Abstract
Purpose
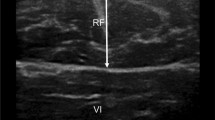
To determine the relationship of the size of the rectus femoris muscle, assessed by ultrasonography, with parameters of muscle strength and body composition that are commonly used in the case-finding of sarcopenia in rehabilitation patients with chronic obstructive pulmonary disease (COPD).
Methods
Cross-sectional pilot study of 18 men with severe COPD and 17 healthy controls. Main outcome variables: cross-sectional area, thickness, and width of the non-dominant rectus femoris muscle obtained by ultrasound, muscle strength determined by voluntary maximum isometric contraction of the quadriceps muscle, and fat-free mass assessed by bioimpedance analysis.
Results
Ultrasounds detected differences in the size of the rectus femoris muscle: cross-sectional area was 4.3 (SD 1.05) cm2 in patients, compared to 5.6 (SD 1.25) cm2 in controls; patients also presented lower quadriceps strength, and fat-free mass index. Cross-sectional area of the rectus femoris muscle showed a moderate correlation with quadriceps strength (R = 0.497, p = 0.036) and fat-free mass (R = 0.584, p = 0.011). In a multivariate linear model adjusted for age, body mass index, fat-free mass and muscle size, muscle strength was 7.44 kg lower (p value = 0.014) in patients, compared to controls.
Conclusions
A causal relationship was observed between the cross-sectional area of the rectus femoris muscle, assessed with ultrasonography, and maximum isometric strength of knee extension in COPD rehabilitation patients. Reduced cross-sectional area was also associated with loss of fat-free mass. Muscle ultrasound and bioimpedance analysis provide complementary and relevant information that could be useful in the case-finding of sarcopenia in COPD patients.


Similar content being viewed by others
References
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F et al (2010) Sarcopenia: European consensus on definition and diagnosis. Age Ageing 39:412–423
Menant JC, Weber F, Lo J, Sturnieks DL, Close JC, Sachdev PS, Brodaty H, Lord SR (2017) Strength measures are better than muscle mass measures in predicting health-related outcomes in older people: time to abandon the term sarcopenia? Osteoporos Int 28:59–70
Gea J, Casadevall C, Pascual S, Orozco-Levi M, Barreiro E (2012) Respiratory diseases and muscle dysfunction. Expert Rev Resp Med. 6:75–90
Maltais F, Decramer M, Casaburi R, Barreiro E, Burelle Y, Debigaré R et al (2014) An official American Thoracic Society/European Respiratory Society Statement: update on limb muscle dysfunction in chronic obstructive pulmonary disase. Am J Respir Crit Care Med 189:e15–e62
Seymour JM, Spruit MA, Hopkinson NS, Natanek SA, Man WD, Jackson A et al (2010) The prevalence of quadriceps weakness in COPD and the relationship with disease severity. Eur Respir J 36:81–88
Decramer M, Gosselink R, Troosters T, Verschueren M, Evers G (1997) Muscle weakness is related to utilization of health care resources in COPD patients. Eur Respir J 10:417–423
Gosselink R, Troosters R, Decramer M (1996) Peripheral muscle weakness contributes to exercise limitation in COPD. Am J Respir Crit Care Med 153:976–980
Mostert R, Goris A, Weling-Scheepers C, Wouters EF, Schols AM (2000) Tissue depletion and health related quality of life in patients with chronic obstructive pulmonary disease. Respir Med 94:859–867
Swallow EB, Reyes D, Hopkinson NS, Man WD, Porcher R, Cetti EJ et al (2007) Quadriceps strength predicts mortality in patients with moderate to severe chronic obstructive pulmonary disease. Thorax 62:115–120
Chien MY, Huang TY, Wu YT (2008) Prevalence of sarcopenia estimated using a bioelectrical impedance analysis prediction equation in community-dwelling elderly people in Taiwan. J Am Geriatr Soc 56:1710–1715
Correa-de-Araujo R, Harris-Love MO, Miljkovic I, Fragala MS, Anthony BW, Manini TM (2017) The need of standardized assessment of muscle quality in skeletal muscle function deficit and other aging-related muscle dysfunctions: a symposium report. Front Physiol. 8:87
Ticinesi A, Meschi T, Narici MV, Lauretani F, Maggio M (2017) Muscle ultrasound and sarcopenia in older individuals: a clinical perspective. J Am Med Dir Assoc. 18:290–300
e Lima KMM, Matta TT, Oliveira LF (2012) Reliability of the rectus femoris muscle cross-sectional area measurements by ultrasonography. Clin Physiol Funct Imaging 32:221–226
Bemben MG (2002) Use of diagnostic ultrasound for assessing muscle size. J Strength Cond Res. 16:103–108
Scott JM, Martin DS, Ploutz-Snyder R, Matz T, Caine T, Downs M, Hackney K, Buxton R, Ryder JW, Ploutz-Snyder L (2017) Panoramic ultrasound: a novel and valid tool for monitoring change in muscle mass. J Cachexia Sarcopenia Muscle. https://doi.org/10.1002/jcsm.12172
Menon M, Houchen L, Harrison S, Singh S, Morgan M (2012) Ultrasound assessment of lower limb muscle mass in response to resistance training in COPD. Respir Res 13:119
Schols AM, Ferreira IM, Franssen FM, Gosker HR, Janssens W, Muscaritoli M et al (2014) Nutritional assessment and therapy in COPD: a European Respiratory Society statement Singh. Eur Respir J. https://doi.org/10.1183/09031936.00070914
Perkisas S, Baudry S, Bauer J, Beckwée D, De Cock AM, Hobbelen H, Jager-Wittenaar H, Kasiukiewicz A, Landi F, Marco E, Merelló A, Piotrowicz K, Sánchez E, Sánchez-Rodríguez D, Scafoglieri A, Cruz-Jentoft A, Vandewoude M (2018) Application of ultrasound for muscle assessment in sarcopenia: towards standardized measurements. Eur Geriatr Med. https://doi.org/10.1007/s41999-018-0104-9
Global Strategy for the Diagnosis, Management and Prevention of COPD. Global initiative for chronic obstructive lung disease (GOLD) 2017. http://goldcopd.org/. Accessed Oct 2018
Cáceres DI, Messaggi-Sartor M, Rodríguez DA, Escalada F, Gea J, Orozco-Levi M et al (2014) Variability in bioelectrical impedance assessment of body composition depending on measurement conditions: influence of fast and rest. Nutr Hosp 30:1359–1365
Deurenberg P, van der Kooij K, Evers P, Hulshof T (1990) Assessment of body composition by bioelectrical impedance in a population aged greater than 60 y. Am J Clin Nutr 51(1):3–6
Schutz Y, Kyle UU, Pichard C (2002) Fat-free mass index and fat mass index percentiles in Caucasians aged 18–98 y. Int J Obesity. Int J Obes Relat Metab Disord 26:953–960
Luna-Heredia E, Martín-Peña G, Ruiz-Galiana J (2005) Handgrip dynamometry in healthy adults. Clin Nutr 24:250–258
Lauretani F, Russo CR, Bandinelli S, Bartali B, Cavazzini C, Di Iorio A et al (2003) Age associated changes in skeletal muscles and their effect on mobility: an operational diagnosis of sarcopenia. J Appl Physiol 95:1851–1860
Sánchez-Rodríguez D, Marco E, Miralles R, Fayos M, Mojal S, Alvarado M et al (2014) Sarcopenia, physical rehabilitation and functional outcomes of patients in a subacute geriatric care unit. Arch Gerontol Geriatr 59:39–43
Sánchez-Rodríguez D, Marco E, Miralles R, Guillén-Solà A, Vázquez-Ibar O, Escalada F et al (2015) Does gait speed contribute to sarcopenia case-finding in a postacute rehabilitation setting? Arch Gerontol Geriatr 61:176–181
Holland AE, Spruit MA, Troosters T, Puhan MA, PepinV Saey D et al (2014) An official European Respiratory Society/American Thoracic Society technical standard: field walking tests in chronic respiratory disease. Eur Resp J. 44:1428–1444
Marquis K, Debigaré R, Lacasse Y, LeBlanc P, Jobin J, Carrier G et al (2002) Midthigh muscle cross-sectional area is a better predictor of mortality than body mass index in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 166:809–813
Schols AM, Broekhuizen R, Weling-Scheepers CA, Wouters EF (2005) Body composition and mortality in chronic obstructive pulmonary disease. Am J Clin Nutr 82:53–59
Seymour JM, Ward K, Sidhu PS, Puthucheary Z, Steier J, Jolley CJ et al (2009) Ultrasound measurement of rectus femoris cross-sectional area and the relationship with quadriceps strength in COPD. Thorax 64:418–423
Bernard S, LeBlanc P, Whittom F et al (1998) Peripheral muscle weakness in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 158:629–634
Henneman E (1985) The size principle: a deterministic output emerges from a set of probabilistic connections. J Exp Biol 115:105–112
Baarends EM, Schols AM, Mostert R, Wouters EF (1997) Peak exercise response in relation to tissue depletion in patients with chronic obstructive pulmonary disease. Eur Respir J 10:2807–2813
Steiner MC, Barton RL, Singh SJ, Morgan MDL (2002) Bedside methods versus dual energy X-ray absorptiometry for body composition measurement in COPD. Eur Resp J. 19:626–631
Lerario MC, Sachs A, Lazaretti-Castro M, Saraiva LG, Jardim JR (2006) Body composition in patients with chronic obstructive pulmonary disease: which method to use in clinical practice? Br J Nutr 96:86–92
Rutten EPA, Spruit MA, Wouters EFM (2010) Critical view on diagnosing muscle wasting by single-frequency bio-electrical impedance in COPD. Resp Med. 104:91–98
Acknowledgements
The authors thank the study participants and other contributors, including but not limited to Joan Vila for statistical support and Elaine Lilly, PhD, for unfailing support, language revisions and suggestions.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Ramírez-Fuentes, C., Mínguez-Blasco, P., Ostiz, F. et al. Ultrasound assessment of rectus femoris muscle in rehabilitation patients with chronic obstructive pulmonary disease screened for sarcopenia: correlation of muscle size with quadriceps strength and fat-free mass. Eur Geriatr Med 10, 89–97 (2019). https://doi.org/10.1007/s41999-018-0130-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-018-0130-7