Abstract
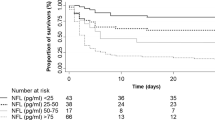
The initial clinical status after subarachnoid hemorrhage (SAH) is an important outcome predictor, but the mechanisms behind the early brain injury (EBI) remains incompletely understood. Elevated neurofilament levels in the cerebrospinal fluid at protracted stages after SAH are associated with poor outcome, but the potential association between plasma neurofilament (pNfL) levels during EBI, disease severity on admission, and poor outcome remains unaddressed. Plasma NfL (pNfL) was measured by single molecule array in 44 SAH patients on admission and 24 h after ictus, as well as in 44 controls. Disease severity on admission was assessed by validated scoring systems, and day 30 modified Rankin Scale (mRS) score was registered. Admission levels of pNfL correlated with clinical disease severity scores (rho = 0.43, p < 0.01 and rho = 0.48, p < 0.001) as well as day 30 mRS score (rho = 0.53, p < 0.001). Each quartile increase in pNfL was independently associated with poor functional status (mRS > 4) [odds ratio = 1.98, 95% confidence interval (CI): 1.01–3.88, p = 0.05]. Non-survivors had higher pNfL than survivors; on admission [17.6 pg/mL (IQR 11.4) vs. 8.4 pg/mL (IQR: 8.9), p < 0.01] and 24 h after ictus [29.9 pg/mL (IQR 90.4) vs 7.8 pg/mL (IQR 26.9), p = 0.01]. Each quartile increase in pNfL was independently associated with reduced survival rate [log-rank = 0.02, hazard ratio = 2.29 (95% CI): 1.15–4.57), p = 0.02]. PNfL levels are associated with disease severity during the EBI phase of SAH. Higher pNfL levels during EBI are associated with poor functional outcome on day 30 after ictus and increased mortality rate.



Similar content being viewed by others
References
Suarez JI, Tarr RW, Selman WR. Aneurysmal subarachnoid hemorrhage. N Engl J Med. 2006;354(4):387–96. https://doi.org/10.1056/NEJMra052732.
Alaraj A, Charbel FT, Amin-Hanjani S. Peri-operative measures for treatment and prevention of cerebral vasospasm following subarachnoid hemorrhage. Neurol Res. 2009;31(6):651–9. https://doi.org/10.1179/174313209x382395.
Bederson JB, Connolly ES Jr, Batjer HH, Dacey RG, Dion JE, Diringer MN, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: a statement for healthcare professionals from a special writing group of the stroke council, American Heart Association. Stroke. 2009;40(3):994–1025. https://doi.org/10.1161/strokeaha.108.191395.
Etminan N, Vergouwen MD, Ilodigwe D, Macdonald RL. Effect of pharmaceutical treatment on vasospasm, delayed cerebral ischemia, and clinical outcome in patients with aneurysmal subarachnoid hemorrhage: a systematic review and meta-analysis. Journal of cerebral blood flow and metabolism : official journal of the International Society of Cerebral Blood Flow and Metabolism. 2011;31(6):1443–51. https://doi.org/10.1038/jcbfm.2011.7.
Macdonald RL, Higashida RT, Keller E, Mayer SA, Molyneux A, Raabe A, et al. Randomized trial of clazosentan in patients with aneurysmal subarachnoid hemorrhage undergoing endovascular coiling. Stroke. 2012;43(6):1463–9. https://doi.org/10.1161/strokeaha.111.648980.
Frontera JA, Ahmed W, Zach V, Jovine M, Tanenbaum L, Sehba F, et al. Acute ischaemia after subarachnoid haemorrhage, relationship with early brain injury and impact on outcome: a prospective quantitative MRI study. J Neurol Neurosurg Psychiatry. 2015;86(1):71–8. https://doi.org/10.1136/jnnp-2013-307313.
Rowland MJ, Hadjipavlou G, Kelly M, Westbrook J, Pattinson KT. Delayed cerebral ischaemia after subarachnoid haemorrhage: looking beyond vasospasm. Br J Anaesth. 2012;109(3):315–29. https://doi.org/10.1093/bja/aes264.
Brisman JL, Song JK, Newell DW. Cerebral aneurysms. N Engl J Med. 2006;355(9):928–39. https://doi.org/10.1056/NEJMra052760.
Sehba FA, Pluta RM, Zhang JH. Metamorphosis of subarachnoid hemorrhage research: from delayed vasospasm to early brain injury. Mol Neurobiol. 2011;43(1):27–40. https://doi.org/10.1007/s12035-010-8155-z.
Khalil M, Teunissen CE, Otto M, Piehl F, Sormani MP, Gattringer T, et al. Neurofilaments as biomarkers in neurological disorders. Nat Rev Neurol. 2018;14(10):577–89. https://doi.org/10.1038/s41582-018-0058-z.
Lu CH, Macdonald-Wallis C, Gray E, Pearce N, Petzold A, Norgren N, et al. Neurofilament light chain: a prognostic biomarker in amyotrophic lateral sclerosis. Neurology. 2015;84(22):2247–57. https://doi.org/10.1212/wnl.0000000000001642.
Lycke JN, Karlsson JE, Andersen O, Rosengren LE. Neurofilament protein in cerebrospinal fluid: a potential marker of activity in multiple sclerosis. J Neurol Neurosurg Psychiatry. 1998;64(3):402–4.
Moseby-Knappe M, Mattsson N, Nielsen N, Zetterberg H, Blennow K, Dankiewicz J, et al. Serum neurofilament light chain for prognosis of outcome after cardiac arrest. JAMA Neurol. 2019;76(1):64–71. https://doi.org/10.1001/jamaneurol.2018.3223.
Rosen H, Karlsson JE, Rosengren L. CSF levels of neurofilament is a valuable predictor of long-term outcome after cardiac arrest. J Neurol Sci. 2004;221(1–2):19–24. https://doi.org/10.1016/j.jns.2004.03.003.
Shahim P, Gren M, Liman V, Andreasson U, Norgren N, Tegner Y, et al. Serum neurofilament light protein predicts clinical outcome in traumatic brain injury. Sci Rep. 2016;6:36791. https://doi.org/10.1038/srep36791.
Shahim P, Zetterberg H, Tegner Y, Blennow K. Serum neurofilament light as a biomarker for mild traumatic brain injury in contact sports. Neurology. 2017;88(19):1788–94. https://doi.org/10.1212/wnl.0000000000003912.
Nylen K, Csajbok LZ, Ost M, Rashid A, Karlsson JE, Blennow K, et al. CSF -neurofilament correlates with outcome after aneurysmal subarachnoid hemorrhage. Neurosci Lett. 2006;404(1–2):132–6. https://doi.org/10.1016/j.neulet.2006.05.029.
Petzold A, Keir G, Kay A, Kerr M, Thompson EJ. Axonal damage and outcome in subarachnoid haemorrhage. J Neurol Neurosurg Psychiatry. 2006;77(6):753–9. https://doi.org/10.1136/jnnp.2005.085175.
Petzold A, Rejdak K, Belli A, Sen J, Keir G, Kitchen N, et al. Axonal pathology in subarachnoid and intracerebral hemorrhage. J Neurotrauma. 2005;22(3):407–14. https://doi.org/10.1089/neu.2005.22.407.
Van Geel WJ, Rosengren LE, Verbeek MM. An enzyme immunoassay to quantify neurofilament light chain in cerebrospinal fluid. J Immunol Methods. 2005;296(1–2):179–85. https://doi.org/10.1016/j.jim.2004.11.015.
Zanier ER, Refai D, Zipfel GJ, Zoerle T, Longhi L, Esparza TJ, et al. Neurofilament light chain levels in ventricular cerebrospinal fluid after acute aneurysmal subarachnoid haemorrhage. J Neurol Neurosurg Psychiatry. 2011;82(2):157–9. https://doi.org/10.1136/jnnp.2009.177667.
Lewis SB, Wolper RA, Miralia L, Yang C, Shaw G. Detection of phosphorylated NF-H in the cerebrospinal fluid and blood of aneurysmal subarachnoid hemorrhage patients. Journal of cerebral blood flow and metabolism : official journal of the International Society of Cerebral Blood Flow and Metabolism. 2008;28(6):1261–71. https://doi.org/10.1038/jcbfm.2008.12.
Kuhle J, Barro C, Andreasson U, Derfuss T, Lindberg R, Sandelius A, et al. Comparison of three analytical platforms for quantification of the neurofilament light chain in blood samples: ELISA, electrochemiluminescence immunoassay and Simoa. Clin Chem Lab Med. 2016;54(10):1655–61. https://doi.org/10.1515/cclm-2015-1195.
Sandgaard E, Troldborg A, Lauridsen SV, Gyldenholm T, Thiel S, Hvas AM. Changes in the Lectin pathway following Intracerebral or spontaneous subarachnoid hemorrhage. Mol Neurobiol. 2019;56(1):78–87. https://doi.org/10.1007/s12035-018-1066-0.
Lauridsen SV, Hvas CL, Sandgaard E, Gyldenholm T, Mikkelsen R, Obbekjaer T, et al. Thromboelastometry shows early Hypercoagulation in patients with spontaneous subarachnoid hemorrhage. World neurosurgery. 2019. https://doi.org/10.1016/j.wneu.2019.06.019.
Poesen K, De Schaepdryver M, Stubendorff B, Gille B, Muckova P, Wendler S, et al. Neurofilament markers for ALS correlate with extent of upper and lower motor neuron disease. Neurology. 2017;88(24):2302–9. https://doi.org/10.1212/wnl.0000000000004029.
Contributors
CVBH, AMH, and TP contributed to the conception and design of the study. CVBH, TG, SVL, NS, AMH, and TP contributed to the acquisition and analysis of data. All authors drafted/revised the manuscript for its intellectual content, approved the final version, and agreed to be accountable for all aspects of the work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding Information
The study was funded by “Laege Sofus Carl Emil Friis og Hustru Olga Doris Friis Legat”; “Grosserer L.F. Foghts Foundation (grant number 21.342),” and the AP Moller Foundation (grant number 17-L0027). CVBH received a scholarship from the Health Research Fund of Central Denmark Region.
Conflict of Interest
None of the authors have any conflicts of interest regarding the present paper but have the following general conflicts of interest: Anne-Mette Hvas has received a speaker’s fee from Astellas, CSL Behring, Bayer, Bristol-Myers Squibb, and Leo Pharma and unrestricted research support from Octapharma, CSL Behring, and Leo Pharma.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
The study was approved by the Regional Ethical Committee of Central Denmark Region (1–10–72-95-14, version 7, 02102017 and 1–10–72-94-14, version 7, 05102017) and the National Data Protection Agency (1–16–02-225-14 and 1–16–02-224-14).
Informed Consent
Written informed consent was obtained from all individual participants included in the study or from their legal representative.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hviid, C.V.B., Lauridsen, S.V., Gyldenholm, T. et al. Plasma Neurofilament Light Chain Is Associated with Poor Functional Outcome and Mortality Rate After Spontaneous Subarachnoid Hemorrhage. Transl. Stroke Res. 11, 671–677 (2020). https://doi.org/10.1007/s12975-019-00761-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-019-00761-4