Abstract
Objective
To evaluate subclinical hypothyroidism in a cohort of children with Down syndrome and identify a TSH level at the time of diagnosis to predict persistent hypothyroidism.
Methods
192 children (age <3 years) with Down syndrome, registered in the Genetic Clinic of a referral tertiary care Hospital from 2010 to 2015 were evaluated with thyroid function test at initial visits and subsequently based on standard protocol. Children with subclinical hypothyroidism were evaluated at 3 years of age after discontinuation of thyroxine for 3 months.
Results
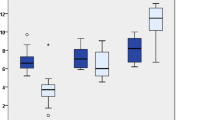
47 (24.5%) children had elevated TSH and among them 43 (91.5%) had subclinical hypothyroidism. Among the subclinical hypothyroidism group, 25 (73.5%) had transient hypothyroidism and 9 (26.5%) persistent hypothyroidism. Initial TSH level at the time of diagnosis was higher in persistent hypothyroidism group as compared to transient group (P= 0.003). The best cut-off level for prediction of persistent hypothyroidism for initial TSH level was 11.6 mIU/L.
Conclusion
Subclinical hypothyroidism, especially transient, is the commonest form of thyroid dysfunction in children with Down syndrome. The initial TSH level may help to predict the possibility of persistence of hypothyroidism.
Similar content being viewed by others
References
Kariyawasam D, Carré A, Luton D, Polak M. Down synd-rome and nonautoimmune hypothyroidisms in neonates and infants. Horm Res Paediatr. 2015;83:126–31.
Tuysuz B, Beker DB. Thyroid dysfunction in children with Down syndrome. Acta Paediatr. 2001;90:1389–93.
Iughetti L, Predieri B, Bruzzi P, Predieri F, Vellani G, Madeo SF, et al. Ten-year longitudinal study of thyroid function in children with Down’s syndrome. Horm Res Paediatr. 2014;82:113–21.
Seshadri KG. Subclinical hypothyroidism in children. Indian J Endocrinol Metab. 2012;16:S156–8.
Unachak K, Tanpaiboon P, Pongprot Y, Sittivangkul R, Silvilairat S, Dejkhamron P, et al. Thyroid functions in children with Down syndrome. J Med Assoc Thai. 2008;91:56–61.
Dayal D, Jain P, Panigrahi I, Bhattacharya A, Sachdeva N. Thyroid dysfunction in Indian children with Down syndrome. Indian Pediatr. 2014;51:751–2.
Claret C, Goday A, Benaiges D, Chillarón JJ, Flores JA, Hernandez E, et al. Subclinical hypothyroidism in the first years of life in patients with Down syndrome. Pediatr Res. 2013;73:674–8.
Kowalczyk K, Pukaj³o K, Malczewska A, Król-Chwastek A, Barg E. L-thyroxine therapy and growth processes in children with Down syndrome. Adv Clin Exp Med. 2013;22:85–92.
Bull MJ. Committee on Genetics, Health Supervision for Children with Down Syndrome. Pediatrics. 2011;128: 393–406.
The Association of Clinical Biochemistry. UK Guidelines for the Use of Thyroid Function Tests, 2006. Available from: https://doi.org/www.british-thyroid-association.org. Accessed November 01, 2017.
Dias VMA, Nunes JCR, Araújo SS, Goulart EMA. Etiological assessment of hyperthyrotropinemia in children with Down’s syndrome. J Pediatr (Rio J). 2005;81:79–84.
Selikowitz M. A five-year longitudinal study of thyroid function in children with Down syndrome. Dev Med Child Neurol. 1993;35:396–401.
Gibson PA, Newton RW, Selby K, Price DA, Leyland K, Addison GM. Longitudinal study of thyroid function in Down’s syndrome in the first two decades. Arch Dis Child. 2005;90:574–8.
Konings CH, van Trotsenburg AS, Ris-Stalpers C, Vulsma T, Wiedijk BM, de Vijlder JJ. Plasma thyrotropin bioactivity in Down’s syndrome children with subclinical hypothyroidism. Eur J Endocrinol. 2001;144:1–4.
Van Trotsenburg AS, Kempers MJ, Endert E, Tijssen JG, de Vijlder JJ, Vulsma T. Trisomy 21 causes persistent congenital hypothyroidism presumably of thyroidal origin. Thyroid. 2006;16:671–80.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sankar, H.V., Anjukrishna, K. & Riaz, I. Thyroid Stimulating Hormone Level at Diagnosis as a Predictor of Persistent Subclinical Hypothyroidism in Children with Down Syndrome. Indian Pediatr 55, 576–578 (2018). https://doi.org/10.1007/s13312-018-1300-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-018-1300-x