Abstract
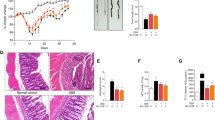
As controversy exists about the efficacy of substance P (SP) in treating ulcerative colitis (UC) with no previous study highlighting the impact of SP on mitochondrial dysfunction in this diseased condition, it became logical to perform the present study. C57BL/6 J mice were administered with DSS @ 3.5%/gm body weight for 3 cycles of 5 days each followed by i.v. dose of SP @ 5nmole per kg for consecutive 7 days. Histopathological features were noticed in the affected colon along with colonic mitochondrial dysfunction, alterations in mitochondrial stress variables and enhanced colonic cell death. Interestingly, SP failed to reverse colitic features and proved ineffective in inhibiting mitochondrial dysfunction. Unexpectedly SP alone seemed to impart detrimental effects on some of the mitochondrial functions, enhanced lipid peroxidation and increased staining intensities for caspases 3 and 9 in the normal colon. To substantiate in vivo findings and to assess free radical scavenging property of SP, Caco-2 cells were exposed to DSS with or without SP in the presence and absence of specific free radical scavengers and antioxidants. Interestingly, in vitro treatment with SP failed to restore mitochondrial functions and its efficacy proved below par compared to SOD and DMSO indicating involvement of O2•− and •OH in the progression of UC. Besides, catalase, L-NAME and MEG proved ineffective indicating non-involvement of H2O2, NO and ONOO− in UC. Thus, SP may not be a potent anti-colitogenic agent targeting colonic mitochondrial dysfunction for maintenance of colon epithelial tract as it lacks free radical scavenging property.








Similar content being viewed by others
References
Aleksandra NA, Nederby NJ, Schmedes A et al (2005) Saliva Interleukin-6 in patients with inflammatory bowel disease. Scand J Gastroenterol 40:1444–1448. https://doi.org/10.1080/00365520510023774
Bang R, Biburger M, Neuhuber WL et al (2004) Neurokininreceptor antagonists protect mice from CD95- and TNF {alpha}-mediated apoptotic liver damage. J Pharmacol Exp Ther 308:926–934. https://doi.org/10.1124/jpet.103.059329
Bar F, Bochmann W, Widok A et al (2013) Mitochondrial gene polymorphisms that protect mice from colitis. Gastroenterol 145:1055–1063. https://doi.org/10.1053/j.gastro.2013.07.015
Berridge MV, Tan AS (1993) Characterization of the cellular reduction of 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT): subcellular localization, substrate dependence, and involvement of mitochondrial electron transport in MTT reduction. Arch Biochem Biophys 303:474–482. https://doi.org/10.1006/abbi.1993.1311
Block ML, Li G, Qin L et al (2006) Potent regulation of microglia-derived oxidative stress and dopaminergic neuron survival: substance P vs. dynorphin. FASEB J 20:251–258. https://doi.org/10.1096/fj.05-4553com
Bockmann S (2002) Substance P (NK(1)) receptor expression by human colonic epithelial cell line Caco-2. Peptides 23:1783–1791. https://doi.org/10.1016/s0196-9781(02)00135-3
Castro-Obregon S, Del RG, Chen SF, Swanson RA, Frankowski H, Rao RV, Stoka V, Vesce S, Nicholls DG, Bredesen DE (2002) A ligand-receptor pair that triggers a non-apoptotic form of programmed cell death. Cell Death Differ 9:807–817
Cui L, Locatelli L, Xie MY (1997) Effect of nucleoside analogs on neurite regeneration and mitochondrial DNA synthesis in PC12 cells. J Pharmacol Exp Therapeut 280:1228–12234 (PMID: 9067308)
Cuzzocrea S, Zingarelli B, Hake P et al (1998) Antiinflammatory effects of mercaptoethylguanidine, a combined inhibitor of nitric oxide synthase and peroxynitrite scavenger, in carrageenan-induced models of inflammation. Free Radic Biol Med 24:450–459. https://doi.org/10.1016/s0891-5849(97)00280-3
Dae YH, Suna K, Hyun SH (2017) Substance-P ameliorates dextran sulfate[1]induced intestinal damage by preserving tissue barrier function. Tissue Eng Regen Med 15(1):63–73
Engel MA, Leffler A, Niedermirtl F et al (2011) TRPA1 and substance P mediate colitis in mice. Gastroenterol 141:1346–1358. https://doi.org/10.1053/j.gastro.2011.07.002
Fujino S, Andoh A, Bamba S et al (2003) Increased expression of interleukin 17 in inflammatory bowel disease. Gut 52:65–70. https://doi.org/10.1136/gut.52.1.65
Habeeb AF (1972) Reaction of protein sulfhydryl groups with Ellman’s reagent. Methods Enzymol 25:457–464. https://doi.org/10.1016/S0076-6879(72)25041-8
Hahn WS, Kuzmicic J, Burrill JS et al (2014) Proinflammatory cytokines differentially regulate adipocyte mitochondrial metabolism, oxidative stress, and dynamics. Am J physiol Endocrinol Metab 306:E1033–E1045. https://doi.org/10.1152/ajpendo.00422.2013
Hatefi Y (1978) Preparation and properties of NADH: Ubiquinone oxidoreductase (complex I), EC 1.6.5.3. Methods Enzymol 53:11–14. https://doi.org/10.1016/S0076-6879(78)53006-1
Hokari R, Lee H, Crawley SC et al (2005) Vasoactive intestinal peptide upregulates MUC2 intestinal mucin via CREB/ATF1. Am J Physiol Gastrointest Liver Physiol 289:G949–G959. https://doi.org/10.1152/ajpgi.00142.2005
Hwang DY, Kim S, Hong HS (2017) Substance-P Ameliorates Dextran Sodium Sulfate-Induced Intestinal Damage by Preserving Tissue Barrier Function. Tissue Eng Regen Med 15:63–73. https://doi.org/10.1007/s13770-017-0085-7
Jackson DN, Theiss AL (2019) Gut bacteria signaling to mitochondria in intestinal inflammation and cancer. Gut microbes 11:285–304. https://doi.org/10.1080/19490976.2019.1592421
Johnson EC, Shafer OT, Trigg JS, Park J, Schooley DA, Dow JA, Taghert PH (2005) A novel diuretic hormone receptor in Drosophila: evidence for conservation of CGRP signaling. J Exp Biol 208:1239–1246
Kang MH, Kim DY, Yi JY et al (2009) Substance P accelerates intestinal tissue regeneration after gamma-irradiation-induced damage. Wound Repair Regen 17:216–223. https://doi.org/10.1111/j.1524-475X.2009.00456.x
Khan FH, Sen T, Maiti AK et al (2005) Inhibition of rat brain mitochondrial electron transport chain activity by dopamine oxidation products during extended in vitro incubation: Implications in Parkinson’s disease. Biochim Biophys Acta 1741:65–74. https://doi.org/10.1016/j.bbadis.2005.03.013
Kim J, Xu M, Xo R et al (2010) Mitochondrial DNA damage is involved in apoptosis caused by pro-inflammatory cytokines in human OA chondrocytes. Osteoarthr cartel 18:424–432. https://doi.org/10.1016/j.joca.2009.09.008
Kitazawa M, Anantharam V, Kanthasamy A et al (2004) Dieldrin promotes proteolytic cleavage of poly (ADPribose) polymerase and apoptosis in dopaminergic cells: protective effect of mitochondrial anti-apoptotic protein Bcl-2. Neurotoxicol 25:589–598. https://doi.org/10.1016/j.neuro.2003.09.014
Komatsu M, Kobayashi D, Saito K et al (2001) Tumor necrosis factor-alpha in serum of patients with inflammatory bowel disease as measured by a highly sensitive immuno-PCR. Clin Chem 47:1297–1301
Koon HW, Zhao D, Zhan Y et al (2007) Substance P mediates antiapoptotic responses in human colonocytes by Akt activation. Proc Natl Acad Sci U S A 104:2013–2018. https://doi.org/10.1073/pnas.0610664104
Levine RL, Garland D, Oliver CN et al (1990) Determination of carbonyl content in oxidatively modified proteins. Methods Enzymol 186:464–478. https://doi.org/10.1016/0076-6879(90)86141-h
Liu N, Wang LH, Guo LL et al (2013) Chronic restraint stress inhibits hair growth via substance P mediated by reactive oxygen species in mice. PLoS ONE 8:e61574. https://doi.org/10.1371/journal.pone.0061574
Lordal M, Soder O, Hellstrom PM (1997) Tachykinins stimulate lipid peroxidation mediated by free radicals in gastrointestinal tract of rat. Dig Dis Sci 42:1524–1529. https://doi.org/10.1023/a:1018835314834
Love JR, Irvine EJ, Fedorak RN (1992) Quality of life in inflammatory bowel disease. J Clin Gastroenterol 14:15–19. https://doi.org/10.1097/00004836-199201000-00005
Lowry OH, Rosebrough NJ, Far AL et al (1951) Protein measurement with Folin-Phenol reagent. J Biol Chem 193:265–275 (PMID: 14907713)
Maiti AK, Sharba S, Navabi N et al (2015) Colonic levels of Vasoactive Intestinal Peptide decrease during infection and exogenous VIP protects epithelial mitochondria against the detrimental effects of TNFα and IFNγ induced during Citrobacter rodentium infection. PLoS ONE 13:e0204567. https://doi.org/10.1371/journal.pone.0204567
Maiti AK, Spoorthi BC, Saha NC et al (2018) Mitigating peroxynitrite mediated mitochondrial dysfunction in aged rat brain by mitochondria-targeted antioxidant MitoQ. Biogerontol 19:271–286. https://doi.org/10.1007/s10522-018-9756-6
Maiti AK, Saha NC, More SS, Panigrahi AK, Paul G (2017) Neuroprotective efficacy of mitochondrial antioxidant MitoQ in suppressing peroxynitrite mediated mitochondrial dysfunction inflicted by lead toxicity in rat brain. Neurotox Res 31:358–372
Nielsen S, Larance B, Degenhardt L, Gowing L, Kehler C, Lintzeris N (2016) Opioid agonist treatment for pharmaceutical opioid dependent people. Cochrane Database Syst Rev 5
Noguchi M, Hiwatashi N, Liu Z et al (1998) Secretion imbalance between tumor necrosis factor and its inhibitor in inflammatory bowel disease. Gut 43:203–209. https://doi.org/10.1136/gut.43.2.203
O’Connor TM, O’Connell J, O’Brien DI et al (2004) The role of substance P in inflammatory disease. J Cell Physiol 201:167–180. https://doi.org/10.1002/jcp.20061
Ohkawa H, Ohishi N, Yagi K (1979) Assay for lipid peroxides in animal tissues by thiobarbituric acid reaction. Analytical Biochem 95:351–358. https://doi.org/10.1016/0003-2697(79)90738-3
Podolsky DK (2002) Inflammatory bowel disease. N Engl J Med 347:417–429. https://doi.org/10.1056/NEJMra020831
Rehman A, Whiteman M, Halliwell B (1997) Scavenging of hydroxyl radicals but not of peroxynitrite by inhibitors and substrates of nitric oxide synthases. Br J Pharmacol 122:1702–1706. https://doi.org/10.1038/sj.bjp.0701556
Sands BE (2000) Therapy of inflammatory bowel disease Gastroenterol 118:S68–S82. https://doi.org/10.1016/s0016-5085(00)70007-2
Santhanam S, Venkatraman A, Ramakrishna BS (2007) Impairment of mitochondrial acetoacetyl CoA thiolase activity in the colonic mucosa of patients with ulcerative colitis. Gut 56:1543–1549. https://doi.org/10.1136/gut.2006.108449
Santhanam S, Rajamanickam S, Motamarry A et al (2012) Mitochondrial electron transport chain complex dysfunction in the colonic mucosa in ulcerative colitis. Inflamm Bowel Dis 18:2158–2168. https://doi.org/10.1002/ibd.22926
Sifroni KG, Damiani CR, Stoffel C et al (2010) Mitochondrial respiratory chain in the colonic mucosal of patients with ulcerative colitis. Mol Cell Biochem 342:111–115. https://doi.org/10.1007/s11010-010-0474-x
Stucchi AF, Shofer S, Leeman S et al (2000) NK-1 antagonist reduces colonic inflammation and oxidative stress in dextran sulfate-induced colitis in rats. Am J Physiol Gastrointest Liver Physiol 279:G1298–G1306. https://doi.org/10.1152/ajpgi.2000.279.6.G1298
Szabo C, Ferrer-Sueta G, Zingarelli B et al (1997) Mercaptoethylguanidine and guanidine inhibitors of nitric-oxide synthase react with peroxynitrite and protect against peroxynitrite-induced oxidative damage. J Biol Chem 272:9030–9036. https://doi.org/10.1074/jbc.272.14.9030
Wharton DC, Tzagaloff TA (1967) Cytochrome oxidase from beef heart mitochondria. Methods Enzymol 10:245–250. https://doi.org/10.1016/0076-6879(67)10048-7
Yamaguchi K, Kumakura S, Murakami T et al (2017) Ketamine suppresses the substance P-induced production of IL-6 and IL-8 by human U373MG glioblastoma/astrocytoma cells. Int J Mol Med 39:687–692. https://doi.org/10.3892/ijmm.2017.2875
Yermolaieva O, Xu R, Schinstock C et al (2004) Methionine sulfoxide reductase A protects neuronal cells against brief hypoxia/reoxygenation. Proc Natl Acad Sci U S A 101:1159–1164. https://doi.org/10.1073/pnas.0308215100
Yoshihara K, Yajima T, Kubo C et al (2006) Role of interleukin 15 in colitis induced by dextran sulphate sodium in mice. Gut 55:334–341. https://doi.org/10.1136/gut.2005.076000
Zhang YZ, Li YY (2014) Inflammatory bowel disease: pathogenesis. World J Gastroenterol 20:91–99. https://doi.org/10.3748/wjg.v20.i1.91
Acknowledgements
The authors are thankful to the Department of Science and Technology (DST), New Delhi, India, for funding this research (Sanctioned No. EMR/SERB/2016/001981).
Funding
Department of Science and Technology (DST), New Delhi, India (Grant No. EMR/SERB/2016/001981).
Author information
Authors and Affiliations
Contributions
Spoorthi B. C. (S.B.C); Shashwati Ghosh (S.G); Ishita Saha (I.S); Sunil S More (S.S.M); Gautham S.A (G.S.A); Arpan K Maiti (A.K.M). S.B.C, S.G, I.S, S.S.M and A.K.M were involved in bench work and performed the experiments. S.B.C, G.S.A, S.S.M and A.K.M designed the work and involved in conceptualization. All authors supported technically. A.K.M provided financial assistance. S.B.C, S.S.M and A.K.M interpreted data and wrote the manuscript, and all authors reviewed it.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest in the publication.
Ethical issue
All experimental protocols were permitted by the ethical committee of animal care and use of Dayananda Sagar University, Bengaluru, Karnataka, India (Registration No. 606/02/C/CPCSEA).
Rights and permissions
About this article
Cite this article
Chandraiah, S.B., Ghosh, S., Saha, I. et al. Substance P failed to reverse dextran sulfate sodium-induced murine colitis mediated by mitochondrial dysfunction: implications in ulcerative colitis. 3 Biotech 11, 199 (2021). https://doi.org/10.1007/s13205-021-02755-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13205-021-02755-2