Abstract
Purpose
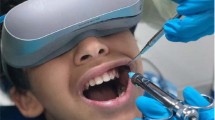
Pediatric dentistry requires more than routine dental knowledge and skills in executing quality dental care. The quality of dental treatment is indirectly proportional to a child’s anxiety and fear. The recent distraction technique, the use of virtual reality (VR) devices has intrigued many researcher’s minds. Therefore, this study was conducted to assess the clinical feasibility and effectiveness of the VR device in reducing pain and anxiety in pediatric patients during mandibular primary molar extraction.
Methods
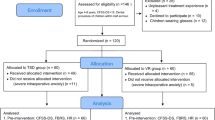
This research trial had 30 healthy children between the ages of 6 and 12 who required mandibular primary molar extraction. The subjects were divided into two groups using a simple randomization method. In the study group (n = 15), extraction was carried out using a VR device, whereas, in the control group (n = 15), extraction was carried out without the use of a VR device. Pre- and post-extraction anxiety levels were measured by Venham’s picture test (VPT) and the heart rate. After the procedure, pain and behavior were evaluated by the Wong-Bakers Faces pain rating scale (WBS) and FLACC Scale respectively.
Results
The pre-extraction values of the VPT and heart rate showed no statistically significant difference. This indicates that participants of both groups had a similar level of anxiety at baseline. There was a statistically significant increase (p = 0.028) between pre- and post-heart rates in the control group, with no significant change in the study group.
Conclusion
The use of a virtual reality device in children can reduce anxiety during primary molar extractions as evaluated by heart rate. Virtual reality devices might be an adjunct to high-quality dental care and to other behavior management methods. Definitive outcomes can be attained by encouraging studies overcoming the present limitations, and considering salivary biochemical indicators for the assessment of these devices.







Similar content being viewed by others
Data availability
Data used and analyzed in this study are available with the corresponding author and can be provided when needed.
References
Agarwal N, Dhawan J, Kumar D, Anand A, et al. Effectiveness of two topical anaesthetic agents used along with audio visual aids in paediatric dental patients. J Clin Diagn Res. 2017;21(1):80–3. https://doi.org/10.7860/JCDR/2017/23180.9217.
Aitken RC. Measurement of feelings using visual analogue scales. Proc R Soc Med. 1969;62(10):989–93.
American academy of pediatric dentistry. Behavior guidance for the pediatric dental patient the reference manual of pediatric dentistry chicago. Amer Acad Ped Dent. 2021;22:306–24.
Armfield JM, Spencer AJ, Stewart JF. Dental fear in Australia: who’s afraid of the dentist? Aust Dent J. 2006;51(1):78–85. https://doi.org/10.1111/j.1834-7819.2006.tb00405.x.
Asl Aminabadi N, Erfanparast L, Sohrabi A, Ghertasi Oskouei S, Naghili A. the impact of virtual reality distraction on pain and anxiety during dental treatment in 4–6-year-old children: a randomized controlled clinical trial. J Dent Res Dent Clin Dent Prosp. 2012;6(4):117–24. https://doi.org/10.5681/joddd.2012.025.
Asvanund Y, Mitrakul K, Juhong RO, Arunakul M. Effect of audio-visual eyeglasses during local anesthesia injections in 5- to 8-year-old children. Quintessence Int. 2015;46(6):513–21. https://doi.org/10.3290/j.qi.a33932.
Atzori B, Lauro Grotto R, Giugni A, Calabrò M, Alhalabi W, Hoffman HG. Virtual reality analgesia for pediatric dental patients. Front Psychol. 2018;23(9):2265. https://doi.org/10.3389/fpsyg.2018.02265.
Bansal A, Jain S, Tyagi P, Jain A. The effect of virtual reality headset using smartphone device on pain and anxiety levels during local anesthetic injection in children with 6–10 years of age paripex Indian. J Res. 2018;7(6):2250–1991.
Beck FM, Weaver JM. Blood pressure and heart rate responses to anticipated high-stress dental treatment. J Dent Res. 1981;60(1):26–9. https://doi.org/10.1177/00220345810600010501.
Buchanan H, Niven N. Validation of a Facial Image Scale to assess child dental anxiety. Int J Paediatr Dent. 2002;12(1):47–52. https://doi.org/10.1046/j.0960-7439.2001.00322.x.
Cunningham A, McPolin O, Fallis R, Coyle C, Best P, McKenna G. A systematic review of the use of virtual reality or dental smartphone applications as interventions for the management of paediatric dental anxiety. BMC Oral Health. 2021;21(1):244. https://doi.org/10.1186/s12903-021-01602-3.
Dahlquist LM, Weiss KE, Law EF, et al. Effects of videogame distraction and a virtual reality type head-mounted display helmet on cold pressor pain in young elementary school-aged children. J Pediatr Psychol. 2010;35(6):617–25. https://doi.org/10.1093/jpepsy/jsp082.
Dak-Albab R, Al-Monaqel MB, Koshha R, Shakhashero H, Soudan R. A comparison between the effectiveness of vibration with Dental vibe and benzocaine gel in relieving pain associated with mandibular injection: a randomized clinical trial. Anaesth Pain Int Care. 2016;20(1):43–9.
Florella M, Sarale C, Ram RD. Audio-visual iatrosedation with video eyeglasses distraction method in pediatric dentistry: A case history. J Int Dent Med Res. 2010;3:133–6.
Folayan MO, Kolawole KA. A critical appraisal of the use of tools for assessing dental fear in children. Afr J Oral Health. 2004;1:54–63. https://doi.org/10.4314/ajoh.v1i1.31306.
Garra G, Singer AJ, Taira BR, Chohan J, et al. Validation of the wong-baker faces pain rating scale in pediatric emergency department patients. Acad Emerg Med. 2010;17(1):50–4. https://doi.org/10.1111/j.1553-2712.2009.00620.x.
Hmud R, Walsh LJ. Dental anxiety: causes, complications, and management approaches. Int Dent. 2007;9(5):6–16.
Lahmann C, Schoen R, Henningsen P, Ronel J, et al. Brief relaxation versus music distraction in the treatment of dental anxiety: A randomized controlled clinical trial. J Am Dent Assoc. 2008;139:317–24. https://doi.org/10.14219/Jada.archive.2008.0161.
Larry LV, Elise GK. Interval rating scales for children’s dental anxiety and uncooperative behavior. Pediatr Dent. 1980;2:195–202.
Mccarthy FM. A clinical study of blood pressure responses to epinephrine-containing local anesthetic solutions. J Dent Res. 1957;36(1):132–41.
McCaul KD, Malott JM. Distraction and coping with pain. Psychol Bull. 1984;95(3):516–33. https://doi.org/10.1037/0033-2909.95.3.516.
Mcelroy CM. 1895 dentistry for children. Calif Dent Assoc Trans. 1895;85:556.
Merkel S, Voepel-Lewis T, Malviya S. Pain assessment in infants and young children: the FLACC scale. Am J Nurs. 2002;102(10):55–8. https://doi.org/10.1097/00000446-200210000-00024.
Messer JG. Stress in dental patients undergoing routine procedures. J Dent Res. 1977;56(4):362–7.
Panda A. Effect of virtual reality distraction on pain perception during dental treatment in children. Int J Oral Care Res. 2017;5(3):1–4. https://doi.org/10.5005/jp-journals-10051-0115.
Polit, D.F. and Beck, C.T. (2008) Nursing Research: Generating and Assessing Evidence for Nursing Practice. 8th Edition, Wolters Kluwer Health/Lippincott Williams & Wilkins, Philadelphia. 796
Prabhakar AR, Marwah N, Raju OS. A comparison between audio and audio-visual distraction techniques in managing anxious pediatric dental patients. J Indian Soc Pedod Prev Dent. 2007;25(4):177–82. https://doi.org/10.4103/0970-4388.37014.
Ram D, Shapira J, Holan G, Magora F, Cohen S, Davidovich E. Audiovisual video eyeglass distraction during dental treatment in children. Quintessence Int. 2010;41(8):673–9.
Riba H, Al-Zahrani S, Al-Buqmi N, Al-JundiA,. A review of behavior evaluation scales in pediatric dentistry and suggested modification to the frankl scale. EC Dental Sci. 2017;16:269–75.
Sharar SR, Miller W, Teeley A, et al. Applications of virtual reality for pain management in burn-injured patients. Expert Rev Neuro. 2008;8(11):1667–74. https://doi.org/10.1586/14737175.8.11.1667.
Slifer KJ, Tucker CL, Dahlquist LM. Helping children and caregivers cope with repeated invasive procedures: how are we doing? J Clin Psychol Med Set. 2002;9:131–52. https://doi.org/10.1023/A:1014944110697.
Sullivan C, Schneider PE, Musselman RJ, Dummett CO Jr, Gardiner D. The effect of virtual reality during dental treatment on child anxiety and behavior. ASDC J Dent Child. 2000;67(3):193–161.
Tailor B, Bargale S, Dave BH, Deshpande A. comparison of virtual reality glasses vs on-screen distraction technique in reduction of pediatric dental anxiety: an in vivo study. J South Asian Assoc Pediatr Dent. 2021;4(1):22–6.
Wismeijer AA, Vingerhoets AJ. The use of virtual reality and audiovisual eyeglass systems as adjunct analgesic techniques: a review of the literature. Ann Behav Med. 2005;30(3):268–78. https://doi.org/10.1207/s15324796abm3003_11.
Acknowledgements
I would like to thank the Faculty and staff of Bharati Dental College and Hospital Pune, Maharashtra, India.
Author information
Authors and Affiliations
Contributions
PDP, LSL, are Concepts, LSL in Design, ARP in Definition of intellectual content, PDP, LSL, in Literature search, PDP, Clinical studies, LSL in Experimental studies, KVP, in Data acquisition, PPS in Data analysis, PDP, LSL, in Manuscript preparation, ARP, in Manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pathak, P.D., Lakade, L.S., Patil, K.V. et al. Clinical evaluation of feasibility and effectiveness using a virtual reality device during local anesthesia and extractions in pediatric patients. Eur Arch Paediatr Dent 24, 379–386 (2023). https://doi.org/10.1007/s40368-023-00801-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-023-00801-6