Abstract
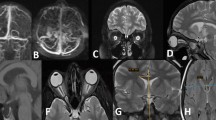
Increased intracranial hypertension (IIH) is a defined clinical condition; however, an unsolved pathophysiologic background usually creates problems in its diagnosis and proper approach. The aim of this study was to emphasize the clinical conditions and brain magnetic resonce imaging (MRI) clues of pediatric patients, especially this clinical entity with high morbidity. Here, we review the etiology, clinical presentation, brain MRI findings, and prognosis of IIH in children. The symptoms’ onset age ranged from 9 months to 16 years. Headache (81%), vomiting (37%), and diplopia (33.3%) were the most frequent symptoms. The most common etiologic factors were found to be obesity and dural venous sinus thrombosis. Cerebrospinal fluid (CSF) opening pressure had mean a mean value of 615.2 ± 248 mm H2O. A significant relationship was found between visual field impairment and height of CSF pressure (p < 0.001). Optic nerve sheath enlargement (88.8%) and optic nerve tortuosity (85.1%) were found as the most common brain MRI findings. Slit-like ventricle (37%), venous sinus thrombosis (29.6%), posterior globe sclera flattening (29.6%), empty sella (25.9%), and intraocular protrusion of the optic nerve (14.8%) were the other findings. A significant relationship was found between CSF opening pressure and the presence of optic nerve tortuosity (p = 0.002), and distension of the optic nerve sheath (p = 0.006). All patients received acetazolamide, only one patient underwent lumboperitoneal shunt, and only one received steroids. In children, IIH can present with different etiologies and symptoms. Brain MRI provides crucial clues in diagnosis. Urgent diagnosis and treatment planning are required to protect vision functions.


Similar content being viewed by others
References
Sismanis A (1987) Otologic manifest ations of benign intracranial hypertension syndrome: diagnosis and management. Laryngoscope 97:1–17
Friedman DI, Jacobson DM (2004) Idiopathic intracranial hypertension. J Neuro ophthalmol 24:138–145
Rangwala LM, Liu GT (2007) Pediatric idiopathic intracranial hypertension. Surv Ophthalmol 52:597–617
Wall M, George D (1991) Idiopathic intracranial hypertension. A prospective study of 50 patients. Brain 114:155–180
Galgano MA, Deshaie EM (2013) An update on the management of pseudotumor cerebri. Clin Neurol Neurosurg 115:252–259
Skau M, Brennum J, Gjerris F, Jensen R (2006) What is new about idiopathic intracranial hypertension? An updated review of mechanism and treatment. Cephalalgia 26:384–399
Thambisetty M, Lavin PJ, Newman NJ, Biousse V (2007) Fulminant idiopathic intracranial hypertension. Neurology 68:229–232
Sinclair AJ, Ball AK, Burdon MA, Clarke CE, Stewart PM, Curnow SJ, Rauz S (2008) Exploring the pathogenesis of IIH: an inflammatory perspective. J Neuroimmunol 201–2:212–220
Ball AK, Clarke CE (2006) Idiopathic intracranial hypertension. Lancet Neurology 5:433–442
Shofty B, Ben-Sira L, Constantini S, Freedman S, Kesler A (2012) Optic nerve sheath diameter on MR imaging: establishment of norms and comparison of pediatric patients with idiopathic intracranial hypertension with healthy controls. Am J Neuroradiol 33:366–369
Bansal L, Niccoli L, Bailey A, Zuccoli G (2014) Imaging the eye in idiopathic intracranial hypertension. Headache 54:1046–1047
Mandelstam S, Moon A (2004) MRI of optic disc edema in childhood idiopathic intracranial hypertension. Pediatr Radiol 34:362
Hirfanoglu T, Aydin K, Serdaroglu A, Havali C (2015) Novel magnetic resonance imaging findings in children with intracranial hypertension. Pediatr Neurol 53:151–156
Degnan AJ, Levy LM (2011) Pseudotumor cerebri: brief review of clinical syndrome and imaging findings. AJNR Am J Neuroradiol 32:1986–1993
Passi N, Degnan AJ, Levy LM (2013) MR imaging of papilledema and visual pathways:effects of increased intracranial pressure and pathophysiologic mechanisms. AJNR Am J Neuroradiol 34:919–924
Maralani PJ, Hassanlou M, Torres C, Chakraborty S, Kingstone M, Patel V, Zackon D, Bussière M (2012) Accuracy of brain imaging in the diagnosis of idiopathic intracranial hypertension. Clin Radiol 67:656–663
Saindane AM, Bruce BB, Riggeal BD, Newman NJ, Biousse V (2013) Association of MRI findings and visual outcome in idiopathic intracranial hypertension. Am J Roentgenol 201:412–418
Agid R, Farb RI, Willinsky RA, Mikulis DJ, Tomlinson G (2006) Idiopathic intracranial hypertension: the validity of cross-sectional neuroimaging signs. Neuroradiology 48:521–527
Seitz J, Held P, Strotzer M, Müller M, Völk M, Lenhart M, Djavidani B, Feuerbach S (2002) Magnetic resonance imaging in patients diagnosed with papilledema: a comparison of 6 different high-resolution T1- and T2-weighted 3-dimensional and 2-dimensional sequences. J Neuroimaging 12:164–171
Babikian P, Corbett J, Bell W (1994) Idiopathic intracranial hypertension in children: the Iowa experience. J Child Neurol 9:144–149
Gordon K (1997) Pediatric pseudotumor cerebri: descriptive epidemiology. Can J Neurol Sci 24:219–221
Rowe FJ (2011) Assessment of visual function in idiopathic intracranial hypertension. Br J Neurosurg 25:45–54
Wall M, White WN (1998) Asymmetric papilledema in idiopathic intracranial hypertension: prospective intraocular comparison of sensory visual function. Invest Ophthalmol Vis Sci 39:134–142
Bidot S, Saindane AM, Peragallo JH, Bruce BB, Newman NJ, Biousse V (2015) Brain imaging in idiopathic intracranial hypertension. J Neuro-Ophthalmol 35:400–411
Rogers DL (2014) A review of pediatric idiopathic intracranial hypertension. Pediatr Clin North Am 61:579–590
Hansen HC, Helmke K (1997) Validation of the optic nerve sheath response to changing cerebrospinal fluid pressure: ultrasound findings during intrathecal infusion tests. J Neurosurg 87:34–40
Görkem SB, Doğanay S, Canpolat M, Koc G, Dogan MS, Per H, Coşkun A (2015) MR imaging findings in children with pseudotumor cerebri and comparison with healthy controls. Childs Nerv Syst 31:373–380
Lim MJ, Pushparajah K, Jan W, Calver D, Lin J-P (2010) Magnetic resonance imaging changes in idiopathic intracranial hypertension in children. J Child Neurol 25:294–299
Agarwal P, Kumar M, Arora V (2010) Clinical profile of cerebral venous sinus thrombosis and the role of imaging in its diagnosis in patients with presumed idiopathic intracranial hypertension. Indian J Ophthalmol 58:153–155
Inokuchi G, Tsutsumi N, Komatsu H, Fujita T, Sawada N, Kumoi K (2013) Persistent petrosquamosal sinus: underlying cause of otitic hydrocephalus with lateral sinus thrombosis. Int J Pediatr Otorhinolaryngol 77:1908–1911
Biousse V, Bruce BB, Newman NJ (2012) Update on the pathophysiology and management of idiopathic intracranial hypertension. J Neurol Neurosurg Psychiatry 83:488–494
Dave SB, Subramanian PS (2014) Pseudotumor cerebri: an update on treatment options. Indian J Ophthalmol 62:996–998
Celebisoy N, Gökçay F, Sirin H, Akyürekli O (2007) Treatment of idiopathic intracranial hypertension: topiramate vs acetazolamide, an open-label study. Acta Neurol Scand 116:322–327
Matthews YY (2008) Drugs used in childhood idiopathic or benign intracranial hypertension. Arch Dis Child Educ Pract Ed 93:19–25
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors declare that they have no conflicts of interest related to the present study.
Ethical approval
The study was conducted in accordance with the Helsinki Declaration and the study protocol was approved by the corporate ethics committee.
Informed consent
Informed consent had been obtained from all all subjects included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kılıç, B., Güngör, S. Clinical features and the role of magnetic resonance imaging in pediatric patients with intracranial hypertension. Acta Neurol Belg 121, 1567–1573 (2021). https://doi.org/10.1007/s13760-020-01415-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-020-01415-1