Abstract
Transendothelial migration of neutrophils in postcapillary venules is a key event in the inflammatory response against pathogens and tissue damage. The precise regulation of this process is incompletely understood. We report that perivascular macrophages are critical for neutrophil migration into skin infected with the pathogen Staphylococcus aureus. Using multiphoton intravital microscopy we showed that neutrophils extravasate from inflamed dermal venules in close proximity to perivascular macrophages, which are a major source of neutrophil chemoattractants. The virulence factor α-hemolysin produced by S. aureus lyses perivascular macrophages, which leads to decreased neutrophil transmigration. Our data illustrate a previously unrecognized role for perivascular macrophages in neutrophil recruitment to inflamed skin and indicate that S. aureus uses hemolysin-dependent killing of these cells as an immune evasion strategy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Kolaczkowska, E. & Kubes, P. Neutrophil recruitment and function in health and inflammation. Nat. Rev. Immunol. 13, 159–175 (2013).
Rigby, K.M. & DeLeo, F.R. Neutrophils in innate host defense against Staphylococcus aureus infections. Semin. Immunopathol. 34, 237–259 (2012).
Nourshargh, S., Hordijk, P.L. & Sixt, M. Breaching multiple barriers: leukocyte motility through venular walls and the interstitium. Nat. Rev. Mol. Cell Biol. 11, 366–378 (2010).
Kansas, G. Selectins and their ligands: current concepts and controversies. Blood 88, 3259–3287 (1996).
Laudanna, C., Kim, J.Y., Constantin, G. & Butcher, E. Rapid leukocyte integrin activation by chemokines. Immunol. Rev. 186, 37–46 (2002).
Massena, S. et al. A chemotactic gradient sequestered on endothelial heparan sulfate induces directional intraluminal crawling of neutrophils. Blood 116, 1924–1931 (2010).
Phillipson, M. et al. Intraluminal crawling of neutrophils to emigration sites: a molecularly distinct process from adhesion in the recruitment cascade. J. Exp. Med. 203, 2569–2575 (2006).
Proebstl, D. et al. Pericytes support neutrophil subendothelial cell crawling and breaching of venular walls in vivo. J. Exp. Med. 209, 1219–1234 (2012).
Bruns, R.R. & Palade, G.E. Studies on blood capillaries. I. General organization of blood capillaries in muscle. J. Cell Biol. 37, 244–276 (1968).
Hickey, W.F. & Kimura, H. Perivascular microglial cells of the CNS are bone marrow-derived and present antigen in vivo. Science 239, 290–292 (1988).
Kim, W.-K. et al. CD163 identifies perivascular macrophages in normal and viral encephalitic brains and potential precursors to perivascular macrophages in blood. Am. J. Pathol. 168, 822–834 (2006).
Chen, G.Y. & Nunez, G. Sterile inflammation: sensing and reacting to damage. Nat. Rev. Immunol. 10, 826–837 (2010).
David, M.Z. & Daum, R.S. Community-associated methicillin-resistant Staphylococcus aureus: epidemiology and clinical consequences of an emerging epidemic. Clin. Microbiol. Rev. 23, 616–687 (2010).
Noskin, G.A. et al. National trends in Staphylococcus aureus infection rates: impact on economic burden and mortality over a 6-year period (1998–2003). Clin. Infect. Dis. 45, 1132–1140 (2007).
Boucher, H.W. & Corey, G.R. Epidemiology of methicillin-resistant Staphylococcus aureus. Clin. Infect. Dis. 46 (suppl. 5), S344–S349 (2008).
Otto, M. Basis of virulence in community-associated methicillin-resistant Staphylococcus aureus. Annu. Rev. Microbiol. 64, 143–162 (2010).
Bubeck Wardenburg, J. & Schneewind, O. Vaccine protection against Staphylococcus aureus pneumonia. J. Exp. Med. 205, 287–294 (2008).
Kennedy, A.D. et al. Targeting of alpha-hemolysin by active or passive immunization decreases severity of USA300 skin infection in a mouse model. J. Infect. Dis. 202, 1050–1058 (2010).
Inoshima, I. et al. A Staphylococcus aureus pore-forming toxin subverts the activity of ADAM10 to cause lethal infection in mice. Nat. Med. 17, 1310–1314 (2011).
Inoshima, N., Wang, Y. & Bubeck Wardenburg, J. Genetic requirement for ADAM10 in severe Staphylococcus aureus skin infection. J. Invest. Dermatol. 132, 1513–1516 (2012).
Wilke, G.A. & Wardenburg, J.B. Role of a disintegrin and metalloprotease 10 in Staphylococcus aureus α-hemolysin–mediated cellular injury. Proc. Natl. Acad. Sci. USA 107, 13473–13478 (2010).
Li, J.L. et al. Intravital multiphoton imaging of immune responses in the mouse ear skin. Nat. Protoc. 7, 221–234 (2012).
Faust, N., Varas, F., Kelly, L.M., Heck, S. & Graf, T. Insertion of enhanced green fluorescent protein into the lysozyme gene creates mice with green fluorescent granulocytes and macrophages. Blood 96, 719–726 (2000).
Constantin, G. et al. Chemokines trigger immediate beta2 integrin affinity and mobility changes: differential regulation and roles in lymphocyte arrest under flow. Immunity 13, 759–769 (2000).
Peters, N.C. et al. In vivo imaging reveals an essential role for neutrophils in leishmaniasis transmitted by sand flies. Science 321, 970–974 (2008).
Mempel, T.R. et al. Regulatory T cells reversibly suppress cytotoxic T cell function independent of effector differentiation. Immunity 25, 129–141 (2006).
Pollard, J.W. Trophic macrophages in development and disease. Nat. Rev. Immunol. 9, 259–270 (2009).
Sasmono, R.T. et al. A macrophage colony-stimulating factor receptor-green fluorescent protein transgene is expressed throughout the mononuclear phagocyte system of the mouse. Blood 101, 1155–1163 (2003).
Nishibu, A., Ward, B.R., Boes, M. & Takashima, A. Roles for IL-1 and TNFalpha in dynamic behavioral responses of Langerhans cells to topical hapten application. J. Dermatol. Sci. 45, 23–30 (2007).
Muzumdar, M.D., Tasic, B., Miyamichi, K., Li, L. & Luo, L. A global double-fluorescent Cre reporter mouse. Genesis 45, 593–605 (2007).
Ludwig, A. et al. Metalloproteinase inhibitors for the disintegrin-like metalloproteinases ADAM10 and ADAM17 that differentially block constitutive and phorbol ester-inducible shedding of cell surface molecules. Comb. Chem. High Throughput Screen. 8, 161–171 (2005).
Lindquist, R.L. et al. Visualizing dendritic cell networks in vivo. Nat. Immunol. 5, 1243–1250 (2004).
Sumaria, N. et al. Cutaneous immunosurveillance by self-renewing dermal gamma delta T cells. J. Exp. Med. 208, 505–518 (2011).
Roediger, B. et al. Cutaneous immunosurveillance and regulation of inflammation by group 2 innate lymphoid cells. Nat. Immunol. 14, 564–573 (2013).
Stark, K. et al. Capillary and arteriolar pericytes attract innate leukocytes exiting through venules and 'instruct' them with pattern-recognition and motility programs. Nat. Immunol. 14, 41–51 (2013).
Sumagin, R. & Sarelius, I.H. Intercellular adhesion molecule-1 enrichment near tricellular endothelial junctions is preferentially associated with leukocyte transmigration and signals for reorganization of these junctions to accommodate leukocyte passage. J. Immunol. 184, 5242–5252 (2010).
Wang, S. et al. Venular basement membranes contain specific matrix protein low expression regions that act as exit points for emigrating neutrophils. J. Exp. Med. 203, 1519–1532 (2006).
Zaba, L.C., Fuentes-Duculan, J., Steinman, R.M., Krueger, J.G. & Lowes, M.A. Normal human dermis contains distinct populations of CD11c+BDCA-1+ dendritic cells and CD163+FXIIIA+ macrophages. J. Clin. Invest. 117, 2517–2525 (2007).
Ginhoux, F. et al. Fate mapping analysis reveals that adult microglia derive from primitive macrophages. Science 330, 841–845 (2010).
May, A.K., Gleason, T.G., Sawyer, R.G. & Pruett, T.L. Contribution of Escherichia coli alpha-hemolysin to bacterial virulence and to intraperitoneal alterations in peritonitis. Infect. Immun. 68, 176–183 (2000).
Foster, T.J. Immune evasion by staphylococci. Nat. Rev. Microbiol. 3, 948–958 (2005).
Bhakdi, S. & Tranum-Jensen, J. Alpha-toxin of Staphylococcus aureus. Microbiol. Rev. 55, 733–751 (1991).
O'Reilly, M., de Azavedo, J.C.S., Kennedy, S. & Foster, T.J. Inactivation of the alpha-haemolysin gene of Staphylococcus aureus 8325–4 by site-directed mutagenesis and studies on the expression of its haemolysins. Microb. Pathog. 1, 125–138 (1986).
Paprotka, K., Giese, B. & Fraunholz, M.J. Codon-improved fluorescent proteins in investigation of Staphylococcus aureus host pathogen interactions. J. Microbiol. Methods 83, 82–86 (2010).
Ni, L. et al. The Staphylococcus aureus pSK41 plasmid-encoded ArtA protein is a master regulator of plasmid transmission genes and contains a RHH motif used in alternate DNA-binding modes. Nucleic Acids Res. 37, 6970–6983 (2009).
Schenk, S. & Laddaga, R.A. Improved method for electroporation of Staphylococcus aureus. FEMS Microbiol. Lett. 73, 133–138 (1992).
Mitchell, A.J. et al. Technical advance: autofluorescence as a tool for myeloid cell analysis. J. Leukoc. Biol. 88, 597–603 (2010).
Ng, L.G. et al. Visualizing the neutrophil response to sterile tissue injury in mouse dermis reveals a three-phase cascade of events. J. Invest. Dermatol. 131, 2058–2068 (2011).
Lo Sardo, V. et al. An evolutionary recent neuroepithelial cell adhesion function of huntingtin implicates ADAM10-Ncadherin. Nat. Neurosci. 15, 713–721 (2012).
Acknowledgements
We thank M. Willcox (University of New South Wales, Sydney) for S. aureus strains, E. Harry (University of Technology Sydney) for S. aureus USA300, T. Graf (Center for Genomic Regulation, Barcelona, Spain) for providing Lyz2gfp/+ mice, D. Hume (University of Edinburgh) for Csf1r-EGFP mice, M.J. Fraunholz (University of Würzburg Biocenter) for the pmRFPmars plasmid, A. Smith, S. Allen and S. Dervish for their technical assistance, and M. Rizk and J. Qin for animal husbandry. This work was supported by grant 1030147 from the National Health and Medical Research Council of Australia (to A.A., R.J., N.F. and W.W.).
Author information
Authors and Affiliations
Contributions
A.A. and W.W. conceived the idea for this project. A.A., R.J., A.J.M. and W.W. wrote the paper. A.A., A.J.M. and B.R. performed immunological and flow cytometry experiments and assisted with imaging experiments. R.J. designed and conducted intravital and confocal imaging experiments. B.R. conducted flow cytometry and imaging experiments. R.J. and A.J.M. performed sorting experiments for perivascular macrophages. A.J.M. performed quantitative PCR experiments and cytometric bead arrays. R.J., A.J.M., B.R. and S.T. performed all other experiments. A.J.B. and N.F. generated fluorescent protein–expressing bacteria. All authors discussed the results and commented on the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Effect of Hla on bacterial infection parameters.
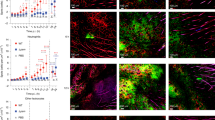
(a) Clinical manifestations, (b) Ear thickness, (c) RBC count following infection of C57BL/6 mice with S. aureus (WT or ΔHla) at various time points. (d) Ear swelling response and (e) RBC count of concomitant injection of purified Hla together with S. aureus (ΔHla) 12h p.i. (f) Neutrophil myeloperoxidase activity in back skin of mice infected with S. aureus (WT or ΔHla) at 12h p.i. MPO activity was normalized to tissue weight. (g) Neutrophil influx into ears infected with S. aureus strain USA300 in the presence or absence of anti-Hla serum. Bars represent mean±SD. Student's two-tailed unpaired t-test was used to determine the P-value. Data are representative of at least two independent experiments. Error bars indicate SD. **P<0.01; ***P<0.001.
Supplementary Figure 2 Hla suppresses the homing of adoptively transferred Lyz2gfp/+ neutrophils to the site of infection.
(a) Confocal imaging of extravasated Lyz2gfp/+ neutrophils in dermis of mice infected with S. aureus (WT or ΔHla) 6h p.i. and 1h following Lyz2gfp/+ bone marrow cell transfer. Blood vessels are visualized by CD31 staining. Scale bar represents 100μm. (b) Flow cytometric analysis of S. aureus (ΔHla) infected tissue 6h p.i. and 1h following Lyz2gfp/+ bone marrow cell transfer showing percentage of extravasated neutrophils (Ly6G+Ly6Cint) and monocytes (Ly6G-Ly6Chi). (c) CCL2, CCL3 and CCL4 protein levels in ears of mice infected with S. aureus (WT or ΔHla). Bars represent mean±SD of five to six mice/group/time point. One-way ANOVA with Tukey's post-test was used to determine the P-value. ***P<0.001.
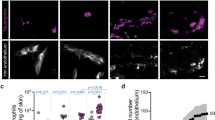
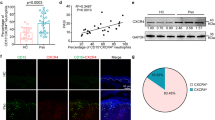
Supplementary Figure 3 Phenotypic analysis of PVM.
(a) Flow cytometric analysis of GFP+ and GFP- macrophages from skin of DPE-GFP mice in comparison to red pulp and peritoneal macrophages. (b) Confocal imaging of cremaster muscle showing the localization of PVM (DPE-GFP, green) in relation to pericytes (anti-smooth muscle actin, red) and endothelial cells (CD31, blue). (c) Expression of Csf1r mRNA transcripts in GFP+ macrophages from DPE-GFP mice. Bars represent mean±SD of 3 independent experiments. (d) Comparative mRNA expression of indicated genes in GFP+ vs. GFP- dermal macrophages from DPE-GFP mice. Bars represent mean±SD of 3 independent experiments. (e) Intravital imaging of ears from Csf1r-EGFP mice showing presence of GFP+ PVM (asterisk). Student's two-tailed unpaired t-test was used to determine the P-value. *P<0.05
Supplementary Figure 4 Neutrophils extravasate adjacent to perivascular macrophages during E. coli infection.
(a) Figure depicts the methodology employed to calculate predicted neutrophil to macrophage correlation (detailed in Materials and Methods section). The total observed extravasation tracks for the blood vessel imaged are overlayed in comparison to the predicted tracks. The insets depict one such event of neutrophil extravasation (red) from blood vessel (blue, vessel wall marked in cyan) in relation to PVM (green, asterisk in main figure). 00:00, min:sec. (b) Time-lapse intravital multi-photon imaging of ear dermis of DPE-GFP mice infected with E. coli depicting the adherence and extravasation of adoptively transferred cells isolated from mT/mG mice (red, numbered 1-4) in close proximity to PVM (DPE-GFP, green). Lines (white) represent migration tracks of selected neutrophils (red) 00:00:00, hr:min:sec. (c) Statistical analysis of neutrophil extravasation site with respect to perivascular macrophages. Numbers of neutrophils extravasating at theoretical/random (white bars) or observed (black bars) distances from GFP+ PVM within the same vessels. Data is cumulative of 50 events of extravasation from 3 independent experiments. (d) Neutrophil influx, (e) ear thickness and (f) RBC counts of ears concomitantly injected with E. coli and Hla (10μg) or only E. coli alone for 12h p.i. Data shown are mean±SEM of 3 independent experiments. P-values were calculated using two-way ANOVA or two-tailed unpaired Student's t-test, **P<0.01; ***P<0.001; ****P<0.0001; NS, not significant.
Supplementary Figure 5 Vascular integrity is unaffected by S. aureus infection.
(a) Confocal imaging of ear whole mounts from untreated DPE-GFP mice (left panels) or animals infected with S. aureus (WT) (right panels). Basement membranes are delineated by laminin and endothelium by CD31 labeling. (b) Intravital imaging of Evans blue (red; conjugated to BSA) leakage from S. aureus (ΔHla or WT) infected tissue 6h p.i. Adoptively transferred neutrophils (green) and SHG (blue) are also depicted. The images are tiles of 1mmx1mm region of ear tissue. (c) Confocal imaging of Thy-1 stained ear whole mounts from untreated DPE-GFP mice (left panels) or animals infected with S. aureus (WT) (right panels) showing no appreciable loss of Thy-1+ cells.
Supplementary Figure 6 Comparable uptake of wild-type and ΔHla S. aureus by neutrophils.
(a) Percent Ly6G+ neutrophils containing RFP-expressing S. aureus strains (WT or ΔHla) were determined by flow cytometry at 12h p.i. (b) Representative dotplots illustrating fluorescence intensity of neutrophils containing RFP-expressing S. aureus (WT or ΔHla). (c) Fluorescence intensity of RFP expressing S. aureus strains as determined by flow cytometry. Data are representative of two independent experiments (four to five mice/group). Error bars indicate SD.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–6 (PDF 13883 kb)
Supplementary Movie 1.
Time-lapse intravital imaging of mice infected with either WT or ΔHla S. aureus depicting neutrophil rolling and sticking in dermal blood vessels (red). The mice were infected 6 h before imaging and neutrophils (green) were adoptively transferred immediately before imaging. Time represents min:s. Increased red background in S. aureus (ΔHla) infection is observed due inflammation induced vascular leakage of Evans blue. (AVI 7381 kb)
Supplementary Movie 2.
Time-lapse intravital imaging of ear dermis of mice infected with S. aureus (ΔHla) depicting hotspots for neutrophil sticking and extravasation from the blood vessel (red). The mice were infected 6 h before imaging, and neutrophils (green) were adoptively transferred immediately prior to imaging. Time represents min:s. (AVI 4718 kb)
Supplementary Movie 3.
Z stack of ear dermis of DPE-GFP mice showing the localisation of GFP+ macrophages (green) along dermal blood vessel (red). Second harmonic generation is depicted in blue. (AVI 454 kb)
Supplementary Movie 4.
Three-dimensional time-lapse reconstruction of Z stacks of ear dermis of DPE-GFP mice showing the homeostatic scanning behaviour of GFP+ macrophages. Time represents h:min:s. (MOV 455 kb)
Supplementary Movie 5.
Time-lapse intravital imaging of ear dermis of mice infected with S. aureus (ΔHla) depicting neutrophil (red) extravasation in relation to GFP+ perivascular macrophages (green). The mice were infected 6 h before imaging, and neutrophils were adoptively transferred immediately before imaging. Time represents h:min:s. (MOV 4240 kb)
Supplementary Movie 6.
In vitro time-lapse imaging of macrophage (green) death in the presence of Hla (7.5μg/ml). Time represents min:s after addition of Hla. (AVI 632 kb)
Supplementary Movie 7.
Three-dimensional time lapse reconstruction of Z stacks of ear dermis of DPE-GFP mice infected with S. aureus (WT) (red) showing the behaviour of GFP+ macrophages in presence of S. aureus (WT). Imaging was performed immediately after injection of the bacterium. Time represents h:min:s. (MOV 1022 kb)
Supplementary Movie 8.
Three-dimensional time lapse reconstruction of Z stacks of ear dermis of DPE-GFP mice infected with S. aureus (ΔHla) (red) showing the behavior of GFP+ macrophages in presence of ΔHla S. aureus (ΔHla). Imaging was performed immediately after injection of the bacterium. Time represents h:min:s. (MOV 2097 kb)
Supplementary Movie 9.
Time-lapse intravital imaging of ear dermis of mice injected with RFP-expressing S. aureus (WT) (red) in relation to perivascular macrophages (green). The mice were injected just before imaging. Time represents h:min:s. (MOV 3846 kb)
Supplementary Movie 10.
Time-lapse intravital imaging of ear dermis of mice injected with fluorescent beads (red) in relation to perivascular macrophages (green). The mice were injected just before imaging. Time represents h:min:s. (MOV 4825 kb)
Supplementary Movie 11.
Time-lapse intravital imaging of ear dermis of mice injected with RFP-expressing S. aureus (ΔHla) (red) in relation to perivascular macrophages (green). The mice were injected just before imaging. Time represents h:min:sec. (MOV 7552 kb)
Supplementary Movie 12.
Time-lapse intravital imaging of ear dermis of dermal dendritic cells (yellow) in CD11c-YFP mice injected with RFP-expressing S. aureus (WT) (red). The mice were injected just before imaging. Time represents h:min: (MOV 3597 kb)
Supplementary Movie 13.
Time-lapse intravital imaging of ear dermis of γδ T cells (green) in CXCR6-GFP mice injected with RFP-expressing S. aureus (WT) (red). The mice were injected just before imaging. Time represents h:min:s. (MOV 4477 kb)
Rights and permissions
About this article
Cite this article
Abtin, A., Jain, R., Mitchell, A. et al. Perivascular macrophages mediate neutrophil recruitment during bacterial skin infection. Nat Immunol 15, 45–53 (2014). https://doi.org/10.1038/ni.2769
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.2769
This article is cited by
-
Neutrophil breaching of the blood vessel pericyte layer during diapedesis requires mast cell-derived IL-17A
Nature Communications (2022)
-
Specialized transendothelial dendritic cells mediate thymic T-cell selection against blood-borne macromolecules
Nature Communications (2021)
-
Immunogenicity Challenges Associated with Subcutaneous Delivery of Therapeutic Proteins
BioDrugs (2021)
-
Visualization of autoantibodies and neutrophils in vivo identifies novel checkpoints in autoantibody-induced tissue injury
Scientific Reports (2020)
-
Neglected interstitial space in malaria recurrence and treatment
Nano Research (2020)