Abstract
Background/Objectives
The emergency department transfer (EDT) rate of residents from nursing homes (NHs) to emergency departments is an important public health issue. The purpose of this study was to examine whether organizational and geographical factors were associated with EDT among older adults living in NHs.
Design
Retrospective analysis using information from patients’ medical charts regarding hospitalization in the last 12 months. Information came from the baseline data of the IQUARE clinical trial.
Participants
5926 residents (86.0 years old, standard deviation, SD = 2.9), from 175 NHs with available data on EDT.
Outcome measure
The EDT rate was estimated for each NH, from the number of residents who were transferred to an emergency department (one transfer or more) in the previous 12 months.
Results
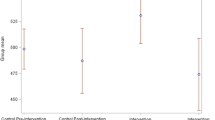
1119 (18.9%, SD = 11.5) residents were transferred to an emergency department at least once during the past year. In adjusted multiple linear regression, NHs located in rural areas had an EDT rate significantly lower than those in urban areas (confidence interval, 95% CI − 10.15, − 2.16, p = 0.003), with an absolute EDT rate of 16.4% (SD = 9.1) versus 20.4% (SD = 12.5); pharmacy for internal use was significantly associated with a lower EDT rate compared with the NHs with no PUI [11.9% (SD = 9.2); 19.1% (SD = 10.1), 95% CI − 16.33, − 3.09, p = 0.004] and the implementation of a personalized care project in NHs was significantly associated with a lower EDT rate [18.6% (SD = 11.4), 22.4% (SD = 12.4), 95% CI − 11.67, − 0.63, p = 0.03].
Conclusion
Our study suggests that a structured plan of care, a strategy to improve medication and being located in rural areas reduce the EDT rate in NH residents.
IQUARE study trial registration number
NCT01703689.
Similar content being viewed by others
Abbreviations
- CN:
-
Coordinating physician
- CP:
-
Coordinating nurse
- ED:
-
Emergency department
- EDT:
-
Emergency Department transfer (per year)
- GMP:
-
Weighted average GIR
- GP:
-
General Practitioner
- 95% CI:
-
95% confidence interval
- INSEE:
-
National Institute of Statistics and Economic Studies
- IQUARE:
-
“l’Impact d’une démarche Qualité sur l’évolution des pratiques et le déclin fonctionnel des Résidents” (Impact of a Quality approach on the development of practices and the functional decline of residents)
- NH:
-
Nursing Home
- PUI:
-
Pharmacy for internal use
References
Graverholt B, Forsetlund L, Jamtvedt G (2014) Reducing hospital admissions from nursing homes: a systematic review. BMC Health Serv Res 14:36
Weissman JS, Gatsonis C, Epstein AM (1992) Rates of avoidable hospitalization by insurance status in Massachusetts and Maryland. JAMA 268:2388–2394
Cameron ID et al (2012) Interventions for preventing falls in older people in care facilities and hospitals. Cochrane Database Syst Rev 12:5465
Lafont C et al (2011) Reducing ‘iatrogenic disability’ in the hospitalized frail elderly. J Nutr Health Aging 15:645–660
Arendts G, Quine S, Howard K (2013) Decision to transfer to an emergency department from residential aged care: a systematic review of qualitative research. Geriatr Gerontol Int 13:825–833
de Souto Barreto P et al (2013) A multicentric individually-tailored controlled trial of education and professional support to nursing home staff: research protocol and baseline data of the IQUARE study. J Nutr Health Aging 17:173–178
Rolland Y et al (2016) Improving the quality of care of long-stay nursing home residents in France. J Am Geriatr Soc 64:193–199
Insee—National Institute of Statistics and Economic Studies. https://www.insee.fr/en/metadonnees/definition/c1501. Accessed 2 Jan 2017
Charlson ME et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Terrell KM, Miller DK (2007) Critical review of transitional care between nursing homes and emergency departments. ResearchGate 15:33–38
de Souto Barreto P et al (2013) Prevalence and associations of the use of proton-pump inhibitors in nursing homes: a cross-sectional study. J Am Med Dir Assoc 14:265–269
Cool C et al (2014) Potentially inappropriate drug prescribing and associated factors in nursing homes. J Am Med Dir Assoc 15:851–859
Ruggiero C et al (2010) Potentially inappropriate drug prescriptions and risk of hospitalization among older, Italian, nursing home residents: the ULISSE project. Drugs Aging 27:747–758
Lau DT et al (2005) Hospitalization and death associated with potentially inappropriate medication prescriptions among elderly nursing home residents. Arch Intern Med 165:68–74
Grabowski DC et al (2008) Predictors of nursing home hospitalization: a review of the literature. Med Care Res Rev 65:3–39
Burgio LD et al (2002) Teaching and maintaining behavior management skills in the nursing home. Gerontol 42:487–496
Ngo J, Holroyd-Leduc JM (2015) Systematic review of recent dementia practice guidelines. Age Ageing 44:25–33
Monette J et al (2008) Effect of an interdisciplinary educational program on antipsychotic prescribing among nursing home residents with dementia. Int J Geriatr Psychiatry 23:574–579
Volicer L et al (1994) Impact of special care unit for patients with advanced Alzheimer’s disease on patients’ discomfort and costs. J Am Geriatr Soc 42:597–603
Briggs R et al (2013) Nursing home residents attending the emergency department: clinical characteristics and outcomes. QJM 106(9):803–808
Author information
Authors and Affiliations
Contributions
XD, PSB and YR conceived the study and designed the statistical analyze. PSB and YR provided statistical advice on study design. XD leads the statistical analyze and drafted the manuscript. All authors contributed substantially to its revision. XD takes responsibility for the paper as a whole.
Corresponding author
Ethics declarations
Conflicts of interest
All authors declare that they have no conflict of interest.
Ethical approval
The research protocol complied with the principles of the Declaration of Helsinki and was approved by the ethics committee of Toulouse University Hospital and the Consultative Committee for Treatment of Research Information on Health (CNIL: 07-438).
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Dubucs, X., de Souto Barreto, P. & Rolland, Y. Organizational and environmental factors associated with transfers of nursing home residents to emergency departments. Eur Geriatr Med 9, 339–346 (2018). https://doi.org/10.1007/s41999-018-0059-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-018-0059-x