Abstract
Assessment of the integrity of the articular cartilage is considered key for the early diagnosis of osteoarthritis (OA). Diffusion-weighted imaging and diffusion tensor imaging have potential as biomarkers for cartilage composition and structure. The value of diffusion to detect compositional and structural changes in the cartilage matrix has been shown in ex vivo experiments for several years. However, it was not until recently that the first clinical studies have been performed. These clinical studies demonstrated the potential of diffusion to detect cartilage damage after injury, to early diagnose OA, and to measure cartilage remodeling after cartilage repair surgery. In this review, we provide a comprehensive overview of the literature on diffusion measurements on cartilage from ex vivo validation to its most recent clinical applications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Magnetic resonance imaging (MRI) has shown great potential in the assessment of cartilage composition and structure in vivo and non-invasively. Assessment of cartilage composition and structure is important in many joint diseases like osteoarthritis (OA). Since articular cartilage is very early involved in OA, assessment of cartilage integrity is key for the early diagnosis of OA and for the validation of new disease-modifying OA drugs.
Most quantitative MRI biomarkers for articular cartilage, aimed at assessing the biochemical composition of articular cartilage, focus on proteoglycan (PG) content: sodium (Na)-imaging [1, 2], delayed gadolinium-enhanced MRI of the cartilage, dGEMRIC [3, 4], T 1ρ relaxation time [5, 6], and glycosaminoglycan chemical exchange-dependent saturation transfer (gagCEST) [7]. However, existing MRI biomarkers do not provide convincing assessment of collagen, with the T 2 relaxation time [8, 9] and magnetization transfer, MT, [10–12] partially sensitive to the collagen. Both T 2 and MT depend on the water and PG content of cartilage matrix [11, 13]. In this review, we will focus on diffusion-weighted imaging (DWI) and diffusion tensor imaging (DTI) as biomarkers to assess the integrity of the cartilage matrix with the potential to provide assessment of PG and collagen.
Diffusion measurements with MRI are a unique technique to probe tissue microstructure at scales of a few microns, which is the relevant scale of tissue organization (e.g., chondrocyte size is ~10 μm, collagen fibril diameter is up to 0.2 μm, with a separation separation ~0.1–3 μm) [14, 15]. Even more important, diffusion measurements can provide separate information of collagen and PG [16]. The collagen network is organized in an arch-like architecture and favors the motion of water along the collagen fibrils inducing anisotropy in the motion of the water, so any measurement of diffusion anisotropy is a measurement of the collagen integrity [16–21]. PG molecules, on the other hand, do not show a preferred orientation and therefore restrict the motion of water molecules equally in all directions and can be detected by the mean vale of diffusion [22–24].
There is also a strong biological motivation to study the diffusion properties of articular cartilage. Since articular cartilage is avascular, molecular diffusion is the dominant mechanism of the transport of small-size nutrients to the chondrocytes and the removal of their metabolic waste products [25, 26]. Even more, the unique viscoelastic mechanical properties of articular cartilage are a consequence of the motion of water through the low permeable cartilage matrix [27]. When a compressive force is applied to the cartilage surface, the low permeable solid matrix induce high frictional drag forces on the fluid component causing a rapid increase in hydraulic pressure. This hydraulic pressure is an efficient mechanism of load support that protects the solid matrix of the cartilage from mechanical stress. During OA, the molecular breakdown of the cartilage matrix causes an increase in its water permeability, which significantly affects its mechanical properties [14].
In this review, we focus on clinical applications of diffusion measurements of articular cartilage. First, we briefly describe how diffusion measurements are performed with MRI. We provide a succinct overview of the result of ex vivo validation of diffusion measurements in the articular cartilage. Than, we review the applications of diffusion imaging to assess cartilage changes after knee injury, to early diagnose OA, and to measure cartilage remodeling after cartilage repair surgery. After each section, we indicate open research questions with important clinical implications that still need to be investigated.
The Measurement of Diffusion with MRI
DWI measures the diffusion constant in a tissue along one direction. DWI requires the application of two gradients separated in time to produce a position-dependent de-phasing and re-phasing of the MRI signal. Water molecules that move between the first and second gradients will not be re-phased thus leading to a decay of the MRI signal. The signal loss due to diffusion follows the well-known exponential decay law,
where S(b) is the signal intensity at a single voxel at the diffusion-weighting b, the so-called b value. The b-value summarizes the contribution of the diffusion-sensitizing gradients to the diffusion-weighting of the MR signal: the gyromagnetic ratio, γ, the strength of the applied gradient, \(\vec{g},\) the time between the diffusion gradients (diffusion time), Δ, and the duration of the diffusion-sensitizing gradient, δ. ADC, is the apparent diffusion coefficient. The term apparent is used to remember that the diffusion constant measured is an effective diffusion constant which depends both on tissue structure and on sequence parameters (e.g., the diffusion time, diffusion direction, etc.).
DWI allows the calculation of a single ADC value along the direction of the diffusion-sensitizing gradients, \(\vec{g}.\) For homogeneous and isotropic mediums (e.g., solutions), ADC is the same in all directions. However, in many biological tissues, like the articular cartilage, the values of ADC depend on the direction. In this case, a diffusion tensor formalism is required to describe the diffusion properties of the tissue.Footnote 1 The diffusion tensor is represented by a symmetric 3 × 3 matrix, i.e. by six independent diffusion constants. To calculate the diffusion tensor, we need to measure the ADC along at least six different diffusion directions.
Since the measured components of the diffusion tensor depends on the slice orientation and the patient position in the magnet, it is customary to report quantities derived from the diffusion components that are orientation-independent. To this end, the diffusion tensor is diagonalized and the eigenvectors, \(\{ \vec{e}_{1} ,\;\vec{e}_{2} ,\;\vec{e}_{3} \} ,\) and their corresponding eigenvalues, {λ 1, λ 2, λ 3}, are calculated. From the eigenvalues, several rotational invariant quantities can be defined [28]. By far the most commonly used are the mean diffusivity (MD) and the fractional anisotropy (FA),
Diffusion Measurements of Articular Cartilage Ex Vivo
The first diffusion measurements in articular cartilage using MRI were performed by Burstein et al. [23]. In their seminal work, spectroscopic measurement of the diffusivity of small solutes (water, Na+, Li+ and \({\text{CF}}_{3} {\text{CO}}_{2}^{ - }\)) in healthy calf cartilage were performed at different diffusion times. Interestingly, the ADC of all these small solutes was the same (~60 % of their values in solution) independently of their charge, indicating the low influence of the fixed charge of the PGs in their diffusivities. Burstein et al. [23] also investigated the change in diffusion properties by selective removal of the glycosaminoglycans (GAG) side chains of the PG with trypsin. Progressive PG depletion resulted in an increase in the diffusion coefficient of water up to 20 %. The change in ADC correlated with the sodium (Na) concentration measured in the articular cartilage.
DWI and DTI of Intact and Artificially Degraded Cartilage
The effect of artificial cartilage degradation on ADC has been investigated by several groups using different methods to degrade the cartilage matrix [29–32, 33••]. Most of the studies degraded the GAG side chains of the PG, as a model of early cartilage degradation occurring in OA. All these studies systematically reported increases of ADC between 5 and 30 % depending of the total amount of GAGs cleaved [29–32, 33••].
Measurements of DTI on cartilage samples after PG depletion resulted in increased MD but no change in the FA [17, 18, 20]. These experiments provided the first evidence that FA is dependent on the collagen architecture of the cartilage matrix. In a study with different degrees of PG extraction, we observed an increase of MD that correlated with PG loss, and no change in FA or the collagen matrix (as measured with polarized light microscopy, PLM) [20].
The hypothesis that the collagen network is responsible for the diffusion anisotropy in cartilage was further supported by the observation that the orientation of the first eigenvector corresponds with the expected zonal arrangement of the collagen matrix in articular cartilage [16]. To better understand the origin of the diffusion anisotropy in articular cartilage, de Visser et al. [19] investigated the correlation between the orientation of the first eigenvector measured with DTI and collagen orientation measured with PLM. From a total of five samples, three showed a good quantitative correlation with PLM and two showed only qualitative similarity. Raya et al. [21] found an excellent correlation between the orientation of the first eigenvector with the zonal arrangement of the collagen [radial (P < 0.01, r 2 = 0.89), transitional (P < 0.01, r 2 = 0.87) and tangential (r 2 = 0.11)] as measured with scanning electron microscopy.
DWI as a Biomarker for the Mechanical Properties of Articular Cartilage
Juráš et al. [34] analyzed the change in several MRI parameters (T 1, T 2, and ADC) before and after compression (15 % strain) and found a 11.5 % decrease in diffusion from 0.96 ± 0.40 × 10−3 to 0.85 ± 0.39 × 10−3 mm2/s. In a subsequent study, Juráš et al. [35] found a positive correlation between the ADC and the equilibrium modulus (r = −0.52) and the relaxation time (r = −0.73). More recently, Aoki et al. [36•] reported significant correlations in porcine knee joints between the ADC in articular cartilage and the viscoelasticity (r 2 = 0.69, P < 0.01) and mechanical relaxation time (r 2 = 0.75, P < 0.01).
Two studies by Greene et al. [37, 38] have analyzed the dynamical change of the ADC under compression. They found evidence that the axial porosity during loading can play an important role in redirecting the flow of the interstitial fluid to the articular surface, thus providing an additional mechanism for cartilage lubrication.
The effect of cartilage compression in DTI parameters has been investigated by de Visser et al. [39]. In this study, they reported increased FA in the 15 % most superficial cartilage and decrease in MD in the 30 % most superficial cartilage (strain up to 30 %). Similar results were observed by Raya et al. [21, 40]. High resolution DTI can provide accurate new information that can be used to validate new models of cartilage biomechanics [41].
Ability of Diffusion to Diagnose Cartilage Damage Ex Vivo
Lin et al. [32, 33••] investigated the value of a multiparametric MR imaging approach to classify samples of nasal bovine cartilage as intact or degraded after mild (6 h) and extensive (24 h) trypsin treatment. Lin et al. [32, 33••] measured the MT ratio, ADC, and T 1 and T 2 relaxation times. T 1 was the single best predictor of cartilage followed closely by the ADC [area under the curve of 0.97 (T 1) and 0.97 (diffusion) for extensive degradation and 0.60 (T 1) and 0.58 (diffusion) for mild degradation] [33••].
Mlynárik et al. [42] investigated the potential of different MRI parameters (including dGEMRIC, T 2, and ADC) to detect cartilage damage in samples obtained from seven patients undergoing knee replacement surgery. ADC was correlated with 14 histological slices (2 per donor) with signs of OA. Increased ADC was found in 10 slices (1.15–1.60 × 10−3 mm2/s) as compared with areas of intact cartilage (0.75–1.20 × 10−3 mm2/s). In four slices, the ADC showed values of intact cartilage (0.85–1.25 × 10−3 mm2/s).
The value of DTI to detect early cartilage degeneration has been quantified ex vivo in samples with early cartilage damage [43•]. Cartilage damage was assessed in safranin O histology slides with the histology OARSI score, which ranges from 0 (healthy) to 6 (bone eburnation). The study included 43 samples which had evidence of early cartilage damage: OARSI grades 0 (n = 14), 1 (n = 11), 2 (n = 12), and 3–4 (n = 6). MD maps of OARSI >0 samples showed increased MD (+25 %) in the superficial cartilage extending deeper with increasing OARSI scores. Reduction of FA (~−35 %) was also observed in OARSI >0 samples (Fig. 1). DTI showed excellent performance in the detection of cartilage damage (accuracy = 95 %; 41 of 43 samples) and good performance in the grading of cartilage damage (accuracy = 74 %; 32 of 43 samples).
Maps of λ l = λ 1, λ t = (λ 1 + λ 2)/2, MD and FA from samples of all OARSI grade groups. Histologic images show progressive cartilage damage from the articular surface to the bone–cartilage interface. The OARSI grade 1 sample shows signs of superficial fibrillation and reduced staining on the articular surface, as compared with the OARSI grade 0 sample. The OARSI 2 sample shows focal discontinuity of the superficial cartilage and chondrocyte clustering in the cartilage surface. The OARSI 3–4 sample shows increased fibrillation with clefts extending to the midcartilage region. This is evidence of cell proliferation adjacent to the fissures and inhomogeneous staining. Maps of λ l, λ t, and MD show a clear trend of increasing values in conjunction with increasing OARSI grade. In contrast, FA had a slight trend of decreasing values in conjunction with increasing OARSI grade (adapted from [43•], with permission)
DWI of Cartilage Repair
Majdišová et al. [44] investigated the correlation between histology and ADC in a model of cartilage repair. Cartilage repair tissue was scanned at 3 T at 5 and 8 weeks after implantation and subsequently analyzed with histology. ADC in cartilage repair decreased from 1.37 ± 0.05 × 10−3 mm2/s at 5 weeks to 1.16 ± 0.22 × 10−3 mm2/s at 8 weeks and was higher than normal adjacent cartilage 0.85 ± 0.05 × 10−3 mm2/s.
Open Questions for Research
The relationship between the mechanical properties and the diffusion measurements still needs further studies that include more realistic models of the cartilage mechanical properties (e.g., biphasic models) and also correlation with tensile and shear properties of the cartilage. The value of diffusion to differentiate fibro-cartilage from hyaline-like cartilage is an interesting question with important clinical applications that still needs to be addressed.
Clinical Applications of Diffusion of Articular Cartilage
Diffusion measurements of articular cartilage are challenging to perform in vivo because of the high resolution needed (<1 mm) and the characteristic low T 2 of articular cartilage (~30 ms). These technical challenges explain the almost 15 year gap between the first paper showing the potential of diffusion-weighted MRI and the first clinical studies on humans.
Feasibility Studies of DWI and DTI of Articular Cartilage
To the best of our knowledge, Gold et al. [45] were the first to report the ADC of articular cartilage measured in vivo in 1998 (Table 1). Gold et al. used an interleaved circular diffusion-weighted echo planar imaging (EPI) sequence using 2D spiral for echo navigation. In this first report the interleave EPI sequence showed acceptable image quality, although resolution (1.3 × 1.7 mm2 in-plane) was still insufficient for cartilage imaging.
Miller et al. [46] used a 3D diffusion-weighted steady state free precession (SSFP) sequence with a 2D navigator to measure diffusion in vivo. SSFP have the advantage of having high SNR and relative short acquisition times (4:40 min per diffusion-weighted image). The drawback of these sequences is that the diffusion quantification is challenging, since it involves knowledge of T 1 and the real flip angle [46–48]. Assuming a uniform T 1 value of 800 ms, the diffusion measured in cartilage was 1.6 × 10−3 mm2/s. However, the diffusion in the synovial fluid varied between 4 to 6 × 10−3 mm2/s, which is higher than the ADC of free water at body temperature, 3 × 10−3 mm2/s. This values are likely due to the assumption of a very short T 1 values in the synovial fluid (i.e. T 1 of 800 ms instead of 3,620 ms [49]). Overestimation of diffusivity in the synovial fluid can be problematic in OA patients with cartilage fibrillation and subsequent infiltration of the synovial fluid in the cartilage matrix.
Different groups have tried to improve the performance of the 3D SSFP sequences by using a 3D double echo steady state (DESS) sequence. Staroswiecki et al. [50] used a combination of 3D DESS images acquired with different repetition and echo times, flip angles and diffusion to calculate T 1, T 2, and ADC. Although the idea of quantifying these parameters with only two acquisitions (two times 6:13 min) is very appealing, the measured ADC showed poor precision with standard deviations up to 40 % for typical cartilage values (T 2 = 20–40 ms and D = 1–1.5 × 10−3 mm2/s). This precision is low to detect the expected 20 % changes in diffusivity with cartilage degradation.
Bieri et al. [51••, 52] proposed to use a 3D DESS sequence in the fast acquisition regime (TR ≪ T 2) with low flip angles, which results in improved SNR and T 2 independence of the signal (Fig. 2). With this technique, the measured ADC on the articular cartilage increased from 1.0 at the bone–cartilage interface to 1.7 × 10−3 mm2/s at the articular surface (Table 1). The ADC in the synovial fluid was 2.6 × 10−3 mm2/s [51••, 52].
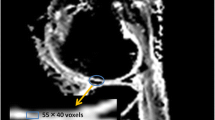
Left in vivo axial nondiffusion and DW-SSFP-echo scans (TE/TR = 15 ms, flip angle = 14°, slice thickness = 3 mm, 16 slices, field of view ([FOV] = 160 × 160 mm2, in-plane resolution = 0.5 × 0.5 mm2, effective b value = 140 s/mm2, three directions, acquisition time per direction = 4:00 min) of in vivo cartilage in the knee joint of a patient after matrix-associated autologous cartilage transplantation. Right quantitative T 1 (top) and diffusion (bottom) imaging show an increase in both T 1 and T 1-corrected diffusion constants for the repair tissue as compared to the control cartilage (adapted from [52], with permission)
Two studies used an EPI sequence to image healthy volunteers. Azuma et al. [53] investigated DTI of articular cartilage in the femoral trochlea of five volunteers. Volunteers were scanned twice, after 10 min standing and after 60 min resting. After resting, a slightly increase in MD in the 10 % of the most superficial cartilage (data interpolation was used) and no change in FA was observed. Zhu et al. [54] imaged the patellar cartilage of 30 healthy subjects. However, in this study, EPI images had insufficient quality with evident geometric distortion, and signs of N/2 ghosting.
Diffusion Measurements of Articular Cartilage After Knee Injury
Due to the low permeability of the cartilage matrix [14], the application of a sudden (1–10 ms), strong compressive force (pressure >14 MPa) causes an abrupt increase in the pore pressure with devastating consequences to the integrity of the cartilage matrix. Ex vivo experiments have shown PG loss, disruption of the collagen network, and cell death by necrosis as a result of compressive overloading of the cartilage matrix [55–58]. After injury, chondrocyte apoptosis occurs with overexpression of matrix-degrading enzymes, which further impels the matrix breakdown [58]. Human studies on ACL rupture patients have shown a high concentration of collagen and PG fragments in the synovial fluid just hours after injury, which decreases with time from the injury but remains increased for years as compared to asymptomatic volunteers [59–61]. Synovial fluids of ACL patients also contains traces of PG synthesis [60]. Histological analysis of ACL rupture patients showed evidence of degeneration of type II collagen while there is a transient increase in the total PG content [62].
Xu et al. [63•] provided first in vivo evidence that diffusion has the potential for the diagnosis of early cartilage degeneration after knee injury. This study included 30 asymptomatic controls and 42 subjects with cartilage injury, which were scanned using a diffusion-weighted EPI sequence (resolution 0.71 × 1.25 mm2). Inclusion criteria were pain in the medial or lateral compartment, a positive McMurray sign and an injury not older than 30 days at the time of MRI (type of injury was not reported). Ten of the 42 subjects with cartilage injury were excluded since they showed significant abnormal cartilage in clinical sequences (T 1-, T 2-, and proton density-weighted). Xu et al. [63•] found significant increases (between 26 and 30 %) in ADC (from 1.44 to 1.80 s/mm2; Table 1). In this study, the images acquired with the EPI sequence showed limited image quality with signs of image distortion.
DTI can provide additional information to ADC. Figure 3 shows an example of DTI acquired in both knees of a 30-year-old subject after ACL rupture using a radial spin-echo DTI (RAISED) sequence.
MD and FA maps of both knees of a 30-year-old male subject after ACL rupture (top ACL ruptured knee, bottom contralateral knee). Imaging was acquired 4 weeks after injury with a radial spin-echo diffusion tensor imaging sequence (RAISED) on a 3 T scanner (TE/TR = 39/1,500 ms, slice thickness = 3 mm, field of view = 154 × 154 mm2, in-plane resolution = 0.74 × 0.74 mm2, b value = 300 s/mm2, six directions, acquisition time per diffusion-weighted image = 2:50 min). Notice the increase in MD and the slightly reduction in FA in the injured knee
Open Questions for Research
The value of diffusion measurements to detect cartilage damage as a consequence of an acute injury has not been investigated. Since mechanical injury affects both the collagen and PG components of the matrix, DTI measurements provide an additional advantage over other imaging biomarkers that only assess one component of the matrix. This is important, since studies have shown that cartilage can partially recover from the PG loss but not from the collagen damage.
Diffusion Measurements in OA
Articular cartilage is one of the first tissues involved in the pathologic process of OA. Cartilage degradation during OA involve loss of the GAGs side chains of the PG [64]. GAGs are responsible for the swelling pressure, and its cleavage results in an abnormal loading of the collagen network [65]. Degradation of PG is followed by proteolysis of the non-collagenous proteins, which cross-bind collagen fibers. This causes loosening of the collagen architecture and swelling of the cartilage matrix [64, 66]. Ultimately, collagen disruption occurs, initiating the cascade of events leading to the loss of the cartilage matrix [67]. Detection of collagen integrity is desired to stage OA and identify patients at risk of progression.
Raya et al. [68••] performed the first in vivo study with healthy and OA subjects using a line scan DTI (LSDTI), which is an extension of the line scan diffusion imaging (LSDI) sequence proposed by Gubdjartsson et al. [69]. The patellar cartilage of 10 OA subjects and 16 healthy controls was scanned at 7 T (Fig. 4). OA subjects had significantly increased MD (+29 %) and showed significantly lesser FA (−26 %) as compared with the healthy controls (Table 1). The ability of each MR imaging parameter to help discriminate healthy subjects from subjects with OA was assessed by using receiver operating characteristic curve (ROC) analysis. For MD, a specificity of 100 % and a sensitivity of 80 % were achieved with an optimal threshold of 1.2 × 10−3 mm2/s. For FA, an optimal threshold of 0.25 led to a specificity of 88 % and sensitivity of 80 %. In the same study, the reproducibility of DTI parameters in 10 healthy controls was calculated for MD (8.1 %) and FA (9.7 %).
Patellar cartilage high-spatial-resolution morphologic MR images and MR imaging parameter maps (MD and FA) in a healthy volunteer (top row 31-year-old man, right knee) and two subjects with OA (patient 1: 60-year-old woman, Kellgren–Lawrence grade of 3, right knee; patient 2: 64-year-old man, Kellgren–Lawrence grade of 2, left knee). FLASH fast low-angle shot (adapted [68••], with permission)
Raya et al. [70] extended the study to include all knee compartments with the LSDTI sequence. In spite of the low number of included subjects (10 healthy controls and 5 OA subjects), significant differences in MD could be found in the lateral tibiofemoral compartment and the patellofemoral compartment (Table 1). Differences in FA between healthy controls and OA subjects were lower and were only significant in the lateral tibia.
Open Questions for Research
The value of diffusion parameters in OA needs to be proven in larger cohorts and at low fields (3 T). The value of DTI to predict the progression of OA needs to be assessed in longitudinal studies.
Diffusion Measurements in Cartilage Repair
Injuries of articular cartilage are often a cause of debilitating knee pain and, if not treated, have a propensity to worsen and eventually lead to OA [71, 72]. Cartilage repair surgery aims to recover knee function in the short term and prevent OA on the long term [73]. Over the years, different repair strategies have been proposed: surgical removal of erased chondral tissue (e.g., shaving, joint debridement, etc.), stimulation of spontaneous repair reaction (e.g., microfracture, MFX), autologous tissue transplantation (e.g., osteochondral transplantation), and transplantation tissue-engineered scaffolds (e.g., matrix autologous chondrocyte transplantation, MACT). Successful cartilage repair has to fill the subchondral lesion with tissue and show congruity with the adjacent cartilage. However, morphological signs of the cartilage repair do not provide insight into the biochemical composition of the cartilage repair tissue [74].
The first in vivo studies of diffusion in the articular cartilage were performed with a variant of the 3D SSFP sequence, which is the diffusion-weighted reversed fat imaging with steady state (3D PSIF) [75, 76••, 77–79]. In these studies, two images with and without diffusion gradients were acquired and the quotient of the signal intensities, the diffusion quotient, was used as a semiquantitative estimate for diffusion-weighting. However, as shown by Buxton and Wu [47, 48], the diffusion quotient is a complex function of the ADC, the T 1 relaxation time, the repetition time, and the flip angle. Thus, changes in the diffusion quotient do not have a clear interpretation in terms of diffusion properties of the cartilage repair tissue.
Mamisch et al. [75] investigated the change in diffusion quotient in a cohort of matrix MACT patients. Patients were divided into two groups depending on the time from surgery: group 1 between 3 and 13 months (n = 6), and group 2 between 19 and 42 months (n = 9). Both groups showed significant increases in the diffusion quotient in cartilage repair (+36 and +11 % for groups 1 and 2, respectively; Table 2) as compared with the surrounding intact cartilage. After 1 year, patients in group 1 showed a significant decrease in the diffusion quotient (−8 %), while no change was observed in group 2 (Fig. 5) [76••].
Fused diffusion color maps of a 24-year-old patient 6 months after MACT surgery due to osteochondritis dissecans, at 6 months (a) and 18 months (b) after surgery. Color-coded diffusion map demonstrates a slight decrease in diffusivity over time within the area of cartilage repair marked by the arrows (adapted from [76••], with permission) (Color figure online)
Welsch et al. [77] measured the diffusion quotient in a cohort of MACT (n = 10) and MFX (n = 10) patients in the femoral condyle. Both MACT and MFX patients presented increased diffusion quotients in cartilage repair tissue with respect to intact cartilage, but no difference in diffusion quotient was found between MACT and MFX patients. Interestingly, a negative correlation (r = −0.557; P = 0.011) between the diffusion quotient and the clinical score for knee pain and function (Tenger–Lysholm score) was found in this study.
The high resolution achievable with the 3D SSFP sequences allows the study of cartilage repair in the ankle on MACT and MFX patients (Table 2) [78, 79]. The diffusion quotient of MACT patients (1.47) was not significantly (P = 0.105) different from the diffusion quotient of the reference cartilage (1.39) [78, 79]. Interestingly, MFX (2.07) showed a significantly increased diffusion quotient compared with intact cartilage (1.50, P < 0.016) but also with MACT repair tissue (P < 0.011) [79]. A significant correlation was found between the diffusion quotient and the time to surgery in MACT patients (Pearson’s coefficient −0.647, r 2 = 0.42, P = 0.043) but not on MFX patients.
Quantification of the diffusion using SSFP sequences is possible. Bieri et al. [52] showed the feasibility of a 3D-DESS sequence to measure a patient with cartilage repair (Fig. 2). They found increased ADC (+22 %) in the repair tissue as compared with the normal cartilage (Table 1).
Spin-echo-based sequences like the LSDTI or the radial acquisition are especially well suited for the measurements of DTI in cartilage repair. Figure 6 shows a MFX patient (male, 28 years old) 8 and 16 months after surgery. Imaging was performed on a 7 T whole body scanner using the LSDTI sequence. Anatomical images (T 1-weighted gradient echo) showed increased filling of the defect after 16 months. At 8 months, DTI parameter maps showed increased MD and decreased FA, most likely due to a poor filling of the defect at 8 months (Table 1). At 16 months, the FA has recovered to almost normal values, although MD still showed high values in the most superficial cartilage.
A 28-year-old male subject imaged 8 and 16 months after MFX surgery. Imaging protocol was performed at 7 T with the LSDTI (same protocol as in [68••]): 8 months after surgery, MD in the cartilage repair was increased (+60 %) and FA decreased (−67 %) with respect to the adjacent intact cartilage (Table 1). At the 16 months follow-up, the FA shows almost normal values (−8 % difference), while the MD was still slightly increased (+15 %), which was more evident in the most superficial half of the repair tissue
Open Questions for Research
There is a need of studies that perform quantitative measurements of diffusion in the cartilage repair. Quantitative measurements can provide additional help in differentiating between fibro cartilage and hyaline-like repair tissue. DTI may offer advantages in studying cartilage remodeling after repair surgery, since it has the potential to trace collagen remodeling with the FA.
Conclusions
Diffusion measurement of articular cartilage is a promising technique, since it provides information on the integrity of the cartilage matrix at the scale of a few microns, which is the scale of the cartilage ultrastructure. Although the idea of using MRI to measure the diffusion properties in articular cartilage is not new, it is not until recently that the first clinical studies have been performed. These first clinical studies have shown the potential of diffusion measurements to detect cartilage damage following cartilage injury, to early diagnose OA, and also to measure cartilage remodeling after cartilage repair surgery. Although the first studies have been very encouraging, the value of diffusion as a clinical biomarker for cartilage composition and structure still needs to be tested in large cohorts. Also, longitudinal studies are required to assess the value of diffusion as a biomarker for the prognosis of further cartilage damage.
Notes
Diffusion measurement of articular cartilage in vivo only uses moderate b values bellow 1,000 s/mm2, so that DTI, which is based on the approximation of Gaussian diffusion, is an adequate model to describe the diffusion properties of articular cartilage.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance, •• Of major importance
Insko EK, Reddy R, Leigh JS. High resolution, short echo time sodium imaging of articular cartilage. J Magn Reson Imaging. 1997;7(6):1056–9.
Reddy R, Li S, Noyszewski E, Kneeland J, Leigh J. In vivo sodium multiple quantum spectroscopy of human articular cartilage. Magn Reson Med. 1997;38(2):207–14.
Tiderius CJ, Olsson LE, Leander P, Ekberg O, Dahlberg L. Delayed gadolinium-enhanced MRI of cartilage (dGEMRIC) in early knee osteoarthritis. Magn Reson Med. 2003;49(3):488–92.
Williams A, Sharma L, McKenzie CA, Prasad PV, Burstein D. Delayed gadolinium-enhanced magnetic resonance imaging of cartilage in knee osteoarthritis: findings at different radiographic stages of disease and relationship to malalignment. Arthritis Rheum. 2005;52(11):3528–35.
Regatte RR, Akella SV, Borthakur A, Kneeland JB, Reddy R. Proteoglycan depletion-induced changes in transverse relaxation maps of cartilage: comparison of T 2 and T 1rho. Acad Radiol. 2002;9(12):1388–94.
Regatte RR, Akella SV, Lonner JH, Kneeland JB, Reddy R. T 1rho relaxation mapping in human osteoarthritis (OA) cartilage: comparison of T 1rho with T 2. J Magn Reson Imaging. 2006;23(4):547–53.
Ling W, Regatte RR, Navon G, Jerschow A. Assessment of glycosaminoglycan concentration in vivo by chemical exchange-dependent saturation transfer (GAGCEST). Proc Natl Acad Sci USA. 2008;105(7):2266–70.
Dardzinski B, Mosher T, Li S, Van Slyke M, Smith M. Spatial variation of T 2 in human articular cartilage. Radiology. 1997;205(2):546–50.
Nieminen MT, Rieppo J, Toyras J, Hakumaki JM, Silvennoinen J, Hyttinen MM, et al. T 2 relaxation reveals spatial collagen architecture in articular cartilage: a comparative quantitative MRI and polarized light microscopic study. Magn Reson Med. 2001;46(3):487–93.
Kim DK, Ceckler TL, Hascall VC, Calabro A, Balaban RS. Analysis of water-macromolecule proton magnetization transfer in articular cartilage. Magn Reson Med. 1993;29(2):211–5.
Gray ML, Burstein D, Lesperance LM, Gehrke L. Magnetization transfer in cartilage and its constituent macromolecules. Magn Reson Med. 1995;34(3):319–25.
Seo GS, Aoki J, Moriya H, Karakida O, Sone S, Hidaka H, et al. Hyaline cartilage: in vivo and in vitro assessment with magnetization transfer imaging. Radiology. 1996;201(2):525–30.
Keenan KE, Besier TF, Pauly JM, Han E, Rosenberg J, Smith RL, et al. Prediction of glycosaminoglycan content in human cartilage by age, T 1ρ and T 2 MRI. Osteoarthr Cartil. 2011;19(2):171–9.
Mow VC, Gu WY, Chen FH. Structure and function of articular cartilage. In: Mow VC, Huiskes R, editors. Basic orthopedics biomechanics and mechano-biology. 3rd ed. Philadelphia: Lippincott Williams and Wilkins; 2005. p. 123–80.
Huntington S. Scanning electron microscopy of cartilage. In: Boyde A, Jones SJ, editors. Cartilage: structure, function, and biochemistry. New York: Academic; 1983. p. 105–48.
Filidoro L, Dietrich O, Weber J, Rauch E, Oerther T, Wick M, et al. High-resolution diffusion tensor imaging of human patellar cartilage: feasibility and preliminary findings. Magn Reson Med. 2005;53(5):993–8. doi:10.1002/mrm.20469.
Meder R, de Visser SK, Bowden JC, Bostrom T, Pope JM. Diffusion tensor imaging of articular cartilage as a measure of tissue microstructure. Osteoarthr Cartil. 2006;14(9):875–81.
Deng X, Farley M, Nieminen MT, Gray M, Burstein D. Diffusion tensor imaging of native and degenerated human articular cartilage. Magn Reson Imaging. 2007;25(2):168–71.
de Visser SK, Bowden JC, Wentrup-Byrne E, Rintoul L, Bostrom T, Pope JM, et al. Anisotropy of collagen fibre alignment in bovine cartilage: comparison of polarised light microscopy and spatially resolved diffusion-tensor measurements. Osteoarthr Cartil. 2008;16(6):689–97. doi:10.1016/j.joca.2007.09.015.
Raya JG, Melkus G, Adam-Neumair S, Dietrich O, Muetzel E, Kahr B, et al. Change of diffusion tensor imaging parameters in articular cartilage with progressive proteoglycan extraction. Investig Radiol. 2011;46(6):401–9. doi:10.1097/RLI.0b013e3182145aa8.
Raya JG, Arnoldi A, Filidoro L, Adam-Neumair S, Melkus G, Dietrich O, et al. Ultra high field diffusion tensor imaging of articular cartilage correlated with histology and scanning electron microscopy. Magn Reson Mater Phys. 2011;24(4):247–58.
Knauss R, Schiller J, Fleischer G, Karger J, Arnold K. Self-diffusion of water in cartilage and cartilage components as studied by pulsed field gradient NMR. Magn Reson Med. 1999;41(2):285–92. doi:10.1002/(SICI)1522-2594(199902)41:2<285:AID-MRM11>3.0.CO;2-3.
Burstein D, Gray ML, Hartman AL, Gipe R, Foy BD. Diffusion of small solutes in cartilage as measured by nuclear magnetic resonance (NMR) spectroscopy and imaging. J Orthop Res. 1993;11(4):465–78. doi:10.1002/jor.1100110402.
Xia Y, Farquhar T, Burton-Wurster N, Vernier-Singer M, Lust G, Jelinski L. Self-diffusion monitors degraded cartilage. Arch Biochem Biophys. 1995;323(2):323–8. doi:10.1006/abbi.1995.9958.
O’Hara BP, Urban JPG, Maroudas A. Influence of cyclic loading on the nutrition of articular cartilage. Ann Rheum Dis. 1990;49(7):536–9.
Maroudas A, Bullough PG, Swanson SAV, Freeman MAR. The permeability of articular cartilage. J Bone Jt Surg Br. 1968;50(1):166–77.
Mow V, Ateshian G, Spilker R. Biomechanics of diarthrodial joints: a review of twenty years of progress. J Biomech Eng. 1993;115(4B):460–7.
Basser PJ, Őzarslan E. Anisotropic diffusion: from the apparent diffusion coefficient to the apparent diffusion tensor. In: Jones DK, editor. Diffusion MRI: theory, methods and applications. New York: Oxford University Press; 2011. p. 79–91.
Xia Y, Farquhar T, Burton-Wurster N, Ray E, Jelinski LW. Diffusion and relaxation mapping of cartilage–bone plugs and excised disks using microscopic magnetic resonance imaging. Magn Reson Med. 1994;31(3):273–82.
Toffanin R, Mlynárik V, Russo S, Szomolányi P, Piras A, Vittur F. Proteoglycan depletion and magnetic resonance parameters of articular cartilage. Arch Biochem Biophys. 2001;390(2):235–42. doi:10.1006/abbi.2001.2338.
Berg A, Singer T, Moser E. High-resolution diffusivity imaging at 3.0 T for the detection of degenerative changes: a trypsin-based arthritis model. Invest Radiol. 2003;38(7):460–6. doi:10.1097/01.rli.0000078762.72335.57.
Lin PC, Reiter DA, Spencer RG. Classification of degraded cartilage through multiparametric MRI analysis. J Magn Reson. 2009;201(1):61–71.
•• Lin PC, Irrechukwu O, Roque R, Hancock B, Fishbein KW, Spencer RG. Multivariate analysis of cartilage degradation using the support vector machine algorithm. Magn Reson Med. 2012;67(6):1815–26. doi:10.1002/mrm.23189. This study investigates the value of a multiparametric MRI approach to classify cartilage degeneration on nasal bovine samples scanned native and after PG depletion. Contrary to most MRI validation experiments which just assess differences after treatment, this manuscript quantifies the value of MRI parameters to classify samples as intact or degraded.
Juráš V, Bittšanský M, Majdišová Z, Trattnig S. In-vitro evaluation of pre- and post-compression states of human articular cartilage using MRI at 3 Tesla. Meas Sci Rev. 2007;7(2):39–42.
Juráš V, Bittšanský M, Majdišová Z, Szomolányi P, Sulzbacher I, Gäbler S, et al. In vitro determination of biomechanical properties of human articular cartilage in osteoarthritis using multi-parametric MRI. J Magn Reson. 2009;197(1):40–7.
• Aoki T, Watanabe A, Nitta N, Numano T, Fukushi M, Niitsu M. Correlation between apparent diffusion coefficient and viscoelasticity of articular cartilage in a porcine model. Skeletal Radiol. 2012;41(9):1087–92. The ADC is correlated with the mechanical properties of articular cartilage measured by indentation and modeled with a viscoelastic model. Significant correlations between ADC and the relaxation time and the viscoelasticity are observed.
Greene GW, Zappone B, Söderman O, Topgaard D, Rata G, Zeng H, et al. Anisotropic dynamic changes in the pore network structure, fluid diffusion and fluid flow in articular cartilage under compression. Biomaterials. 2010;31(12):3117–28.
Greene GW, Zappone B, Zhao B, Söderman O, Topgaard D, Rata G, et al. Changes in pore morphology and fluid transport in compressed articular cartilage and the implications for joint lubrication. Biomaterials. 2008;29(33):4455–62.
de Visser SK, Crawford RW, Pope JM. Structural adaptations in compressed articular cartilage measured by diffusion tensor imaging. Osteoarthr Cartil. 2008;16(1):689–97.
Raya JG, Melkus G, Adam-Neumair S, Dunham K, Dietrich O, Putz R, et al., editors. Multiparametric assessment of healthy and OA articular cartilage under loading at 17.6 T. In: 19th congress of the International Society of the Magnetic Resonance in the Medicine (ISMRM). Montreal, Canada; 2011. p. 3207.
Pierce DM, Trobin W, Raya JG, Trattnig S, Bischof H, Galser C, et al. DT-MRI based computation of collagen fiber deformation in human articular cartilage: a feasibility study. Ann Biomed Eng. 2010;38(7):2447–63.
Mlynárik V, Sulzbacher I, Bittšanský M, Fuiko R, Trattnig S. Investigation of apparent diffusion constant as an indicator of early degenerative disease in articular cartilage. J Magn Reson Imaging. 2003;17(4):440–4. doi:10.1002/jmri.10276.
• Raya JG, Melkus G, Adam-Neumair S, Dietrich O, Muetzel E, Reiser M, et al. Diffusion-tensor imaging of human articular cartilage specimens with early signs of cartilage damage. Radiology. 2013;266(3):831–41. This study tests the ability of DTI to classify samples with histological early signs of OA as intact or damaged. Results show excellent accuracy of the classification (95 %) and good accuracy (74 %) of the grading of the damage as compared with the histology.
Majdišová Z, Szomolányi P, Juráš V, Trattnig S, editors. MRI study of the repair tissue following ACI in the defect of the human cartilage specimens. In: 16th Annual meeting and exhibition of the International Society of Magnetic Resonance in the Medicine. Toronto, ON, Canada; 2008.
Gold GE, Butts K, Fechner KP, Bergman G, Beaulieu CF, Lang PK, et al. In vivo diffusion-weighted imaging of cartilage. In: 6th Scientific meeting and exhibition of the International Society of Magnetic Resonance in the Medicine, Sidney, Australia, 1998. p. 1066.
Miller KL, Hargreaves BA, Gold GE, Pauly JM. Steady-state diffusion-weighted imaging of in vivo knee cartilage. Magn Reson Med. 2004;5(1):394–8.
Wu EX, Buxton RB. Effect of diffusion on the steady-state magnetization with pulsed field gradients. J Magn Reson. 1990;90(2):243–53.
Buxton RB. The diffusion sensitivity of fast steady-state free precession imaging. Magn Reson Med. 1993;29(2):235–43.
Gold GE, Han E, Stainsby J, Wright G, Brittain J, Beaulieu CF. Musculoskeletal MRI at 3.0 T: relaxation times and image contrast. Am J Roentgenol. 2004;183(2):343–51.
Staroswiecki E, Granlund KL, Alley MT, Gold GE, Hargreaves BA. Simultaneous estimation of T(2) and apparent diffusion coefficient in human articular cartilage in vivo with a modified three-dimensional double echo steady state (DESS) sequence at 3 T. Magn Reson Med. 2012;67(4):1086–96.
•• Bieri O, Ganter C, Scheffler K. Quantitative in vivo diffusion imaging of cartilage using double echo steady-state free precession. Magn Reson Med. 2012;. doi:10.1002/mrm.23275. This article describes a new strategy to perform diffusion measurements of the articular cartilage with a 3D DESS sequence that does not requires additional measurement of the T 1 relaxation time. The proposed method solves one of the major limitations of steady state sequences for quantification of diffusion measurements.
Bieri O, Ganter C, Welsch GH, Trattnig S, Mamisch TC, Scheffler K. Fast diffusion-weighted steady state free precession imaging of in vivo knee cartilage. Magn Reson Med. 2012;67(3):691–700.
Azuma T, Nakai R, Takizawa O, Tsutsumi S. In vivo structural analysis of articular cartilage using diffusion tensor magnetic resonance imaging. Magn Reson Imaging. 2009;27(9):1242–8.
Zhu SC, Shi DP, Xuan A. Human patellar cartilage: echo planar diffusion-weighted MR imaging findings at 3.0 T. Clin Imaging. 2012;36(3):199–202.
Morel V, Quinn TM. Cartilage injury by ramp compression near the gel diffusion rate. J Orthop Res. 2004;22(1):145–51.
Quinn TM, Allen RG, Shalet BJ, Perumbuli P, Hunziker EB. Matrix cell injury due to sub-impact loading of adult bovine cartilage explants: effect of strain rates and peak stress. J Orthop Res. 2001;19(2):242–9.
Quinn TM, Grodzinsky AJ, Hunziker EB, Sandy JD. Effects of injurious compression on matrix turnover around individual cells in calf articular cartilage explants. J Orthop Res. 1998;16(4):490–9.
Kurz B, Lemke AK, Fay J, Pufe T, Grodzinsky AJ, Schünke M. Pathomechanics of cartilage destruction by mechanical injury. Ann Anat. 2005;187:473–85.
Lohmander LS, Dahlberg L, Ryd L, Heinegård D. Increased levels of proteoglycan fragments in knee joint fluid after injury. Arthritis Rheum. 1989;32(11):1434–42.
Lohmander LS, Ionescu M, Jugessur H, Poole AR. Changes in joint cartilage aggrecan after knee injury and in osteoarthritis. Arthritis Rheum. 1999;42(3):534–44.
Lohmander LS, Yoshihara Y, Roos H, Kobayashi T, Yamada H, Shinmei M. Procollagen II C-propeptide in joint fluid: changes in concentration with age, time after knee injury, and osteoarthritis. J Rheumatol. 1996;23(10):1765–9.
Nelson F, Billinghurst RC, Pidoux I, Reiner A, Langworthy M, McDermott M, et al. Early post-traumatic osteoarthritis-like changes in human articular cartilage following rupture of anterior cruciate ligament. Osteoarthr Cartil. 2006;14:114–9.
• Xu J, Xie G, Di Y, Bai M, Zhao X. Value of T 2-mapping and DWI in the diagnosis of early knee cartilage injury. J Radiol Case Rep. 2011;5(2):13–8. First clinical study to indicate that knee injury can change the diffusion properties of articular cartilage.
Heinegård D. Cartilage matrix destruction. In: Bronner F, Farach-Carson MC, editors. Bone and osteoarthritis. Topics in bone biology, vol. 4. London: Springer; 2007. p. 81–95.
Maroudas AI. Balance between swelling pressure and collagen tension in normal and degenerate cartilage. Nature. 1976;260(5554):808–9.
Maroudas A, Venn M. Chemical composition and swelling of normal and osteoarthrotic femoral head cartilage. II. Swelling. Ann Rheum Dis. 1977;36(5):399–406.
Heinegård D, Saxne T. The role of the cartilage matrix in osteoarthritis. Nature Rev Rheumatol. 2011;7:50–56. doi:10.1038/nrrheum.2010.198.
•• Raya JG, Horng A, Dietrich O, Krasnokutsky S, Beltran LS, Storey P, et al. Articular cartilage: in vivo diffusion-tensor imaging. Radiology. 2012;262(2):550–9. This study demonstrated for the first time the value of DTI to detect OA subjects with early changes of cartilage damage from healthy subjects. DTI parameters provided high accuracy (92 %) in discriminating asymptomatic form OA subjects.
Gudbjartsson H, Maier SE, Mulkern RV, Morocz IA, Patz S, Jolesz FA. Line scan diffusion imaging. Magn Reson Med. 1996;36(4):509–19.
Raya JG, Notohamiprodjo M, Krasnokutsky S, Gyftopoulos S, Glaser C, editors. In vivo diffusion tensor imaging (DTI) of articular cartilage of healthy and osteoarthritis (OA) subjects with coverage of all cartilage plates. In: 20th Annual meeting and exhibition of the International Society of Magnetic Resonance in the Medicine. Melbourne, VIC, Australia; 2012. p. 502.
Messner K, Maletius W. The long-term prognosis for severe damage to weight-bearing cartilage in the knee: a 14-year clinical and radiographic follow-up in 28 young athletes. Acta Orthop Scand. 1996;67(2):165–8.
Stufkens SA, Knupp M, Horisberger M, Lampert C, Hintermann B. Cartilage lesions and the development of osteoarthritis after internal fixation of ankle fractures: a prospective study. J Bone Jt Surg Am. 2010;92(2):279–86.
Minas T. Cartilage repair and regeneration. In: Minas T, editor. A primer in cartilage repair and joint preservation of the knee. Philadelphia: Elsevier; 2001. p. 8–21.
Potter H, Foo LF, Pearle AD. MRI and articular cartilage. Evaluating lesions and postrepair tissue. In: Williams III RJ, editor. Cartilage repair strategies. Totowa: Humana; 2007. p. 19–35.
Mamisch TC, Menzel MI, Welsch GC, Bittersohl B, Salomonowitz E, Szomolányi P, et al. Steady-state diffusion imaging for MR in vivo evaluation of reparative cartilage after matrix-associated autologous chondrocyte transplantation at 3 Tesla—preliminary results. Eur J Radiol. 2008;65:72–9.
•• Friederich KM, Mamisch TC, Plank C, Langs G, Marlovits S, Salomonowitz E, et al. Diffusion-weighted imaging for the follow-up of patients after matrix-associated autologous chondrocyte transplantation. Eur J Radiol. 2010;73:622–8. This article provides the first longitudinal study on cartilage repair, and demonstrates evidence of the value of diffusion measurements to detect changes longitudinally.
Welsch GC, Trattnig S, Domayer S, Marlovits S, White LM, Mamisch TC. Multimodal approach in the use of clinical scoring, morphological MRI and biochemical T 2-mapping and diffusion-weighted imaging in their ability to assess differences between cartilage repair tissue after microfracture therapy and matrix-associated autologous chondrocyte transplantation: a pilot study. Osteoarthr Cartil. 2009;17:1219–27.
Quirbach S, Trattnig S, Marlovits S, Zimmermann V, Domayer S, Dorotka R, et al. Initial results of in vivo high-resolution morphological and biochemical cartilage imaging of patients after matrix-associated autologous chondrocyte transplantation (MACT) of the ankle. Skeletal Radiol. 2009;38(8):751–60.
Apprich S, Trattnig S, Welsch GH, Noebauer-Huhmann IM, Sokolwski M, Hirschfeld C, et al. Assessment of articular cartilage repair tissue after matrix-associated autologous chondrocyte transplantation or the microfracture technique in the ankle joint using diffusion-weighted imaging at 3 Tesla. Osteoarthr Cartil. 2012;20:703–11.
Compliance with Ethics Guidelines
Conflict of Interest
José G. Raya declares that he has no conflicts of interest.
Human and Animal Rights and Informed Consent
The study was approved by the Institutional Review Board and performed in compliance with HIPAA. All subjects provided written informed consent.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Cartilage Imaging.
Rights and permissions
About this article
Cite this article
Raya, J.G. Diffusion-Weighted Imaging and Diffusion Tensor Imaging. Curr Radiol Rep 2, 37 (2014). https://doi.org/10.1007/s40134-013-0037-5
Published:
DOI: https://doi.org/10.1007/s40134-013-0037-5