Abstract
Introduction
Experimental data support the involvement of complement in the pathogenesis of antineutrophil antibody associated vasculitis, and clinical studies describe a more severe disease phenotype in patients with antineutrophil antibody associated vasculitis and complement activation. In the present study, we looked for an association between circulating serum complement factor 3 levels at diagnosis and outcomes.
Methods
One hundred sixty-four patients with antineutrophil antibody associated vasculitis who underwent kidney biopsy at our center during the last 15 years were retrospectively reviewed. Patients were categorized according to their serum complement factor 3 level at diagnosis. Patient and renal survival were compared between those above and below the median serum complement factor 3 at diagnosis.
Results
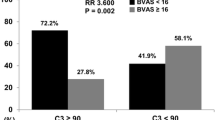
During the first year, 6 patients died and 53 reached end-stage renal disease. Death or end-stage renal disease at one-year were significantly more common in the low serum complement factor 3 group (44 vs. 29%, p = 0.037). In the multivariable analysis, serum complement factor 3 was the strongest negative outcome predictor (HR, 95%CI 0.118, (0.021–0.670)). The lower the serum complement factor 3 level at baseline, the higher the risk of dialysis and death. The risk was particularly high for both endpoints if the serum complement factor 3 concentration was below 0.9 g/l at baseline.
Conclusion
Complement activation at diagnosis may identify a distinct subgroup of patients with antineutrophil antibody associated vasculitis and higher risk for poor outcomes. However, it remains to be proven whether inhibition of serum complement factor 3 is beneficial and safe in the clinical setting.
Graphical abstract





Similar content being viewed by others
Data availability
Data can be shared, after publication, in fully anonymous form after request.
References
Schreiber A, Rousselle A, Becker JU, von Mässenhausen A, Linkermann A, Kettritz R (2017) Necroptosis controls NET generation and mediates complement activation, endothelial damage, and autoimmune vasculitis. Proc Natl Acad Sci USA 114(45):E9618–E9625. https://doi.org/10.1073/pnas.1708247114
Augusto JF, Langs V, Demiselle J, Lavigne C, Brilland B, Duveau A et al (2016) Low serum complement C3 Levels at diagnosis of renal ANCA-associated vasculitis is associated with poor prognosis. PLoS ONE 11(7):e0158871. https://doi.org/10.1371/journal.pone.0158871
Chen M, Xing GQ, Yu F, Liu G, Zhao MH (2009) Complement deposition in renal histopathology of patients with ANCA-associated pauci-immune glomerulonephritis. Nephrol Dial Transplant 24(4):1247–1252. https://doi.org/10.1093/ndt/gfn586
Villacorta J, Diaz-Crespo F, Acevedo M, Cavero T, Guerrero C, Praga M et al (2016) Circulating C3 levels predict renal and global outcome in patients with renal vasculitis. Clin Rheumatol 35(11):2733–2740. https://doi.org/10.1007/s10067-016-3384-9
Villacorta J, Diaz-Crespo F, Acevedo M, Guerrero C, Campos-Martin Y, García-Díaz E et al (2016) Glomerular C3d as a novel prognostic marker for renal vasculitis. Hum Pathol 56:31–39. https://doi.org/10.1016/j.humpath.2016.05.015
Jayne DRW, Bruchfeld AN, Harper L, Schaier M, Venning MC, Hamilton P et al (2017) Randomized trial of C5a receptor inhibitor avacopan in ANCA-associated vasculitis. J Am Soc Nephrol 28(9):2756–2767. https://doi.org/10.1681/asn.2016111179
Jayne DRW, Merkel PA, Schall TJ, Bekker P (2021) Avacopan for the treatment of ANCA-associated vasculitis. N Engl J Med 384(7):599–609. https://doi.org/10.1056/NEJMoa2023386
Kimoto Y, Horiuchi T (2022) The complement system and ANCA associated vasculitis in the era of anti-complement drugs. Front Immunol 13:926044. https://doi.org/10.3389/fimmu.2022.926044
Osman M, Cohen Tervaert JW, Pagnoux C (2021) Avacopan for the treatment of ANCA-associated vasculitis. Expert Rev Clin Immunol 17(7):717–726. https://doi.org/10.1080/1744666x.2021.1932466
Roccatello D, Fenoglio R, Oddone V, Sciascia S (2022) How the availability of anti-C5a agents could change the management of antineutrophil cytoplasmic antibody-associated vasculitis. Kidney Blood Press Res 47(8):506–513. https://doi.org/10.1159/000525357
Tesar V, Hruskova Z (2022) Complement inhibition in ANCA-associated vasculitis. Front Immunol 13:888816. https://doi.org/10.3389/fimmu.2022.888816
Trivioli G, Vaglio A (2020) The rise of complement in ANCA-associated vasculitis: from marginal player to target of modern therapy. Clin Exp Immunol 202(3):403–406. https://doi.org/10.1111/cei.13515
Watts R, Lane S, Hanslik T, Hauser T, Hellmich B, Koldingsnes W et al (2007) Development and validation of a consensus methodology for the classification of the ANCA-associated vasculitides and polyarteritis nodosa for epidemiological studies. Ann Rheum Dis 66(2):222–227. https://doi.org/10.1136/ard.2006.054593
Samman KN, Ross C, Pagnoux C, Makhzoum JP (2021) Update in the management of ANCA-associated vasculitis: recent developments and future perspectives. Int J Rheumatol 2021:5534851. https://doi.org/10.1155/2021/5534851
Jayne DR, Gaskin G, Rasmussen N, Abramowicz D, Ferrario F, Guillevin L et al (2007) Randomized trial of plasma exchange or high-dosage methylprednisolone as adjunctive therapy for severe renal vasculitis. J Am Soc Nephrol 18(7):2180–2188. https://doi.org/10.1681/asn.2007010090
Walsh M, Casian A, Flossmann O, Westman K, Höglund P, Pusey C et al (2013) Long-term follow-up of patients with severe ANCA-associated vasculitis comparing plasma exchange to intravenous methylprednisolone treatment is unclear. Kidney Int 84(2):397–402. https://doi.org/10.1038/ki.2013.131
Walsh M, Collister D, Zeng L, Merkel PA, Pusey CD, Guyatt G et al (2022) The effects of plasma exchange in patients with ANCA-associated vasculitis: an updated systematic review and meta-analysis. BMJ 376:e064604. https://doi.org/10.1136/bmj-2021-064604
Mukhtyar C, Lee R, Brown D, Carruthers D, Dasgupta B, Dubey S et al (2009) Modification and validation of the birmingham vasculitis activity score (version 3). Ann Rheum Dis 68(12):1827–1832. https://doi.org/10.1136/ard.2008.101279
Berden AE, Ferrario F, Hagen EC, Jayne DR, Jennette JC, Joh K et al (2010) Histopathologic classification of ANCA-associated glomerulonephritis. J Am Soc Nephrol 21(10):1628–1636. https://doi.org/10.1681/asn.2010050477
Brix SR, Noriega M, Tennstedt P, Vettorazzi E, Busch M, Nitschke M et al (2018) Development and validation of a renal risk score in ANCA-associated glomerulonephritis. Kidney Int 94(6):1177–1188. https://doi.org/10.1016/j.kint.2018.07.020
Lionaki S, Boletis JN (2022) Hypocomplementemia at diagnosis of antineutrophil cytoplasmic autoantibody glomerulonephritis is an independent risk factor for a worst outcome. Kidney Int Rep 7(3):661. https://doi.org/10.1016/j.ekir.2022.01.1043
Tampe D, Baier E, Hakroush S, Tampe B (2022) Low serum levels of complement C3c at diagnosis indicate poor outcome in antineutrophil cytoplasmic antibody-associated glomerulonephritis. Kidney Int Rep 7(3):660–661. https://doi.org/10.1016/j.ekir.2021.12.038
Lee T, Gasim A, Derebail VK, Chung Y, McGregor JG, Lionaki S et al (2014) Predictors of treatment outcomes in ANCA-associated vasculitis with severe kidney failure. Clin J Am Soc Nephrol 9(5):905–913. https://doi.org/10.2215/cjn.08290813
Huizenga N, Zonozi R, Rosenthal J, Laliberte K, Niles JL, Cortazar FB (2020) Treatment of aggressive antineutrophil cytoplasmic antibody-associated vasculitis with eculizumab. Kidney Int Rep 5(4):542–545. https://doi.org/10.1016/j.ekir.2019.11.021
Sobotta M, Moerer O, Gross O (2021) Case report: eculizumab and ECMO rescue therapy of severe ards in goodpasture syndrome. Front Med (Lausanne). 8:720949. https://doi.org/10.3389/fmed.2021.720949
Kitamura F, Yamaguchi M, Nishimura M, Katsuno T, Ito M, Sugiyama H et al (2022) Anti-neutrophil cytoplasmic antibody-associated vasculitis complicated by thrombotic microangiopathy with posterior reversible encephalopathy syndrome successfully treated with eculizumab: a case report. Mod Rheumatol Case Rep 6(2):254–259. https://doi.org/10.1093/mrcr/rxac029
Manenti L, Vaglio A, Gnappi E, Maggiore U, Allegri L, Allinovi M et al (2015) Association of serum C3 concentration and histologic signs of thrombotic microangiopathy with outcomes among patients with ANCA-associated renal vasculitis. Clin J Am Soc Nephrol 10(12):2143–2151. https://doi.org/10.2215/cjn.00120115
Acknowledgements
FGS and PRM are supported by grants from the Deutsche Forschungsgemeinschaft SFB 854 (project A01; GRK 2408, project 8) and grants ME-1365/7-2 and ME-1365/9-2.
Author information
Authors and Affiliations
Contributions
FGS and CC conceived the study. VH searched files and retrieved patient data. MJG contributed to the acquisition of patient data. CC wrote the manuscript. FGS did the statistical analysis and created the Tables and Figures. PRM read and edited the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
The trial was conducted in accordance with local laws and the internationally accepted principles of good clinical practice, which have their origin in the Declaration of Helsinki. The local ethics committee approved the study.
Informed consent
Written informed consent was obtained from each participant.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Scurt, F.G., Hirschfeld, V., Ganz, M. et al. Low levels of complement factor C3 at diagnosis can predict outcome in antineutrophil antibody associated vasculitis. J Nephrol 36, 2281–2293 (2023). https://doi.org/10.1007/s40620-023-01683-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-023-01683-z