Abstract
Background
Frailty has been associated with a higher incidence of overall postoperative complications and mortality. However, the influence of frailty on the risk of venous thromboembolism (VTE) in patients with hip fracture following surgery remains unclear. We performed a meta-analysis to systematically evaluate the above association.
Methods
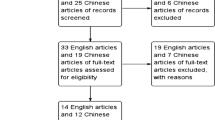
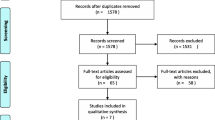
PubMed, Embase, Cochrane Library, Wanfang and CNKI were searched for relevant observational studies comparing the incidence of postoperative VTE in patients of hip fracture with and without frailty. Data collection, literature searching, and statistical analysis were conducted independently by two authors. Using a heterogeneity-incorporating random-effects model, the results were pooled.
Results
In this meta-analysis, 9509 patients from nine cohort studies were included. Pooled results showed that compared to those without frailty, patients with frailty at admission had a higher incidence of postoperative VTE (odds ratio [OR]: 2.59, 95% confidence interval [CI]: 1.25–5.39, p = 0.01; I2 = 66%). Subgroup analysis suggested the association between frailty and postoperative VTE was more remarkable in studies of patients with frailty prevalence < 50% (OR 6.28, 95% CI 3.31–11.90, p < 0.001; I2 = 8%) as compared to those ≥ 50% (OR 1.30, 95% CI 0.80–2.11, p = 0.28; I2 = 0%; p for subgroup difference < 0.001). Further meta-analyses showed that frailty at baseline was associated with a higher incidence of deep venous thrombosis (OR 3.15, 95% CI 1.33–7.47, p = 0.009; I2 = 59%), but not pulmonary embolism (OR 1.13, 95% CI 0.59–2.16, p = 0.72; I2 = 0%).
Conclusion
Frailty is associated with a higher incidence of postoperative VTE in patients with hip fracture.



Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
References
Williamson S, Landeiro F, McConnell T et al (2017) Costs of fragility hip fractures globally: a systematic review and meta-regression analysis. Osteoporos Int 28:2791–2800. https://doi.org/10.1007/s00198-017-4153-6
Griffiths R, Babu S, Dixon P et al (2021) Guideline for the management of hip fractures 2020: guideline by the Association of Anaesthetists. Anaesthesia 76:225–237. https://doi.org/10.1111/anae.15291
Veronese N, Maggi S (2018) Epidemiology and social costs of hip fracture. Injury 49:1458–1460
Bhandari M, Swiontkowski M (2017) Management of acute hip fracture. N Engl J Med 377:2053–2062. https://doi.org/10.1056/NEJMcp1611090
Sheehan KJ, Guerrero EM, Tainter D et al (2019) Prognostic factors of in-hospital complications after hip fracture surgery: a scoping review. Osteoporos Int 30:1339–1351. https://doi.org/10.1007/s00198-019-04976-x
Segon YS, Summey RD, Slawski B et al (2020) Surgical venous thromboembolism prophylaxis: clinical practice update. Hosp Pract (1995) 48:248–257. https://doi.org/10.1080/21548331.2020.1788893
MacDonald DRW, Neilly D, Schneider PS et al (2020) Venous thromboembolism in hip fracture patients: a subanalysis of the FAITH and HEALTH Trials. J Orthop Trauma 34:S70–S75. https://doi.org/10.1097/BOT.0000000000001939
Beauchamp-Chalifour P, Belzile EL, Michael R et al (2022) The risk of venous thromboembolism in surgically treated hip fracture: a retrospective cohort study of 5184 patients. Orthop Traumatol Surg Res 108:103142
Ngarmukos S, Kim KI, Wongsak S et al (2021) Asia-Pacific venous thromboembolism consensus in knee and hip arthroplasty and hip fracture surgery: Part 1. Diagnosis and risk factors. Knee Surg Relat Res 33:18. https://doi.org/10.1186/s43019-021-00099-y
Mamtora PH, Fortier MA, Barnett SR et al (2020) Peri-operative management of frailty in the orthopedic patient. J Orthop 22:304–307. https://doi.org/10.1016/j.jor.2020.05.024
Hoogendijk EO, Afilalo J, Ensrud KE et al (2019) Frailty: implications for clinical practice and public health. Lancet 394:1365–1375. https://doi.org/10.1016/S0140-6736(19)31786-6
Inoue T, Maeda K, Nagano A et al (2020) Undernutrition, sarcopenia, and frailty in fragility hip fracture: advanced strategies for improving clinical outcomes. Nutrients. https://doi.org/10.3390/nu12123743
Yan B, Sun W, Wang W et al (2022) Prognostic significance of frailty in older patients with hip fracture: a systematic review and meta-analysis. Int Orthop 46:2939–2952. https://doi.org/10.1007/s00264-022-05605-9
Ma Y, Wang A, Lou Y et al (2022) Effects of frailty on outcomes following surgery among patients with hip fractures: a systematic review and meta-analysis. Front Med (Lausanne) 9:829762. https://doi.org/10.3389/fmed.2022.829762
Page MJ, Moher D, Bossuyt PM et al (2021) PRISMA 2020 explanation and elaboration: updated guidance and exemplars for reporting systematic reviews. BMJ 372:n160. https://doi.org/10.1136/bmj.n160
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Higgins J, Thomas J, Chandler J et al (2021) Cochrane Handbook for Systematic Reviews of Interventions version 6.2. The Cochrane Collaboration. www.training.cochrane.org/handbook
Wells GA, Shea B, O'Connell D et al (2010) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558. https://doi.org/10.1002/sim.1186
Patsopoulos NA, Evangelou E, Ioannidis JP (2008) Sensitivity of between-study heterogeneity in meta-analysis: proposed metrics and empirical evaluation. Int J Epidemiol 37:1148–1157. https://doi.org/10.1093/ije/dyn065
Egger M, Davey Smith G, Schneider M et al (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Kua J, Ramason R, Rajamoney G et al (2016) Which frailty measure is a good predictor of early post-operative complications in elderly hip fracture patients? Arch Orthop Trauma Surg 136:639–647. https://doi.org/10.1007/s00402-016-2435-7
Chan S, Wong EKC, Ward SE et al (2019) The predictive value of the clinical frailty scale on discharge destination and complications in older hip fracture patients. J Orthop Trauma 33:497–502. https://doi.org/10.1097/BOT.0000000000001518
You L, Wu KQ (2020) Effect of Frality on perioperative risk and prognosis in elderly patients with hip fracture. J Nanchang Univ 8:95
Zhu SQ, Xing YH, Zhang L et al (2020) Predictive value of Frail Scale and CHS index on postoperative outcomes in elderly patients with hip fracture. J Clin Anesthesiol 36:962–965. https://doi.org/10.12089/jca.2020.10.006
Sang WA, Durrani H, Liu H et al (2021) Frailty score as a predictor of outcomes in geriatric patients with isolated hip fractures. Am Surg. https://doi.org/10.1177/00031348211058629
Chen ZF, Yu XH, Zhao B (2022) Risk factor of postoperative lower exemity deep venous thrombosis in geriatric hip fracture patients. J Clin Emerg 23:237–241. https://doi.org/10.13201/j.issn.1009-5918.2022.04.003
Hao XY, Ouyang CL, Xu ZY et al (2022) Clinical application of modified frailty index in predicting complications after hip fracture in the elderly. Chin J Mult Organ Dis Elderly 21:481. https://doi.org/10.11915/j.issn.1671-5403.2022.07.104
Tram MK, O’Connor CM, Qian AS et al (2022) Frailty is associated with increased 30-day adverse events and hospitalization costs after primary total hip arthroplasty. J Arthroplasty 37:S925–S930.e4
Zhou Y, Wang L, Cao A et al (2022) Modified frailty index combined with a prognostic nutritional index for predicting postoperative complications of hip fracture surgery in elderly. J Invest Surg 35:1739–1746. https://doi.org/10.1080/08941939.2022.2101166
Song Y, Wu Z, Huo H et al (2022) The impact of frailty on adverse outcomes in geriatric hip fracture patients: a systematic review and meta-analysis. Front Public Health 10:890652. https://doi.org/10.3389/fpubh.2022.890652
Folsom AR, Boland LL, Cushman M et al (2007) Frailty and risk of venous thromboembolism in older adults. J Gerontol A Biol Sci Med Sci 62:79–82
Lutsey PL, Windham BG, Misialek JR et al (2020) Long-term association of venous thromboembolism with frailty, physical functioning, and quality of life: the atherosclerosis risk in communities study. J Am Heart Assoc 9:e015656. https://doi.org/10.1161/JAHA.119.015656
Ebrahimian S, Lee C, Tran Z et al (2022) Association of frailty with outcomes of resection for colonic volvulus: a national analysis. PLoS ONE 17:e0276917. https://doi.org/10.1371/journal.pone.0276917
Phan K, Kim JS, Lee NJ et al (2017) Frailty is associated with morbidity in adults undergoing elective anterior lumbar interbody fusion (ALIF) surgery. Spine J 17:538–544
Putthapiban P, Vutthikraivit W, Rattanawong P et al (2020) Association of frailty with all-cause mortality and bleeding among elderly patients with acute myocardial infarction: a systematic review and meta-analysis. J Geriatr Cardiol 17:270–278. https://doi.org/10.11909/j.issn.1671-5411.2020.05.006
Proietti M, Romiti GF, Raparelli V et al (2022) Frailty prevalence and impact on outcomes in patients with atrial fibrillation: a systematic review and meta-analysis of 1,187,000 patients. Ageing Res Rev 79:101652
Yoon JY, Kim S, Chang JS et al (2020) Venous thromboembolism after delayed surgery for a hip fracture: a retrospective cohort study. Geriatr Gerontol Int 20:1151–1156. https://doi.org/10.1111/ggi.14055
Imamura K, Yamamoto S, Suzuki Y et al (2023) Comparison of the association between six different frailty scales and clinical events in patients on hemodialysis. Nephrol Dial Transplant 38:455–462. https://doi.org/10.1093/ndt/gfac047
Sukkriang N, Punsawad C (2020) Comparison of geriatric assessment tools for frailty among community elderly. Heliyon 6:e04797. https://doi.org/10.1016/j.heliyon.2020.e04797
Baldawi M, Awad ME, McKelvey G et al (2023) Neuraxial anesthesia significantly reduces 30-day venous thromboembolism rate and length of hospital stay in primary total hip arthroplasty: a stratified propensity score-matched cohort analysis. J Arthroplasty 38:108–116
Wang X, Jiang Z, Li Y et al (2022) Prevalence of preoperative Deep Venous Thrombosis (DVT) following elderly intertrochanteric fractures and development of a risk prediction model. BMC Musculoskelet Disord 23:417. https://doi.org/10.1186/s12891-022-05381-y
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Contributions
HZ, FW, and BL conceived the study. HZ and FW performed a database search, literature identification, quality evaluation, and data extraction, HZ, JS, YL, ZZ, and XW performed statistical analyses and interpreted the data. HZ and FW drafted the manuscript. BL critically revised the manuscript. All authors approved the submission.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval and consent to participate
Not applicable.
Statement of human and animal rights
This study does not contain any studies with human or animals performed by any of the authors.
Informed consent
For this type of study, consent is not required.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, H., Wu, F., Sun, J. et al. The impact of frailty evaluation on the risk of venous thromboembolism in patients with hip fracture following surgery: a meta-analysis. Aging Clin Exp Res 35, 2413–2423 (2023). https://doi.org/10.1007/s40520-023-02529-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-023-02529-1