Abstract
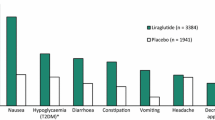
Globally, obesity has reached epidemic proportions and poses an ever increasing burden from a societal and healthpayer perspective. Although lifestyle interventions are fundamental in its management, in the real world setting most obese or overweight adults require adjunctive pharmacotherapy to achieve clinically relevant reductions in bodyweight (i.e. a ≥5 % reduction). Subcutaneous liraglutide (Saxenda®) 3 mg once daily is indicated as an adjunct to a reduced-calorie diet and increased physical activity for chronic bodyweight management in adults with an initial body mass index (BMI) of ≥30 kg/m2 (obese) or a BMI of ≥27 kg/m2 (overweight) and at least one bodyweight-related comorbidity [e.g. hypertension, dyslipidaemia, type 2 diabetes mellitus or obstructive sleep apnoea (OSA)]. In phase III trials (32 or 56 weeks’ duration) in these populations, subcutaneous liraglutide was associated with clinically relevant reductions in fasting bodyweight and was generally well tolerated. Liraglutide was significantly more effective than placebo in terms of reductions in fasting bodyweight and waist circumference, and improvements in some biomarkers of cardiovascular risk. Improvements in bodyweight were maintained after up 2 years of liraglutide therapy. In nondiabetic adults with moderate to severe OSA, liraglutide improved apnoea-hypopnoea index scores at 32 weeks, which was largely driven by significant reductions in bodyweight. In the absence of head-to-head trials, the relative position of individual anti-obesity drugs remains to be fully determined. In the meantime, liraglutide is an emerging option, as an adjunct to a reduced-calorie diet and increased physical activity, for chronic bodyweight management in obese adults and overweight adults with at least one bodyweight-related comorbidity.

Similar content being viewed by others
References
World Health Organization. Obesity and overweight: fact sheet no. 311. 2014. http://www.who.int/mediacentre/factsheets/fs311/en/. Accessed 22 Jan 2015.
Guh DP, Zhang W, Bansback N, et al. The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health. 2009;9:88.
Angulo P. Nonalcoholic fatty liver disease. N Engl J Med. 2002;346(16):1221–31.
Bray GA. Why do we need drugs to treat the patient with obesity? Obesity. 2013;21(5):893–9.
Collaboration Lancet Prospective Studies, Whitlock G, Lewington S, et al. Body-mass index and cause-specific mortality in 900,000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009;373:1083–96.
Jensen MD, Ryan DH, Apovian CM, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults. J Am Coll Cardiol. 2014;63(25 Pt B):2985–3023.
Wright F, Boyle S, Baxter K, et al. Understanding the relationship between weight loss, emotional well-being and health-related quality of life in patients attending a specialist obesity weight management service. J Health Psychol. 2013;18(4):574–86.
Kuna ST, Reboussin DM, Borradaile KE, et al. Long-term effect of weight loss on obstructive sleep apnea severity in obese patients with type 2 diabetes. Sleep. 2013;36(5):641–9.
Ebbert JO, Elrashidi MY, Jensen MD. Managing overweight and obesity in adults to reduce cardiovascular disease risk. Curr Atheroscler Rep. 2014;16:445.
National Institute for Health and Care Excellence. Obesity: identification, assessment and management of overweight and obesity in children, young people and adults. Partial update of CG43. 2014. http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0071374/. Accessed 20 Feb 2014.
Muscogiuri G, Cignarelli A, Giorgino F, et al. GLP-1: benefits beyond pancreas. J Endocrinol Invest. 2014;37:1143–53.
Holst JJ. Incretin hormones and the satiation signal. Int J Obesity. 2013;37:1161–8.
Madsbad S. The role of glucagon-like peptide-1 impairment in obesity and potential therapuetic implications. Diabetes Obes Metab. 2014;16(1):9–21.
Iepsen EW, Torekov SS, Holst JJ. Therapies for inter-relating diabetes and obesity: GLP-1 and obesity. Expert Opin Pharmacother. 2014;15(17):2487–500.
Ørskov C, Poulsen SS, Moller M, et al. Glucagon-like peptide 1 receptors in the subfornical organ and the area postrema are accessible to circulating glucagon-like peptide 1. Diabetes. 1996;45(6):832–5.
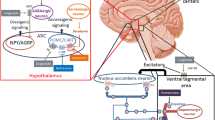
Secher A, Jelsing J, Baquero AF, et al. The arcuate nucleus mediates GLP-1 receptor agonist liraglutide-dependent weight loss. J Clin Invest. 2014;124(10):4473–88.
Scott LJ. Liraglutide: a review of its use in patients with type 2 diabetes mellitus. Drugs. 2014;74(18):2161–74.
Novo Nordisk. Saxenda® liragluitde (rDNA) injection: US prescribing information. 2014. http://www.saxenda.com/. Accessed 21 Jan 2014.
Pyke C, Heller RS, Kirk RK, et al. GLP-1 localization in monkey and human tissue: novel distribution revealed with extensively validated monoclonal antibody. Endocrinology. 2014;155(4):1280–90.
Horowitz M, Flint A, Jones KL, et al. Effect of the once-daily human GLP-1 analogue liraglutide on appetite, energy intake, energy expenditure and gastric emptying in type 2 diabetes. Diabetes Res Clin Pract. 2012;97(2):258–66.
Van Can J, Sloth B, Jensen CB, et al. Effects of the once-daily GLP-1 analog liraglutide on gastric emptying, glycemic parameters, appetite and energy metabolism in obese, non-diabetic adults. Int J Obes. 2014;38(6):784–93.
Inoue K, Maeda N, Kashine S, et al. Short-term effects of liraglutide on visceral fat adiposity, appetite, and food preference: a pilot study of obese Japanese patients with type 2 diabetes. Cardiovasc Diabetol. 2011;10:109.
Fujishima Y, Maeda N, Inoue K, et al. Efficacy of liraglutide, a glucagon-like peptide-1 (GLP-1) analogue, on body weight, eating behavior, and glycemic control, in Japanese obese type 2 diabetes. Cardiovasc Diabetol. 2012;11:107.
Jendle J, Nauck MA, Matthews DR, et al. Weight loss with liraglutide, a once-daily human glucagon-like peptide-1 analogue for type 2 diabetes treatment as monotherapy or added to metformin, is primarily as a result of a reduction in fat tissue. Antimicrob Agents Chemother. 2009;11(12):1163–72.
Li CJ, Yu Q, Yu P, et al. Changes in liraglutide-induced body composition are related to modifications in plasma cardiac natriuretic peptides levels in obese type 2 diabetic patients. Cardiovasc Diabetol. 2014;13:36.
European Medicines Agency. Saxenda: summary of product characteristics. 2015. http://ec.europa.eu/health/documents/community-register/html/h992.htm#EndOfPage. Accessed 26 Mar 2015.
Astrup A, Rössner S, Van Gaal L, et al. Effects of liraglutide in the treatment of obesity: a randomised, double- blind, placebo-controlled study. Lancet. 2009;374(9701):1606–16.
Wadden TA, Hollander P, Klein S, et al. Weight maintenance and additional weight loss with liraglutide after low-calorie-diet-induced weight loss: the SCALE Maintenance randomized study. Int J Obes. 2013;37(11):1443–51.
Pi-Sunyer FX, Astrup A, Fujioka K, et al. Liraglutide 3.0 mg reduces the prevalence of prediabetes and delays onset of type 2 diabetes in overweight and obese adults: results from Scale Obesity and Prediabetes, a randomized, double-blind and placebo-controlled 56-week trial [abstract no. SAT-0925]. Endocr Rev. 2014;35(3 Suppl).
DeFronzo R, Bergenstal R, Bode B, et al. Effect of liraglutide 3.0 mg cessation on efficacy and safety/tolerability after 56 weeks’ treatment in obese/overweight adults with type 2 diabetes: SCALE Diabetes [abstract no. 76]. Diabetologia. 2014;57(1 Suppl 1):S38–9.
Wilding JPH, Astrup A, Fujioka K, et al. Efficacy and safety of liraglutide 3.0 mg for weight management in overweight and obese adults: the SCALE Obesity and Prediabetes, a randomised, double-blind and placebo-controlled trial [abstract no. T4:RS2.3]. Obes Facts. 2014;7(Suppl 1):15.
Wilding J, Astrup A, Fujioka K, et al. Liraglutide 3.0 mg improves insulin secretion and action in overweight and obese adults without diabetes: results from Scale Obesity and Prediabetes, a randomized, double-blind and placebo-controlled 56-week trial [abstract no. SAT-0931]. Endocr Rev. 2014;35(3 Suppl).
Pi-Sunyer X, Fujioka K, Le Roux C, et al. Liraglutide 3.0 mg reduces the prevalence of prediabetes and delays onset of type 2 diabetes in overweight/obese adults: the SCALE Obesity and Prediabetes trial [abstract no. 73]. Diabetologia. 2014;57(1 Suppl 1):S37.
Wilding J, Astrup A, Fujioka K, et al. In overweight and obese adults, liraglutide 3.0 mg reduces the prevalence of pre-diabetes and delays the onset of type 2 diabetes: SCALE obesity and pre-diabetes trial [abstract no. P134]. Diabet Med. 2015;32(Suppl 1):71.
Bode B, DeFronzo R, Bergenstal R, et al. Effect of liraglutide 3.0/1.8 mg on body weight and cardiometabolic risk factors in overweight/obese adults with type 2 diabetes: SCALE Diabetes randomised, double-blind, 56-week trial [abstract no. 181]. Diabetologia. 2014;57(1 Suppl 1):S83.
Novo Nordisk. FDA briefing document NDA 206321: liraglutide injection, 3 mg. 2014. http://www.fda.gov. Accessed 28 Jan 2014.
Blackman A, Foster G, Zammit G, et al. Liraglutide 3.0 mg reduces severity of obstructive sleep apnoea and body weight in obese individuals with moderate or severe disease: SCALE Sleep Apnoea trial [abstract no. 184]. Diabetologia. 2014;57(1 Suppl 1):S85.
Astrup A, Carraro R, Finer N, et al. Safety, tolerability and sustained weight loss over 2 years with the once-daily human GLP-1 analog, liraglutide. Int J Obes. 2012;36(6):843–54.
Klein S, Allison DB, Heymsfield SB, et al. Waist circumference and cardiometabolic risk. A consensus statement for shaping America’s health: Association for Weight Management and Obesity Prevention; NAASO, the Obesity Society; the American Society for Nutrition; and the American Diabetes Association. Diabetes Care. 2007;30(6):1647–52.
Davies MJ, Bergenstal R, Bode B, et al. Liraglutide 3.0 mg for weight management in obese/overweight adults with type 2 diabetes: SCALE Diabetes 56-week randomised, double-blind, placebo-controlled trial [abstract no. 39]. Diabetologia. 2014(1 Suppl 1):S22–S3.
Le Roux C, Lau DCW, Astrup A, et al. Safety and tolerability of liraglutide 3.0 mg in overweight and obese adults: the SCALE obesity and prediabetes randomised trial [abstract no. 833]. Diabetologia. 2014;57(1 Suppl 1):S338.
Hegedus L, Moses AC, Zdravkovic M, et al. GLP-1 and calcitonin concentration in humans: lack of evidence of calcitonin release from sequential screening in over 5000 subjects with type 2 diabetes or nondiabetic obese subjects treated with the human GLP-1 analog, liraglutide. J Clin Endocrinol Metab. 2011;96(3):853–60.
Health News Network. Health Canada approves Saxenda® (liraglutide) for the treatment of chronic weight management. 2015. http://www.chrgonline.com. Accessed 20 Mar 2015.
Barja-Fernandez S, Leis R, Casanueva FF, et al. Drug devlopment strategies for the treatment of obesity: how to ensure efficacy, safety, and sustainable weight loss. Drug Design Dev Therapy. 2014;8:2391–400.
FDA. FDA approves weight-management drug Contrave. 2014. http://www.fda.gov. Accessed 20 Mar 2015.
European Medicines Agency. Mysimba 8 mg/90 mg prolonged release tablets: summary of product characteristics. 2015. http://www.ema.europa.eu. Accessed 20 Apr 2015.
Egan AG, Blind E, Dunder K, et al. Pancreatic safety and incretin-based drugs: FDA and EMA assessment. N Engl J Med. 2014;370(9):794–7.
Arena Pharmaceuticals GmbH. Belviq (lorcaserin hydrochloride) tablets, for oral use: US prescribing information. 2012. https://www.belviq.com/. Accessed 16 Feb 2015.
Vivus Inc. Qsymia (phentermine and topiramate extended-release) capsules, for oral use: US prescribing information. 2014. http://qsymia.com/. Accessed 16 Feb 2015.
Orexigen Therapeutics Inc. Contrave (naltrexone HCl and bupropion HCl) extended-release tablets: US prescribing information. 2014. http://www.orexigen.com. Accessed 23 Mar 2015.
FDA. Part 15: Confidentiality of interim results in cardiovacular outcome safety trials. 2014. http://www.fda.gov. Accessed 20 Mar 2015.
Disclosure
The preparation of this review was not supported by any external funding. During the peer review process, the manufacturer of the agent under review was offered an opportunity to comment on this article. Changes resulting from comments received were made by the author on the basis of scientific and editorial merit. Lesley Scott is a salaried employee of Adis/Springer.
Author information
Authors and Affiliations
Corresponding author
Additional information
The manuscript was reviewed by: M. C. Mancini, Sao Paulo University, Endocrinology and Metabology Service, Obesity and Metabolic Syndrome Group, Sao Paulo, Brazil; J. L. Pérez-Castrillón, Rio Hortega University Hospital, University of Valladolid, Institute of Endocrinology and Nutrition, Valladolid, Spain; T. Tzotzas, Agios Pavlos General Hospital, Thessaloniki, Greece; W. M. Valencia, Geriatrics Research, Education and Clinical Center (GRECC) and Endocrine Section, Miami VA Medical Center, Miami, FL, USA.
Rights and permissions
About this article
Cite this article
Scott, L.J. Liraglutide: A Review of Its Use in the Management of Obesity. Drugs 75, 899–910 (2015). https://doi.org/10.1007/s40265-015-0408-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40265-015-0408-8