Abstract
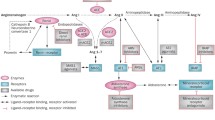
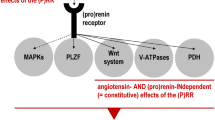
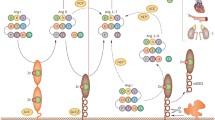
Hypertension is one of the major risk factor able to promote development and progression of several cardiovascular diseases, including left ventricular hypertrophy and dysfunction, myocardial infarction, stroke, and congestive heart failure. Also, it is one of the major driven of high cardiovascular risk profile in patients with metabolic complications, including obesity, metabolic syndrome and diabetes, as well as in those with renal disease. Thus, effective control of hypertension is a key factor for any preventing strategy aimed at reducing the burden of hypertension-related cardiovascular diseases in the clinical practice. Among various regulatory and contra-regulatory systems involved in the pathogenesis of cardiovascular and renal diseases, renin-angiotensin system (RAS) plays a major role. However, despite the identification of renin and the availability of various assays for measuring its plasma activity, the specific pathophysiological role of RAS has not yet fully characterized. In the last years, however, several notions on the RAS have been improved by the results of large, randomized clinical trials, performed in different clinical settings and in different populations treated with RAS inhibiting drugs, including angiotensin converting enzyme (ACE) inhibitors and antagonists of the AT1 receptor for angiotensin II (ARBs). These findings suggest that the RAS should be considered to have a central role in the pathogenesis of different cardiovascular diseases, for both therapeutic and preventive purposes, without having to measure its level of activation in each patient. The present document will discuss the most critical issues of the pathogenesis of different cardiovascular diseases with a specific focus on RAS blocking agents, including ACE inhibitors and ARBs, in the light of the most recent evidence supporting the use of these drugs in the clinical management of hypertension and hypertension-related cardiovascular diseases.


Similar content being viewed by others
References
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Bohm M, et al. 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2013;34(28):2159–219.
Volpe M, Rosei EA, Ambrosioni E, Cottone S, Cuspidi C, Borghi C, et al. 2012 consensus document of the Italian Society of Hypertension (SIIA): strategies to improve blood pressure control in Italy: from global cardiovascular risk stratification to combination therapy. High Blood Press Cardiovasc Prev. 2013;20(1):45–52.
Angeli F, Angeli E, Cavallini C, Ambrosio G, Mazzotta G, Reboldi G, et al. Electrocardiographic abnormalities of left ventricular repolarization: prognostic implications in hypertensive post-menopausal women. Maturitas. 2010;67(2):159–65.
Task Force on the management of STseamiotESoC, Steg PG, James SK, Atar D, Badano LP, Blomstrom-Lundqvist C, et al. ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur Heart J. 2012;33(20):2569–619.
Task Force M, Montalescot G, Sechtem U, Achenbach S, Andreotti F, Arden C, et al. 2013 ESC guidelines on the management of stable coronary artery disease: the Task Force on the management of stable coronary artery disease of the European Society of Cardiology. Eur Heart J. 2013;34(38):2949–3003.
Ackerman MJ, Priori SG, Willems S, Berul C, Brugada R, Calkins H, et al. HRS/EHRA expert consensus statement on the state of genetic testing for the channelopathies and cardiomyopathies this document was developed as a partnership between the Heart Rhythm Society (HRS) and the European Heart Rhythm Association (EHRA). Heart Rhythm. 2011;8(8):1308–39.
Mosterd A, Hoes AW. Clinical epidemiology of heart failure. Heart. 2007;93(9):1137–46.
McMurray JJ, Adamopoulos S, Anker SD, Auricchio A, Bohm M, Dickstein K, et al. ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2012;33(14):1787–847.
Hamada K, Taniguchi Y, Shimamura Y, Inoue K, Ogata K, Ishihara M, et al. Serum level of soluble (pro)renin receptor is modulated in chronic kidney disease. Clin Exp Nephrol. 2013;17(6):848–56.
Batenburg WW, Danser AH. (Pro)renin and its receptors: pathophysiological implications. Clin Sci (Lond). 2012;123(3):121–33.
Sim MK. Des-aspartate-angiotensin I, a novel angiotensin AT(1) receptor drug. Eur J Pharmacol. 2015;5(760):36–41.
Lorenz JN. Chymase: the other ACE? Am J Physiol Ren Physiol. 2010;298(1):F35–6.
Romero CA, Orias M, Weir MR. Novel RAAS agonists and antagonists: clinical applications and controversies. Nat Rev Endocrinol. 2015;11(4):242–52.
Dzau VJ. Tissue renin-angiotensin system in myocardial hypertrophy and failure. Arch Intern Med. 1993;153(8):937–42.
Capuano F, Rossi F. Farmaci del sistema cardiovascolare del sangue e del rene. In: Medica EM, editor. Farmacologia: principi di base e applicazioni terapeutiche; 2011.
Ferrao FM, Lara LS, Lowe J. Renin-angiotensin system in the kidney: what is new? World J Nephrol. 2014;3(3):64–76.
Etelvino GM, Peluso AA, Santos RA. New components of the renin-angiotensin system: alamandine and the MAS-related G protein-coupled receptor D. Curr Hypertens Rep. 2014;16(6):433.
von Lueder TG, Atar D, Krum H. Current role of neprilysin inhibitors in hypertension and heart failure. Pharmacol Ther. 2014;144(1):41–9.
Gu J, Noe A, Chandra P, Al-Fayoumi S, Ligueros-Saylan M, Sarangapani R, et al. Pharmacokinetics and pharmacodynamics of LCZ696, a novel dual-acting angiotensin receptor-neprilysin inhibitor (ARNi). J Clin Pharmacol. 2010;50(4):401–14.
Shliakhto EV, Konradi AO, Moiseeva OM. Molecular, genetic, and cellular aspects of the heart and vessel remodeling in hypertension (review). Ter Arkh. 2004;76(6):51–8.
Sankaranarayanan K, Chakraborty R, Boerwinkle EA. Ionizing radiation and genetic risks. VI. Chronic multifactorial diseases: a review of epidemiological and genetical aspects of coronary heart disease, essential hypertension and diabetes mellitus. Mutat Res. 1999;436(1):21–57.
Williams RR, Dadone MM, Hunt SC, Jorde LB, Hopkins PN, Smith JB, et al. The genetic epidemiology of hypertension: a review of past studies and current results for 948 persons in 48 Utah pedigrees. Prog Clin Biol Res. 1984;147:419–42.
Schlager G. Spontaneous hypertension in laboratory animals. A review of the genetic implications. J Hered. 1972;63(1):35–8.
Andreadis EA, Angelopoulos ET, Kolyvas GN, Agaliotis GD, Mousoulis CG, Mousoulis GP. The effect of aliskiren versus ramipril-based treatment on the Ambulatory Arterial Stiffness Index in hypertensive patients. Int Angiol. 2014;33(1):78–83.
Ohsawa M, Tamura K, Kanaoka T, Wakui H, Maeda A, Dejima T, et al. Addition of aliskiren to Angiotensin receptor blocker improves ambulatory blood pressure profile and cardiorenal function better than addition of benazepril in chronic kidney disease. Int J Mol Sci. 2013;14(8):15361–75.
Kanaoka T, Tamura K, Ohsawa M, Wakui H, Maeda A, Dejima T, et al. Effects of aliskiren-based therapy on ambulatory blood pressure profile, central hemodynamics, and arterial stiffness in nondiabetic mild to moderate hypertensive patients. J Clin Hypertens (Greenwich). 2012;14(8):522–9.
Agenzia Italiana per il Famraco (AIFA). Rapporto dell’Osservatorio sull’impiego dei Medicinali (OsMed) 2014. Uso dei Farmaci in Italia. 2015 [cited 2015 August, 20]. http://www.agenziafarmaco.gov.it/it/content/luso-dei-farmaci-italia-rapporto-osmed-2014.
Weir MR, Yadao AM, Purkayastha D, Charney AN. Effects of high- and low-sodium diets on ambulatory blood pressure in patients with hypertension receiving aliskiren. J Cardiovasc Pharmacol Ther. 2010;15(4):356–63.
Chen Y, Meng L, Shao H, Yu F. Aliskiren vs. other antihypertensive drugs in the treatment of hypertension: a meta-analysis. Hypertens Res. 2013;36(3):252–61.
Harel Z, Gilbert C, Wald R, Bell C, Perl J, Juurlink D, et al. The effect of combination treatment with aliskiren and blockers of the renin-angiotensin system on hyperkalaemia and acute kidney injury: systematic review and meta-analysis. BMJ. 2012;344:e42.
Nickenig G, Ostergren J, Struijker-Boudier H. Clinical evidence for the cardiovascular benefits of angiotensin receptor blockers. J Renin Angiotensin Aldosterone Syst. 2006;7(Suppl 1):S1–7.
Zhenfeng Z, Huilan S, Junya J, Dong L, Shan L. A systematic review and meta-analysis of aliskiren and angiotension receptor blockers in the management of essential hypertension. J Renin Angiotensin Aldosterone Syst. 2011;12(2):102–12.
Strauss MH, Hall AS. Angiotensin receptor blockers may increase risk of myocardial infarction: unraveling the ARB-MI paradox. Circulation. 2006;114(8):838–54.
Bangalore S, Kumar S, Wetterslev J, Messerli FH. Angiotensin receptor blockers and risk of myocardial infarction: meta-analyses and trial sequential analyses of 147,020 patients from randomised trials. BMJ. 2011;342:d2234.
Epstein BJ, Gums JG. Angiotensin receptor blockers versus ACE inhibitors: prevention of death and myocardial infarction in high-risk populations. Ann Pharmacother. 2005;39(3):470–80.
Tsuyuki RT, McDonald MA. Angiotensin receptor blockers do not increase risk of myocardial infarction. Circulation. 2006;114(8):855–60.
Volpe M, Tocci G, Trimarco B, Mancia G. Angiotensin II receptor blockers and risk of myocardial infarction: a meta-analysis of randomized clinical trials updated until May 1, 2008. High Blood Press Cardiovasc Prev. 2008;15(3):171–215.
Investigators O, Yusuf S, Teo KK, Pogue J, Dyal L, Copland I, et al. Telmisartan, ramipril, or both in patients at high risk for vascular events. N Engl J Med. 2008;358(15):1547–59.
Swedberg K, Held P, Kjekshus J, Rasmussen K, Ryden L, Wedel H. Effects of the early administration of enalapril on mortality in patients with acute myocardial infarction. Results of the Cooperative New Scandinavian Enalapril Survival Study II (CONSENSUS II). N Engl J Med. 1992;327(10):678–84.
The CONSENSUS Trial Study Group. Effects of enalapril on mortality in severe congestive heart failure. Results of the Cooperative North Scandinavian Enalapril Survival Study (CONSENSUS). N Engl J Med. 1987;316(23):1429–35.
The SOLVD Investigators. Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med. 1991;325(5):293–302.
Vantrimpont P, Rouleau JL, Wun CC, Ciampi A, Klein M, Sussex B, et al. Additive beneficial effects of beta-blockers to angiotensin-converting enzyme inhibitors in the Survival and Ventricular Enlargement (SAVE) Study. SAVE Investigators. J Am Coll Cardiol. 1997;29(2):229–36.
Pfeffer MA, Swedberg K, Granger CB, Held P, McMurray JJ, Michelson EL, et al. Effects of candesartan on mortality and morbidity in patients with chronic heart failure: the CHARM-Overall programme. Lancet. 2003;362(9386):759–66.
Cohn JN, Tognoni G. A randomized trial of the angiotensin-receptor blocker valsartan in chronic heart failure. N Engl J Med. 2001;345(23):1667–75.
Pitt B, Poole-Wilson PA, Segal R, Martinez FA, Dickstein K, Camm AJ, et al. Effect of losartan compared with captopril on mortality in patients with symptomatic heart failure: randomised trial–the Losartan Heart Failure Survival Study ELITE II. Lancet. 2000;355(9215):1582–7.
Pitt B, Segal R, Martinez FA, Meurers G, Cowley AJ, Thomas I, et al. Randomised trial of losartan versus captopril in patients over 65 with heart failure (Evaluation of Losartan in the Elderly Study, ELITE). Lancet. 1997;349(9054):747–52.
Pfeffer MA, McMurray JJ, Velazquez EJ, Rouleau JL, Kober L, Maggioni AP, et al. Valsartan, captopril, or both in myocardial infarction complicated by heart failure, left ventricular dysfunction, or both. N Engl J Med. 2003;349(20):1893–906.
The SOLVD Investigattors. Effect of enalapril on mortality and the development of heart failure in asymptomatic patients with reduced left ventricular ejection fractions. N Engl J Med. 1992;327(10):685–91.
Dahlof B, Devereux RB, Kjeldsen SE, Julius S, Beevers G, de Faire U, et al. Cardiovascular morbidity and mortality in the Losartan Intervention For Endpoint reduction in hypertension study (LIFE): a randomised trial against atenolol. Lancet. 2002;359(9311):995–1003.
Castro Hevia J, Antzelevitch C, Tornes Barzaga F, Dorantes Sanchez M, Dorticos Balea F, Zayas Molina R, et al. Tpeak-Tend and Tpeak-Tend dispersion as risk factors for ventricular tachycardia/ventricular fibrillation in patients with the Brugada syndrome. J Am Coll Cardiol. 2006;47(9):1828–34.
Haller H, Ito S, Izzo JL Jr, Januszewicz A, Katayama S, Menne J, et al. Olmesartan for the delay or prevention of microalbuminuria in type 2 diabetes. N Engl J Med. 2011;364(10):907–17.
Schneider MP, Hua TA, Bohm M, Wachtell K, Kjeldsen SE, Schmieder RE. Prevention of atrial fibrillation by renin-angiotensin system inhibition a meta-analysis. J Am Coll Cardiol. 2010;55(21):2299–307.
Wolk R, Mazurek T, Lusawa T, Wasek W, Rezler J. Left ventricular hypertrophy increases transepicardial dispersion of repolarisation in hypertensive patients: a differential effect on QTpeak and QTend dispersion. Eur J Clin Invest. 2001;31(7):563–9.
Corrao G, Parodi A, Zambon A, Heiman F, Filippi A, Cricelli C, et al. Reduced discontinuation of antihypertensive treatment by two-drug combination as first step. Evidence from daily life practice. J Hypertens. 2010;28(7):1584–90.
Corrao G, Zambon A, Parodi A, Poluzzi E, Baldi I, Merlino L, et al. Discontinuation of and changes in drug therapy for hypertension among newly-treated patients: a population-based study in Italy. J Hypertens. 2008;26(4):819–24.
Mancia G, Parodi A, Merlino L, Corrao G. Heterogeneity in antihypertensive treatment discontinuation between drugs belonging to the same class. J Hypertens. 2011;29(5):1012–8.
Wolk R, Stec S, Kulakowski P. Extrasystolic beats affect transmural electrical dispersion during programmed electrical stimulation. Eur J Clin Invest. 2001;31(4):293–301.
Zhao X, Xie Z, Chu Y, Yang L, Xu W, Yang X, et al. Association between Tp-e/QT ratio and prognosis in patients undergoing primary percutaneous coronary intervention for ST-segment elevation myocardial infarction. Clin Cardiol. 2012;35(9):559–64.
Sauer A, Wilcox JE, Andrei AC, Passman R, Goldberger JJ, Shah SJ. Diastolic electromechanical coupling: association of the ECG T-peak to T-end interval with echocardiographic markers of diastolic dysfunction. Circ Arrhythm Electrophysiol. 2012;5(3):537–43.
Passino C, Magagna A, Conforti F, Buralli S, Kozakova M, Palombo C, et al. Ventricular repolarization is prolonged in nondipper hypertensive patients: role of left ventricular hypertrophy and autonomic dysfunction. J Hypertens. 2003;21(2):445–51.
Acknowledgments
The Authors wish to thank Mrs Daniela Cimmaruta and Mrs Annalisa Capuano for their help and assistance in preparing the English version of this consensus document.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
C. Borghi: On behalf of the SIIA Task Force.
F. Rossi: On behalf of the SIF Task Force.
The list of the members of the SIIA and SIF Task Force are given in “Appendix”.
Appendix
Appendix
Members of the SIIA Task Force: Enrico Agabiti Rosei (Brescia), Nicola De Luca (Napoli), GiovanBattista Desideri (L’Aquila), Giuseppe Mancia (Milan), Paolo Pauletto (Padova), Gianfranco Parati (Milan), Roberto Pontremoli (Genova), Giuseppe Schillaci (Chieti), Michele Stornello (Siracusa). Giuliano Tocci (Rome), Franco Veglio (Torino), Agostino Virdis (Pisa), Massimo Volpe (Rome).
Members of the SIF Task Force: Pier Luigi Canonico (Novara), Giuseppe Cirino (Napoli), Salvatore Cuzzocrea (Messina), Romano Danesi (Pisa), Monica Di Luca (Milano), Giorgio Cantelli Forti (Bologna), Armando Genazzani (Torino), Giovan Battista Leproux (Roma), Luca Steardo (Roma).
Scientific Advisor: Prof. Bruno Trimarco, President of the Italian Society of Cardiovascular Prevention (SIPREC), Hypertension Research Center, and Department of Advanced Biomedical Sciences, Federico II University, Naples, Italy.
Rights and permissions
About this article
Cite this article
Borghi, C., SIIA Task Force., Rossi, F. et al. Role of the Renin-Angiotensin-Aldosterone System and Its Pharmacological Inhibitors in Cardiovascular Diseases: Complex and Critical Issues. High Blood Press Cardiovasc Prev 22, 429–444 (2015). https://doi.org/10.1007/s40292-015-0120-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-015-0120-5