Abstract
Background:
Evidence increasingly supports that prostate cancer is initiated by the malignant transformation of stem cells (SCs). Furthermore, many SC-signalling pathways are shown to be shared in prostate cancer. Therefore, we planned transcriptome characterisation of adult prostate SCs as a strategy to consider new targets for cancer treatment.
Methods:
Intuitive pathway analysis was used for putative target discovery in 12 matched selections of human prostate SCs, transiently amplifying cells and terminally differentiated cells. These were pooled into three groups according to the stage of differentiation for mRNA microarray analysis. Targets identified were validated using uncultured primary tissue (n=12), functional models of prostate cancer and a tissue microarray consisting of benign (n=42) and malignant prostate (n=223).
Results:
A deficiency in class 1 UDP glucuronosyltransferase (UGT) enzymes (UGT1A) was identified in prostate SCs, which are involved in androgen catabolism. Class 1 UGT enzyme expression was also downregulated in cancer SCs and during progression to metastatic castration-resistant prostate cancer (CRPC). Reduction of UGT1A expression in vitro was seen to improve cell survival and increase androgen receptor (AR) activity, as shown by upregulation of prostate-specific antigen expression.
Interpretation:
Inactivation of intracellular androgen catabolism represents a novel mechanism to maintain AR activity during CRPC.
Similar content being viewed by others
Main
Mechanistic studies of tumorigenesis point towards stem cells (SCs) being the cell of origin in prostate cancer initiation, suggesting stem pathways have a crucial role in the early stages of cancer development (Gu et al, 2007; Goldstein et al, 2010; Lawson et al, 2010). Furthermore, known stem pathways have been seen to be aberrantly expressed as the prostate cancer progresses (Linn et al, 2010; Jia et al, 2011; Kregel et al, 2013). Characterisation of the genes at play within prostate SCs, and characterising these same markers in the malignant setting may identify unique therapeutic opportunities for the treatment of prostate cancer.
We have recently demonstrated the presence of the androgen receptor (AR) within normal human prostate SCs (Williamson et al, 2012), so identification of specific novel AR pathway processes within these cells will be of particular importance. Such mechanisms may explain the maintenance of androgen ‘addiction’ in the malignant setting during cancer progression despite androgen deprivation, as it is established that the AR pathway has diverse roles depending on the degree of prostate differentiation (Gregory et al, 1998; Buchanan et al, 2001; Mousses et al, 2001; Chen et al, 2004; Taplin and Balk, 2004; Attard et al, 2009; Bonkhoff and Berges, 2010; Lee et al, 2012).
Human prostate SCs can be enriched by their expressions of α2β1-integrins and CD133 (Richardson et al, 2004). In this work, we describe gene expression signatures associated with SCs (α2β1HI CD133+VE), transiently amplifying (TAP) cells (α2β1HI CD133−VE) and terminally differentiated (TD) cells (α2β1LOW CD133−VE) following the intuitive pathway analysis of transcriptome characterisation of human prostates. Within normal prostate SCs, we discovered a deficiency in class 1 UDP (uridine 5′-diphospho)-glucuronosyltransferase; UGT) enzymes (UGTA1), which are regulators of androgen catabolism. Our functional in vitro models of prostate cancer demonstrated that UGT1A knock down leads to upregulation of prostate-specific antigen (PSA) along with increased cell survival. Furthermore, reduced UGT1A expression was shown to be a feature of clinical prostate cancer that was associated with a poorer prognosis.
Materials and methods
Tissue collection and gene expression array analysis
Human prostate samples were collected from a total of 50 patients and processed, as previously described (Williamson et al, 2012), to yield α2β1HI CD133+VE cells (stem progenitors), α2β1HICD133−VE (transiently amplifying progenitors) and α2β1LOW CD133−VE (differentiated) epithelial cells without culturing (Richardson et al, 2004; Heer et al, 2006; Williamson et al, 2012). These immediately underwent RNA isolation (micro RNeasy, Qiagen, Manchester, UK), with only the highest quality samples being taken forward for analysis. To ensure the highest quality of data, before being taken forward for study, samples must have demonstrated an RNA integrity number >8.0 in each selected fraction. This approach yielded 12 high-quality matched patient samples to be taken forward for further analysis (Supplementary Table 1). These were pooled using a validated methodology to account for biological variance (Kendziorski et al, 2005; Zhang et al, 2007) creating three pooled samples of α2β1HI CD133+VE, α2β1HI CD133−VE and α2β1LOW CD133−VE. These samples were then investigated on Affymetrix (High Wycombe, UK) U133 plus 2.0 chips. Detailed methods and analyses used are outlined in depth in the Supplementary Information.
Quantitative real-time PCR analysis
MessageBOOSTER cDNA synthesis amplification kit (Epicentre Biotechnologies, Madison, WI, USA) was employed for prospective validation of gene signatures identified in the microarray on the unpooled individual sorted samples. Real-time PCR (Applied Biosystems (Life Technologies, Paisley, UK) 7900HT) was performed on subsequent cDNA libraries using SYBR Green (Invitrogen, Life Technologies, Paisley, UK) and cDNA-specific primers sets detailed in Supplementary Table 2. All data were normalised to the housekeeping gene GAPDH.
Maintenance of prostate cancer cell lines
Human prostate benign cell line BPH-1 in addition to human prostate cancer cell lines LNCaP and VCaP (American Type Culture Collection (ATCC), Manassas, VA, USA) were maintained in RPMI 1640 medium (Sigma, Gillingham, UK) containing 10% fetal calf serum (Sigma) and 2 mM L-glutamine (Sigma), referred to as complete medium. The isogenic androgen-independent cell line LNCaP-AI, used to mimic castration resistant prostate cancer (CRPC; Halkidou et al, 2003), was maintained in steroid-depleted media; RPMI 1640 medium (Sigma) containing 10% heat-inactivated dextran charcoal-treated fetal calf serum (Hyclone, Fisher Scientific, Loughborough, UK) and 2 mM L-glutamine (Sigma).
Small-interfering RNA knock down
Cells were seeded in six-well plates before being transfected with either non-silencing small-interfering RNA (siRNA) or equivalent concentration UGT1A siRNA (sequences are listed in Supplementary Information) using Lipofectamine RNAiMAX (Invitrogen). Additional methods, including western blot, are available in Supplementary Information.
Clonogenicity assays
Colony-forming assays were performed by plating 2000 viable cells in individual wells of a six-well dish for 14 days, fixing in Carnoy’s fixative (Sigma) and counterstaining with 1% Crystal Violet (Sigma). Colony counting was performed by ColCount automated colony counter (Oxford Optronix, Milton, UK).
Tissue microarray staining and scoring
Class 1 UGT enzyme staining was carried out on a tissue microarray consisting of benign (n=42) and malignant prostate (n=223) material derived from radical prostatectomy or trans-urethral resection of the prostate (Heer et al, 2004). Sections were deparaffinised and rehydrated before undergoing antigen retrieval under pressure in 0.01 M sodium citrate buffer and were treated for endogenous peroxidase activity. Sections were stained with 1 : 100 UGT1A antibody (Sc-25847, Santa Cruz Biotechnology, Heidelberg, Germany) and the Menapath two-step HRP universal polymer kit (A. Menarini Diagnostics Ltd., Winnersh-Wokingham, UK), according to the manufacturer’s recommendations. Immunostaining was classified as absent (0), weak (1), moderate (2) or strong (3) by a consultant uropathologist (Mantilla). Staining was correlated to clinical parameters using Kruskal–Wallis test, Mann–Whitney U-test, Log-rank analysis and Cox regression analysis. Where appropriate, P<0.05 was considered statistically significant.
Results
Post-hybridisation quality assurance of microarray data series
Quality assessment of samples confirmed 3′-end/-middle (3′/M) ratios for housekeeping genes below the required threshold of 3, which confirms linear amplification of samples before running of samples and was in keeping with the high-quality threshold set for the samples utilised (Supplementary Figure S3). Investigation of the top genes up- and downregulated between the epithelial fractions confirmed CD133 as the top ranked differentially expressed transcript in the comparison with the α2β1HI CD133+VE and α2β1HI CD133−VE fractions (17.88-fold increase in the α2β1HI CD133+VE fraction). Distinct gene signatures were observed for each of the transcript profiles for prostate SCs, TAPs and TD cells, and prospective validation of these transcript patterns during differentiation was confirmed using CD133 and p63 real-time PCR (Supplementary Figure S3), with patterns of expression for key markers of prostate differentiation (AR, KLK2, KLK3 and TMPRSS2) matching those shown previously (Williamson et al, 2012).
Differential androgen metabolism and signalling is observed in SCs, CSCs and throughout disease progression
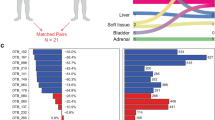
Pathway ontology analysis was undertaken to characterise groups of genes altered during prostate differentiation based on their interacting biological function. Pathway analyses comparing the α2β1HI CD133+VE fraction of SCs with the α2β1HI CD133−VE fraction of early differentiation-committed cells (TAPs) highlighted ‘testosterone biosynthesis, metabolism’ as one of the top ranked differentially expressed pathways (P<0.001; Figure 1). Detailed interrogation of the androgen pathways revealed no change in gene expression within the anabolic component of testosterone biosynthesis during normal prostate differentiation (Supplementary Figure S4). However, the catabolic pathways showed a significant difference but only in the UGT1A-enzyme family. Class 1 UGT enzyme expression showed 4- to 10-fold downregulation in normal SCs compared with more differentiated cells, depending upon the different probe sets for this family in the array (Figure 1B and Supplementary Figure S5). UDP glucuronosyltransferase enzymes remove hydrophobic molecules, such as testosterone, from cells by glucuronidation. Previous studies on testosterone glucuronidation have concentrated on the class 2 enzymes in the prostate and in prostate cancer, specifically UGT2B7, UGT2B15 and UGT2B17 (Belanger et al, 2003; Chouinard et al, 2007); however, these were seen to be unaltered between the three epithelial fractions of this study (Supplementary Figure S5). Of note, the specific probe set for UGT1A8 was the third most downregulated probe set (10-fold, P<0.001) in the comparison between the α2β1HI CD133+VE and the α2β1HI CD133−VE fraction. Assessment of individual UGT1A enzymes using isoform-specific real-time PCR primer sets in unpooled individual human prostate samples confirmed UGT1A8 as the highest expressed enzyme in the α2β1LOW CD133−VE TD fraction, and that none of the UGTA1 enzymes were detectable in the α2β1HI CD133+VE SC fraction (Figure 2A). Meta-analyses of UGTA1 enzyme expression in studies of prostate SCs and cancer SCs (CSCs; Birnie et al, 2008) corroborated these findings, showing decreased expression in both SCs and CSCs compared with differentiated cells (P<0.01, gene set enrichment analysis (GSEA); Figure 2B). Moreover, assessment of UGTA1 enzymes in clinical transcriptome data from cases of prostate cancer progression (Varambally et al, 2005) confirmed further reduced expression in CRPC compared with early prostate cancer (P<0.01, GSEA; Figure 2C). Reduced UGT1A expression in progenitor cells suggests a potential mechanism for the accumulation of androgens within prostate cancer cells during androgen deprivation therapy, and UGT1A expression remains depressed in CRPC.
Pathway analysis of prostate hierarchy. (A) (GeneGo Inc., St Joseph, MI, USA) analysis comparing genes two-fold different between the α2β1HI CD133+VE and α2β1HI CD133−VE fractions. Top 10 pathways are ranked according to their statistical significance (inverse log P-value). (B) Metacore-annotated pathway map (GeneGo Inc.) for testosterone biosynthesis and metabolism comparing the α2β1HI CD133+VE with the α2β1HI CD133−VE fraction. Blue thermometers indicate downregulation of genes in the α2β1HI CD133+VE fraction.
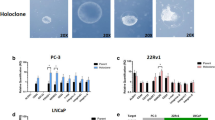
Expression of UGTA1 enzymes in the prostate differentiation and prostate cancer progression. Error bars represent s.e. of the mean. (A) Expression of individual UGTA1 enzymes following real-time PCR normalised to GAPDH (n=6). (B) The GSEA for UGT1A comparisons in stem cell (SC) and cancer SC (CSC) vs terminally differentiated (TD) normal and terminally differentiated cancer (CTD) cells, respectively. Barcode plots are graphical representations of the Wilcox gene-set test results using ranks. The ranks of the sorted log-fold changes between conditions run along the x axis from high (pink) to low (green). Black lines represent matches to the UGTA1 enzymes. P-values are given in the tables below for the alternative hypothesis that the UGTA1 enzymes tend to be (i) upregulated in the data set or (ii) downregulated. (C) The GSEA for comparisons of UGT1A expression in benign prostate (Ben.), primary prostate cancer (1°) and castrate-resistant metastatic cancer (Mets).
Reduction in UGT1A expression is seen in cell line models of CRPC and leads to increased AR activity
The functional effects of reduced UGTA1 enzymes expression were explored using functional models of prostate cancer. Class 1 UGT protein expression was confirmed in the benign prostatic cell line BPH-1 and the androgen-dependent cell line LNCaP; however, reduced levels of expression for UGT1A were seen in both the isogenic LNCaP-AI and castration-resistant derived line VCaP (Figure 3A). To explore whether reduced UGT1A expression was a functional feature of prostate cancer progression, LNCaP cells were transfected with siRNA targeting the UGTA1 enzymes in standard steroid-containing medium. Following UGT1A knock down, increased AR activity was evident by increased PSA expression despite no change in AR expression compared with scrambled siRNA control (Figure 3B). Furthermore, following UGT1A knock down LNCaP cells were seen to have a two-fold increase in clonogenicity compared with scrambled siRNA controls (P<0.05; Figure 3C). These data confirm that AR is more active in cells, which is probably because of the presence of relatively higher intracellular levels of steroids expected with lower levels of UGT1A.
Functional characterisation of altered UGT1A expression in prostate cancer. (A) Representative western blot analysis measuring expression of UGT1A. (B) Representative western blot analysis of UGT1A, AR and PSA following knock down with UGT1A siRNA. (C) A 2D colony-forming efficiency of LNCaP in complete medium following knock down with UGT1A siRNA (n=3; P<0.05).
Class 1 UGT enzyme expression is downregulated in clinical prostate cancer progression
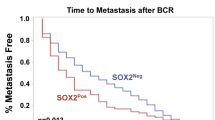
Decreasing levels of UGT1A immunostaining was associated with increasingly aggressive disease, as determined by D′Amico prostate cancer risk (based on Gleason grade, stage and presenting PSA; P=0.04, Kruskal–Wallis test; Figure 4A and B). Low levels of UGT1A expression were also associated with increased serum PSA levels upon clinical presentation (P=0.003, Mann–Whitney U–test; Figure 4C), consistent with reduced UGT1A expression increasing intracellular testosterone bioavailability and AR activity. Interestingly, despite patients with low UGT1A expression being associated with higher-risk disease, they initially responded much better to hormonal therapy than those with high UGT1A expression (P=0.03, Mann–Whitney U-test; Figure 4D), suggesting a more pronounced ligand-dependant AR activity in tumours with low UGT1A expression. However, this initial responsiveness to hormones is transient as reduced UGT1A expression correlated with a significant reduction in patient survival (P=0.025, Log-rank analysis; Figure 4E). In particular, this survival effect was pronounced in patients with metastatic disease (P=0.038, Log-rank analysis; Figure 4F). Interestingly, time to CRPC was not significantly different between high- and low-UGT groups, and it may be that different hormone-escape pathways are established in these two groups during progression to death from the advent of CRPC. Although Cox multivariate analysis showed that UGT1A expression did not confer additional prognostic indication of survival independent of grade and stage, we nevertheless show that reduced UGT1A expression correlates with an increased AR signalling, supporting its role as a mechanism of castration resistance.
Expression of UGT1A within a tissue microarray of prostate cancer ( n =265; benign n =42, malignant n =223). Error bars represent s.e. of the mean. (A) Representative images of UGT1A staining in prostate tissue. (B) Staining intensity for UGT1A for samples stratified for D′Amico risk. (C) Presenting PSA levels according to staining intensity for UGT1A. (D) Prostate-specific antigen nadir levels following hormonal therapy according to UGT1A expression (E) A Kaplan–Meier plot demonstrating survival according to UGT1A staining intensities of 0–1 (blue line) and 2–3 (green line). (F) Kaplan–Meier plots of prostate cancer survival in patients without metastases (left hand plot) or with metastases (right hand plot) with UGT1A staining intensity of 0–1 (blue line) or 2–3 (green line).
Discussion
There is growing evidence that it is the SCs in the ageing prostate that acquire the required mutations to become the cell of origin for malignant transformation and that prostate tumours are maintained by a hierarchal CSC model (Collins et al, 2005; Gu et al, 2007; Goldstein et al, 2010; Lawson et al, 2010; Williamson et al, 2012). However, the relevance of the signalling pathways maintaining these cells types during progression of the disease into lethal CRPC remains poorly understood. A transcriptome-based target discovery approach, looking at the pathways within the SC hierarchy and their role in the malignant setting would be of interest. This approach was explored in this paper and revealed novel target pathways.
There is an ongoing debate over the nature of the SC organisation of the prostate epithelium. Most models of prostate homoeostasis have advocated the presence of undifferentiated SCs within the basal compartment of the prostate (English et al, 1987; Isaacs and Coffey, 1989; Richardson et al, 2004). In particular, a single basally derived SC has been shown to regenerate a fully differentiated prostate epithelium (Leong et al, 2008). The location of the SC niche, however, has been questioned following the identification of luminally derived castration-resistant Nkx3.1 cells (CARNs) (Germann et al, 2012), which are also capable of reconstituting the prostate epithelium from a single cell. An alternative model comes from mouse lineage-tracing experiments that show basally derived multipotent SCs give rise to unipotent basal and luminal progenitors during postnatal development; however, in the adult gland, the epithelium is maintained by unipotent progenitors specific for basal and luminal layers (Choi et al, 2012; Ousset et al, 2012). Although mice models remain an important tool for the prostate modelling of tumorigenesis and differentiation, studies of human material remains the gold standard and continue to support a basal SC in the human prostate. Recent lineage tracking in human tissue demonstrated that all epithelial cells share a clonal origin (Blackwood et al, 2011) and most published work supports a human basal SC (Richardson et al, 2004; Goldstein et al, 2008).
One of the issues faced when investigating small numbers of samples (<12) with microarray technology is the potential for outlier patient-specific differences masking more critical underlying population differences between fractions (Kendziorski et al, 2005; Zhang et al, 2007). To minimise the potential for this in our study, we opted to investigate more the transcriptome of the prostate as a target discovery platform using a validated pooling strategy. This pooling strategy has been demonstrated to account for biological variance within populations when ⩾12 cases are included and has been validated in gene array studies (Kendziorski et al, 2005; Zhang et al, 2007). The limitation of any pooling strategy is the potential to mask expressions in subsets of the general population; however, the subsequent targets will be more generalisable to the broader population. To prevent spurious samples affecting this analysis, we carried out a stringent inclusion criteria based on RNA quality before inclusion in our study and only included the 12 samples that met our criteria, out of the 50 we screened. Furthermore, to ensure subsequent targets were representative, we carried out validation in unpooled selected samples and found the results were representative of individual samples and not a result of outliers within the pool. Finally, we were able to demonstrate the significance of these targets in external data cohorts by demonstrating that these same genes were important within previous transcriptome studies of SCs (n=7 benign and n=8 malignant) and clinical prostate cancer (n=4 benign, n=5 primary prostate cancer and n=4 metastatic cancers) (Varambally et al, 2005; Birnie et al, 2008).
With this target discovery approach, we demonstrate that specific SC pathways were still maintained in early and advanced prostate cancer. Specifically, the identification of a novel deficiency in testosterone catabolism within normal human SCs, in addition to CSCs and advanced prostate cancer, highlights mechanisms that support a persistent ‘addiction’ of prostate cancer cells to AR ligands in CRPC (Reid et al, 2010; Williamson et al, 2012). Although previous studies of testosterone glucuronidation have concentrated on the role of class II UGT enzymes on androgen responsiveness within prostate cancer, it is both class I and class II UGT enzymes that are required to fully di-glucuronidate testosterone for cellular export (Murai et al, 2006). In particular, UGT1A8 is the only UDP glucuronidation enzyme uniquely capable of di-glucuronidation, which is required to fully catabolise DHT (Murai et al, 2006) and has a specific activity against C19 steroids (androgens), that is, 2- to 20-fold greater than most class II UGT enzymes (Tukey and Strassburg, 2000).
We have previously demonstrated that normal SCs of the prostate express low levels of active AR, but that differentiated cells express higher levels of the receptor with higher AR activity. In the normal setting, despite a deficiency in UGT1A enzymes, it appears the receptor is tightly regulated in SCs (Williamson et al, 2012). It is in the cancer setting, where AR function is already overactive and being actively driven (Feldman and Feldman, 2001; Attard et al, 2009; Bonkhoff and Berges, 2010), that deficiency in UGT1A seems to contribute to pathogenesis, with low expression of the enzymes correlating with poor prognosis and downregulation in vitro seen to contribute to AR activation. Deficiency in UGT1A enzymes provides an additional mechanism to maintain AR signalling in CRPC, contributing to recognised phenomena of androgen hypersensitivity, AR amplification and local testosterone production (Feldman and Feldman, 2001). Attempts were made to determine whether these cells had increased testosterone levels using mass spectroscopy; however, because of in vitro culture conditions with large quantities of steroids that can passively cross the cell surface, the system was saturated while preparing specimens, and we were unable to determine intracellular levels with accurate sensitivity. Nevertheless, PSA expression remains an excellent proxy for AR pathway upregulation in our data.
Studies of UGTA1 enzymes have been limited to date, in part because of the similarities of each enzyme to each other. Future studies characterising mechanisms of UGTA1 enzyme gene silencing would be of therapeutic interest in prostate cancer. Our work supports models of CRPC where there is a persistent reliance of prostate cancer cells on AR signalling and AR ligands, reinforcing a mechanistic role for newer therapies that target testosterone and highlights a novel androgen catabolism pathway for target development.
Change history
20 August 2013
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Attard G, Cooper CS, de Bono JS (2009) Steroid hormone receptors in prostate cancer: a hard habit to break? Cancer Cell 16 (6): 458–462.
Belanger A, Pelletier G, Labrie F, Barbier O, Chouinard S (2003) Inactivation of androgens by UDP-glucuronosyltransferase enzymes in humans. Trends Endocrinol Metab 14 (10): 473–479.
Birnie R, Bryce SD, Roome C, Dussupt V, Droop A, Lang SH, Berry PA, Hyde CF, Lewis JL, Stower MJ, Maitland NJ, Collins AT (2008) Gene expression profiling of human prostate cancer stem cells reveals a pro-inflammatory phenotype and the importance of extracellular matrix interactions. Genome Biol 9 (5): R83.
Blackwood JK, Williamson SC, Greaves LC, Wilson L, Rigas AC, Sandher R, Pickard RS, Robson CN, Turnbull DM, Taylor RW, Heer R (2011) In situ lineage tracking of human prostatic epithelial stem cell fate reveals a common clonal origin for basal and luminal cells. J Pathol 225 (2): 181–188.
Bonkhoff H, Berges R (2010) From pathogenesis to prevention of castration resistant prostate cancer. Prostate 70 (1): 100–112.
Buchanan G, Irvine RA, Coetzee GA, Tilley WD (2001) Contribution of the androgen receptor to prostate cancer predisposition and progression. Cancer Metastasis Rev 20 (3-4): 207–223.
Chen CD, Welsbie DS, Tran C, Baek SH, Chen R, Vessella R, Rosenfeld MG, Sawyers CL (2004) Molecular determinants of resistance to antiandrogen therapy. Nat Med 10 (1): 33–39.
Choi N, Zhang B, Zhang L, Ittmann M, Xin L (2012) Adult murine prostate basal and luminal cells are self-sustained lineages that can both serve as targets for prostate cancer initiation. Cancer Cell 21 (2): 253–265.
Chouinard S, Barbier O, Belanger A (2007) UDP-glucuronosyltransferase 2B15 (UGT2B15) and UGT2B17 enzymes are major determinants of the androgen response in prostate cancer LNCaP cells. J Biol Chem 282 (46): 33466–33474.
Collins AT, Berry PA, Hyde C, Stower MJ, Maitland NJ (2005) Prospective identification of tumorigenic prostate cancer stem cells. Cancer Res 65 (23): 10946–10951.
English HF, Santen RJ, Isaacs JT (1987) Response of glandular versus basal rat ventral prostatic epithelial cells to androgen withdrawal and replacement. Prostate 11 (3): 229–242.
Feldman BJ, Feldman D (2001) The development of androgen-independent prostate cancer. Nat Rev Cancer 1 (1): 34–45.
Germann M, Wetterwald A, Guzman-Ramirez N, van der Pluijm G, Culig Z, Cecchini MG, Williams ED, Thalmann GN (2012) Stem-like cells with luminal progenitor phenotype survive castration in human prostate cancer. Stem Cells 30 (6): 1076–1086.
Goldstein AS, Huang J, Guo C, Garraway IP, Witte ON (2010) Identification of a cell of origin for human prostate cancer. Science 329 (5991): 568–571.
Goldstein AS, Lawson DA, Cheng D, Sun W, Garraway IP, Witte ON (2008) Trop2 identifies a subpopulation of murine and human prostate basal cells with stem cell characteristics. Proc Natl Acad Sci USA 105 (52): 20882–20887.
Gregory CW, Hamil KG, Kim D, Hall SH, Pretlow TG, Mohler JL, French FS (1998) Androgen receptor expression in androgen-independent prostate cancer is associated with increased expression of androgen-regulated genes. Cancer Res 58 (24): 5718–5724.
Gu G, Yuan J, Wills M, Kasper S (2007) Prostate cancer cells with stem cell characteristics reconstitute the original human tumor in vivo. Cancer Res 67 (10): 4807–4815.
Halkidou K, Gnanapragasam VJ, Mehta PB, Logan IR, Brady ME, Cook S, Leung HY, Neal DE, Robson CN (2003) Expression of Tip60, an androgen receptor coactivator, and its role in prostate cancer development. Oncogene 22 (16): 2466–2477.
Heer R, Collins AT, Robson CN, Shenton BK, Leung HY (2006) KGF suppresses alpha2beta1 integrin function and promotes differentiation of the transient amplifying population in human prostatic epithelium. J Cell Sci 119 (Pt 7): 1416–1424.
Heer R, Douglas D, Mathers ME, Robson CN, Leung HY (2004) Fibroblast growth factor 17 is over-expressed in human prostate cancer. J Pathol 204 (5): 578–586.
Isaacs JT, Coffey DS (1989) Etiology and disease process of benign prostatic hyperplasia. Prostate Suppl 2: 33–50.
Jia X, Li X, Xu Y, Zhang S, Mou W, Liu Y, Lv D, Liu CH, Tan X, Xiang R, Li N (2011) SOX2 promotes tumorigenesis and increases the anti-apoptotic property of human prostate cancer cell. J Mol Cell Biol 3 (4): 230–238.
Kendziorski C, Irizarry RA, Chen KS, Haag JD, Gould MN (2005) On the utility of pooling biological samples in microarray experiments. Proc Natl Acad Sci USA 102 (12): 4252–4257.
Kregel S, Kiriluk KJ, Rosen AM, Cai Y, Reyes EE, Otto KB, Tom W, Paner GP, Szmulewitz RZ, Vander Griend DJ (2013) Sox2 is an androgen receptor-repressed gene that promotes castration-resistant prostate cancer. PLoS One 8 (1): e53701.
Lawson DA, Zong Y, Memarzadeh S, Xin L, Huang J, Witte ON (2010) Basal epithelial stem cells are efficient targets for prostate cancer initiation. Proc Natl Acad Sci USA 107 (6): 2610–2615.
Lee SO, Ma Z, Yeh CR, Luo J, Lin TH, Lai KP, Yamashita S, Liang L, Tian J, Li L, Jiang Q, Huang CK, Niu Y, Yeh S, Chang C (2012) New therapy targeting differential androgen receptor signaling in prostate cancer stem/progenitor vs non-stem/progenitor cells. J Mol Cell Biol 5 (1): 14–26.
Leong KG, Wang BE, Johnson L, Gao WQ (2008) Generation of a prostate from a single adult stem cell. Nature 456 (7223): 804–808.
Linn DE, Yang X, Sun F, Xie Y, Chen H, Jiang R, Chumsri S, Burger AM, Qiu Y (2010) A role for OCT4 in tumor initiation of drug-resistant prostate cancer cells. Genes Cancer 1 (9): 908–916.
Mousses S, Wagner U, Chen Y, Kim JW, Bubendorf L, Bittner M, Pretlow T, Elkahloun AG, Trepel JB, Kallioniemi OP (2001) Failure of hormone therapy in prostate cancer involves systematic restoration of androgen responsive genes and activation of rapamycin sensitive signaling. Oncogene 20 (46): 6718–6723.
Murai T, Samata N, Iwabuchi H, Ikeda T (2006) Human UDP-glucuronosyltransferase, UGT1A8, glucuronidates dihydrotestosterone to a monoglucuronide and further to a structurally novel diglucuronide. Drug Metab Dispos 34 (7): 1102–1108.
Ousset M, Van Keymeulen A, Bouvencourt G, Sharma N, Achouri Y, Simons BD, Blanpain C (2012) Multipotent and unipotent progenitors contribute to prostate postnatal development. Nat Cell Biol 14 (11): 1131–1138.
Reid AH, Attard G, Danila DC, Oommen NB, Olmos D, Fong PC, Molife LR, Hunt J, Messiou C, Parker C, Dearnaley D, Swennenhuis JF, Terstappen LW, Lee G, Kheoh T, Molina A, Ryan CJ, Small E, Scher HI, de Bono JS (2010) Significant and sustained antitumor activity in post-docetaxel, castration-resistant prostate cancer with the CYP17 inhibitor abiraterone acetate. J Clin Oncol 28 (9): 1489–1495.
Richardson GD, Robson CN, Lang SH, Neal DE, Maitland NJ, Collins AT (2004) CD133, a novel marker for human prostatic epithelial stem cells. J Cell Sci 117 (Pt 16): 3539–3545.
Taplin ME, Balk SP (2004) Androgen receptor: a key molecule in the progression of prostate cancer to hormone independence. J Cell Biochem 91 (3): 483–490.
Tukey RH, Strassburg CP (2000) Human UDP-glucuronosyltransferases: metabolism, expression, and disease. Ann Rev Pharmacol Toxicol 40: 581–616.
Varambally S, Yu J, Laxman B, Rhodes DR, Mehra R, Tomlins SA, Shah RB, Chandran U, Monzon FA, Becich MJ, Wei JT, Pienta KJ, Ghosh D, Rubin MA, Chinnaiyan AM (2005) Integrative genomic and proteomic analysis of prostate cancer reveals signatures of metastatic progression. Cancer Cell 8 (5): 393–406.
Williamson SC, Hepburn AC, Wilson L, Coffey K, Ryan-Munden CA, Pal D, Leung HY, Robson CN, Heer R (2012) Human alpha(2)beta(1) (HI) CD133(+VE) epithelial prostate stem cells express low levels of active androgen receptor. PLoS One 7 (11): e48944.
Zhang W, Carriquiry A, Nettleton D, Dekkers JC (2007) Pooling mRNA in microarray experiments and its effect on power. Bioinformatics 23 (10): 1217–1224.
Acknowledgements
We acknowledge Dr Anne Collins and Prof Norman Maitland (University of York, UK) who provided training in primary prostate epithelial SC selection and the Newcastle University Bioinformatics Support Unit. This work was supported by Newcastle upon Tyne NHS Trustees and Cancer Research UK.
Author Contributions
Experiments were carried out by SCW, RM, ACH, AM, and LW. Data analysis was performed by SCW, RM, and RH. Intellectual input was provided by SCW CNR, HYL, and RH, and manuscript preparation was done by SCW and RH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License.
Supplementary Information accompanies this paper on British Journal of Cancer website
Supplementary information
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Williamson, S., Mitter, R., Hepburn, A. et al. Characterisations of human prostate stem cells reveal deficiency in class I UGT enzymes as a novel mechanism for castration-resistant prostate cancer. Br J Cancer 109, 950–956 (2013). https://doi.org/10.1038/bjc.2013.399
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bjc.2013.399
Keywords
This article is cited by
-
Surface acoustic wave (SAW) techniques in tissue engineering
Cell and Tissue Research (2021)
-
The induction of core pluripotency master regulators in cancers defines poor clinical outcomes and treatment resistance
Oncogene (2019)
-
UGT1A polymorphisms associated with worse outcome in colorectal cancer patients treated with irinotecan-based chemotherapy
Cancer Chemotherapy and Pharmacology (2018)
-
UDP-glucuronosyltransferases and biochemical recurrence in prostate cancer progression
BMC Cancer (2017)