Abstract
Objective
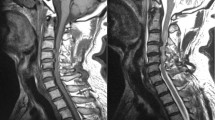
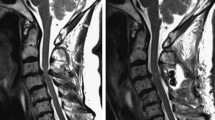
To evaluate the efficacy of the posterior hybrid technique (PHT) for the treatment of traumatic cervical spinal cord injury without vertebral fracture or dislocation with high signal intensity on T2WI (CSCIH).
Methods
A comparative analysis of clinical efficacy between CSCIH patients who underwent anterior decompression and fusion (ADF) surgery and those who underwent PHT surgery was retrospectively conducted. Demographic characteristics, cervical range of motion (CRM), cross-sectional area of spinal cord (CSASC), spinal canal area residual rate (SCARR), high signal intensity ratio (HSIR), Cervical Japanese Orthopedic Association (CJOA) score, and neck disability index (NDI) were assessed.
Results
Forty-three CSCIH cases with PHT and 46 CSCIH cases with ADF were collected from January 2013 to January 2017. The CRM in patients with PHT was superior to that in patients with ADF at the final follow-up (64.21 ± 18.46° vs. 48.71 ± 19.34°, p = 0.0002). The SCARR also showed greater improvements in the PHT group than in the ADF group (final follow-up: 93.54 ± 11.09% vs. 88.13 ± 10.84%, p = 0.022). Both groups indicated significant improvements in the CSASC and HSIR (p < 0.05); however, no significant differences were observed between the two groups. All patients showed improvements in the CJOA score and the NDI after surgery (p < 0.05). At the 6-month follow-up, the ADF group had better NDI scores than the PHT group (31.17 ± 10.42 vs. 36.78 ± 9.65, p = 0.010), whereas the PHT group exhibited better improvements than the ADF group at the final follow-up (66.86 ± 9.28% vs. 57.67 ± 10.22%, p < 0.0001).
Conclusion
The PHT was as effective as ADF in the treatment of CSCIH, whereas the PHT was superior in the improvement of patients’ health-related quality of life and in CRM preservation during the long-term follow-up.


Similar content being viewed by others
References
Maeda, T., Ueta, T., Mori, E., et al. (2012). Soft-tissue damage and segmental instability in adult patients with cervical spinal cord injury without major bone injury. Spine, 37(25), E1560–E1566. https://doi.org/10.1097/BRS.0b013e318272f345
Oichi, T., Oshima, Y., Okazaki, R., et al. (2016). Preexisting severe cervical spinal cord compression is a significant risk factor for severe paralysis development in patients with traumatic cervical spinal cord injury without bone injury: A retrospective cohort study. European Spine Journal, 25(1), 96–102. https://doi.org/10.1007/s00586-015-4142-4
Kawano, O., Ueta, T., Shiba, K., et al. (2010). Outcome of decompression surgery for cervical spinal cord injury without bone and disc injury in patients with spinal cord compression: A multicenter prospective study. Spinal Cord, 48(7), 548–553. https://doi.org/10.1038/sc.2009.179
Uchida, K., Nakajima, H., Takeura, N., et al. (2014). Prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy. The Spine Journal, 14(8), 1601–1610. https://doi.org/10.1016/j.spinee.2013.09.038
Vedantam, A., & Rajshekhar, V. (2013). Does the type of T2-weighted hyperintensity influence surgical outcome in patients with cervical spondylotic myelopathy? A review. European Spine Journal, 22(1), 96–106. https://doi.org/10.1007/s00586-012-2483-9
Sun, Q., Hu, H., Zhang, Y., et al. (2011). Do intramedullary spinal cord changes in signal intensity on MRI affect surgical opportunity and approach for cervical myelopathy due to ossification of the posterior longitudinal ligament? European Spine Journal, 20(9), 1466–1473. https://doi.org/10.1007/s00586-011-1813-7
Wang, J., Li, J., & Cai, L. (2018). Effects of treatment of cervical spinal cord injury without fracture and dislocation in a medium-to long-term follow-up study. World Neurosurgery, 113, e515–e520. https://doi.org/10.1016/j.wneu.2018.02.071
Matsushita, A., Maeda, T., Mori, E., et al. (2017). Can the acute magnetic resonance imaging features reflect neurologic prognosis in patients with cervical spinal cord injury? Spine J, 17(9), 1319–1324. https://doi.org/10.1016/j.spinee.2017.05.009
Suri, A., Chabbra, R. P., Mehta, V. S., et al. (2003). Effect of intramedullary signal changes on the surgical outcome of patients with cervical spondylotic myelopathy. Spine J, 3(1), 33–45.
Ikegami, S., Takahashi, J., Misawa, H., et al. (2018). Spinal cord MRI signal changes at 1 year after cervical decompression surgery is useful for predicting midterm clinical outcome: An observational study using propensity scores. Spine J, 18(5), 755–761. https://doi.org/10.1016/j.spinee.2017.09.004
Fehlings, M. G., Rabin, D., Sears, W., et al. (2010). Current practice in the timing of surgical intervention in spinal cord injury. Spine, 35(21 Suppl), S166–S173. https://doi.org/10.1097/BRS.0b013e3181f386f6
Hirai, T., Yoshii, T., Sakai, K., et al. (2018). Long-term results of a prospective study of anterior decompression with fusion and posterior decompression with laminoplasty for treatment of cervical spondylotic myelopathy. Journal of Orthopaedic Science, 23(1), 32–38. https://doi.org/10.1016/j.jos.2017.07.012
Liu, X., Min, S., Zhang, H., et al. (2014). Anterior corpectomy versus posterior laminoplasty for multilevel cervical myelopathy: A systematic review and meta-analysis. European Spine Journal, 23(2), 362–372. https://doi.org/10.1007/s00586-013-3043-7
Joaquim, A. F., Murar, J., Savage, J. W., et al. (2014). Dysphagia after anterior cervical spine surgery: A systematic review of potential preventative measures. Spine J, 14(9), 2246–2260. https://doi.org/10.1016/j.spinee.2014.03.030
Daniels, A. H., Riew, K. D., Yoo, J. U., et al. (2008). Adverse events associated with anterior cervical spine surgery. Journal of American Academy of Orthopaedic Surgeons, 16(12), 729–738.
Hirabayashi, K., Toyama, Y., & Chiba, K. (1999). Expansive laminoplasty for myelopathy in ossification of the longitudinal ligament. Clinical Orthopaedics and Related Research, 359, 35–48. https://doi.org/10.1097/00003086-199902000-00005
Krappinger, D., Lindtner, R. A., Zegg, M. J., et al. (2019). Spondylotic traumatic central cord syndrome: A hidden discoligamentous injury? European Spine Journal, 28(2), 434–441. https://doi.org/10.1007/s00586-018-5796-5
Chen, Y., Chen, D., Wang, X., et al. (2013). Significance of segmental instability in cervical ossification of the posterior longitudinal ligament and treated by a posterior hybrid technique. Archives of Orthopaedic and Trauma Surgery, 133(2), 171–177. https://doi.org/10.1007/s00402-012-1658-5
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors declared that they have no potential conflict of interest. The manuscript submitted does not contain information about medical device(s)/drug(s).
Ethical approval
The research project was approved by the ethics department of Shanghai Changzheng Hospital, Shanghai. We have consensus with all participants. All the procedures were done under the Declaration of Helsinki and relevant policies in China.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, J., Tao, Z., Tang, Y. et al. Posterior Hybrid Technique for the Treatment of Traumatic Cervical Spinal Cord Injury with High Signal Intensity on T2WI. JOIO 57, 768–775 (2023). https://doi.org/10.1007/s43465-023-00854-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-023-00854-1