Abstract
Introduction
During sleep there is reduction of blood pressure (BP) caused by a decrease of the sympathetic nervous tone. This nocturnal “dipping” phenomenon, assessable with ambulatory blood pressure monitoring (ABPM), is blunted with increasing age.
Aim
To assess the effect of hospitalization on night-time BP fall in old-elderly patients.
Methods
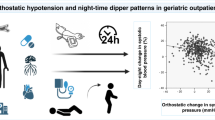
We analysed 78 ABPM of old-elderly hospitalized patients (mean age 91 ± 0.5 years) and those of 18 outpatients as control group. The nocturnal BP fall was assessed calculating: the dipping value (DV) i.e. the difference between mean diurnal systolic BP (mDSBP) and mean nocturnal systolic BP (mNSBP) and the “dipping pattern” i.e. mNSBP/mDSBPx100.
Results
Hospitalized patients showed a lower rate of normal dipping patterns (9 vs. 39%), an higher rate of reverse dippers (59 vs. 28%; p < 0.05) and a lower DV (−0.9 ± 1 vs. 9 ± 4 mmHg; p < 0.05) than patients of control group. At multivariate regression analysis including age, gender and hospitalization, DV was significantly correlated only with the hospitalization (β −0.3, t −2.9; p < 0.05).
Conclusions
In old-elderly hospitalized patients nocturnal BP fall is abolished. This enhancement of the age related reduction of nocturnal BP dipping may be due to the stress associated with hospital environment.
Similar content being viewed by others
References
O’Brien E, Sheridan J, O’Malley K. Dippers and non-dippers. Lancet. 1988;2:397.
Parati G, Stergiou G, O’Brien E, Asmar R, Beilin L, Bilo G, et al. European Society of Hypertension practice guidelines for ambulatory blood pressure monitoring. J Hypertens. 2014;32:1359–66.
Somers VK, Dyken ME, Mark AL, Abboud FM. Sympathetic-nerve activity during sleep in normal subjects. N Engl J Med. 1993;328:303–7.
Millar-Craig MW, Bishop CN, Raftery EB. Circadian variation of blood-pressure. Lancet. 1978;1:795–7.
Ohkubo T, Hozawa A, Yamaguchi J, Kikuya M, Ohmori K, Michimata M, et al. Prognostic significance of the nocturnal decline in blood pressure in individuals with and without high 24-h blood pressure: the Ohasama study. J Hypertens. 2002;20:2183–9.
Salles GF, Reboldi G, Fagard RH, Cardoso CR, Pierdomenico SD, Verdecchia P, et al. Prognostic effect of the nocturnal blood pressure fall in hypertensive patients: the ambulatory blood pressure collaboration in patients with hypertension (ABC-H) meta-analysis. Hypertension. 2016;67:693–700.
Staessen JA, Bieniaszewski L, O’Brien E, Gosse P, Hayashi H, Imai Y, et al. Nocturnal blood pressure fall on ambulatory monitoring in a large international database. The “Ad Hoc” Working Group. Hypertension. 1997;29:30–9.
O’Sullivan C, Duggan J, Atkins N, O’Brien E. Twenty-four-hour ambulatory blood pressure in community-dwelling elderly men and women, aged 60–102 years. J Hypertens. 2003;21:1641–7.
O’Brien E, Parati G, Stergiou G, Asmar R, Beilin L, Bilo G, et al. European Society of Hypertension position paper on ambulatory blood pressure monitoring. J Hypertens. 2013;31:1731–68.
O’Brien E. Twenty-four-hour ambulatory blood pressure measurement in clinical practice and research: a critical review of a technique in need of implementation. J Intern Med. 2011;269:478–95.
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Böhm M, et al. 2013 Practice guidelines for the management of arterial hypertension of the European Society of Hypertension (ESH) and the European Society of Cardiology (ESC): ESH/ESC Task Force for the Management of Arterial Hypertension. J Hypertens. 2013;31:1925–38.
Bertinieri G, Grassi G, Rossi P, Meloni A, Ciampa M, Annoni G, et al. 24-hour blood pressure profile in centenarians. J Hypertens. 2002;20:1765–9.
Fagard R, Grassi G. Blood pressure response to acute physical and mental stress. In: Mancia G, Grassi G, Kjeldsen SE, editors. Manual of Hypertension of the European Society of Hypertension. London: UK Informa Healthcare; 2008. p. 184–9.
van den Meiracker AH, Man in ‘t Veld AJ, van Eck HJ, Wenting GJ, Schalekamp MA. Determinants of short-term blood pressure variability. Effect of bed rest and sensory deprivation in essential hypertension. Am J Hypertens. 1988;1:22–6.
Prince PN, Vitiello MV, Raskind MA, Thorpy MJ. Geriatrics: sleep disorders and aging. N Engl J Med. 1990;323:520–6.
Christensen M. Noise levels in a general intensive care unit: a descriptive study. Nurs Crit Care. 2007;12:188–97.
Flaherty JH. Insomnia among hospitalized older persons. Clin Geriatr Med. 2008;24:51–67.
Buxton OM, Ellenbogen JM, Wang W, Carballeira A, O’Connor S, Cooper D, et al. Sleep disruption due to hospital noises: a prospective evaluation. Ann Intern Med. 2012;157:170–9.
Hinderliter AL, Routledge FS, Blumenthal JA, Koch G, Hussey MA, Wohlgemuth WK, Sherwood A. Reproducibility of blood pressure dipping: relation day-to-day variability in sleep quality. J Am Soc Hypertens. 2013;7:432–9.
Grassi G, Seravalle G, Quarti-Trevano F, Dell’Oro R, Bombelli M, Cuspidi C, et al. Adrenergic, metabolic, and reflex abnormalities in reverse and extreme dipper hypertensives. Hypertension. 2008;52:925–31.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval and informed consent
This article refers to retrospective analysis of ABPMs recorded with the informed consent of patients.
Rights and permissions
About this article
Cite this article
Salvo, F., Lonati, C., Berardi, M. et al. Nocturnal Blood Pressure Dipping is Abolished in Old-Elderly Hospitalized Patients. High Blood Press Cardiovasc Prev 24, 413–417 (2017). https://doi.org/10.1007/s40292-017-0224-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-017-0224-1