Abstract
Purpose
The trend of regenerative medicine is shifting toward the potency of Umbilical Cord Mesenchymal–derived Secretome (UC-MSCs-derived secretome) in treating many diseases such as Type 2 Diabetes Mellitus (T2DM). The UC-MSCs-derived secretome consists of wide range of biological active molecules, such as cytokines, mRNAs, and growth factors. T2DM patient’s serum is used as precondition treatment to induce the UC-MSCs secretome that could benefit in regenerative medicine.
Methods
In brief, UC-MSCs were cultured with T2DM patient’s serum for 24 hours and the culture media was collected. Flow cytometry was used to detect the Angiopoietin-2 (Ang-2), Hepatocytes Growth Factor (HGF), Interleukins-10 (IL-10), Stem Cell Factor (SCF), Granulocyte–Macrophage Colony-Stimulating Factor (GM-CSF), Vascular Endothelial Growth Factor (VEGF), Epidermal Growth Factor (EGF), and Fibroblast Growth Factor (FGF) in UC-MSCs-derived secretome.
Results
A significant increase (p < 0.05) was observed in all detected growth factors and cytokines in the UC-MSCs secretome, except for the IL-10 which was decreasing.
Conclusion
The preconditioning treatment with T2DM patient’s serum that has a chronic inflammation condition altered the expression of the growth factors and cytokine release by the UC-MSCs. However, further study to analyze the potency and efficacy of UC-MSCs-derived secretome from preconditioned with T2DM patient’s serum is needed in T2DM model.
Lay Summary
Umbilical Cord Mesenchymal–derived Secretome (UC-MSCs-derived secretome) has been used for treating many diseases. Up to now, there is no specific secretome to treat certain diseases. In this study, we used Type 2 Diabetes Mellitus (T2DM) patient’s serum as precondition treatment to induce the UC-MSCs secretome that could benefit in treating T2DM. However, further study to analyze the potency and efficacy of UC-MSCs-derived secretome from preconditioned with T2DM patient’s serum is needed in T2DM model.





Similar content being viewed by others
Data Availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request. The reference journals used to support this study are included within the article and cited at relevant places within the test as references.
References
Han Y, Li X, Zhang Y, Han Y, Chang F, Ding J. Mesenchymal stem cells for regenerative medicine. Cells. 2019;8:886. https://doi.org/10.3390/cells8080886.
Merimi M, El-Majzoub R, Lagneaux L, Moussa Agha D, Bouhtit F, Meuleman N, et al. The therapeutic potential of mesenchymal stromal cells for regenerative medicine: current knowledge and future understandings. Front Cell Dev Biol. 2021;9:661532. https://doi.org/10.3389/fcell.2021.661532.
Shi Y, Wang Y, Li Q, Liu K, Hou J, Shao C, et al. Immunoregulatory mechanisms of mesenchymal stem and stromal cells in inflammatory diseases. Nat Rev Nephrol. 2018;14:493–507. https://doi.org/10.1038/s41581-018-0023-5.
Praven Kumar L, Kandoi S, Misra R, Vijayalakshmi S, Rajagopal K, Verma RS. The mesenchymal stem cell secretome: a new paradigm towards cell-free therapeutic mode in regenerative medicine. Cytokine Growth Factor Rev. 2019;46:1–9. https://doi.org/10.1016/j.cytogfr.2019.04.002.
Liang X, Ding Y, Zhang Y, Tse H-F, Lian Q. Paracrine mechanisms of mesenchymal stem cell-based therapy: current status and perspectives. Cell Transplant. 2014;23:1045–59. https://doi.org/10.3727/096368913X667709.
Jimenez-Puerta GJ, Marchal JA, López-Ruiz E, Gálvez-Martín P. Role of mesenchymal stromal cells as therapeutic agents: potential mechanisms of action and implications in their clinical use. J Clin Med. 2020;9:445. https://doi.org/10.3390/jcm9020445.
Phelps J, Sanati-Nezhad A, Ungrin M, Duncan NA, Sen A. Bioprocessing of mesenchymal stem cells and their derivatives: toward cell-free therapeutics. Stem Cells Int. 2018;2018:1–23. https://doi.org/10.1155/2018/9415367.
Meiliana A, Dewi NM, Wijaya A. Mesenchymal stem cell secretome: cell-free therapeutic strategy in regenerative medicine. Indones Biomed J. 2019;11(2):113–24. https://doi.org/10.18585/inabj.v11i2.839.
Cunningham CJ, Redondo-Castro E, Allan SM. The therapeutic potential of the mesenchymal stem cell secretome in ischaemic stroke. J Cereb Blood Flow Metab. 2018;38:1276–92. https://doi.org/10.1177/0271678X18776802.
Ferreira JR, Teixeira GQ, Santos SG, Barbosa MA, Almeida-Porada G, Gonçalves RM. Mesenchymal stromal cell secretome: influencing therapeutic potential by cellular pre-conditioning. Front Immunol. 2018;9:2837. https://doi.org/10.3389/fimmu.2018.02837.
Hu C, Li L. Preconditioning influences mesenchymal stem cell properties in vitro and in vivo. J Cell Mol Med. 2018;22:1428–42. https://doi.org/10.1111/jcmm.13492.
Wang M, Yuan Q, Xie L. Mesenchymal stem cell-based immunomodulation: properties and clinical application. Stem Cells Int. 2018;2018:1–12. https://doi.org/10.1155/2018/3057624.
Castro-Manrreza ME, Montesinos JJ. Immunoregulation by mesenchymal stem cells: biological aspects and clinical applications. J Immunol Res. 2015;2015:1–20. https://doi.org/10.1155/2015/394917.
Tsalamandris S, Antonopoulos AS, Oikonomou E, Papamikroulis G-A, Vogiatzi G, Papaioannou S, et al. The role of inflammation in diabetes: current concepts and future perspectives. Eur Cardiol Rev. 2019;14:50–9. https://doi.org/10.15420/ecr.2018.33.1.
Chen F, Wang J, Liu X, Ma X, Zhang X, Huang T, et al. Levels of inflammatory cytokines in type 2 diabetes patients with different urinary albumin excretion rates and their correlation with clinical variables. J Diabetes Res. 2013;2013:1–6. https://doi.org/10.1155/2013/138969.
Chouw A, Sartika CR, Milanda T, Faried A. Effect of serum from type 2 diabetes mellitus patient in mesenchymal stem cell-derived secretome total protein. Cytotherapy. 2021;23:S194. https://doi.org/10.1016/S1465324921006095.
Yang Y-HK, Ogando CR, Wang See C, Chang T-Y, Barabino GA. Changes in phenotype and differentiation potential of human mesenchymal stem cells aging in vitro. Stem Cell Res Ther. 2018;9:131. https://doi.org/10.1186/s13287-018-0876-3.
Nagamura-Inoue T. Umbilical cord-derived mesenchymal stem cells: their advantages and potential clinical utility. World J Stem Cells. 2014;6:195. https://doi.org/10.4252/wjsc.v6.i2.195.
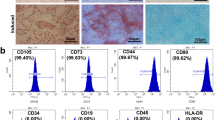
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini FC, Krause DS, et al. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy. 2006;8:315–7. https://doi.org/10.1080/14653240600855905.
Smith JR, Pfeifer K, Petry F, Powell N, Delzeit J, Weiss ML. Standardizing umbilical cord mesenchymal stromal cells for translation to clinical use: selection of GMP-compliant medium and a simplified isolation method. Stem Cells Int. 2016. https://doi.org/10.1155/2016/6810980.
Mishra M, Kumar H, Bajpai S, Singh RK, Tripathi K. Level of serum IL-12 and its correlation with endothelial dysfunction, insulin resistance, proinflammatory cytokines and lipid profile in newly diagnosed type 2 diabetes. Diabetes Res Clin Pract. 2011;94:255–61. https://doi.org/10.1016/j.diabres.2011.07.037.
Chen L, Xu Y, Zhao J, Zhang Z, Yang R, Xie J, et al. Conditioned medium from hypoxic bone marrow-derived mesenchymal stem cells enhances wound healing in mice. PLoS ONE. 2014;9:e96161. https://doi.org/10.1371/journal.pone.0096161.
Kehl D, Generali M, Mallone A, Heller M, Uldry A-C, Cheng P, et al. Proteomic analysis of human mesenchymal stromal cell secretomes: a systematic comparison of the angiogenic potential. NPJ Regen Med. 2019;4:8. https://doi.org/10.1038/s41536-019-0070-y.
Zarrouki B, Benterki I, Fontes G, Peyot M-L, Seda O, Prentki M, et al. Epidermal growth factor receptor signaling promotes pancreatic -cell proliferation in response to nutrient excess in rats through mTOR and FOXM1. Diabetes. 2014;63:982–93. https://doi.org/10.2337/db13-0425.
Yaghini N, Mahmoodi M, Asadikaram GR, Hassanshahi GH, Khoramdelazad H, Kazemi AM. Serum levels of interleukin 10 (IL-10) in patients with type 2 diabetes. Iran Red Crescent Med J. 2011;13:752.
Acknowledgements
We would like to express our gratitude to Andi Wijaya, PhD from Prodia Laboratory, and Dr. Med. Sc. Melisa Intan Barliana and Dr. Tina Rostinawati from Universitas Padjadjaran. We also like to thank all the laboratory personnel from Prodia StemCell Laboratory for their help in this research.
Author information
Authors and Affiliations
Contributions
AC conducted the research and wrote the manuscript. CRS conceived the original idea. AF and TM review the manuscript.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
The ethical advisory board of University of Padjadjaran has approved this study with ethical number 672/UN6.KEP.EC/2020. All the study was conducted in Prodia StemCell (ProSTEM) laboratory. All donors of human sample provided their written informed consent prior to any intervention.
Consent for Publication
There is no consent for publication applicable for this article.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chouw, A., Sartika, C.R., Milanda, T. et al. Effect of Type 2 Diabetes Mellitus Patient’s Serum as Preconditioning on Umbilical Cord Mesenchymal–Derived Secretome Production. Regen. Eng. Transl. Med. 8, 607–614 (2022). https://doi.org/10.1007/s40883-022-00259-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40883-022-00259-w