Abstract
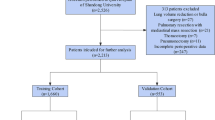
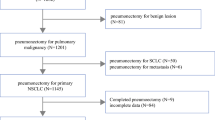
The goal of the study is to evaluate the different risk factors and stratify the patients, before the surgery, into distinct risk classes. We retrospectively reviewed pre, peri, and postoperative outcomes of 366 consecutive patients who underwent pneumonectomy for lung cancer between the last 10 years (2009–2019). We classified the patients into four classes, depending on preoperative assessments. Differences between groups were assessed with the log-rank test. Multivariable Cox proportional hazards regression analysis was used to assess the independent prognostic significance of the variables associated with the development of BPF at univariate analysis. Finally, we performed non-linear [artificial neural network (ANN)] multiple regression analyses. All tests were two-sided, and p values < 0.05 were considered significant. Fifty-one patients (13.9%) out of 366 developed BPF. Male sex (p = 0.048), right side (p = 0.015), postoperative pulmonary complications (p = 0.0139) and adjuvant treatments (p = 0.0169) were the independent predicting factors of fistulas in multivariate analysis. The right side (p = 0.043) and adjuvant treatments (p = 0.032) were the independent predicting factors of BPF after the ANN analysis. Based on multivariate and artificial neural network analysis and our experience, we observed a trend of growing risk of BPF in the first 4 weeks (early fistula), considering the four classes. Preoperative differentiation of the patients into four risk classes could allow a correct stratification of the growing risk of developing early BPF. This information could be significant to share with patients and the other physicians during the decision-making process, to minimise the risk of BPF.


Similar content being viewed by others
References
Schussler O, Alifano M, Dermine H et al (2006) Postoperative pneumonia after major lung resection. Am J Respir Crit Care Med 173:1161–1169
Algar FJ, Alvarez A, Salvatierra A et al (2003) Predicting pulmonary complications after pneumonectomy for lung cancer. Eur J Cardiothorac Surg 23:201–208
Groth SS, Burt BM, Sugarbaker DJ (2015) Management of complications after pneumonectomy. Thorac Surg Clin 25:335–348
Janet-Vendroux A, Loi M, Bobbio A et al (2020) Which is the role of pneumonectomy in the era of parenchymal sparing procedures? Early/long-term survival and functional results of a single-center experience. Lung Shanghai Chest 2015(193):965–973
McManigle JE, Fletcher GL, Tenholder MF (1990) Bronchoscopy in the management of bronchopleural fistula. Chest 97:1235–1238
Cerfolio RJ (2001) The incidence, etiology and prevention of postresectional bronchopleural fistula. Semin Thorac Cardiovasc Surg 13:3–7
Sirbu H, Busch T, Aleksic I et al (2001) Bronchopleural fistula in the surgery of non-small cell lung cancer: incidence, risk factors and management. Ann Thorac Cardiovasc Surg 7:330–336
Haraguchi S, Koizumi K, Hioki M et al (2006) Analysis of risk factors for postpneumonectomy bronchopleural fistulas in patients with lung cancer. J Nippon Med Sch 73:314–319
Turk AE, Karanas YL, Cannon W et al (2000) Stage closure of complicated bronchopleural fistulas. Ann Plastic Surg 45:560–564
Mazzella A, Pardolesi A, Maisonneuve P et al (2018) Bronchopleural fistula after pneumonectomy: risk factors and management, focusing on open-window thoracostomy. Semin Thorac Cardiovasc Surg 30:104–113
Vandenbroucke JP, von Elm E, Altman DG et al (2014) Strengthening the reporting of observational studies in epidemiology (STROBE): explanation and elaboration. Int J Surg 12:1500–1524
R Core Team (2013) R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. URL http://www.R-project.org/. RStudio Team (2020). RStudio: Integrated Development for R. RStudio, PBC, Boston, MA URL http://www.rstudio.com/
Neural designer, data mining and learning analytics tools. Edutech wiki. May 2015
Cerfolio RJ (2001) The incidence, etiology, and prevention of postresectional bronchopleural fistula. Semin Thorac Cardiovasc Surg 13:3–7
Mammana M, Marulli G, Zuin A, Perissinotto E, Comacchio GM, De Franceschi E, Rea F (2020) Postpneumonectomy bronchopleural fistula: analysis of risk factors and the role of bronchial stump coverage. Surg Today 50:114–212
Haraguchi S, Koizumi K, Hioki M, Hirata T, Hirai K, Mikami I, Kubokura H, Enomoto Y, Kinoshita H, Shimizu K (2006) Analysis of risk factors for postpneumonectomy bronchopleural fistulas in patients with lung cancer. J Nippon Med Sch 73:314–319
Sfyridis PG, Kapetanakis EI, Baltayiannis NE et al (2007) Bronchial stump buttressing with an intercostal muscle flap in diabetic patients. Ann Thorac Surg 84:967–971
McManus LM, Bloodworth RC, Prihoda TJ, Blodgett JL, Pinckard RN (2001) Agonist-dependent failure of neutrophil function in diabetes correlates with extent of hyperglycemia. J Leukoc Biol 70:395–404
Furnary AP, Zerr KJ, Grunkemeier GL, Starr A (1999) Continuous intravenous insulin infusion reduces the incidence of deep sternal wound infection in diabetic patients after cardiac surgical procedures. Ann Thorac Surg 67:352–360
Li S, Fan J, Liu J et al (2016) Neoadjuvant therapy and risk of bronchopleural fistula after lung cancer surgery: a systematic meta-analysis of 14,912 patients. Jpn J Clin Oncol 46:534–546
Zakkar M, Kanagasabay R, Hunt I (2014) No evidence that manual closure of the bronchial stump has a lower failure rate than mechanical stapler closure following anatomical lung resection. Interact Cardiovasc Thorac Surg 18:488–493
Di Maio M, Perrone F, Deschamps C, Rocco G (2015) A meta-analysis of the impact of bronchial stump coverage on the risk of bronchopleural fistula after pneumonectomy. Eur J Cardiothorac Surg 48:196–200
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Research involving human participants and/or animals
The research was conducted according to recommendations outlined in the Declaration of Helsinki.
Informed consent
Written informed consent to undergo the procedure and the use of clinical imaging data for scientific or educational purposes, or both, was obtained from all patients before the operation.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mazzella, A., Bertolaccini, L., Sedda, G. et al. Pneumonectomy and broncho-pleural fistula: predicting factors and stratification of the risk. Updates Surg 74, 1471–1478 (2022). https://doi.org/10.1007/s13304-022-01290-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-022-01290-w