Abstract
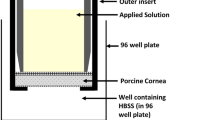
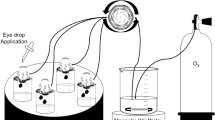
Nepafenac, the amide analog of the NSAID amfenac, was examined in vitro for its bioactivation by ocular tissue components and its ability to permeate external ocular barriers. Rabbit tissues catalyzed a concentration-dependent conversion of nepafenac to amfenac. The order of specific hydrolytic activity is retina/choroid ≫ iris/ciliary body. Corneal tissue showed only minimal activity. Similarly, in human ocular cadaver tissue the specific activity of iris/ciliary body was greater than cornea. Continued perfusion of the corneal epithelium demonstrated a nearly six-fold greater permeation coefficient for nepafenac (k p = 727 × 10−6 min−1) than for diclofenac (k p = 127 × 10−6 min−1). Superior permeation of conjunctival and scleral tissue by nepafenac (k p = 128 × 10−6 min−1) compared to diclofenac (k p = 80 × 10−6 min−1) was also evident. Short term perfusion (5 min) of the corneal surface with 0.1% nepafenac resulted in sustained flux of drug across the cornea for 6 h. Under identical conditions only 3.3 μM of diclofenac accumulated on the corneal endothelial side compared to 16.7 μM nepafenac. The enhanced permeability of nepafenac, combined with rapid bioactivation to amfenac by the iris/ciliary body and retina/choroid, make it a target specific NSAID for inhibiting prostaglandin formation in the anterior and posterior segments of the eye.
Similar content being viewed by others
REFERENCES
SANCILIO, L. F., D. L. REESE, S. CHEUNG, and R. S. ALPHIN. 1977. AHR-5850: a potent anti-inflammatory compound. Agents Actions, 7:133-144.
WALSH, D. A., H. W. MORAN, D. A. SHAMBLEE, I. M. UWAYDAH, W. J. WELSTEAD, JR., L. F. SANCILIO, and W. N. DANNENBURG. 1984. Anti-inflammatory agents. 3. Synthesis and pharmacological evaluation of 2-amino-3-benzoylphenylacetic acid and analogues. J. Med. Chem., 27:1379-1388.
WALSH, D. A., H. W. MORAN, D. A. SHAMBLEE, W. J. WELSTEAD, JR., J. C. NOLAN, L. F. SANCILIO, and G. GRAFF. 1990. Anti-inflammatory agents. 4. Syntheses and biological evaluation of potential prodrugs of 2-amino-3-benzoylbenzeneacetic acid and 2-amino-3-(4-chlorobenzoyl) benzeneacetic acid. J. Med. Chem., 33:2296-2304.
JAIN, A. K., C. C. HUNLEY, J. KUEBEL, F. G. MCMAHON, and J. J. RYAN. 1986. Analgesic efficacy of amfenac, aspirin and placebo after extraction of impacted teeth. Pharmacotherapy, 6:236-240.
GAMACHE, D. A., G. GRAFF, M. T. BRADY, J. M. SPELLMAN, and J. M. YANNI. Nepafenac, a unique nonsteroidal prodrug with potential utility in the treatment of trauma-induced ocular inflammation. I. Assessment of anti-inflammatory efficacy. (In press).
SCHOENWALD, R., and H. HUANG. 1983. Corneal penetration behavior of beta-blocking agents. I. Physicochemical factors. J. Pharm. Sci., 72:1266-1271.
FRANZ, T. H. The theory and practice of the Franz diffusion cell. 1978. In: Current Problems in Dermatology. 7. Karger, Basel, 58-68.
KATO, Y., M. SHIMOKAWA, T. YOKOYAMA. 1993. Simultaneous determination of amfenac sodium and its metabolite (7-benzoyl-2-oxindole) in human plasma by high-performance liquid chromatography. J. Chromat., 616:67-71.
GRASS, G. M., and J. R. ROBINSON. 1988. Mechanisms of corneal drug penetration I: In vivo and in vitro kinetics. J. Pharm. Sci., 77:3-14.
GRASS, G. M., and J. R. ROBINSON. 1988. Mechanisms of corneal drug penetration II: Ultrastructural analysis of potential pathways for drug movement. J. Pharm. Sci., 77:15-23.
SALL, K. N., and T. A. PASQUINE. The Nepafenac Dose-Response Study Group. 1998. Nepafenac is effective in reducing anterior chamber inflammation following cataract surgery. Invest. Ophthalmol. Vis. Sci., 39(suppl):851.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Ke, TL., Graff, G., Spellman, J.M. et al. Nepafenac, a Unique Nonsteroidal Prodrug with Potential Utility in the Treatment of Trauma-Induced Ocular Inflammation: II. In Vitro Bioactivation and Permeation of External Ocular Barriers. Inflammation 24, 371–384 (2000). https://doi.org/10.1023/A:1007001131987
Issue Date:
DOI: https://doi.org/10.1023/A:1007001131987