi.org/10.1038/bmt.2015.193.
Schmid C, Labopin M, Nagler A, Bornhauser M, Finke J, Fassas A, et al. Donor lymphocyte infusion in the treatment of first hematological relapse after allogeneic stem-cell transplantation in adults with acute myeloid leukemia: a retrospective risk factors analysis and comparison with other strategies by the EBMT Acute Leukemia Working Party. J Clin Oncol. 2007;25:4938–45. https://doi.org/10.1200/jco.2007.11.6053.
Schmid C, Labopin M, Nagler A, Niederwieser D, Castagna L, Tabrizi R, et al. Treatment, risk factors, and outcome of adults with relapsed AML after reduced intensity conditioning for allogeneic stem cell transplantation. Blood. 2012;119:1599–606. https://doi.org/10.1182/blood-2011-08-375840.
Saraceni F, Labopin M, Forcade E, Kröger N, Socié G, Niittyvuopio R, et al. Allogeneic stem cell transplant in patients with acute myeloid leukemia and karnofsky performance status score less than or equal to 80%: A study from the acute leukemia working party of the European Society for Blood and Marrow Transplantation (EBMT). Cancer Med. 2021;10:23–33. https://doi.org/10.1002/cam4.3593.
Ringden O, Boumendil A, Labopin M, Canaani J, Beelen D, Ehninger G, et al. Outcome of Allogeneic Hematopoietic Stem Cell Transplantation in Patients Age >69 Years with Acute Myelogenous Leukemia: On Behalf of the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation. Biol Blood Marrow Transplant 2019. e-pub ahead of print 2019/06/11; https://doi.org/10.1016/j.bbmt.2019.05.037.
Nagler A, Dholaria B, Labopin M, Socie G, Huynh A, Itälä-Remes M, et al. The impact of anti-thymocyte globulin on the outcomes of Patients with AML with or without measurable residual disease at the time of allogeneic hematopoietic cell transplantation. Leukemia. 2020;34:1144–53. https://doi.org/10.1038/s41375-019-0631-5.
Acknowledgements
We thank all the European Society for Blood and Marrow Transplantation (EBMT) centers and national registries for contributing patients to this study (Supplementary Appendix Material). We also thank the data managers for their excellent work and the patients who contributed their data.
Author information
Authors and Affiliations
Contributions
AN, MM, and ML- contributed to the conception and design of the study; ML- analyzed the data; AN, BD, BNS, ML, MM- contributed to the writing of the manuscript; All authors critically reviewed the manuscript and approved the final version.
Corresponding author
Ethics declarations
Competing interests
HCR received consulting and lecture fees from Abbvie, AstraZeneca, Vertex and Merck. HCR received research funding from Gilead Pharmaceuticals. HCR is a co-founder of CDL Therapeutics GmbH. BD reported Institutional research funding: Takeda, Janssen, Angiocrine, Pfizer, Poseida, MEI, Sorrento. Consultancy: Jazz, Gamida Cell, MJH BioScience The remaining authors report no relevant conflict of interest concerning this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
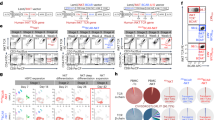
The original online version of this article was revised: The caption of Fig. 1 was corrected to read “Transplant outcomes. Non-relapse mortality (a, NRM), relapse incidence (b, RI), leukemia-free survival (c, LFS), and overall survival (d, OS) of patients receiving reduced intensity versus myeloablative conditioning regimen”.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nagler, A., Peczynski, C., Dholaria, B. et al. Impact of conditioning regimen intensity on outcomes of second allogeneic hematopoietic cell transplantation for secondary acute myelogenous leukemia. Bone Marrow Transplant 57, 1116–1123 (2022). https://doi.org/10.1038/s41409-022-01693-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-022-01693-8
This article is cited by
-
Validation of the transplant conditioning intensity (TCI) index for allogeneic hematopoietic cell transplantation
Bone Marrow Transplantation (2024)
-
Continuously improving outcome over time after second allogeneic stem cell transplantation in relapsed acute myeloid leukemia: an EBMT registry analysis of 1540 patients
Blood Cancer Journal (2024)
-
Non-T-depleted haploidentical transplantation with post-transplant cyclophosphamide in patients with secondary versus de novo AML in first complete remission: a study from the ALWP/EBMT
Journal of Hematology & Oncology (2023)