Abstract
Prostate cancer has the widest racial disparities of any cancer, and these disparities appear at every stage of the cancer continuum. This review focuses on the disparities in prostate cancer between Black and White men, spanning from prevention and screening to clinical outcomes. We conduct an expansive review of the literature on racial disparities in prostate cancer, interpret the findings, and discuss areas of unmet need in research. We provide an overview of epidemiologic concepts necessary to understanding the current state of prostate cancer disparities, discuss the complexities of studying race, and review potential drivers of disparities in incidence and mortality. We argue that the cause of this disparity is multifactorial and due to a combination of social and environmental factors. The path forward needs to focus on enrolling and retaining Black men in prostate cancer clinical trials and observational studies and identifying potential interventions to improve prevention and clinical outcomes in Black men.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
DeSantis CE, Miller KD, Goding Sauer A, Jemal A, Siegel RL. Cancer statistics for African Americans, 2019. CA Cancer J Clin. 2019;69:211–33.
Mokdad AH, Dwyer-Lindgren L, Fitzmaurice C, Stubbs RW, Bertozzi-Villa A, Morozoff C, et al. Trends and patterns of disparities in cancer mortality among US Counties, 1980-2014. J Am Med Assoc. 2017;317(Jan):388–406.
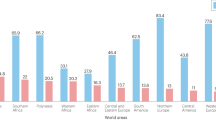
Culp MBB, Soerjomataram I, Efstathiou JA, Bray F, Jemal A. Recent global patterns in prostate cancer incidence and mortality rates. Eur Urol. 2020;77:38–52. https://doi.org/10.1016/j.eururo.2019.08.005.
Ellis L, Canchola AJ, Spiegel D, Ladabaum U, Haile R, Lin Gomez S. Racial and ethnic disparities in cancer survival: the contribution of tumor, sociodemographic, institutional, and neighborhood characteristics. J Clin Oncol. 2017;36:25–33. https://doi.org/10.1200/JCO.2017. Available from
Klebaner D, Courtney PT, Rose BS. Effect of healthcare system on prostate cancer-specific mortality in African American and non-Hispanic white men. J Clin Oncol. 2021;39:23–23.
Dess RT, Hartman HE, Mahal BA, Soni PD, Jackson WC, Cooperberg MR, et al. Association of black race with prostate cancer-specific and other-cause mortality. JAMA Oncol. 2019;5:975–83.
Mahal BA, Berman RA, Taplin M-E, Huang FW. Prostate cancer–specific mortality across gleason scores in black vs nonblack men. J Am Med Assoc. 2018;320(Dec):2479–81.
Williams VL, Awasthi S, Fink AK, Pow-Sang JM, Park JY, Gerke T, et al. African-American men and prostate cancer-specific mortality: a competing risk analysis of a large institutional cohort, 1989–2015. Cancer Med. 2018;7(May):2160–71.
Gerke T, Awasthi S, Yamoah K. Biology vs access to care—relative contribution to racial disparities in prostate cancer. JAMA Oncol. 2019;5(Dec):1809–10.
Schaefer RT. Encyclopedia of race, ethnicity, and society. Thousand Oaks: SAGE Publications; 2008.
Kaplan JB, Bennett T. Use of race and ethnicity in biomedical publication. J Am Med Assoc 2003;289:2709–16.
Giovannucci E, Liu Y, Platz EA, Stampfer MJ, Willett WC. Risk factors for prostate cancer incidence and progression in the health professionals follow-up study. Int J Cancer 2007;121:1571–8.
Pernar CH, Ebot EM, Wilson KM, Mucci LA. The epidemiology of prostate cancer. Cold Spring Harb Perspect Med. 2018;8:a030361. https://doi.org/10.1101/cshperspect.a030361.
Mucci LA, Hjelmborg JB, Harris JR, Czene K, Havelick DJ, Scheike T, et al. Familial risk and heritability of cancer among twins in Nordic countries. JAMA. 2017;315:68–76.
Conti DV, Darst BF, Moss LC, Saunders EJ, Sheng X, Chou A, et al. Trans-ancestry genome-wide association meta-analysis of prostate cancer identifies new susceptibility loci and informs genetic risk prediction. Nat Genet. 2021;53:65–75.
Haiman CA, Chen GK, Blot WJ, Strom SS, Berndt SI, Kittles RA, et al. Characterizing genetic risk at known prostate cancer susceptibility loci in African Americans. PLoS Genet. 2011;7:1–11.
Conti DV, Wang K, Sheng X, Bensen JT, Hazelett DJ, Cook MB, et al. Two novel susceptibility loci for prostate cancer in men of African Ancestry. J Natl Cancer Inst. 2017;109:8–12.
Ginde AA, Liu MC, Camargo CA. Demographic differences and trends of vitamin D insufficiency in the US Population, 1988-2004. Arch Intern Med. 2009;169(Mar):626–32.
Pool LR, Ning H, Lloyd-Jones DM, Allen NB. Trends in racial/ethnic disparities in cardiovascular health among US adults from 1999-2012. J Am Heart Assoc. 2017;6. https://doi.org/10.1161/JAHA.117.006027.
Jackson CL, Szklo M, Yeh HC, Wang NY, Dray-Spira R, Thorpe R, et al. Black-white disparities in overweight and obesity trends by educational attainment in the United States, 1997–2008. J Obes. 2013;2013:140743–49.
Iyer HS, James P, Valeri L, Hart JE, Pernar CH, Mucci LA, et al. The association between neighborhood greenness and incidence of lethal prostate cancer. Environ Epidemiol. 2020;4:e091.
Krieger N, Feldman JM, Kim R, Waterman PD. Cancer incidence and multilevel measures of residential economic and racial segregation for cancer registries. JNCI Cancer Spectr. 2018;2:1–10.
Jones MR, Diez-Roux AV, Hajat A, Kershaw KN, O’Neill MS, Guallar E, et al. Race/ethnicity, residential segregation, and exposure to ambient air pollution: the Multi-Ethnic Study of Atherosclerosis (MESA). Am J Public Health 2014;104:2130–7.
Kloog I, Haim A, Stevens RG, Portnov BA. Global co-distribution of light at night (LAN) and cancers of prostate, colon, and lung in men. Chronobiol Int. 2009;26:108–25.
Garcia-Saenz A, de Miguel AS, Espinosa A, Valentin A, Aragonés N, Llorca J, et al. Evaluating the association between artificial light-at-night exposure and breast and prostate cancer risk in Spain (Mcc-spain study). Environ Health Perspect. 2018;126:1–11.
Vigneswaran HT, Jagai JS, Greenwald DT, Patel AP, Kumar M, Dobbs RW, et al. Association between environmental quality and prostate cancer stage at diagnosis. Prostate Cancer Prostatic Dis. 2021 https://doi.org/10.1038/s41391-021-00370-z.
Kearns JT, Adeyemi O, Anderson WE, Hetherington TC, Taylor YJ, Zhu J, et al. Contemporary racial disparities in PSA screening in a large, integrated health care system. J Clin Oncol. 2020;38:308.
Preston MA, Gerke T, Carlsson SV, Signorello L, Sjoberg DD, Markt SC, et al. Baseline prostate-specific antigen level in midlife and aggressive prostate cancer in black men (Figure presented.). Eur Urol. 2019;75(Mar):399–407.
Moyer VA. Screening for Prostate Cancer: U.S. Preventive Services Task Force Recommendation Statement [Internet]. Available from https://annals.org.
Drazer MW, Huo D, Eggener SE. National prostate cancer screening rates after the 2012 US Preventive Services Task Force recommendation discouraging prostate-specific antigen-based screening. J Clin Oncol. 2015;33(Aug):2416–23.
Kensler KH, Pernar CH, Mahal BA, Nguyen PL, Trinh Q-D, Kibel AS, et al. Racial and ethnic variation in PSA testing and prostate cancer incidence following the 2012 USPSTF recommendation. JNCI J Natl Cancer Inst. 2021;113:719–726.
Kelly SP, Anderson WF, Rosenberg PS, Cook MB. Past, current, and future incidence rates and burden of metastatic prostate cancer in the United States. Eur Urol. Focus 2018;4(Jan):121–7.
Grossman DC, Curry SJ, Owens DK, Bibbins-Domingo K, Caughey AB, Davidson KW, et al. Screening for prostate cancer: US preventive services task force recommendation statement. J Am Med Assoc 2018;319(May):1901–13.
Nyame YA, Gulati R, Heijnsdijk EAM, Tsodikov A, Mariotto AB, Gore JL, et al. The impact of intensifying prostate cancer screening in black men: a model-based analysis. JNCI J Natl Cancer Inst. 2021. https://doi.org/10.1093/jnci/djab072.
Halabi S, Dutta S, Tangen CM, Rosenthal M, Petrylak DP, Thompson IM, et al. Overall survival of black and white men with metastatic castration-resistant prostate cancer treated with docetaxel. J Clin Oncol. 2019;37:403–10.
Roach M, Pilepich MV, Asbell SO, Mohiuddin M, Grignon D. Race and survival of men treated for prostate cancer on radiation therapy oncology group phase III randomized trials. J Urol. 2003;169:245–250.
Halabi S, Dutta S, Tangen CM, Rosenthal M, Petrylak DP, Chi KN, et al. Clinical outcomes in men of diverse ethnic backgrounds with metastatic castration-resistant prostate cancer. J Clin Oncol. 2020;31(Apr):930–41.
Spratt DE, Chen YW, Mahal BA, Osborne JR, Zhao SG, Morgan TM, et al. Individual patient data analysis of randomized clinical trials: impact of black race on castration-resistant prostate cancer outcomes. Eur Urol Focus. 2016;2:532–9.
Sartor O, Armstrong AJ, Ahaghotu C, McLeod DG, Cooperberg MR, Penson DF, et al. Survival of African-American and Caucasian men after sipuleucel-T immunotherapy: outcomes from the PROCEED registry. Prostate Cancer Prostatic Dis. 2020;23:517–26. Available from https://doi.org/10.1038/s41391-020-0213-7.
Zhao H, Howard LE, De Hoedt A, Terris MK, Amling CL, Kane CJ, et al. Racial discrepancies in overall survival among men treated with 223radium. J Urol. 2020;203:331–7.
Ramalingam S, Humeniuk MS, Hu R, Rasmussen J, Healy P, Wu Y, et al. Prostate-specific antigen response in black and white patients treated with abiraterone acetate for metastatic castrate–resistant prostate cancer. Urol Oncol Semin Orig Investig. 2017;35(Jun):418–24.
George DJ, Heath EI, Sartor AO, Sonpavde G, Berry WR, Healy P, et al. Abi Race: A prospective, multicenter study of black (B) and white (W) patients (pts) with metastatic castrate resistant prostate cancer (mCRPC) treated with abiraterone acetate and prednisone (AAP). J Clin Oncol. 2018;36:LBA5009–LBA5009.
Mahal BA, Alshalalfa M, Kensler KH, Chowdhury-Paulino I, Kantoff P, Mucci LA, et al. Racial differences in genomic profiling of prostate cancer. New Engl. J. Med. 2020;383:1081–3.
Zhou CK, Young D, Yeboah ED, Coburn SB, Tettey Y, Biritwum RB, et al. TMPRSS2:ERG gene fusions in prostate cancer of west African men and aMeta-analysis of racial differences. Am J Epidemiol. 2017;186(Dec):1352–61.
Tosoian JJ, Almutairi F, Morais CL, Glavaris S, Hicks J, Sundi D, et al. Prevalence and Prognostic Significance of PTEN Loss in African-American and European-American men undergoing radical prostatectomy. Eur Urol. 2017;71(May):697–700.
Koga Y, Song H, Chalmers ZR, Newberg J, Kim E, Carrot-Zhang J, et al. Genomic profiling of prostate cancers from men with African and European Ancestry. Clin Cancer Res. 2020;26(Sep):4651–60.
Yuan J, Kensler KH, Hu Z, Zhang Y, Zhang T, Jiang J, et al. Integrative comparison of the genomic and transcriptomic landscape between prostate cancer patients of predominantly African or European genetic ancestry. PLoS Genet. 2020;16:1–26. https://doi.org/10.1371/journal.pgen.1008641.
Ahearn TU, Pettersson A, Ebot EM, Gerke T, Graff RE, Morais CL, et al. A prospective investigation of PTEN loss and ERG expression in lethal prostate cancer. J Natl Cancer Inst. 2016;108:djv346.
Abeshouse A, Ahn J, Akbani R, Ally A, Amin S, Andry CD, et al. The molecular taxonomy of primary prostate. Cancer Cell 2015;163(Nov):1011–25.
Pernar CH, Ebot EM, Pettersson A, Graff RE, Giunchi F, Ahearn TU, et al. A prospective study of the association between physical activity and risk of prostate cancer defined by clinical features and TMPRSS2:ERG. Eur Urol. 2019;76(Jul):33–40.
Creed JH, Berglund AE, Rounbehler RJ, Awasthi S, Cleveland JL, Park JY, et al. Commercial gene expression tests for prostate cancer prognosis provide paradoxical estimates of race-specific risk. Cancer Epidemiol Biomark Prev. 2020;29(Jan):246–53.
Cullen J, Lynch JA, Klein EA, Van Den Eeden SK, Carroll PR, Mohler JL, et al. Multicenter comparison of 17-gene genomic prostate score as a predictor of outcomes in African American and Caucasian American Men with clinically localized prostate cancer. J Urol. 2021;205(Apr):1047–54.
Feng FY, Huang HC, Spratt DE, Zhao S (George), Sandler HM, et al. Validation of a 22-gene genomic classifier in patients with recurrent prostate cancer: an ancillary study of the NRG/RTOG 9601 randomized clinical trial. JAMA Oncol. 2021;7:544–552.
Canter DJ, Reid J, Latsis M, Variano M, Halat S, Rajamani S, et al. Comparison of the prognostic utility of the cell cycle progression score for predicting clinical outcomes in African American and Non-African American Men with localized prostate cancer. Eur Urol. 2019;75(Mar):515–22.
Murphy AB, Abern MR, Liu L, Wang H, Hollowell CMP, Sharifi R, et al. Impact of a genomic test on treatment decision in a predominantly African American population with favorable-risk prostate cancer: a randomized trial. J Clin Oncol. 2021;39:1660–70.
Rencsok EM, Bazzi LA, McKay RR, Huang FW, Friedant A, Vinson J, et al. Diversity of enrollment in prostate cancer clinical trials: current status and future directions. Cancer Epidemiol Biomark Prev. 2020;29(Jul):1374–80.
Spratt DE, Osborne JR. Disparities in castration-resistant prostate cancer trials. J. Clin. Oncol. 2015;33:1101–3.
Rivers D, August EM, Sehovic I, Lee Green B, Quinn GP, A systematic review of the factors influencing African Americans’ participation in cancer clinical trials. Contemp. Clin. Trials 2013;35:13–32.
Langford AT, Resnicow K, Dimond EP, Denicoff AM, Germain DS, McCaskill-Stevens W, et al. Racial/ethnic differences in clinical trial enrollment, refusal rates, ineligibility, and reasons for decline among patients at sites in the National Cancer Institute’s Community Cancer Centers Program. Cancer 2014;120(Mar):877–84.
Anwuri VV, Hall LE, Mathews K, Springer BC, Tappenden JR, Farria DM, et al. An institutional strategy to increase minority recruitment to therapeutic trials. Cancer Causes Control 2013;24(Oct):1797–809.
Ghebre RG, Jones LA, Wenzel JA, Martin MY, Durant RW, Ford JG. State-of-the-science of patient navigation as a strategy for enhancing minority clinical trial accrual. Cancer 2014;120:1122–30.
Acknowledgements
We thank the Prostate Cancer Foundation for its ongoing support. LAM was a Prostate Cancer Foundation Young Investigator.
Author information
Authors and Affiliations
Contributions
Conceptualization: LAM, DG, DS, and ICP, Literature review: ICP and CE, Writing: ICP, CE, and LAM, Editing: LAM, DS, RV, and DG. All authors reviewed and approved the paper prior to submission.
Corresponding author
Ethics declarations
Conflict of interest
D.G.: American Association for Cancer Research—Sr Editor, Astellas—Consultant, Research, Advisory Board. AstraZeneca—Research, Consultant, Advisory Board, CAPI-281 Steering Committee member. Axess Oncology—Independent Contractor. Bayer H/C Pharmaceuticals—Consultant, Speaker, Honorarium, Travel accommodations, SC. BMS—Consultant, Research, Steering Committee. Calithera—Research. Capio Biosciences—Scientific Advisory Board. Constellation Pharmaceuticals—Consultant (09/2020). EMD Serono—Honorarium. Exelixis, Inc.—Research, Consultant, Speaker, Honorarium, Travel accommodations Flatiron—Consultant. Ipsen—Honorarium. Janssen Pharmaceuticals—Research, Consultant, Independent Data Monitoring Committee (IDMC). Merck Sharp & Dohme—Consultant. Michael J. Hennessey Associates—Honorarium, Consultant. Millennium Medical Publishing, Clinical Advances in Hematology & Oncology—Co-Editor-in-Chief. Modra Pharmaceuticals B.V.—Advisory Board. Myovant Sciences, Inc.—Consultant. NCI Genitourinary Steering Committee member (Leidos Biomedical Research Inc.). Nektar Therapeutics—Steering Committee. Novartis—Research. Physician Education Resource LLC—Consultant. Pfizer—Research, Consultant, Steering Committee, Honorarium. Propella TX—Consultant (formerly Vizuri). RevHealth, LLC—Consultant—01/2021. Sanofi—Research, Consultant, Speaker, Honorarium, Travel accommodations. UroGPO—Honorarium. UroToday—Honorarium, Travel accommodations. D.S.: Personal fees: Janssen, Blue Earth, Boston Scientific, AstraZeneca. Funding: Janssen. The remaining authors declare that they have no conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chowdhury-Paulino, I.M., Ericsson, C., Vince Jr., R. et al. Racial disparities in prostate cancer among black men: epidemiology and outcomes. Prostate Cancer Prostatic Dis 25, 397–402 (2022). https://doi.org/10.1038/s41391-021-00451-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41391-021-00451-z
This article is cited by
-
The complex interplay of modifiable risk factors affecting prostate cancer disparities in African American men
Nature Reviews Urology (2024)
-
Racial and socioeconomic disparities in survival improvement of eight cancers
BJC Reports (2024)
-
Recent advances and future perspectives in the therapeutics of prostate cancer
Experimental Hematology & Oncology (2023)
-
Race-dependent association of clinical trial participation with improved outcomes for high-risk prostate cancer patients treated in the modern era
Prostate Cancer and Prostatic Diseases (2023)
-
Genetic and biological drivers of prostate cancer disparities in Black men
Nature Reviews Urology (2023)