-
PDF
- Split View
-
Views
-
Cite
Cite
Kwan Chang Kim, Kwang Ree Cho, Yong-Jin Kim, Dae-Won Sohn, Ki-Bong Kim, Long-term results of the Cox-Maze III procedure for persistent atrial fibrillation associated with rheumatic mitral valve disease: 10-year experience, European Journal of Cardio-Thoracic Surgery, Volume 31, Issue 2, February 2007, Pages 261–266, https://doi.org/10.1016/j.ejcts.2006.11.017
Close - Share Icon Share
Abstract
Objective: We evaluated the long-term results of the Cox-Maze III procedure (CM-III) for persistent atrial fibrillation (AF) associated with rheumatic mitral valve (MV) disease. Methods: We analyzed 127 patients who underwent the CM-III combined with a rheumatic MV procedure between 1994 and 2004. In-hospital mortalities were excluded from the study. Results: There were 10 late deaths and the mean follow-up duration was 7.1 ± 2.8 years (range, 13 months to 11.5 years). Normal sinus rhythm was restored in 88.2% (112/127) after the CM-III. Right atrial contractility was demonstrable in 100% (112/112) and left atrial contractility in 68.8% (77/112) of the patients restored to sinus rhythm. Fifteen patients never regained sinus rhythm after the CM-III (AF treatment failure). Permanent pacemakers were implanted in 4.7% (6/127) of the patients during the follow-up. Late recurrence of AF developed in 34 of 112 patients at 44 ± 27 months postoperatively, and sinus rhythm was restored in 29 of 34 patients by administration of an antiarrhythmic medication. Independent risk factors for late AF recurrence were longer duration of AF (>60 months) (odds ratio (OR) = 2.758, p = 0.025), increased left atrial size (OR = 1.113, p = 0.004). Freedom from AF recurrence was 93% at 1-year, 82% at 3 years, 71% at 5 years, and 63% at 7 years. Risk factors for AF treatment failure were longer duration of AF (>60 months) (p ≪ 0.001) and increased patient age (p = 0.030). A higher prevalence of significant late tricuspid regurgitation was observed in patients with AF treatment failure and those with late AF recurrence. Conclusions: The CM-III for persistent AF associated with rheumatic MV disease demonstrated a progressively decreased cure rate during the follow-up period. Early surgical therapy, aggressive left atrial reduction, and correction of tricuspid regurgitation at the time of surgery may increase the long-term success rate.
1 Introduction
Atrial fibrillation (AF) is the most common sustained arrhythmia in patients with mitral valve (MV) disease, and the surgical correction of AF combined with MV surgery has been shown to have advantages in terms of survival, cardiac function, and freedom from stroke and cardiac events [1–3].
The Maze procedure is currently regarded as an efficient surgical technique for the management of medically refractory AF, and has shown similar efficacy in patients with AF associated with valvular, coronary, or congenital heart disease compared with that in patients with lone AF [4]. However, the early surgical results for AF associated with MV disease, especially rheumatic MV disease, have been reported to be less effective [5,6], and the long-term surgical results for AF associated with rheumatic MV disease have not been reported.
The aims of this study were (1) to assess the long-term results of the Cox-Maze III procedure (CM-III) for persistent AF associated with rheumatic MV disease and (2) to elucidate the risk factors for late AF recurrence and AF treatment failure in patients with rheumatic MV disease.
2 Patients and methods
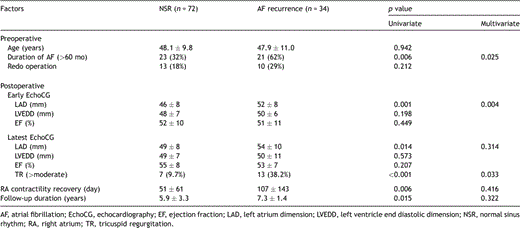
A total of 127 patients, who underwent the CM-III for persistent AF combined with procedures to correct rheumatic MV disease between April 1994 and December 2004, were studied (Table 1 ). In-hospital mortalities were excluded from the study. There were 45 men and 82 women, with a mean age of 49.3 ± 10.0 years (range, 24–73 years) at the time of operation. The mean duration of AF before the operation was 6.4 ± 6.2 years (range, 1 month to 25 years). Concomitant MV procedures were MV replacement in 106 patients and MV repair in 21 patients (Table 1).
Our indications to perform the concomitant CM-III were persistent AF of more than 6-month duration before the operation (110 of 127 patients), presence of left atrial (LA) thrombi (46 of 127 patients), or medical history of previous thromboembolic events (34 of 127 patients).
All of the patients in this study had persistent AF, defined as continuous AF of more than 1-month duration before the operation and not self-terminating, in which cardioversion had not been indicated or attempted. Electrocardiogram (ECG) evidence of AF was checked at two or more separate visits at least 1 month apart, without evidence of sinus conversion. The duration of AF was defined as the months between the earliest date when AF was reliably documented in the medical records and the operation date. We diagnosed rheumatic MV disease based on past medical history of rheumatic fever, intraoperative findings of MV defects, or morphologic evaluation of the operatively excised MV in cases of MV replacement.
Late recurrence of AF was defined as recurrent AF or atrial flutter occurring at least 6 months after postoperative conversion to sinus rhythm. If the patient developed early postoperative AF or late recurrent AF, the patient was treated with an antiarrhythmic agent such as amiodarone or flecainide. Cardioversion was not used because none of the patients showed hemodynamic compromise during AF episodes. AF treatment failure was defined as permanent AF or junctional rhythm of more than 1 year after the CM-III in spite of the addition of an antiarrhythmic medication. Risk factors for AF treatment failure were analyzed by comparing the group of patients who were in permanent AF or junctional rhythm (n = 15) and those who were in sinus rhythm after the CM-III (n = 112).
We initially performed the CM-III in the manner that Cox and associates [7] had described previously. In November 1996, we modified this procedure and replaced some of the incisions with a linear line of ablations [8]. However, the basic lesion set remained unchanged.
The patient clinical profiles and follow-up outcomes were recorded prospectively in a computer-based database system. The closing date for enrolling patient follow-up data for this study was December 31, 2005. Thus all patients had a minimum of 12 months follow-up. All deaths occurring outside of the hospital were confirmed by contacting the patient’s relatives or county death records. The study protocol was reviewed by the Institutional Review Board and approved as a minimal risk retrospective study (Approval Number: H-0509-502-157) that did not require individual consent based on the institutional guidelines for waiving consent.
2.1 Postoperative follow-up
Postoperative ECG was used to determine the presence of AF. ECG was continuously monitored during the patient’s stay in the intensive care unit, and the standard 12-lead ECG was checked daily during the postoperative hospital stay, and at 1, 3, 6, and 12 months postoperatively, and every 6 months thereafter. To evaluate cardiac function and the recovery of the atrial contraction, transthoracic echocardiography (TTE) was performed before discharge, and at 3, 6, and 12 months postoperatively, and every other year thereafter.
2.2 Statistical analysis
Data were collected and managed in Microsoft Excel 2003 and analyzed with SPSS 12.0 software (SPSS, Inc., Chicago, IL). Twelve preoperative and postoperative variables were evaluated in a univariate analysis to identify potential predictors of late AF recurrence, AF treatment failure, and sinus conversion failure after late AF recurrence. Univariate analyses were performed for all relevant categoric variables by means of χ2 analysis and Student’s t tests for continuous variables. Cox proportional hazard model was used to determine the independent predictors of late AF recurrence. Kaplan–Meier survival curve estimated the freedom from AF recurrence. All results were expressed as mean ± standard deviation, and a value of p less than 0.05 was considered statistically significant.
3 Results
3.1 Early postoperative data
The mean aortic cross-clamp time for all patients was 140 ± 39 min, and the mean cardiopulmonary bypass time was 228 ± 64 min. Postoperative complications were perioperative supraventricular tachyarrhythmias including AF (47.2%, 60/127), intra-aortic balloon pump therapy (5.5%, 7/127), reoperation for bleeding (3.9%, 5/127), transient acute renal failure (3.1%, 4/127), and aggravation of previous hemiplegia (0.8%, 1/127). Perioperative supraventricular tachyarrhythmias were usually transient, and sinus rhythm was restored in 88.2% (112/127) of patients during the follow-up. Seventy-six patients (59.8%) were discharged from the hospital in sinus rhythm. Fifteen patients never restored to sinus rhythm after the CM-III (permanent AF in 13 patients and junctional rhythm in 2 patients), and they were regarded as the AF treatment failure group. Right atrial (RA) contractility was demonstrable in 100% (112/112) and left atrial contractility in 68.8% (77/112) of the patients who were restored to sinus rhythm. RA and LA contractilities were restored a mean of 75 ± 108 days and 164 ± 188 days after the operation, respectively. LA contractility was restored significantly later at a lower rate than RA contractility in patients with rheumatic MV disease (p ≪ 0.05).
3.2 Late follow-up
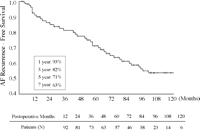
Late follow-up was achieved in 92.1% (117 of 127) of patients, with a mean follow-up duration of 7.2 ± 2.7 years (range, 13 months to 11.5 years). There were 10 late deaths (2 pancreas cancers, 1 intracerebral hemorrhage, 1 sepsis, 1 cardiomyopathy, 1 myocardial infarction, 1 breast cancer, 1 suicide, and 2 unknown causes) during the period. Permanent pacemakers were implanted in 6 of 127 patients (4.7%) due to sick sinus syndrome or tachycardia–brachycardia syndrome during the follow-up. Reoperations were performed in seven patients during the follow-up (paravalvular leakage in three patients, redo operation after MV repair in two patients, redo operation for significant late tricuspid regurgitation (TR) in one patient, and infective endocarditis in one patient). Of the 94 patients who were in sinus rhythm at the latest follow-up, AF was controlled by surgery alone in 73.4% (69/94) of patients and by the addition of an antiarrhythmic agent in 26.6% (25/94) of patients. The rate of freedom from AF decreased to 93% at 1 year, 82% at 3 years, 71% at 5 years, and 63% at 7 years (Fig. 1 ).
3.3 Late recurrence of AF and AF treatment failure
Late AF recurrence developed in 34 of 112 patients (30%) at least 6 months after sinus conversion during the follow-up. Late recurrence of AF developed at a mean of 44 ± 27 months (range, 7 months to 8.3 years) postoperatively. Patients with late AF recurrence demonstrated a higher prevalence of late tricuspid regurgitation at the latest TTE (p = 0.033), when compared with those in sinus rhythm.
Multivariate analysis identified longer duration of preoperative AF (>60 months) (odds ratio (OR) = 2.758, p = 0.025) and larger postoperative LA diameter (OR = 1.113, p = 0.004) as independent risk factors for late AF recurrence (Table 2 ).
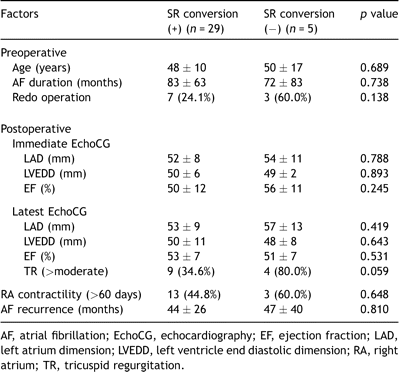
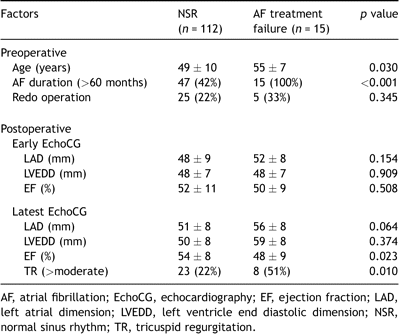
Of 34 patients who developed late AF recurrence, 29 patients were restored to sinus rhythm by administration of an antiarrhythmic agent. Patients who failed to return to sinus rhythm after late AF recurrence tended to have a higher prevalence of late TR (>moderate) at the latest TTE (p = 0.059) (Table 3 ). Fifteen patients (permanent AF in 13 patients and junctional rhythm in 2 patients) never regained sinus rhythm after the CM-III. Patients with AF treatment failure showed lower left ventricular ejection fraction (p = 0.023) and a higher incidence of late TR at the latest TTE (p = 0.010), when compared with those who regained sinus rhythm after the CM-III. Preoperative risk factors for AF treatment failure after the CM-III included older age (p = 0.030) and longer duration of preoperative AF in univariate analysis (p ≪ 0.001) (Table 4 ).
4 Discussion
This study revealed four main findings. First, the CM-III for persistent AF associated with rheumatic MV disease demonstrated a progressively decreased rate of freedom from AF during the follow-up period. Second, risk factors for late AF recurrence included longer duration of preoperative AF and larger postoperative LA size. Third, risk factors for AF treatment failure after the CM-III included older age at operation and longer duration of preoperative AF. Fourth, patients with late AF recurrence as well as those with AF treatment failure showed a higher prevalence of late TR (>moderate), when compared with those in sinus rhythm.
Since Cox and associates [9,10] have demonstrated that the CM-III patients revealed a higher incidence of postoperative sinus rhythm, less arrhythmia recurrence, and improved atrial transport function than patients who underwent either the Maze I or Maze II procedure, the CM-III has been regarded as the technique of choice for the management of medically refractory AF. Regarding the long-term results after the CM-III, Prasad and associates [4] demonstrated that the overall freedom from AF at a mean follow-up of 5.4 years was 96.6% and there was no difference between the lone AF and concomitant procedure groups. On the contrary, many other long-term results of the Maze procedure combined with MV surgery demonstrated a decreased freedom from AF during the follow-up period [3,11,12]. Izumoto and associates [11] demonstrated a gradual attrition rate of sinus rhythm maintenance in the Maze patients who underwent the combined cardiac surgery. The probability of sinus rhythm maintenance at 1 year was 88.8% and at 5 years was 64.8%, showing an attrition rate of 0.6% per patient month. The present study also showed a progressively decreased rate of freedom from AF during the follow-up period: 93% at 1 year, 82% at 3 years, 71% at 5 years, and 63% at 7 years. Progressively decreasing freedom from AF in patients with rheumatic MV disease is largely dependent on the late recurrence of AF, and is assumed to derive from progressive rheumatic changes to the atrial wall or degeneration of atrial tissue resulting from pressure and volume overloading that occurs in valvular heart disease.
Postoperative atrial tachyarrhythmias, including AF, have been reported to occur commonly after the Maze procedure [6,9,10,13]. Postoperative AF recorded during the first 3 months postoperatively is considered early AF recurrence, and that recorded later is considered late AF recurrence. Ad and associates [13] reported that late AF recurrence occurred in 30.9% of patients and explained the mechanisms of late AF recurrence as progressive LA dilatation after surgery, or degree of atrial remodeling and its degree of reversibility at the time of the Maze procedure. Previous studies [3,13–15] demonstrated that predictors for late AF recurrence were history of early postoperative AF recurrence, longer duration of preoperative AF, larger LA diameter, and Cox-Maze procedure version. In the present study, late AF recurrence developed in 30% of patients at least 6 months after sinus rhythm conversion during the follow-up, and sinus rhythm was restored in 85% of patients by administration of an antiarrhythmic agent. Patients with late AF recurrence demonstrated a higher prevalence of late TR (>moderate), when compared with those in sinus rhythm. Risk factors for late AF recurrence were longer duration of preoperative AF and larger postoperative LA diameter. Of 34 patients who developed late AF recurrence, 29 patients were restored to sinus rhythm by administration of an antiarrhythmic agent. Five patients who failed to be restored to sinus rhythm tended to have a higher prevalence of late TR (>moderate) at the latest TTE. Our data suggested active treatment of late AF recurrence. In addition, early surgical therapy, and LA reduction and correction of TR at the time of surgery were also suggested to reduce late AF recurrence.
Although the previous study [6] suggested that AF associated with rheumatic MV disease could also be cured with a high rate of success, a rather low sinus conversion rate was assumed to derive from rheumatic changes or degeneration of atrial tissue that occurred in valvular heart disease [16]. The risk factors for AF treatment failure in previous studies [3,17] included larger LA diameter, longer duration of AF, and smaller f-wave voltage in V1. The present study showed 11.8% of patients (15 of 127) were permanently in AF or junctional rhythm after surgery and were defined as AF treatment failure. The patients with AF treatment failure showed lower left ventricular ejection fraction and higher incidence of significant late TR at the latest TTE when compared with those who regained sinus rhythm after the CM-III. The risk factors for AF treatment failure included older age and longer duration of preoperative AF.
Preoperative functional TR may decrease gradually after MV surgery with reduction of right ventricular pressure or volume overload; however, TR often progresses late after surgery even without left-sided valvular dysfunction [18–20]. The mechanism of progression of TR after MV surgery has been elusive [19–21]. AF itself was recognized as one of the predisposing factors for late TR [19,20]. In patients with persistent AF, AF may induce mechanical and electrical remodeling of both atria, leading to atrial dilatation. RA dilatation may induce tricuspid annulus dilation with resultant TR progression. MV annulus distortion by MV surgery may be a cause of increased LA pressure [21], which leads to increased right ventricular afterload and eventually right-sided chamber enlargement and late TR. In the present study, sixteen patients who showed more than a moderate degree of TR after a MV procedure were treated by tricuspid annuloplasty and none of the patients developed more than a mild degree of TR early after surgery. However, patients with AF treatment failure showed lower left ventricular ejection fraction and a higher incidence of late TR, suggesting that permanent AF may affect the worsening of TR and left ventricular function over time in patients undergoing MV surgery. Patients with late AF recurrence also demonstrated a higher prevalence of late TR, which might suggest that progression of TR after rheumatic MV surgery predisposed late AF recurrence after the CM-III.
As the present study demonstrated a high incidence of early postoperative tachyarrhythmias including AF and a later and lower restoration rate of LA contractility than RA contractility, we recommended to our patients who had undergone MV repair or MVR using a bioprosthetic valve that anticoagulation be continued at least six or more months postoperatively even if the patient was in sinus rhythm and there had been no thromboembolic events. Although reduced LA contractility was demonstrated, we expected the vulnerability to thromboembolic events to be minimized because the LA auricle, the main site of thrombi formation, was excised and synchronous contraction of the LA with the left ventricle was restored, regardless of the strength of the contraction [9]. We did not experience any late thromboembolic complications in 117 survivors with a mean follow-up of 7.2 ± 2.7 years.
In summary, the CM-III for persistent AF associated with rheumatic MV disease demonstrated a progressively decreased rate of freedom from AF during the follow-up period. Early surgical therapy, and left atrial reduction and correction of tricuspid regurgitation at time of surgery may increase the long-term success rate.
Presented at the joint 20th Annual Meeting of the European Association for Cardio-thoracic Surgery and the 14th Annual Meeting of the European Society of Thoracic Surgeons, Stockholm, Sweden, September 10–13, 2006.
Appendix A
Conference discussion
Dr L.R. Guo (London, Ontario, Canada): It's a very important paper. I have a couple of questions.
Number one, you said that the in-hospital deaths were excluded. What is that number?
Number two, when you talk about the Maze procedure for rheumatic heart disease, how is that different? What do you do with the left atrial isthmus?
Dr Kim: Our in-hospital mortality was 2.3%.
I did not hear your second question exactly. Can you say that again, please?
Dr Guo: You said the Maze procedure is specifically for rheumatic heart disease, but how is that different? What do you do with the left atrial isthmus?
Dr U.O. von Oppell (Cardiff, Wales, U.K.): How are you treating the left atrial isthmus, the area between the pulmonary veins and the mitral annulus?
Dr Kim: During the early period we dissected the left atrial isthmus by surgical incision, and in November 1996 we modified this procedure and replaced the line of incision with cryoablation.
Dr von Oppell: Used cryoprobe?
Dr Kim: Yes.
Dr G. Iyer (Bangalore, India): Over a 10-year period, have you used the same technique of doing the Maze, because I’m sure it affects the results of what you have said.
Dr Kim: We initially performed the Cox-Maze procedure in the manner that Dr. Cox had described. In November 1996 we modified this procedure and replaced some of the incisions with a linear line of cryoablations. However, the basic lesion set remained unchanged.
Dr Iyer: I guess the point I’m trying to make is can you combine the two populations together and interpret the results as one or should you look at them separately?
Dr Kim: Yes, both groups were included in this study.
Dr J. Melo (Lisbon, Portugal): I have two questions. You have presented your results with an attrition rate of around 4% per year. With some other groups, like ourselves, we have published also and reported that in mitral rheumatic patients with permanent A-Fib, the attrition rate after surgery is in the range of 3–5% per year of patients going back into atrial fibrillation. Still in your presentation, you have always been talking on recurrence of atrial fibrillation. My question is, do you have the information on your incidence of normal sinus rhythm after 10 years, not free of atrial fibrillation but normal sinus rhythm? What is the incidence of normal sinus rhythm after 10 years?
My second question refers to thromboembolic events in your patients. Can you give us information about it?
Dr Kim: Of the 94 patients who were in sinus rhythm at the latest follow-up, A-Fib was controlled by surgery alone in 73% (69 of 94 patients) of patients and by the addition of an antiarrhythmic agent, in 27% (25 of 94 patients) of patients.
Regarding the second question, we did not experience any late thromboembolic complications in 117 survivors with a mean follow-up period of 7.2 years. We had only one case of intracerebral hemorrhage, but we did not experience any thromboembolic complications.