Abstract
Objective
To evaluate the impact of antenatal corticosteroid therapy (ACS) on birth outcomes in term infants exposed during pregnancy.
Study design
Exposed newborns were compared with non-exposed controls in a 1 to 2 design. Multivariate analysis was used to assess the effect of ACS exposure on neonatal outcomes.
Result
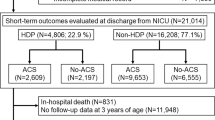
408 newborns were included (136 exposed to ACS, 272 non-exposed). Mean ± SD head circumference (HC) was 33.7 ± 1.4 vs 34.3 ± 1.6 cm, p = 0.001 in exposed vs controls; birth weight was 3.1 ± 0.4 vs 3.3 ± 0.4 kg, p = 0.0001; and birth height was 47.9 ± 2.1 vs. 49.1 ± 2.0 cm, p < 0.0001. Hypocalcemia (4.4 vs 0.7%, p = 0.019) and feeding difficulties (5.1 vs 1.5%, p = 0.047) were significantly more common in exposed newborns. Multivariate analysis for HC showed a significant independent association with ACS exposure (β = −0.5, p = 0.009).
Conclusion
Term newborns exposed to ACS have lower birth HC and higher risk of neonatal complications.
Clinical trial registration
NCT05640596.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Liggins GC, Howie RN. A controlled trial of antepartum glucocorticoid treatment for prevention of the respiratory distress syndrome in premature infants. Pediatrics. 1972;50:515–25.
Philip AGS. The evolution of neonatology. Pediatr Res. 2005;58:799–815. https://doi.org/10.1203/01.PDR.0000151693.46655.66.
Ancel P-Y, Goffinet F, Kuhn P, Langer B, Matis J.EPIPAGE-2 Writing Group et al. Survival and morbidity of preterm children born at 22 through 34 weeks’ gestation in France in 2011: results of the EPIPAGE-2 cohort study. JAMA Pediatr. 2015;169:230–8. https://doi.org/10.1001/jamapediatrics.2014.3351.
Effect of corticosteroids for fetal maturation on perinatal outcomes. NIH Consens Statement. 1994;12:1–24.
Smrcek JM, Schwartau N, Kohl M, Berg C, Geipel A, Krapp M, Diedrich K, Ludwig M. Antenatal corticosteroid therapy in premature infants. Arch Gynecol Obstet. 2005;271:26–32. https://doi.org/10.1007/s00404-004-0664-4.
Cabrol D, Goffinet F, Carbonne B, Drefus M. La menace d’accouchement prématuré (MAP) a membranes intactes. J Gyn Obs Biol Rep 2002.
Frändberg J, Sandblom J, Bruschettini M, Maršál K, Kristensen K. Antenatal corticosteroids: a retrospective cohort study on timing, indications and neonatal outcome. Acta Obstet Gynecol Scand. 2018;97:591–7. https://doi.org/10.1111/aogs.13301.
Optimal timing of antenatal corticosteroid administration and preterm neonatal and early childhood outcomes. Am J Obstet Gynecol MFM. 2020. https://doi.org/10.1016/j.ajogmf.2019.100077.
Jobe AH, Wada N, Berry LM, Ikegami M, Ervin MG. Single and repetitive maternal glucocorticoid exposures reduce fetal growth in sheep. Am J Obstet Gynecol. 1998;178:880–5. https://doi.org/10.1016/s0002-9378(98)70518-6.
Scheepens A, van de Waarenburg M, van den Hove D, Blanco CE. A single course of prenatal betamethasone in the rat alters postnatal brain cell proliferation but not apoptosis. J Physiol. 2003;552:163–75. https://doi.org/10.1113/jphysiol.2003.043414.
Rodriguez A, Wang Y, Ali Khan A, Cartwright R, Gissler M, Järvelin M-R. Antenatal corticosteroid therapy (ACT) and size at birth: a population-based analysis using the Finnish Medical Birth Register. PLoS Med. 2019;16:e1002746. https://doi.org/10.1371/journal.pmed.1002746.
Crowther CA, Middleton PF, Voysey M, Askie L, Zhang S, Martlow TK. et al. Effects of repeat prenatal corticosteroids given to women at risk of preterm birth: An individual participant data meta-analysis. PLoS Med. 2019;16:e1002771. https://doi.org/10.1371/journal.pmed.1002771.
Räikkönen K, Gissler M, Kajantie E. Associations between maternal antenatal corticosteroid treatment and mental and behavioral disorders in children. JAMA. 2020;323:1924–33. https://doi.org/10.1001/jama.2020.3937.
Aviram A, Murphy K, McDonald S, Asztalos E, Zaltz A, Redelmeier D. et al. Antenatal corticosteroids and neurodevelopmental outcomes in late preterm births. Arch Dis Child Fetal Neonatal Ed. 2022;107:250–5. https://doi.org/10.1136/archdischild-2021-322152.
Melamed N, Asztalos E, Murphy K, Zaltz A, Redelmeier D, Shah BR. et al. Neurodevelopmental disorders among term infants exposed to antenatal corticosteroids during pregnancy: a population-based study. BMJ Open. 2019;9:e031197. https://doi.org/10.1136/bmjopen-2019-031197.
Harding JE, Harris DL, Hegarty JE, Alsweiler JM, McKinlay CJ. An emerging evidence base for the management of neonatal hypoglycaemia. Early Hum Dev. 2017;104:51–6. https://doi.org/10.1016/j.earlhumdev.2016.12.009.
Cho WI, Yu HW, Chung HR, Shin CH, Yang SW, Choi CW. et al. Clinical and laboratory characteristics of neonatal hypocalcemia. Ann Pediatr Endocrinol Metab. 2015;20:86–91. https://doi.org/10.6065/apem.2015.20.2.86.
Lauria E. Courbes personnalisées versus courbes standardisées pour l’évaluation de la croissance périnatale: une étude prospective dans le service de Néonatologie à la Maternité Régionale Universitaire de Nancy. https://hal.univ-lorraine.fr/hal-01733457v.
Thorp JA, Jones PG, Knox E, Clark RH. Does antenatal corticosteroid therapy affect birth weight and head circumference?. Obstet Gynecol. 2002;99:101–8. https://doi.org/10.1016/S0029-7844(01)01656-8.
Murphy KE, Hannah ME, Willan AR, Hewson SA, Ohlsson A, Kelly EN. et al. Multiple courses of antenatal corticosteroids for preterm birth (MACS): a randomised controlled trial. Lancet Lond Engl. 2008;372:2143–51. https://doi.org/10.1016/S0140-6736(08)61929-7.
Abbasi S, Hirsch D, Davis J, Tolosa J, Stouffer N, Debbs R. et al. Effect of single versus multiple courses of antenatal corticosteroids on maternal and neonatal outcome. Am J Obstet Gynecol. 2000;182:1243–9. https://doi.org/10.1067/mob.2000.104789.
Bevilacqua E, Brunelli R, Anceschi MM. Review and meta-analysis: benefits and risks of multiple courses of antenatal corticosteroids. J Matern Fetal Neonatal Med. 2010;23:244–60. https://doi.org/10.1080/14767050903165222.
Diguisto C, Arthuis C, Couderchet J, Morgan AS, Perrotin F, Rivière O. et al. Impact of antenatal corticosteroids on head circumference of full-term newborns: a French multicenter cohort study. Acta Obstet Gynecol Scand. 2020;99:1147–54. https://doi.org/10.1111/aogs.13839.
Stathis SL, O’Callaghan M, Harvey J, Rogers Y. Head circumference in ELBW babies is associated with learning difficulties and cognition but not ADHD in the school-aged child. Dev Med Child Neurol. 1999;41:375–80. https://doi.org/10.1111/j.1469-8749.1999.tb00622.x.
Wapner RJ, Sorokin Y, Mele L, Johnson F, Dudley DJ, Spong CY. et al. Long-term outcomes after repeat doses of antenatal corticosteroids. N Engl J Med. 2007;357:1190–8. https://doi.org/10.1056/NEJMoa071453.
Ninan K, Liyanage SK, Murphy KE, Asztalos EV, McDonald SD. Evaluation of long-term outcomes associated with preterm exposure to antenatal corticosteroids: a systematic review and meta-analysis. JAMA Pediatr. 2022;176:e220483. https://doi.org/10.1001/jamapediatrics.2022.0483.
Ninan K, Gojic A, Wang Y, Asztalos EV, Beltempo M, Murphy KE. et al. The proportions of term or late preterm births after exposure to early antenatal corticosteroids, and outcomes: systematic review and meta-analysis of 1.6 million infants. BMJ. 2023;382:e076035. https://doi.org/10.1136/bmj-2023-076035.
Rakers F, Schleußner E, Muth I, Hoyer D, Rupprecht S, Schiecke K. et al. Association between antenatal glucocorticoid exposure and the activity of the stress system, cognition, and behavior in 8- to 9-year-old children: a prospective observational study. Acta Obstet Gynecol Scand. 2022;101:996–1006. https://doi.org/10.1111/aogs.14386.
Bruschettini M, van den Hove DLA, Gazzolo D, Bruschettini P, Blanco CE, Steinbusch HWM. A single course of antenatal betamethasone reduces neurotrophic factor S100B concentration in the hippocampus and serum in the neonatal rat. Brain Res Dev Brain Res. 2005;159:113–8. https://doi.org/10.1016/j.devbrainres.2005.07.003.
Patel PD, Katz M, Karssen AM, Lyons DM. Stress-induced changes in corticosteroid receptor expression in primate hippocampus and prefrontal cortex. Psychoneuroendocrinology. 2008;33:360–7. https://doi.org/10.1016/j.psyneuen.2007.12.003.
Khan A, Rodriguez A, Kaakinen M, Pouta A, Hartikainen AL, Jarvelin MR. Does in utero exposure to synthetic glucocorticoids influence birthweight, head circumference and birth length? A systematic review of current evidence in humans. Paediatr Perinat Epidemiol. 2011;251:20–36. https://doi.org/10.1111/j.1365-3016.2010.01147.x.
Rodríguez-Pinilla E, Prieto-Merino D, Dequino G, Mejías C, Fernández P, Martínez-Frías M-L, et al. [Antenatal exposure to corticosteroids for fetal lung maturation and its repercussion on weight, length and head circumference in the newborn infant]. Med Clin (Barc). 2006;127:361–7. https://doi.org/10.1157/13092436.
Norberg H, Stålnacke J, Diaz Heijtz R, Smedler A-C, Nyman M, Forssberg H, et al. Antenatal corticosteroids for preterm birth: dose-dependent reduction in birthweight, length and head circumference. Acta Paediatr Oslo Nor 1992. 2011;100:364–9. https://doi.org/10.1111/j.1651-2227.2010.02074.x.
Yadav DRD, Chaudhary U, Shrestha N. Risk factors associated with low birth weight. J Nepal Health Res Counc. 2011;9:159–64. https://doi.org/10.33314/jnhrc.v0i0.266.
Kramer MS, Séguin L, Lydon J, Goulet L. Socio-economic disparities in pregnancy outcome: why do the poor fare so poorly? Paediatr Perinat Epidemiol. 2000;14:194–210. https://doi.org/10.1046/j.1365-3016.2000.00266.x
Cobo T, Kacerovsky M, Jacobsson B. Risk factors for spontaneous preterm delivery. Int J Gynecol Obstet. 2020;150:17–23. https://doi.org/10.1002/ijgo.13184.
Buonocore F, McGlacken-Byrne SM, Del Valle I, Achermann JC. Current insights into adrenal insufficiency in the newborn and young infant. Front Pediatr. 2020;8:619041. https://doi.org/10.3389/fped.2020.619041.
Taylor HC, Ali MY. Transient ionized hypocalcemia and secondary hyperparathyroidism accompanying acute adrenal insufficiency. Endocr Pract. 1998;4:159–64.
Gyamfi-Bannerman C, Thom EA, Blackwell SC, Tita ATN, Reddy UM, Saade GR, et al. Antenatal corticosteroids for women at risk of late preterm delivery. N Engl J Med. 2016;374:1311–20. https://doi.org/10.1056/NEJMoa1516783.
di Pasquo E, Saccone G, Angeli L, Dall’Asta A, Borghi E, Fieni S, et al. Determinants of neonatal hypoglycemia after antenatal administration of corticosteroids (ACS) for lung maturation: Data from two referral centers and review of the literature. Early Hum Dev. 2020;143:104984. https://doi.org/10.1016/j.earlhumdev.2020.104984.
Ustun N, Hocaoğlu M, Turgut A, Arslanoğlu S, Ovalı F. Does antenatal corticosteroid therapy improve neonatal outcomes in late preterm birth? J Matern Fetal Neonatal Med. 2021:1–7. https://doi.org/10.1080/14767058.2021.2015576.
Tegethoff M, Pryce C, Meinlschmidt G. Effects of intrauterine exposure to synthetic glucocorticoids on fetal, newborn, and infant hypothalamic-pituitary-adrenal axis function in humans: a systematic review. Endocr Rev. 2009;30:753–89. https://doi.org/10.1210/er.2008-0014.
Braun T, Challis JR, Newnham JP, Sloboda DM. Early-life glucocorticoid exposure: the hypothalamic-pituitary-adrenal axis, placental function, and long-term disease risk. Endocr Rev. 2013;34:885–916. https://doi.org/10.1210/er.2013-1012.
Yao T-C, Chang S-M, Wu C-S, Tsai Y-F, Sheen K-H, Hong X, et al. Association between antenatal corticosteroids and risk of serious infection in children: nationwide cohort study. BMJ. 2023;382:e075835. https://doi.org/10.1136/bmj-2023-075835.
Schmitz T, Alberti C, Ursino M, Baud O, Aupiais C. Full versus half dose of antenatal betamethasone to prevent severe neonatal respiratory distress syndrome associated with preterm birth: study protocol for a randomised, multicenter, double blind, placebo-controlled, non-inferiority trial (BETADOSE). BMC Pregnancy Childbirth. 2019;19:67 https://doi.org/10.1186/s12884-019-2206-x.
Author information
Authors and Affiliations
Contributions
CB: designed and conceptualized study; analyzed the data; drafted the manuscript for intellectual content. J-MH: Designed and conceptualized study, revised the manuscript for intellectual content. EJ: designed and conceptualized study, performed the statistical analysis, analyzed the data and revised the manuscript. OM: Designed and conceptualized study, revised the manuscript for intellectual content. CB: designed and conceptualized study, performed the statistical analysis and revised the manuscript. ER: designed and conceptualized study; analyzed the data; drafted the manuscript for intellectual content and revised the manuscript
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Best, C., Hascoet, JM., Jeanbert, E. et al. Impact of corticosteroid exposure on preterm labor in neonates eventually born at term. J Perinatol 44, 195–202 (2024). https://doi.org/10.1038/s41372-023-01831-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01831-0
This article is cited by
-
Antenatale Steroide – nicht immer und nicht immer wieder
Die Gynäkologie (2024)