Abstract
Background
The impact of high serum phosphorus in the general population is still debated. Studies are heterogeneous, most lack an adjustment for parathyroid hormone, vitamin D and phosphorus intake and the effect might differ by gender and renal function. We investigated the association between serum phosphorus and mortality in American adults.
Methods
We prospectively analyzed 5698 non-pregnant and non-CKD adults from the National Health and Nutrition Examination Survey (NHANES) 2003–2006. Serum phosphorus and potential confounders including parathyroid hormone, 25(OH)vitamin D and phosphorus intake were evaluated. All-cause, cardiovascular- and cancer-related deaths were recorded through December 31st, 2015. Sex-specific terciles of serum phosphorus were used to fit adjusted Cox proportional hazard models for mortality. Analysis was stratified by gender and renal function.
Results
A total of 590 deaths were recorded over a median follow-up of 81 months. Women showed higher serum phosphorus than men. The adjusted hazard ratio (HR) for all-cause mortality was 1.35 (95% CI 1.08–1.58) (p = 0.033) for the third tercile (versus second tercile). This increased risk was present in participants with estimated glomerular filtration rate (eGFR) below 90 ml/min/1.73 m2 but not above, although interaction was not significant (p = 0.12). Interaction by gender, phosphorus intake, PTH and fasting time was also not detected. For cardiovascular and cancer mortality, the adjusted HR was 0.81 (95% CI 0.33–2.00) (p = NS) and 1.45 (95% CI 0.77–2.72) (p = NS), respectively.
Conclusions
We demonstrated that the highest tercile of serum phosphorus is associated with increased all-cause mortality, irrespective of PTH, 25(OH)vitamin D or phosphorus intake. This association may differ by gender and renal function, but larger studies testing for effect modification are needed.
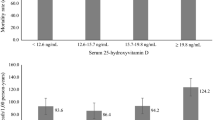
Graphic abstract




Similar content being viewed by others
Code and data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Martin KJ, González EA (2007) Metabolic bone disease in chronic kidney disease. J Am Soc Nephrol 18(3):875–885
Block GA, Klassen PS, Lazarus JM et al (2004) Mineral metabolism, mortality, and morbidity in maintenance hemodialysis. J Am Soc Nephrol 15(8):2208–2218. https://doi.org/10.1097/01.asn.0000133041.27682.a2
Da J, Xie X, Wolf M et al (2015) Serum phosphorus and progression of CKD and mortality: a meta-analysis of cohort studies. Am J Kidney Dis 66(2):258–265. https://doi.org/10.1053/j.ajkd.2015.01.009
Bellasi A, Mandreoli M, Baldrati L et al (2011) Chronic kidney disease progression and outcome according to serum phosphorus in mild-to-moderate kidney dysfunction. Clin J Am Soc Nephrol 6(4):883–891
Campos-Obando N, Lahousse L, Brusselle G et al (2018) Serum phosphate levels are related to all-cause, cardiovascular and COPD mortality in men. Eur J Epidemiol 33(9):859–871. https://doi.org/10.1007/s10654-018-0407-7
Yoo KD, Kang S, Choi Y et al (2016) Sex, age, and the association of serum phosphorus with all-cause mortality in adults with normal kidney function. Am J Kidney Dis 67(1):79–88. https://doi.org/10.1053/j.ajkd.2015.06.027
Onufrak SJ, Bellasi A, Cardarelli F et al (2009) Investigation of gender heterogeneity in the associations of serum phosphorus with incident coronary artery disease and all-cause mortality. Am J Epidemiol 169(1):67–77
Bergwitz C, Juppner H (2010) Regulation of phosphate homeostasis by PTH, vitamin D, and FGF23. Annu Rev Med 61:91–104. https://doi.org/10.1146/annurev.med.051308.111339
Yang B, Lu C, Wu Q et al (2016) Parathyroid hormone, cardiovascular and all-cause mortality: a meta-analysis. Clin Chim Acta 455:154–160. https://doi.org/10.1016/j.cca.2016.01.034
Wulaningsih W, Michaelsson K, Garmo H et al (2013) Inorganic phosphate and the risk of cancer in the Swedish AMORIS study. BMC cancer 13(1):257
Levey AS, Stevens LA, Schmid CH et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612. https://doi.org/10.7326/0003-4819-150-9-200905050-00006
Bai W, Li J, Liu J (2016) Serum phosphorus, cardiovascular and all-cause mortality in the general population: a meta-analysis. Clin Chim Acta 461:76–82. https://doi.org/10.1016/j.cca.2016.07.020
Chang WX, Xu N, Kumagai T et al (2016) The impact of normal range of serum phosphorus on the incidence of end-stage renal disease by a propensity score analysis. PLoS ONE 11(4):e0154469. https://doi.org/10.1371/journal.pone.0154469
Zhang D, Maalouf NM, Adams-Huet B et al (2014) Effects of sex and postmenopausal estrogen use on serum phosphorus levels: a cross-sectional study of the National Health and Nutrition Examination Survey (NHANES) 2003–2006. Am J Kidney Dis 63(2):198–205
Block GA (2000) Prevalence and clinical consequences of elevated Ca x P product in hemodialysis patients. Clin Nephrol 54(4):318–324
Hou Y, Li X, Sun L et al (2017) Phosphorus and mortality risk in end-stage renal disease: a meta-analysis. Clin Chim Acta 474:108–113. https://doi.org/10.1016/j.cca.2017.09.005
Caravaca F, Villa J, Garcia de Vinuesa E et al (2011) Relationship between serum phosphorus and the progression of advanced chronic kidney disease. Nefrologia 31(6):707–715. https://doi.org/10.3265/Nefrologia.pre2011.Sep.11089
Wannamethee SG, Sattar N, Papcosta O et al (2013) Alkaline phosphatase, serum phosphate, and incident cardiovascular disease and total mortality in older men. Arterioscler Thromb Vasc Biol 33(5):1070–1076. https://doi.org/10.1161/ATVBAHA.112.300826
Dominguez JR, Kestenbaum B, Chonchol M et al (2013) Relationships between serum and urine phosphorus with all-cause and cardiovascular mortality: the Osteoporotic Fractures in Men (MrOS) Study. Am J Kidney Dis 61(4):555–563. https://doi.org/10.1053/j.ajkd.2012.11.033
Larsson TE, Olauson H, Hagstrom E et al (2010) Conjoint effects of serum calcium and phosphate on risk of total, cardiovascular, and noncardiovascular mortality in the community. Arterioscler Thromb Vasc Biol 30(2):333–339. https://doi.org/10.1161/ATVBAHA.109.196675
Chang AR, Anderson C (2017) Dietary phosphorus intake and the kidney. Annu Rev Nutr 37:321–346. https://doi.org/10.1146/annurev-nutr-071816-064607
Parmar MS (2018) Phosphorus in kidney disease: culprit or bystander? Cleve Clin J Med 85(8):639–642. https://doi.org/10.3949/ccjm.85a.18013
Kawamura H, Tanaka S, Ota Y et al (2018) Dietary intake of inorganic phosphorus has a stronger influence on vascular-endothelium function than organic phosphorus. J Clin Biochem Nutr 62(2):167–173. https://doi.org/10.3164/jcbn.17-97
Chang AR, Lazo M, Appel LJ et al (2014) High dietary phosphorus intake is associated with all-cause mortality: results from NHANES III. Am J Clin Nutr 99(2):320–327. https://doi.org/10.3945/ajcn.113.073148
Chang AR, Grams ME (2014) Serum phosphorus and mortality in the Third National Health and Nutrition Examination Survey (NHANES III): effect modification by fasting. Am J Kidney Dis 64(4):567–573. https://doi.org/10.1053/j.ajkd.2014.04.028
de Boer IH, Rue TC, Kestenbaum B (2009) Serum phosphorus concentrations in the third National Health and Nutrition Examination Survey (NHANES III). Am J Kidney Dis 53(3):399–407. https://doi.org/10.1053/j.ajkd.2008.07.036
Santamaria R, Diaz-Tocados JM, Pendon-Ruiz de Mier MV et al (2018) Increased phosphaturia accelerates the decline in renal function: a search for mechanisms. Sci Rep 8(1):13701. https://doi.org/10.1038/s41598-018-32065-2
Blaine J, Chonchol M, Levi M (2015) Correction. Renal control of calcium, phosphate, and magnesium homeostasis. Clin J Am Soc Nephrol 10(10):1886–1887. https://doi.org/10.2215/cjn.08840815
Rashid G, Bernheim J, Green J et al (2007) Parathyroid hormone stimulates endothelial expression of atherosclerotic parameters through protein kinase pathways. Am J Physiol Renal Physiol 292(4):F1215–F1218. https://doi.org/10.1152/ajprenal.00406.2006
Hagstrom E, Hellman P, Larsson TE et al (2009) Plasma parathyroid hormone and the risk of cardiovascular mortality in the community. Circulation 119(21):2765–2771. https://doi.org/10.1161/circulationaha.108.808733
Gutierrez OM (2013) The connection between dietary phosphorus, cardiovascular disease, and mortality: where we stand and what we need to know. Adv Nutr 4(6):723–729. https://doi.org/10.3945/an.113.004812
Mathew S, Tustison KS, Sugatani T et al (2008) The mechanism of phosphorus as a cardiovascular risk factor in CKD. J Am Soc Nephrol 19(6):1092–1105. https://doi.org/10.1681/asn.2007070760
Camalier CE, Young MR, Bobe G et al (2010) Elevated phosphate activates N-ras and promotes cell transformation and skin tumorigenesis. Cancer Prev Res (Phila) 3(3):359–370. https://doi.org/10.1158/1940-6207.CAPR-09-0068
Kidney Disease: Improving Global Outcomes (KDIGO) CKD-MBD Work Group (2009) KDIGO clinical practice guideline for the diagnosis, evaluation, prevention, and treatment of Chronic Kidney Disease-Mineral and Bone Disorder (CKD-MBD). Kidney Int Suppl 113:S1
Wheeler DC, Winkelmayer WC (2017) KDIGO 2017 clinical practice guideline update for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD) foreword. Kidney Int Suppl 7(1):1–59
Acknowledgements
The authors thank the participants and staff of the NHANES. The authors thank João Sérgio Neves, MD, from Serviço de Endocrinologia, Diabetes e Metabolismo, Centro Hospitalar Universitário de São João, Faculdade de Medicina, Universidade do Porto (Porto, Portugal) who provided insight that greatly assisted the statistical analysis.
Funding
This work was supported through the Cardiovascular Research Center (UnIC, FCT 51/94) by the Portuguese Foundation for Science and Technology and by the project NETDIAMOND (POCI-01-0145-FEDER-016385, supported by European Structural and Investment Funds and Lisbon's Regional Operational Program 2020). Funders of this study had no role in the study design; collection, analysis, or interpretation of the data; writing of the report; or the decision to submit this report for publication.
Author information
Authors and Affiliations
Contributions
Research idea: LM. Literature search, study design, data analysis and first manuscript draft preparation: LM, FG, LP. Interpretation of the results and critical revision of the manuscript: SS, PCC, LP. Each author contributed important intellectual content during manuscript drafting or revision, accepts personal accountability for the author’s own contributions, read and approved the final manuscript and agrees to ensure that questions pertaining to the accuracy or integrity of any portion of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no relevant financial interests.
Ethics approval
NHANES protocols were approved by the National Center for Health Statistics Ethics Review Board: NHANES 2003–2004 (Protocol #98-12) and NHANES 2005–2006 (Protocol #2005-06).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mendonça, L., Gonçalves, F., Sampaio, S. et al. Association between serum phosphorus and mortality in NHANES 2003–2006: the effect of gender and renal function. J Nephrol 35, 165–178 (2022). https://doi.org/10.1007/s40620-021-00969-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-021-00969-4



