Abstract
Purpose
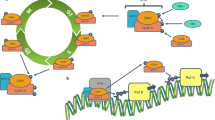
Neuroblastoma (NB) is an aggressive pediatric malignancy that typically occurs in infants and children under the age of 5 years. High-stage tumors relapse frequently even after aggressive multimodal treatment, resulting in therapy resistance and eventually in patient death. Clearly, new biologically-targeted drugs are needed that more efficiently suppress tumor growth and prevent relapse. We and others previously showed that polyamines such as spermidine play an essential role in NB tumorigenesis and that DFMO, an inhibitor of the central polyamine synthesis gene ODC, is effective in vitro and in vivo, prompting its evaluation in NB clinical trials. However, the specific molecular actions of polyamines remain poorly defined. Spermidine and deoxyhypusine synthase (DHPS) are essential components in the hypusination-driven post-translational activation of eukaryotic initiation factor 5A (eIF5A).
Methods
We assessed the role of DHPS in NB and the impact of its inhibition by N 1-guanyl-1,7-diaminoheptane (GC7) on tumor cell growth using cell proliferation assays, Western blot, immunofluorescence microscopy, and Affymetrix micro-array mRNA expression analyses in NB tumor samples.
Results
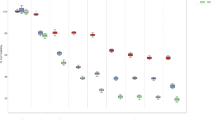
We found that GC7 inhibits NB cell proliferation in a dose-dependent manner, through induction of the cell cycle inhibitor p21 and reduction of total and phosphorylated Rb proteins. Strikingly, high DHPS mRNA expression correlated significantly with unfavorable clinical parameters, including poor patient survival, in a cohort of 88 NB tumors (all P < 0.04).
Conclusions
These results suggest that spermidine and DHPS are key contributing factors in NB tumor proliferation through regulation of the p21/Rb signaling axis.







Similar content being viewed by others
References
G.M. Brodeur, Neuroblastoma: biological insights into a clinical enigma. Nat Rev Cancer 3, 203–216 (2003)
N.K. Cheung, M.A. Dyer, Neuroblastoma: developmental biology, cancer genomics and immunotherapy. Nat Rev Cancer 13, 397–411 (2013)
J.M. Maris, Recent advances in neuroblastoma. N Engl J Med 362, 2202–2211 (2010)
J.M. Maris, M.D. Hogarty, R. Bagatell, S.L. Cohn, Neuroblastoma Lancet 369, 2106–2120 (2007)
J.R. Park, A. Eggert, H. Caron, Neuroblastoma: biology, prognosis, and treatment. Hematol Oncol Clin North Am 24, 65–86 (2010)
M. Schwab, F. Westermann, B. Hero, F. Berthold, Neuroblastoma: biology and molecular and chromosomal pathology. Lancet Oncol 4, 472–480 (2003)
D.L. Baker, M.L. Schmidt, S.L. Cohn, J.M. Maris, W.B. London, A. Buxton, D. Stram, R.P. Castleberry, H. Shimada, A. Sandler, R.C. Shamberger, A.T. Look, C.P. Reynolds, R.C. Seeger, K.K. Matthay, G. Children’s Oncology, Outcome after reduced chemotherapy for intermediate-risk neuroblastoma. N Engl J Med 363, 1313–1323 (2010)
S.L. Cohn, A.D. Pearson, W.B. London, T. Monclair, P.F. Ambros, G.M. Brodeur, A. Faldum, B. Hero, T. Iehara, D. Machin, V. Mosseri, T. Simon, A. Garaventa, V. Castel, K.K. Matthay, The International Neuroblastoma Risk Group (INRG) classification system: an INRG task force report. J Clin Oncol 27, 289–297 (2009)
S.G. Kreissman, R.C. Seeger, K.K. Matthay, W.B. London, R. Sposto, S.A. Grupp, D.A. Haas-Kogan, M.P. Laquaglia, A.L. Yu, L. Diller, A. Buxton, J.R. Park, S.L. Cohn, J.M. Maris, C.P. Reynolds, J.G. Villablanca, Purged versus non-purged peripheral blood stem-cell transplantation for high-risk neuroblastoma (COG A3973): a randomised phase 3 trial. Lancet Oncol 14, 999–1008 (2013)
D.R. Strother, W.B. London, M.L. Schmidt, G.M. Brodeur, H. Shimada, P. Thorner, M.H. Collins, E. Tagge, S. Adkins, C.P. Reynolds, K. Murray, R.S. Lavey, K.K. Matthay, R. Castleberry, J.M. Maris, S.L. Cohn, Outcome after surgery alone or with restricted use of chemotherapy for patients with low-risk neuroblastoma: results of children’s oncology group study P9641. J Clin Oncol 30, 1842–1848 (2012)
A. Canete, M. Gerrard, H. Rubie, V. Castel, A. Di Cataldo, C. Munzer, R. Ladenstein, B. Brichard, J.D. Bermudez, J. Couturier, B. de Bernardi, A.J. Pearson, J. Michon, Poor survival for infants with MYCN-amplified metastatic neuroblastoma despite intensified treatment: the international society of paediatric oncology European neuroblastoma experience. J Clin Oncol 27, 1014–1019 (2009)
B.H. Kushner, K. Kramer, M.P. LaQuaglia, S. Modak, K. Yataghene, N.K. Cheung, Reduction from seven to five cycles of intensive induction chemotherapy in children with high-risk neuroblastoma. J Clin Oncol 22, 4888–4892 (2004)
A.S. Bachmann, The role of polyamines in human cancer: prospects for drug combination therapies. Hawaii Med J 63, 371–374 (2004)
R.A. Casero Jr., L.J. Marton, Targeting polyamine metabolism and function in cancer and other hyperproliferative diseases. Nat Rev Drug Discov 6, 373–390 (2007)
A.E. Pegg, Polyamine metabolism and its importance in neoplastic growth and a target for chemotherapy. Cancer Res 48, 759–774 (1988)
A.E. Pegg, D.J. Feith, Polyamines and neoplastic growth. Biochem Soc Trans 35, 295–299 (2007)
E.W. Gerner, F.L. Meyskens Jr., Polyamines and cancer: old molecules, new understanding. Nat Rev Cancer 4, 781–792 (2004)
D.L. Koomoa, L.P. Yco, T. Borsics, C.J. Wallick, A.S. Bachmann, Ornithine decarboxylase inhibition by {alpha}-difluoromethylornithine activates opposing signaling pathways via phosphorylation of both Akt/Protein Kinase B and p27Kip1 in Neuroblastoma. Cancer Res 68, 9825–9831 (2008)
C.J. Wallick, I. Gamper, M. Thorne, D.J. Feith, K.Y. Takasaki, S.M. Wilson, J.A. Seki, A.E. Pegg, C.V. Byus, A.S. Bachmann, Key role for p27Kip1, retinoblastoma protein Rb, and MYCN in polyamine inhibitor-induced G1 cell cycle arrest in MYCN-amplified human neuroblastoma cells. Oncogene 24, 5606–5618 (2005)
D.L. Koomoa, T. Borsics, D.J. Feith, C.C. Coleman, C.J. Wallick, I. Gamper, A.E. Pegg, A.S. Bachmann, Inhibition of S-adenosylmethionine decarboxylase by inhibitor SAM486A connects polyamine metabolism with p53-Mdm2-Akt/protein kinase B regulation and apoptosis in neuroblastoma. Mol Cancer Ther 8, 2067–2075 (2009)
D.L. Koomoa, D. Geerts, I. Lange, J. Koster, A.E. Pegg, D.J. Feith, A.S. Bachmann, DFMO/eflornithine inhibits migration and invasion downstream of MYCN and involves p27Kip1 activity in neuroblastoma. Int J Oncol 42, 1219–1228 (2013)
K. Samal, P. Zhao, A. Kendzicky, L.P. Yco, H. McClung, E. Gerner, M. Burns, A.S. Bachmann, G. Sholler, AMXT-1501, a novel polyamine transport inhibitor, synergizes with DFMO in inhibiting neuroblastoma cell proliferation by targeting both ornithine decarboxylase and polyamine transport. Int J Cancer 133, 1323–1333 (2013)
M.D. Hogarty, M.D. Norris, K. Davis, X. Liu, N.F. Evageliou, C.S. Hayes, B. Pawel, R. Guo, H. Zhao, E. Sekyere, J. Keating, W. Thomas, N.C. Cheng, J. Murray, J. Smith, R. Sutton, N. Venn, W.B. London, A. Buxton, S.K. Gilmour, G.M. Marshall, M. Haber, ODC1 Is a critical determinant of MYCN Oncogenesis and a therapeutic target in neuroblastoma. Cancer Res 68, 9735–9745 (2008)
R.J. Rounbehler, W. Li, M.A. Hall, C. Yang, M. Fallahi, J.L. Cleveland, Targeting ornithine decarboxylase impairs development of MYCN-amplified neuroblastoma. Cancer Res 69, 547–553 (2009)
G. Sholler, E. Currier, D.L. Koomoa, A.S. Bachmann, synergistic inhibition of neuroblastoma tumor development by targeting ornithine decarboxylase and topoisomerase II. In 14th Advances in Neuroblastoma Research (ANR) Conference, Stockholm, Sweden, POT74 (2010)
G. Sholler, E. Gerner, G. Bergendahl, B.J. LaFleur, A. VanderWerff, T. Ashilkaga, W. Ferguson, W. Roberts, R.K. Wada, D. Eslin, J. Kraveka, J. Kaplan, D. Mitchell, N.S. Parikh, K. Neville, L. Sender, T. Higgins, M. Kawakita, K. Hiramatsu, S.S. Moriya, A.S. Bachmann, A phase I trial of DFMO as a single agent and in combination with etoposide in patients with refractory or recurrent neuroblastoma. In Annual Meeting of the American Association for Cancer Research (AACR), Washington, D.C., LB-179 (2013)
A.S. Bachmann, D. Geerts, G. Sholler, Neuroblastoma: Ornithine decarboxylase and polyamines are novel targets for therapeutic intervention. In Pediatric Cancer, Neuroblastoma: Diagnosis, Therapy, and Prognosis, ed. by M.A. Hayat, Springer Publisher, 91–103 (2012)
A.S. Bachmann, V.A. Levin, Clinical applications of polyamine-based therapeutics. In Polyamine Drug Discovery, ed. by P.M. Woster and R.A. Casero, Jr., Royal Society of Chemistry, 257–276 (2012)
U. Bachrach, Naturally occurring polyamines: interaction with macromolecules. Curr Protein Pept Sci 6, 559–566 (2005)
A.E. Pegg, Mammalian polyamine metabolism and function. IUBMB Life 61, 880–894 (2009)
H.M. Wallace, A.V. Fraser, A. Hughes, A perspective of polyamine metabolism. Biochem J 376, 1–14 (2003)
M.H. Park, K. Nishimura, C.F. Zanelli, S.R. Valentini, Functional significance of eIF5A and its hypusine modification in eukaryotes. Amino Acids 38, 491–500 (2010)
E.A. Paz, B. LaFleur, E.W. Gerner, Polyamines are oncometabolites that regulate the LIN28/let-7 pathway in colorectal cancer cells. Mol Carcinog 53(Suppl 1), E96–106 (2014)
E.W. Gerner, Cancer chemoprevention locks onto a new polyamine metabolic target. Cancer Prev Res 3, 125–127 (2010)
J. Jakus, E.C. Wolff, M.H. Park, J.E. Folk, Features of the spermidine-binding site of deoxyhypusine synthase as derived from inhibition studies. Effective inhibition by bis- and mono-guanylated diamines and polyamines. J Biol Chem 268, 13151–13159 (1993)
M.H. Park, E.C. Wolff, Y.B. Lee, J.E. Folk, Antiproliferative effects of inhibitors of deoxyhypusine synthase. Inhibition of growth of Chinese hamster ovary cells by guanyl diamines. J Biol Chem 269, 27827–27832 (1994)
Y. Lee, H.K. Kim, H.E. Park, M.H. Park, Y.A. Joe, Effect of N1-guanyl-1,7-diaminoheptane, an inhibitor of deoxyhypusine synthase, on endothelial cell growth, differentiation and apoptosis. Mol Cell Biochem 237, 69–76 (2002)
A. Slack, Z. Chen, R. Tonelli, M. Pule, L. Hunt, A. Pession, J.M. Shohet, The p53 regulatory gene MDM2 is a direct transcriptional target of MYCN in neuroblastoma. Proc Natl Acad Sci U S A 102, 731–736 (2005)
P. Fardin, A. Barla, S. Mosci, L. Rosasco, A. Verri, R. Versteeg, H.N. Caron, J.J. Molenaar, I. Ora, A. Eva, M. Puppo, L. Varesio, A biology-driven approach identifies the hypoxia gene signature as a predictor of the outcome of neuroblastoma patients. Mol Cancer 9, 185 (2010)
I. Revet, G. Huizenga, A. Chan, J. Koster, R. Volckmann, P. van Sluis, I. Ora, R. Versteeg, D. Geerts, The MSX1 homeobox transcription factor is a downstream target of PHOX2B and activates the Delta-Notch pathway in neuroblastoma. Exp Cell Res 314, 707–719 (2008)
T. Barrett, D.B. Troup, S.E. Wilhite, P. Ledoux, D. Rudnev, C. Evangelista, I.F. Kim, A. Soboleva, M. Tomashevsky, K.A. Marshall, K.H. Phillippy, P.M. Sherman, R.N. Muertter, R. Edgar, NCBI GEO: archive for high-throughput functional genomic data. Nucleic Acids Res 37, D885–890 (2009)
V. Bewick, L. Cheek, J. Ball, Statistics review 12: survival analysis. Crit Care 8, 389–394 (2004)
T. Borsics, E. Lundberg, D. Geerts, D.L. Koomoa, J. Koster, K. Wester, A.S. Bachmann, Subcellular distribution and expression of prenylated Rab acceptor 1 domain family, member 2 (PRAF2) in malignant glioma: influence on cell survival and migration. Cancer Sci 101, 1624–1631 (2010)
J.E. Gawecka, D. Geerts, J. Koster, M.J. Caliva, F.J. Sulzmaier, J. Opoku-Ansah, R.K. Wada, A.S. Bachmann, J.W. Ramos, PEA15 impairs cell migration and correlates with clinical features predicting good prognosis in neuroblastoma. Int J Cancer 131, 1556–1568 (2012)
D. Geerts, J. Koster, D. Albert, D.L. Koomoa, D.J. Feith, A.E. Pegg, R. Volckmann, H. Caron, R. Versteeg, A.S. Bachmann, The polyamine metabolism genes ornithine decarboxylase and antizyme 2 predict aggressive behavior in neuroblastomas with and without MYCN amplification. Int J Cancer 126, 2012–2024 (2010)
D. Geerts, C.J. Wallick, D.L. Koomoa, J. Koster, R. Versteeg, R.C. Go, A.S. Bachmann, Expression of prenylated Rab acceptor 1 domain family, member 2 (PRAF2) in neuroblastoma: correlation with clinical features, cellular localization, and cerulenin-mediated apoptosis regulation. Clin Cancer Res 13, 6312–6319 (2007)
I. Lange, D. Geerts, D.J. Feith, G. Mocz, J. Koster, A.S. Bachmann, Novel interaction of ornithine decarboxylase with sepiapterin reductase regulates neuroblastoma cell proliferation. J Mol Biol 426, 332–346 (2014)
L.P. Yco, D. Geerts, J. Koster, A.S. Bachmann, PRAF2 stimulates cell proliferation and migration and predicts poor prognosis in neuroblastoma. Int J Oncol 42, 1408–1416 (2013)
C. Scuoppo, C. Miething, L. Lindqvist, J. Reyes, C. Ruse, I. Appelmann, S. Yoon, A. Krasnitz, J. Teruya-Feldstein, D. Pappin, J. Pelletier, S.W. Lowe, A tumour suppressor network relying on the polyamine-hypusine axis. Nature 487, 244–248 (2012)
J. Lu, Z.P. Chen, Y.P. Yan, S. Knapp, H. Schugar, K.Y. Chen, Aminohexanoic hydroxamate is a potent inducer of the differentiation of mouse neuroblastoma cells. Cancer Lett 160, 59–66 (2000)
A.D. Luchessi, T.D. Cambiaghi, S.M. Hirabara, R.H. Lambertucci, L.R. Silveira, I.L. Baptista, A.S. Moriscot, C.M. Costa-Neto, R. Curi, Involvement of eukaryotic translation initiation factor 5A (eIF5A) in skeletal muscle stem cell differentiation. J Cell Physiol 218, 480–489 (2009)
M. Preukschas, C. Hagel, A. Schulte, K. Weber, K. Lamszus, H. Sievert, N. Pallmann, C. Bokemeyer, J. Hauber, M. Braig, S. Balabanov, Expression of eukaryotic initiation factor 5A and hypusine forming enzymes in glioblastoma patient samples: implications for new targeted therapies. PLoS One 7, e43468 (2012)
J.J. Molenaar, R. Domingo-Fernandez, M.E. Ebus, S. Lindner, J. Koster, K. Drabek, P. Mestdagh, P. van Sluis, L.J. Valentijn, J. van Nes, M. Broekmans, F. Haneveld, R. Volckmann, I. Bray, L. Heukamp, A. Sprussel, T. Thor, K. Kieckbusch, L. Klein-Hitpass, M. Fischer, J. Vandesompele, A. Schramm, M.M. van Noesel, L. Varesio, F. Speleman, A. Eggert, R.L. Stallings, H.N. Caron, R. Versteeg, J.H. Schulte, LIN28B induces neuroblastoma and enhances MYCN levels via let-7 suppression. Nat Genet 44, 1199–1206 (2012)
Acknowledgments
We thank Dr. Jason Shohet (Texas Children’s Hospital, Houston, TX) and Dr. Giselle Sholler (Helen DeVos Children’s Hospital, Grand Rapids, MI) for providing neuroblastoma cell lines MYCN2 and Be(2)-C, respectively. Dr. Patrick Woster (Medical University of South Carolina, Charleston, SC) is thanked for providing us with DFMO. This work was supported by the National Cancer Institute R01 grant CA-111419 (André S. Bachmann), The Daniel K. Inouye College of Pharmacy internal funds (André S. Bachmann), the Dutch Cancer Society (“KWF Kankerbestrijding”) UVA2005-3665 (Dirk Geerts), and the European Union COST Action BM0805 (Dirk Geerts).
Conflict of interest
The authors have declared that no competing interest exists.
Author contributions
A.S.B. and A.B.. designed experiments; A.B., D.G., and J.K. performed experiments and analyzed raw data; and A.S.B., A.B.., and D.G. wrote the paper. All authors reviewed and edited the final manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bandino, A., Geerts, D., Koster, J. et al. Deoxyhypusine synthase (DHPS) inhibitor GC7 induces p21/Rb-mediated inhibition of tumor cell growth and DHPS expression correlates with poor prognosis in neuroblastoma patients. Cell Oncol. 37, 387–398 (2014). https://doi.org/10.1007/s13402-014-0201-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-014-0201-9