Abstract
Objective
Our study sought to determine whether metabolites from a retrospective collection of banked cord blood specimens could accurately estimate gestational age and to validate these findings in cord blood samples from Busia, Uganda.
Study Design
Forty-seven metabolites were measured by tandem mass spectrometry or enzymatic assays from 942 banked cord blood samples. Multiple linear regression was performed, and the best model was used to predict gestational age, in weeks, for 150 newborns from Busia, Uganda.
Results
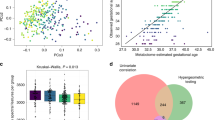
The model including metabolites and birthweight, predicted the gestational ages within 2 weeks for 76.7% of the Ugandan cohort. Importantly, this model estimated the prevalence of preterm birth <34 weeks closer to the actual prevalence (4.67% and 4.00%, respectively) than a model with only birthweight which overestimates the prevalence by 283%.
Conclusion
Models that include cord blood metabolites and birth weight appear to offer improvement in gestational age estimation over birth weight alone.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Data collected for the study including individual participant data and data dictionaries defining fields in the datasets have been made available to others through request to the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) Data and Specimen Hub (DASH): https://dash.nichd.nih.gov/Resource/Tutorial. Data available include de-identified individual level screening and enrollment data, individual participant data, repeated measures during pregnancy, QTc repeated measures, repeated doses for vomiting, and corresponding data dictionaries. Related study documents made available include the study protocol, statistical analysis plan, case report forms, and informed consent documents. Data can be accessed through the NICHD-DASH website (https://dash.nichd.nih.gov/Study/20027) following user registration and a research data request process. The NICHD DASH Data Access Committee reviews all requests to determine that a requester’s proposed use of the data is scientifically and ethically appropriate and does not conflict with constraints or informed consent limitations identified by the institutions that submitted the data. Metabolic data can be accessed through the Bill & Melinda Gates foundation following appropriate procedures and data access request process.
References
Lawn JE, Kinney M. Preterm birth: now the leading cause of child death worldwide. Sci Transl Med. 2014;6:263ed21.
Rijken MJ, De Livera AM, Lee SJ, Boel ME, Rungwilailaekhiri S, Wiladphaingern J, et al. Quantifying low birth weight, preterm birth and small-for-gestational-age effects of malaria in pregnancy: a population cohort study. PLoS One. 2014;9:e100247.
Fries N, Dhombres F, Massoud M, Stirnemann JJ, Bessis R, Haddad G, et al. The impact of optimal dating on the assessment of fetal growth. BMC Pregnancy Childbirth. 2021;21:167.
LaGrone LN, Sadasivam V, Kushner AL, Groen RS. A review of training opportunities for ultrasonography in low and middle income countries. Trop Med Int Health. 2012;17:808–19.
Anchang-Kimbi JK, Achidi EA, Apinjoh TO, Mugri RN, Chi HF, Tata RB, et al. Antenatal care visit attendance, intermittent preventive treatment during pregnancy (IPTp) and malaria parasitaemia at delivery. Malar J. 2014;13:162.
Gottlieb AG, Galan HL. Nontraditional sonographic pearls in estimating gestational age. Semin Perinatol. 2008;32:154–60.
Lindstrom L, Ageheim M, Axelsson O, Hussain-Alkhateeb L, Skalkidou A, Bergman E. Swedish intrauterine growth reference ranges of biometric measurements of fetal head, abdomen and femur. Sci Rep. 2020;10:22441.
Stevenson A, Joolay Y, Levetan C, Price C, Tooke L. A comparison of the accuracy of various methods of postnatal gestational age estimation; including ballard score, foot length, vascularity of the anterior lens, last menstrual period and also a clinician’s non-structured assessment. J Trop Pediatr. 2021;67:fmaa113.
Kieler H, Axelsson O, Nilsson S, Waldenstrom U. Comparison of ultrasonic measurement of biparietal diameter and last menstrual period as a predictor of day of delivery in women with regular 28 day-cycles. Acta Obstet Gynecol Scand. 1993;72:347–9.
Lynch CD, Zhang J. The research implications of the selection of a gestational age estimation method. Paediatr Perinat Epidemiol. 2007;21:86–96.
Tunon K, Eik-Nes SH, Grottum P. A comparison between ultrasound and a reliable last menstrual period as predictors of the day of delivery in 15,000 examinations. Ultrasound Obstet Gynecol. 1996;8:178–85.
Ballard JL, Khoury JC, Wedig K, Wang L, Eilers-Walsman BL, Lipp R. New Ballard Score, expanded to include extremely premature infants. J Pediatr. 1991;119:417–23.
Dubowitz LM, Dubowitz V, Goldberg C. Clinical assessment of gestational age in the newborn infant. J Pediatr. 1970;77:1–10.
Karl S, Li Wai Suen CS, Unger HW, Ome-Kaius M, Mola G, White L, et al. Preterm or not-an evaluation of estimates of gestational age in a cohort of women from Rural Papua New Guinea. PLoS One. 2015;10:e0124286.
Alexander GR, de Caunes F, Hulsey TC, Tompkins ME, Allen M. Validity of postnatal assessments of gestational age: a comparison of the method of Ballard et al. and early ultrasonography. Am J Obstet Gynecol. 1992;166:891–5.
Sanders M, Allen M, Alexander GR, Yankowitz J, Graeber J, Johnson TR, et al. Gestational age assessment in preterm neonates weighing less than 1500 grams. Pediatrics. 1991;88:542–6.
Jelliffe-Pawlowski LL, Norton ME, Baer RJ, Santos N.Rutherford GW. Gestational dating by metabolic profile at birth: a California cohort study. Am J Obstet Gynecol. 2016;214:511e1–511e13..
Ryckman KK, Berberich SL, Dagle JM. Predicting gestational age using neonatal metabolic markers. Am J Obstet Gynecol. 2016;214:515e1–515e13..
Wilson K, Hawken S, Potter BK, Chakraborty P, Walker M, Ducharme R.et al. Accurate prediction of gestational age using newborn screening analyte data. Am J Obstet Gynecol. 2016;214:513e1–513e9..
Chawanpaiboon S, Vogel JP, Moller AB, Lumbiganon P, Petzold M, Hogan D, et al. Global, regional, and national estimates of levels of preterm birth in 2014: a systematic review and modelling analysis. Lancet Glob Health. 2019;7:e37–e46.
Lee AC, Katz J, Blencowe H, Cousens S, Kozuki N, Vogel JP, et al. National and regional estimates of term and preterm babies born small for gestational age in 138 low-income and middle-income countries in 2010. Lancet Glob Health. 2013;1:e26–36.
Kong S, Day LT, Zaman SB, Peven K, Salim N, Sunny AK, et al. Birthweight: EN-BIRTH multi-country validation study. BMC Pregnancy Childbirth. 2021;21:240.
Murphy, MS, Hawken S, Cheng W, Wilson LA, Lamoureux M, Henderson M, et al. External validation of postnatal gestational age estimation using newborn metabolic profiles in Matlab, Bangladesh. Elife. 2019;8:e42627.
Oltman SP, Jasper EA, Kajubi R, Ochieng T, Kakuru A, Adrama H, et al. Gestational age dating using newborn metabolic screening: a validation study in Busia, Uganda. J Glob Health. 2021;11:04012.
Bennett MJ. Newborn screening for metabolic diseases: saving children’s lives and improving outcomes. Clin Biochem. 2014;47:693–4.
Clinical Laboratory Standards Institute. Blood collection on filter paper for newborn screening programs: approved standard. Wayne, PA: Clinical Laboratory Standards Institute; 2013.
Ryckman KK, Berberich SL, Shchelochkov OA, Cook DE, Murray JC. Clinical and environmental influences on metabolic biomarkers collected for newborn screening. Clin Biochem. 2013;46:133–8.
Acknowledgements
We thank the women who participated in the study, the dedicated study staff, practitioners at Masafu General Hospital, and members of the Infectious Diseases Research Collaboration (IDRC). We would also like to thank the staff at the State of Iowa Hygienic Laboratory for sample processing and analysis and Nancy Weathers and Bruce Bedell at the University of Iowa for data and sample management.
Funding
This research was support by grants from the Eunice Kennedy Shriver National Institute of Child Health and Human Development (P01 HD059454) and the Bill and Melinda Gates Foundation (OPP1134783, OPP1141549, OPP1127641). The content is solely the responsibility of the authors and does not necessarily represent the official views of the Eunice Kennedy Shriver National Institute of Child Health and Human Development or the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
KKR and EAJ designed the study analysis plan, performed analyses, drafted the initial manuscript, and reviewed and revised the manuscript. SPO, RK, TO, AK, HA, MO, and PO helped collect and analyze specimens and data and reviewed and revised the manuscript. EER, JMD, JCM, MK, TDC, GD, TR, PJ, and LLJ-P provided critical input on the intellectual content of the manuscript and reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The study was approved by the ethics committees of Makerere University School of Biomedical Sciences (Kampala, Uganda), the Uganda National Council for Science and Technology (Kampala, Uganda), the University of California San Francisco (San Francisco, CA, USA) and the University of Iowa (Iowa City, IA, USA). All study participants provided written informed consent.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jasper, E.A., Oltman, S.P., Rogers, E.E. et al. Targeted newborn metabolomics: prediction of gestational age from cord blood. J Perinatol 42, 181–186 (2022). https://doi.org/10.1038/s41372-021-01253-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01253-w