Abstract
Objectives
The SARS-CoV-2 (COVID-19) pandemic is recognized as a mass traumatic event in which COVID-19-related stress (CS) can indicate other trauma- and/or stressor-related disorder. The facets of mindfulness (observing, describing, acting with awareness, nonjudging, and nonreacting) have been linked to reductions in stress-related symptoms and thus may protect against CS. We extended previous research by evaluating mindfulness facets as resilience skills negatively related to CS.
Method
Undergraduate students (n = 495) completed an online battery of questionnaires. A subsample of students endorsing clinically elevated CS (n = 165) was also evaluated. We utilized hierarchical regression to account statistically for the mindfulness facets in addition to indicators of psychological distress (e.g., negative affect, neuroticism, dissociation) and social desirability. We performed analyses twice, once in the overall sample, and once in the high CS subsample.
Results
Less observing and greater nonjudging related to reduced CS while other study variables were controlled for in the overall sample. In contrast, acting with awareness and nonjudging negatively related to CS in the subsample, but were not related to CS when we accounted for psychological-distress variables that positively related to CS in the analysis.
Conclusions
Although variables indicative of psychological distress robustly contribute to CS, observing, acting with awareness, and nonjudging may be mindfulness skills that can be targeted to buffer clinically significant CS.
Preregistration
This study was not pre-registered.
Similar content being viewed by others
The ongoing SARS-CoV-2 (COVID-19) pandemic has persisted for several years with over 43% of the total world population being infected with the virus and a true estimated mortality of over 15 million people (Barber et al., 2022). Researchers have categorized the COVID-19 pandemic as a mass traumatic event due to its scale and psychological impact (e.g., Boden et al., 2021; Solomon et al., 2021). Although the pandemic may not directly affect everyone, the term mass trauma is apt considering that many people have reported experiencing COVID-19-related stress (CS) that is indicative of other trauma- and/or stressor-related disorder (Horesh & Brown, 2020; Solomon et al., 2021).
CS can include trauma- and/or stressor-related symptoms such as intrusions (e.g., nightmares, flashbacks), avoidance, negative mood and thinking, and hyperarousal difficulties (e.g., hypervigilance, irritability) that can have detrimental effects on mental and physical health (Pacella et al., 2013). Tang et al. (2020) found that the prevalence rate of increased CS 1 month after the onset of the pandemic was 2.70% in a large sample of university students. Recent meta-analytic data determined that 31.80% of young adults (18–30 years old) experienced clinically elevated CS since the start of the pandemic (Liu et al., 2020), which could be linked to fears of contracting the virus, stress from quarantining when exposed or infected, and/or from witnessing individuals afflicted with or deceased following infection (Tang et al., 2020).
In addition to fears of dying from the virus, safety measures (e.g., quarantines, social distancing), which successfully curtailed the spread of the virus, may have inadvertently exacerbated the adverse psychological effects of the pandemic and put people at risk for CS (Brooks et al., 2020; Hossain et al., 2020; Rubin & Wessely, 2020). During the pandemic, psychological distress and related variables, such as negative emotionality and anxiety, were associated with poor quality of life and CS (Bonichini & Tremolada, 2021; Casagrande et al., 2020). Similarly, greater neuroticism, often a sign of a person’s susceptibility to distress, increased the odds of developing clinically significant CS (Di Crosta et al., 2020). High rates of pathological dissociation (44.90%) documented during the pandemic have also been linked longitudinally to increases in CS (Benzakour et al., 2021). Thus, variables associated with generalized psychological distress, namely anxiety, dissociation, negative affect, and neuroticism, may greatly contribute to high CS and are important to account for when testing relations with CS.
Moreover, how individuals cope during the pandemic may have influenced the degree to which they experienced CS. García-Batista et al. (2021) found that healthcare workers who demonstrated reduced emotion regulation and greater emotional suppression also exhibited increased stress during the pandemic. Research indicated that avoidance-based coping (e.g., substance use) was related to greater CS compared with problem-focused coping (e.g., safety planning, behavioral activation; Greene et al., 2021; Park et al., 2020). Additionally, the association between pathological personality traits and CS was fully mediated by variables relevant to coping, specifically emotion regulation and dissociation (Velotti et al., 2021). Given that coping difficulties are associated with increased stress during the pandemic, studies investigating resilience factors that facilitate coping with distress are paramount to identifying avenues for mitigating CS.
Mindfulness is a self-regulatory coping skill theorized to be well-suited for promoting resilience in the face of CS (Polizzi et al., 2020; Thompson et al., 2011). Mindfulness is defined as attending to one’s inner experiences (e.g., thoughts, emotions, sensations) purposefully in a moment-to-moment manner with nonjudgmental awareness (Kabat-Zinn, 2002). The therapeutic effect of mindfulness is well documented, with evidence supporting mindfulness-based interventions as being effective at alleviating trauma- and/or stressor-related disorders (e.g., Hopwood & Schutte, 2017; Schumer et al., 2018; Sun et al., 2021). Mindfulness may reduce stress following mass traumas by counteracting avoidance of inner experiences, which can enhance coping via an improved ability to identify, regulate, and tolerate distressing stimuli (e.g., Aliche et al., 2021; Thompson et al., 2011; Williston et al., 2021). The purposeful and nonjudgmental awareness central to mindfulness may bolster psychological well-being when external circumstances present an uncontrollable situation, such as a global pandemic (Klainin-Yobas et al., 2016).
Given that mindfulness is consistently related to reductions in stress, researchers have investigated mindfulness as a protective coping mechanism during the COVID-19 pandemic (e.g., Jones et al., 2019). For example, Conversano et al. (2020) reported that dispositional mindfulness exhibited strong negative associations with psychological distress and symptoms due to the pandemic, and Zhu et al. (2021) found that mindfulness practitioners endorsed lower levels of pandemic-related distress (e.g., depression, anxiety) compared with non-practitioners. Furthermore, Liu et al. (2023) determined that state mindfulness moderated the relation between the subjective severity of the pandemic and CS such that this association was negative at higher levels of state mindfulness and positive at lower levels. Mindfulness may also help individuals flexibly identify and engage in preventive health behaviors that curb the spread of COVID-19 (e.g., social distancing, handwashing) and decrease residual anxiety (Haliwa et al., 2020; Wielgus et al., 2020). Moreover, mindfulness-based online interventions have been developed to address CS (e.g., Bossi et al., 2022).
Although prior research has provided strong support for mindfulness as a resilience strategy, which may mitigate stress during the pandemic, only one study (Boekhorst & Duijndam, 2023) to our knowledge, which was conducted simultaneously with our research, has tested if specific mindfulness skills (i.e., facets) are associated with less CS. Mindfulness is conceptualized as encompassing five facets: observing, describing, acting with awareness, nonjudging, and nonreacting (Baer et al., 2006, 2008). Researchers have emphasized investigating these facets granularly to discern which can enhance coping with stress (e.g., Martin et al., 2018). Boekhorst and Duijndam (2023) found that all mindfulness facets negatively correlated with CS, except for observing, which was not significantly correlated with CS in a large Dutch sample. They also demonstrated that describing and nonjudging were the only facets related to total CS and trauma-related CS in regression models accounting for all facets, sex, age, marital status, education level, and chronic illness. However, their models did not account for psychological-distress variables and social desirability, which can potentially influence associations with CS.
Moreover, Carpenter et al. (2019) conducted a meta-analysis that documented that most mindfulness facets, with the exception of observing, were negatively associated with affective symptoms. Thus, observing one’s inner experiences in combination with lower levels of other facets could be insufficient to impact, or may even exacerbate, stress in non-meditators (Desrosiers et al., 2013; Lilja et al., 2013; Stanley et al., 2019). Notably, acting with awareness and nonjudging have emerged as factors that robustly defend against trauma-related stress compared to the other facets (Boden et al., 2012; Owens et al., 2012). Studies involving trauma-exposed individuals indicated that increased acting with awareness and nonjudging exhibited stronger relations with fewer symptoms relative to other facets. These two facets may help people to refocus on the present moment with nonjudgmental awareness when engaging with stressful stimuli, thereby diminishing intrusions from past events and accompanying negative thoughts and emotions (Martin et al., 2018; Stephenson et al., 2017). Accordingly, testing the relation between mindfulness facets and CS may provide important implications for clinical care that can refine strategies for coping with pandemic stress to alleviate, or even prevent, other trauma- and/or stressor-related disorder.
We extend previous research by utilizing hierarchical regression models to test if mindfulness facets are related to CS, while accounting statistically for psychological-distress indicators (i.e., neuroticism, dissociation, state anxiety, negative affect) and social desirability. Importantly, our focus on individual facets allows for the identification of targeted ways to optimize mindfulness-based interventions that can promote resilience to CS. Given the consistent negative relation between mindfulness and stress, as well as the pandemic’s status as a mass trauma, we also analyzed a subsample of participants endorsing clinically elevated CS linked broadly to the pandemic to inform the clinical care of individuals diagnosed with other trauma- and/or stressor-related disorder associated with the COVID-19 pandemic (Norrholm et al., 2021). We performed analyses twice, once in the overall sample, and once in the high CS subsample.
In line with data indicating that observing is the only facet not related to CS and psychological symptoms, we hypothesized that all mindfulness facets will be negatively correlated with CS, except for observing, which will not be significantly associated with CS in both the overall sample and high CS subsample. Furthermore, we predicted that describing, acting with awareness, nonjudging, and nonreacting will be negatively related to CS in regression models accounting for all facets across both samples. Given the robust negative associations of trauma- and/or stressor-related symptoms with acting with awareness and nonjudging, we hypothesized that these facets would remain associated with CS when controlling statistically for variables indicative of psychological distress (i.e., neuroticism, dissociation, state anxiety, negative affect) and social desirability in both samples. Additionally, based on research supporting a consistent positive association between psychological distress and CS, we predicted that all psychological-distress variables will be positively correlated with CS and remain related to CS when other explanatory variables (i.e., mindfulness facets, social desirability) are accounted for in regression models across both samples.
Method
Participants
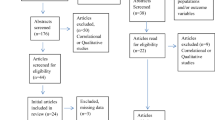
Five hundred and fifty-five undergraduate students were recruited from a large university in the Northeast United States. They then completed a battery of online questionnaires (see “Procedure” below for details). We assessed data validity using participants’ completion status, score on the Conscientious Responders Scale (CRS; Marjanovic et al., 2014), response to the primary outcome measure (i.e., whether participants skipped the entire Posttraumatic Stress Disorder Checklist for DSM-5 [PCL-5; Blevins et al., 2015], completion duration, and response style (i.e., providing the same response across multiple questionnaires). We removed participants from the study and thus excluded them from analyses for the following reasons: not completing the online survey (n = 32), having a CRS score indicating random responding (n = 5), and completing the entire online survey in less than 30 min (n = 23). After removing these participants, no individuals skipped the entire PCL-5 or used the same response across multiple measures.
Overall Sample
The resulting overall sample size was 495. This sample was mostly female (67.90% female and 32.10% male). Participants self-identified as White (69.90%), Black or African American (7.50%), Asian (20.00%), Native American or Native Alaskan (0.80%), Native Hawaiian or other Pacific Islander (0.40%), and other (4.80%). The mean age was M = 19.19 (SD = 1.08; range: 18–23). One participant did not respond to the age question.
High CS Subsample
We also analyzed a subsample of participants reporting clinically elevated CS (see “Data Analyses” below for details on how this subsample was determined). The size of the subsample was 165. The subsample was mostly female (69.70% female and 30.30% male). Participants self-identified as White (64.80%), Black or African American (11.50%), Asian (23.00%), Native American or Native Alaskan (0.60%), and other (5.50%). The mean age was M = 19.30 (SD = 1.22; range: 18–23).
Procedure
Undergraduate students participated in the study for course credit. They completed questionnaires administered through an online survey website (Qualtrics.com). All questionnaires were randomized.
Measures
PCL-5
The PCL-5 (Blevins et al., 2015) is a self-report instrument designed to assess trauma- and/or stressor-related symptoms and was used to index CS in our study. The PCL-5 has demonstrated excellent internal consistency and convergent and discriminant validity (Blevins et al., 2015). Because the present study aimed to quantify CS during the pandemic, we modified the PCL-5 instructions in the following manner to assess symptoms anchored to this global event: “For the following questions, please answer regarding your experiences with the COVID-19 global pandemic.” The PCL-5 exhibited excellent internal consistency (Cronbach’s α = 0.95) in the overall sample and good internal consistency (Cronbach’s α = 0.84) in the high CS subsample.
Five Facet Mindfulness Questionnaire (FFMQ)
The FFMQ (Baer et al., 2006) is a 39-item self-report inventory that measures mindfulness based on the five-facet model. Participants rate the extent to which each item describes them on a Likert scale from 1 (Never or very rarely true) to 5 (Very often or always true). In addition to a total score, five facet scores can be derived for Observing, Describing, Acting with Awareness, Nonjudging, and Nonreacting. The FFMQ has demonstrated positive relations with measures of meditation experience and well-being, as well as a negative relation with psychological distress (Baer et al., 2008). The FFMQ total score exhibited good internal consistency in both samples (Cronbach’s α = 0.84 in the overall sample and Cronbach’s α = 0.82 in the high CS subsample), with subscale internal consistency ranging from sufficient (Observing, Cronbach’s α = 0.75 in the high CS subsample) to excellent (Nonjudging, Cronbach’s α = 0.91 in the overall sample).
NEO Five-Factor Inventory (NEO-FFI)
The NEO-FFI (Costa & McCrae, 1992) is a self-report questionnaire that indexes personality dimensionally according to the Big Five model. Participants rate each item on a Likert scale from 1 (strongly disagree) to 5 (strongly agree). We administered only the 12-item neuroticism subscale. The NEO-FFI is a valid measure of neuroticism in university students (e.g., Anisi et al., 2012). The NEO-FFI neuroticism subscale exhibited good internal consistency (Cronbach’s α = 0.82) in the overall sample and sufficient internal consistency (Cronbach’s α = 0.71) in the high CS subsample.
Marlowe-Crowne Social Desirability Scale Form C (M-C Form C)
The M-C Form C (Reynolds, 1982) is a 13-item scale used to determine the extent to which participants represent themselves in a socially desirable way. The M-C Form C exhibited acceptable internal consistency in both samples (Cronbach’s α = 0.64 in the overall sample and Cronbach’s α = 0.63 in the high CS subsample). These internal consistency estimates were anticipated given that the M-C Form C has exhibited low internal consistency in prior research (e.g., Tan et al., 2022).
Dissociative Experiences Scale-II (DES-II)
The DES-II (Carlson & Putnam, 1993) is a 28-item self-report questionnaire that quantifies trait dissociation across absorption, depersonalization/derealization, and amnestic dissociation. Participants rate the frequency of dissociative experiences in their daily lives on a scale from 0% (never) to 100% (always). Higher scores on the DES-II are associated with dissociative psychopathology (Carlson & Putnam, 1993). The DES-II exhibited excellent internal consistency in both samples (Cronbach’s α = 0.93 in both samples). Using the established cutoff score of equal to or greater than 30 on the DES-II to determine clinically significant levels of dissociation (Carlson et al., 1993), 18.01% of participants (87 of 483) reported clinically significant dissociation in the overall sample, whereas 30.63% (49 of 160) endorsed clinically significant dissociation in the high CS subsample prior to estimating missing data.
Positive and Negative Affect Schedule (PANAS)
The PANAS (Watson et al., 1988) is a self-report measure of positive and negative affect. The 20 items assessed affect at the time of survey administration. The PANAS’s subscales have demonstrated convergent and discriminant validity with measures of general distress and dysfunction, depression, and anxiety (Watson et al., 1988). The PANAS’s positive affect subscale exhibited excellent internal consistency in both samples (Cronbach’s α = 0.91 in the overall sample and Cronbach’s α = 0.92 in the high CS subsample). The negative affect subscale demonstrated good internal consistency in both samples (Cronbach’s α = 0.89 in the overall sample and Cronbach’s α = 0.88 in the high CS subsample).
State/Trait Anxiety Inventory (STAI)
The STAI (Spielberger, 1983) is a self-report measure that indexes transient (i.e., state) and enduring (i.e., trait) expressions of anxiety. We administered only the state anxiety subscale. Participants are asked to rate 20 items from 1 (not at all) to 4 (very much so) about how they feel at the moment, with higher scores indicating more significant anxiety. The STAI’s state anxiety subscale exhibited excellent internal consistency in the overall sample (Cronbach’s α = 0.91) and good internal consistency in the high CS subsample (Cronbach’s α = 0.89).
CRS
The CRS (Marjanovic et al., 2014) identifies random response patterns in psychological-inventory data. Five items are embedded randomly throughout a survey and require participants to respond in a particular way (e.g., “Choose the first option–‘strongly disagree’–in answering this question”). Participants receive a score of one for each correctly answered item, and their score for each item is summed to derive a total CRS score. A score of two or lower accurately identifies 93% of random responders (Marjanovic et al., 2014). We used this measure as a check for data validity; participants who scored two or lower were removed from the dataset (see “Participants” above for details).
Data Analyses
We determined a high CS subsample using a cutoff score of 33 on the PCL-5. A PCL-5 score of 33 is a widely used and research-informed cut score suggestive of clinically elevated symptoms (e.g., Bovin et al., 2016). Participants with a PCL-5 score equal to or greater than this cutoff score were included in the high CS subsample.
We used SPSS Version 23 for statistical analyses and calculated total scores for all study variables, except for deriving a mean score for the DES-II. We included the M-C Form C to control for social desirability in statistical models. We first conducted Pearson correlations to test the associations between the study variables and CS as measured by the PCL-5, with the strengths of these correlations determined using Cohen’s (1988) recommendations (0.10 = weak, 0.30 = moderate, and 0.50 = strong). Next, we entered variables significantly correlated with CS into a hierarchical multiple regression analysis to determine robustness of relations. We first entered the facets of mindfulness into the hierarchical regression (Model 1), then entered variables indicative of psychological distress (e.g., neuroticism, dissociation, negative affect) into the regression (Model 2), and finally entered social desirability (Model 3). In the regression analyses, we examined suppression effects (i.e., sign flips between correlation coefficients and regression weights), tolerance, and variance inflation factor to detect any problems with multicollinearity that could lead to spurious results (Tu et al., 2008). We conducted the same set of analyses in both the overall sample and high CS subsample. Our hierarchical approach to the data analyses rigorously ascertains the incremental variance accounted for by variables in each model, which affords the opportunity to evaluate unique variance and specify interpretations of the full model. Because we analyzed the data using hierarchical regressions, we adopted a more liberal alpha level of p ≤ 0.05 to determine significance so potentially meaningful associations significant at higher p-values were not ruled out by a more conservative alpha level when multiple variables were accounted for in regression models.
Results
Missing Data
After removing participants from the study for data validity purposes, analyses revealed the presence of missing data for the M-C Form C, DES-II, FFMQ, and PANAS, with up to 2.50% missing for any single scale. Initial missing data analyses indicated that data were not missing completely at random. However, the pattern of missing data suggested that the DES-II had many high values, and the FFMQ’s Nonreacting subscale had many low values. Thus, these variables were transformed using a square root transformation for the DES-II and a square transformation for the Nonreacting subscale. Missing data analyses were then rerun and indicated that data were missing completely at random. Accordingly, we estimated missing composite scores (i.e., total and mean scores) for study measures using expectation maximization. The transformed variables were used in subsequent analyses.
Overall Sample
Table 1 presents variable descriptives and the correlations among the study variables and CS in the overall sample. Neuroticism and negative affect strongly correlated with CS (p-values < 0.001). CS moderately correlated with dissociation, mindfulness, observing, acting with awareness, nonjudging, and state anxiety (p-values < 0.001). Social desirability and describing weakly correlated with CS (p-values < 0.001). All significant correlations were in the expected direction, except observing was positively related to CS. Nonreacting (p = 0.17) and positive affect (p = 0.41) were not significantly correlated with CS.
Based on the correlations, we entered neuroticism, social desirability, dissociation, observing, describing, acting with awareness, nonjudging, negative affect, and state anxiety into a hierarchical multiple regression analysis with CS as the outcome. The FFMQ total was not entered due to potential multicollinearity issues with the individual mindfulness facets. The final model of this hierarchical regression that included all the variables revealed suppression effects for describing and state anxiety, so these variables were removed, and the analysis was rerun (Tu et al., 2008).
Table 2 presents results from the full hierarchical regression analysis in the overall sample. First, we entered the mindfulness facets (i.e., observing, acting with awareness, and nonjudging) into the regression (Model 1). This model explained a significant 31.20% of the variance in CS (p < 0.001). Within the model, less observing (p < 0.05), greater acting with awareness (p < 0.001), and greater nonjudging (p < 0.001) all significantly related to reduced CS. Next, we entered variables indicative of psychological distress into the hierarchical regression (i.e., neuroticism, dissociation, negative affect) while controlling for the mindfulness facets (Model 2). This model significantly explained an additional 16.50% of the variance in CS (p < 0.001, 47.70% total variance). Within this model, neuroticism, dissociation, and negative affect significantly related to CS in the expected directions (p-values < 0.001). Notably, observing and nonjudging remained significantly related to CS (p-values < 0.05), whereas acting with awareness was no longer significantly related to CS (p = 0.09) when psychological-distress variables were included in the regression. Finally, we entered social desirability into the regression while accounting for all other variables (Model 3). This model did not significantly explain any additional unique variance in CS (p = 0.80, 0.00% model variance, 47.70% total variance), and social desirability was not significantly related to CS (p = 0.80). All previous significant relations remained and acting with awareness was still not significantly related to CS when social desirability was included in the regression.
High CS Subsample
Table 1 presents variable descriptives and the correlations between the study variables and CS in the high CS subsample. CS moderately correlated with neuroticism, dissociation, acting with awareness, and nonjudging (p-values < 0.001). Also, CS weakly correlated with social desirability, mindfulness, observing, nonreacting, and negative affect (p-values < 0.05). All significant correlations were in the expected direction, except observing and nonreacting were positively related to CS. Describing (p = 0.42), positive affect (p = 0.52), and state anxiety (p = 0.06) were not significantly correlated with CS.
Based on the correlations, we entered neuroticism, social desirability, dissociation, observing, acting with awareness, nonjudging, nonreacting, and negative affect into a hierarchical multiple regression analysis with CS as the outcome. The FFMQ total was again not entered due to potential multicollinearity issues with the individual mindfulness facets. Table 3 presents results from the full hierarchical regression analysis in the high CS subsample. First, the mindfulness facets (i.e., observing, acting with awareness, nonjudging, nonreacting) were entered into the regression (Model 1). This model explained a significant 18% of the variance in CS (p < 0.001). Within the model, acting with awareness (p < 0.01) and nonjudging (p < 0.05) significantly related to CS in the expected directions whereas observing (p = 0.37) and nonreacting (p = 0.22) were not significantly related to CS.
Next, we entered variables indicative of psychological distress into the hierarchical regression (i.e., neuroticism, dissociation, negative affect) while controlling for the mindfulness facets (Model 2). This model significantly explained an additional 8.20% of the variance in CS (p = 0.001, 26.20% total variance). Within this model, neuroticism (p = 0.05) and dissociation (p < 0.01) significantly related to CS in the expected directions, but negative affect was not significantly related to CS (p = 0.20). Notably, none of the mindfulness facets remained significantly related to CS when psychological-distress variables were included in the regression (p-values > 0.13). Finally, we entered social desirability into the regression while accounting for all other variables (Model 3). This model did not explain significant variance in CS (p = 0.33, 0.40% model variance, 26.70% total variance), and social desirability was not significantly related to CS (p = 0.33). Dissociation was the only variable that remained significantly related to CS (p < 0.01) when social desirability was included in the regression.
Discussion
Mindfulness can be a powerful tool for helping people cope with stress during the COVID-19 pandemic. We tested facets of mindfulness as resilience strategies that may be related to reduced CS using a hierarchical regression approach while accounting statistically for indicators of psychological distress in a large undergraduate sample. Social desirability, which minimally impacted the outcome variable, was also controlled for in regression models. Notably, 33.33% of participants reported clinically elevated CS. This percentage is comparable to research documenting significant posttraumatic stress rates during the pandemic (31.80–37%; Liu et al., 2020; Park et al., 2020). Thus, over 30% of individuals appear likely to develop clinically elevated CS and likely meet criteria for other trauma- and/or stressor-related disorder. These high rates of CS further support the need to identify and evaluate evidence-based coping and intervention strategies, such as mindfulness skills, that foster resilience and reduce distress attributed to the COVID-19 pandemic (Polizzi et al., 2020).
We first interpret results from correlations to contextualize the linear associations observed in our study based on the extant literature and then interpret regression analyses to clarify nuances in these associations which we used to refine the implications of our study. In line with hypotheses, describing, acting with awareness, and nonjudging exhibited weak-to-moderate negative correlations with CS in the overall sample, and acting with awareness and nonjudging demonstrated moderate negative correlations with CS in the high CS subsample. Furthermore, larger correlation coefficients were observed for Acting with Awareness and Nonjudging relative to other facet subscales across both samples. These findings are consonant with the facet model of mindfulness and indicate that acting with awareness and nonjudging may be the mindfulness facets with greater negative associations with CS (e.g., Baer et al., 2006; Boekhorst & Duijndam, 2023; Martin et al., 2018). Also, in support of hypotheses, neuroticism, dissociation, and negative affect displayed weak-to-strong positive correlations across both samples. State anxiety and CS demonstrated a moderate positive correlation in the overall sample but did not significantly correlate with CS in the high CS subsample. Taken together, our results imply that these indicators of psychological distress may be related to increased CS that disrupt functioning during the pandemic (Bishop & Forster, 2013; Benzakour et al., 2021; Di Crosta et al., 2020).
Some correlations of mindfulness facets with CS were inconsistent with our hypotheses. Observing exhibited weak-to-moderate positive correlations with CS across both samples. Prior research has supported a weak positive association between observing and trauma and/or stressor-related symptoms (e.g., Stanley et al., 2019). This link may indicate that merely observing one’s inner experiences while maintaining low levels of the other facets, such as acting with awareness and nonjudging, could increase distress and hypervigilance during the pandemic and worsen CS in non-meditating samples (Desrosiers et al., 2013; Lilja et al., 2013; Stanley et al., 2019; Stephenson et al., 2017). Nonreacting displayed a weak positive correlation with CS in the high CS subsample. This positive association has been documented in clinical samples (e.g., Cheng et al., 2021) and could possibly be explained by nonreacting functioning as a pathway to emotional suppression that exacerbates CS, especially hyperarousal (García-Batista et al., 2021; Iani et al., 2019; Reffi et al., 2019). Additionally, nonreacting was not correlated with CS in the overall sample, and describing was not correlated with CS in the subsample. Research has supported that nonreacting and describing are negatively associated with trauma- and/or stressor-related symptomatology (e.g., Boekhorst & Duijndam, 2023; Carpenter et al., 2019). However, Hagen et al. (2016) found that facets of mindfulness, including nonreacting and describing, were not associated with posttraumatic stress symptoms in a small sample of Tsunami disaster survivors. Given that our sample is similar to participants in Hagen et al. (2016), insofar as they linked symptoms to mass traumatic events, future studies replicating our results in samples exposed to mass traumas are needed. Perhaps there is an optimal level of describing and nonreacting during a mass trauma necessary to motivate coping and other adaptive behaviors that reduce stress. Studies testing describing and nonreacting as moderators of distress during the COVID-19 pandemic are warranted (e.g., van Son et al., 2015).
Regression models chiefly supported psychological-distress variables as robust contributors to CS. These results were generally consistent with hypotheses regarding the relations between indicators of generalized psychological distress and CS. Models involving psychological-distress variables explained unique variance in CS. More specifically, neuroticism, dissociation, and negative affect were positively related to CS when statistically accounting for all study variables (i.e., mindfulness facets, psychological-distress indicators, social desirability) in the overall sample. In the high CS subsample, neuroticism and dissociation were positively associated with CS when accounting for the mindfulness facets and negative affect, but only greater dissociation was related to higher CS when controlling for all study variables. The robust relations observed between psychological-distress variables and CS support the literature implying that maladaptive processes may contribute more to trauma- and/or stressor-related diagnoses than adaptive processes (e.g., Mattson et al., 2018; Short et al., 2018). Accordingly, individuals who have a propensity to view events in negative ways (e.g., Di Crosta et al., 2020), detach from reality in response to stress (e.g., Benzakour et al., 2021), and/or experience high negative emotionality are likely at risk for greater CS during the pandemic (e.g., Bonichini & Tremolada, 2021). These processes, especially dissociation, given its consistent association with CS across both samples, may constitute maladaptive stress responses that hinder the resilience process by limiting personal resources, such as problem-focused coping and adaptive emotion regulation, and can set the stage for clinically significant CS (e.g., García-Batista et al., 2021; Greene et al., 2021; Park et al., 2020). Still, the contributions of neuroticism, dissociation, and negative affect to CS should be directly compared to other potential risk factors (e.g., trait anxiety, emotional dysregulation, avoidance) in future studies.
Although regression models including the facets of mindfulness explained unique variance in CS, they were mixed regarding our hypotheses about the facets. Less observing and greater nonjudging were associated with reduced CS in the overall sample while accounting statistically for all study variables. Thus, merely focusing on one’s inner experiences during the pandemic may be implicated in emotional over-engagement that exacerbates CS (e.g., Stanley et al., 2019). In contrast, nonjudging inner experiences may be linked to less CS in the general population, possibly via greater ability to accept and regulate emotional reactions to uncontrollable circumstances encountered during the pandemic (e.g., Boekhorst & Duijndam, 2023; Polizzi et al., 2018). In the high CS subsample, no mindfulness facets were significantly related to CS beyond indicators of psychological distress. Yet, acting with awareness and nonjudging were the only facets that negatively related to CS during the pandemic when controlling for other mindfulness facets (i.e., observing, nonreacting). These findings further support acting with awareness and nonjudging as mindfulness skills that may be particularly pertinent to reducing, or even preventing, stress in response to a mass trauma such as the COVID-19 pandemic (e.g., Boekhorst & Duijndam, 2023; Carpenter et al., 2019; Martin et al., 2018).
More broadly, results from both samples imply that maladaptive processes may mediate the relation between the mindfulness facets and CS insofar as the relations between facets and CS were weakened and/or no longer significant when distress-related variables were included in regression models. For example, nonjudgmentally staying present while engaging in deliberate actions when interacting with feared internal and external stimuli, rather than just observing or avoiding them, may mitigate clinically significant CS during the pandemic via weakened maladaptive processes (e.g., Liu et al., 2023; Thompson et al., 2011), such as reductions in neurotic tendencies (Hanley et al., 2019), dissociative experiences (D’Antoni et al., 2022), and negative affect (Roos et al., 2020). Accordingly, viewing one’s inner experience in a nonjudgmental manner in combination with intentionally identifying avenues for adaptive behaviors during the pandemic, perhaps based on personal meaning and values, may foster resilience by facilitating engagement with distressing stimuli (e.g., Haliwa et al., 2020; Martin et al., 2018; Polizzi et al., 2020). Future longitudinal studies testing this proposed mediation model are warranted to replicate and extend our findings.
In sum, our findings are applicable to individuals experiencing clinically significant CS that likely meet diagnostic criteria for other trauma- and/or stressor-related disorder. Given the preliminary nature of our study, we temper implications and emphasize that further research is needed to support our findings. Nevertheless, maladaptive processes, particularly dissociation, were robustly related to CS in regression models across both samples. Although additional research is warranted, these findings imply that assessing for these difficulties and subsequently modifying therapeutic techniques, such as mindfulness-based strategies, to target them may further bolster coping and treatment response when addressing CS. We also observed significant correlations between greater mindfulness and less CS in both samples, which preliminarily supports the use of mindfulness-based interventions to address CS (e.g., Bossi et al., 2022). These interventions may benefit from emphasizing observing, acting with awareness, and nonjudging based on results demonstrating that these facets were associated with CS in regression models. Accordingly, clinical trial research is needed to investigate how the effects of mindfulness-based treatments on distress-related variables during the pandemic can be optimized by techniques targeting observing, acting with awareness, and nonjudging to promote resilience.
Limitations and Future Research
Our study is not without its limitations. Primarily, our design was cross-sectional with a sample of undergraduate students. As our ability to draw causal inferences about associations is limited, we were careful to not conclude that participants’ posttraumatic stress symptoms were “due to” the pandemic. Rather, we, more conservatively, described our findings in terms CS generally associated with the pandemic. Also, our findings may not be fully generalizable to other samples, especially culturally diverse, trauma-exposed populations. The majority of participants self-identified their race as White, which limits the generalizability of findings to racially and ethnically diverse populations. Nevertheless, 33.33% of the present sample reported clinically elevated CS, which is comparable to rates of clinically significant posttraumatic stress symptoms during the pandemic and thus strengthens the implications of our findings (Liu et al., 2020; Park et al., 2020). Studies testing the longitudinal relations among the mindfulness facets and posttraumatic stress during the pandemic with culturally diverse, trauma-exposed samples are imperative to replicate our findings.
The PCL-5 was modified so that participants broadly linked their responses to the COVID-19 pandemic. Although the pandemic has been labeled a mass trauma (e.g., Boden et al., 2021), participants did not anchor their symptom ratings to specific criterion A events during the pandemic. Thus, we emphasize that our findings are relevant for individuals diagnosed with other trauma- and/or stressor-related disorder and not posttraumatic stress disorder because we did not assess criterion A events (Norrholm et al., 2021). Future studies distinguishing individuals’ symptom severity in response to the overall pandemic, compared with discrete pandemic-related traumatic events, may be beneficial to elucidate the clinical impact of the pandemic. Moreover, diagnoses were not confirmed with a structured interview, nor was a measure of past trauma exposure administered. Research assessing posttraumatic stress symptoms attributed to pandemic-related traumatic events using a diagnostic interview and indexing the potentially moderating role of past trauma exposure is warranted. We also did not include measures of other trauma-related variables that may impact individuals’ experience of a new traumatic event, such as past trauma exposure and trauma-related discrimination, and the influence of these variables should be examined in future research. Finally, the internal consistency of the M-C Form C was low in both samples, although it was similar to internal consistencies documented in previous studies of this measure (e.g., Tan et al., 2022).
Our study investigated the facets of mindfulness as resilience coping strategies that negatively related to CS. We utilized a hierarchical regression approach while accounting statistically for variables pertinent to psychological distress and social desirability. Findings chiefly supported psychological-distress indicators (i.e., dissociation, neuroticism) as robust contributors to clinically elevated CS broadly linked to the pandemic. However, acting with awareness and nonjudging emerged as the facets that negatively related to CS, whereas observing was positively associated with CS. Although future longitudinal studies are needed, our findings broadly imply that the facets of mindfulness can be utilized in different ways to improve functioning during the pandemic. Providing psychoeducation about observing inner experiences may help people better understand its relation to increased CS, so they are more likely to practice this skill and employ other mindfulness facets. In addition, tailoring evidence-based coping mechanisms and psychological treatments to emphasize acting with awareness and nonjudging may greatly reduce CS. These techniques could be vital to promoting resilience that defends against the development and maintenance of other trauma- and/or stressor-related disorder attributed to the COVID-19 pandemic.
Data Availability
Data is available upon request.
References
Aliche, C. J., Ifeagwazi, C. M., Mefoh, P. C., Eze, J. E., & Chukwuorji, J. C. (2021). Experiential avoidance mediates the relations between mindfulness and PTSD symptoms severity in terrorist attack survivors. Nordic Psychology, 73(2), 191–207. https://doi.org/10.1080/19012276.2020.1852953
Anisi, J., Majdiyan, M., Joshanloo, J., & Ghoharikamel, Z. (2012). Validity and reliability of NEO Five-Factor Inventory (NEO-FFI) on university students. International Journal of Behavioral Sciences, 5(4), 351–355.
Baer, R. A., Smith, G. T., Hopkins, J., Krietemeyer, J., & Toney, L. (2006). Using self-report assessment methods to explore facets of mindfulness. Assessment, 13(1), 27–45. https://doi.org/10.1177/1073191105283504
Baer, R. A., Smith, G. T., Lykins, E., Button, D., Krietemeyer, J., Sauer, S., Walsh, E., Duggan, D., & Williams, J. M. G. (2008). Construct validity of the five facet mindfulness questionnaire in meditating and nonmeditating samples. Assessment, 15(3), 329–342. https://doi.org/10.1177/1073191107313003
Barber, R. M., Sorensen, R. J., Pigott, D. M., Bisignano, C., Carter, A., Amlag, J. O., Collins, J. K., Abbafati, C., Adolph, C., Allorant, A., Aravkin, A. Y., Bang-Jensen, B. L., Castro, E., Chakrabarti, S., Cogen, R. M., Combs, E., Comfort, H., Cooperrider, K., Xiaochen, D., … & Murray, C. J. (2022). Estimating global, regional, and national daily and cumulative infections with SARS-CoV-2 through Nov 14, 2021: A statistical analysis. The Lancet, 399(10344), 2351–2380. https://doi.org/10.1016/S0140-6736(22)00484-6
Benzakour, L., Braillard, O., Mazzola, V., Gex, D., Nehme, M., Perone, S. A., Agoritsas, T., Kopp, G., Cereghetti, S., Bondolfi, G., & Lador, F. (2021). Impact of peritraumatic dissociation in hospitalized patients with COVID-19 pneumonia: A longitudinal study. Journal of Psychiatric Research, 140, 53–59. https://doi.org/10.1016/j.jpsychires.2021.05.031
Bishop, S., & Forster, S. (2013). Trait anxiety, neuroticism, and the brain basis of vulnerability to affective disorder. In J. Armony & P. Vuilleumier (Eds.), The Cambridge handbook of human affective neuroscience (pp. 553–574). Cambridge University Press. https://doi.org/10.1017/CBO9780511843716.031
Blevins, C. A., Weathers, F. W., Davis, M. T., Witte, T. K., & Domino, J. L. (2015). The Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5): Development and initial psychometric evaluation. Journal of Traumatic Stress, 28(6), 489–498. https://doi.org/10.1002/jts.22059
Boden, M. T., Bernstein, A., Walser, R. D., Bui, L., Alvarez, J., & Bonn-Miller, M. O. (2012). Changes in facets of mindfulness and posttraumatic stress disorder treatment outcome. Psychiatry Research, 200(2–3), 609–613. https://doi.org/10.1016/j.psychres.2012.07.011
Boden, M., Zimmerman, L., Azevedo, K. J., Ruzek, J. I., Gala, S., Abdel Magid, H. S., Cohen, N., Walser, R., Mahtani, N. D., Hoggatt, K. J., & McLean, C. P. (2021). Addressing the mental health impact of COVID-19 through population health. Clinical Psychology Review, 85, 102006. https://doi.org/10.1016/j.cpr.2021.102006
Boekhorst, M. G., & Duijndam, S. (2023). The association between facets of mindfulness and COVID-19 related distress: A cross-sectional study. Acta Psychologica, 233, 103826. https://doi.org/10.1016/j.actpsy.2023.103826
Bonichini, S., & Tremolada, M. (2021). Quality of Life and Symptoms of PTSD during the COVID-19 Lockdown in Italy. International Journal of Environmental Research and Public Health, 18(8), 4385. https://doi.org/10.3390/ijerph18084385
Bossi, F., Zaninotto, F., D’Arcangelo, S., Lattanzi, N., Malizia, A. P., & Ricciardi, E. (2022). Mindfulness-based online intervention increases well-being and decreases stress after Covid-19 lockdown. Scientific Reports, 12(1), 6483. https://doi.org/10.1038/s41598-022-10361-2
Bovin, M. J., Marx, B. P., Weathers, F. W., Gallagher, M. W., Rodriguez, P., Schnurr, P. P., & Keane, T. M. (2016). Psychometric properties of the PTSD Checklist for Diagnostic and Statistical Manual of Mental Disorders-Fifth Edition (PCL-5) in Veterans. Psychological Assessment, 28(11), 1379–1391. https://doi.org/10.1037/pas0000254
Brooks, S. K., Webster, R. K., Smith, L. E., Woodland, L., Wessely, S., Greenberg, N., & Rubin, G. J. (2020). The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. The Lancet, 395(10227), 912–920. https://doi.org/10.1016/S0140-6736(20)30460-8
Carlson, E. B., & Putnam, F. W. (1993). An update on the Dissociative Experiences Scale. Dissociation, 6(1), 16–27.
Carlson, E. B., Putnam, F. W., Ross, C. A., Torem, M., Coons, P., Dill, D. L., Loewenstein, R. J., & Braun, B. G. (1993). Validity of the Dissociative Experiences Scale in screening for multiple personality disorder: A multicenter study. The American Journal of Psychiatry, 150(7), 1030–1036. https://doi.org/10.1176/ajp.150.7.1030
Carpenter, J. K., Conroy, K., Gomez, A. F., Curren, L. C., & Hofmann, S. G. (2019). The relationship between trait mindfulness and affective symptoms: A meta-analysis of the Five Facet Mindfulness Questionnaire (FFMQ). Clinical Psychology Review, 74, 101785. https://doi.org/10.1016/j.cpr.2019.101785
Casagrande, M., Favieri, F., Tambelli, R., & Forte, G. (2020). The enemy who sealed the world: Effects quarantine due to the COVID-19 on sleep quality, anxiety, and psychological distress in the Italian population. Sleep Medicine, 75, 12–20. https://doi.org/10.1016/j.sleep.2020.05.011
Cheng, Z. H., Lozier, C. C., Lewis, M. M., O’Neil, M. E., Luoma, J. B., & Morasco, B. J. (2021). Investigating the role of psychological inflexibility, mindfulness, and self-compassion in PTSD. Journal of Contextual Behavioral Science, 22, 102–107. https://doi.org/10.1016/j.jcbs.2021.10.004
Cohen, J. (1988). Set correlation and contingency tables. Applied Psychological Measurement, 12(4), 425–434. https://doi.org/10.1177/014662168801200410
Conversano, C., Di Giuseppe, M., Miccoli, M., Ciacchini, R., Gemignani, A., & Orrù, G. (2020). Mindfulness, age and gender as protective factors against psychological distress during COVID-19 pandemic. Frontiers in Psychology, 11, 1900. https://doi.org/10.3389/fpsyg.2020.01900
Costa, P. T., & McCrae, R. R. (1992). Revised NEO Personality Inventory (NEO PI-R) and NEO Five-Factor Inventory (NEO-FFI) Professional Manual. Psychological Assessment Resources, Inc.
Di Crosta, A., Palumbo, R., Marchetti, D., Ceccato, I., La Malva, P., Maiella, R., Cipi, M., Roma, P., Mammarella, N., Verrocchio, M. C., & Di Domenico, A. (2020). Individual differences, economic stability, and fear of contagion as risk factors for PTSD symptoms in the COVID-19 emergency. Frontiers in Psychology, 11, 2329. https://doi.org/10.3389/fpsyg.2020.567367
D'Antoni, F., Feruglio, S., Matiz, A., Cantone, D., & Crescentini, C. (2022). Mindfulness meditation leads to increased dispositional mindfulness and interoceptive awareness linked to a reduced dissociative tendency. Journal of Trauma & Dissociation, 23(1), 8–23. https://doi.org/10.1080/15299732.2021.1934935
Desrosiers, A., Klemanski, D. H., & Nolen-Hoeksema, S. (2013). Mapping mindfulness facets onto dimensions of anxiety and depression. Behavior Therapy, 44(3), 373–384. https://doi.org/10.1016/j.beth.2013.02.001
García-Batista, Z. E., Guerra-Peña, K., Kandany, V. N., Marte, M. I., Garrido, L. E., Cantisano-Guzmán, L. M., Moretti, L., & Medrano, L. A. (2021). COVID-19 pandemic and health worker stress: The mediating effect of emotional regulation. PLoS ONE, 16(11), e0259013. https://doi.org/10.1371/journal.pone.0259013
Greene, T., Harju-Seppänen, J., Adeniji, M., Steel, C., Grey, N., Brewin, C. R., Bloomfield, M. A., & Billings, J. (2021). Predictors and rates of PTSD, depression and anxiety in UK frontline health and social care workers during COVID-19. European Journal of Psychotraumatology, 12(1), 1882781. https://doi.org/10.1080/20008198.2021.1882781
Hagen, C., Lien, L., Hauff, E., & Heir, T. (2016). Is mindfulness protective against PTSD? A neurocognitive study of 25 Tsunami disaster survivors. Journal of Negative Results in Biomedicine, 15(1), 13. https://doi.org/10.1186/2Fs12952-016-0056-x
Haliwa, I., Lee, J., Wilson, J., & Shook, N. J. (2020). Mindfulness and engagement in COVID-19 preventive behavior. Preventive Medicine Reports, 20, 101246. https://doi.org/10.1016/j.pmedr.2020.101246
Hanley, A. W., de Vibe, M., Solhaug, I., Gonzalez-Pons, K., & Garland, E. L. (2019). Mindfulness training reduces neuroticism over a 6-year longitudinal randomized control trial in Norwegian medical and psychology students. Journal of Research in Personality, 82, 103859. https://doi.org/10.1016/j.jrp.2019.103859
Hopwood, T. L., & Schutte, N. S. (2017). A meta-analytic investigation of the impact of mindfulness-based interventions on post traumatic stress. Clinical Psychology Review, 57, 12–20. https://doi.org/10.1016/j.cpr.2017.08.002
Horesh, D., & Brown, A. D. (2020). Traumatic stress in the age of COVID-19: A call to close critical gaps and adapt to new realities. Psychological Trauma, 12(4), 331–335. https://doi.org/10.1037/tra0000592
Hossain, M. M., Sultana, A., & Purohit, N. (2020). Mental health outcomes of quarantine and isolation for infection prevention: a systematic umbrella review of the global evidence. Epidemiology and Health, 42, e2020038. https://doi.org/10.4178/epih.e2020038
Iani, L., Lauriola, M., Chiesa, A., & Cafaro, V. (2019). Associations between mindfulness and emotion regulation: The key role of describing and nonreactivity. Mindfulness, 10(2), 366–375. https://doi.org/10.1007/s12671-018-0981-5
Jones, D. R., Lehman, B. J., Noriega, A., & Dinnel, D. L. (2019). The effects of a short-term mindfulness meditation intervention on coping flexibility. Anxiety, Stress, & Coping, 32(4), 347–361. https://doi.org/10.1080/10615806.2019.1596672
Kabat-Zinn, J. (2002). Meditation is about paying attention. Reflections The SoL Journal, 3(3), 68–71. https://doi.org/10.1162/152417302317363949
Klainin-Yobas, P., Ramirez, D., Fernandez, Z., Sarmiento, J., Thanoi, W., Ignacio, J., & Lau, Y. (2016). Examining the predicting effect of mindfulness on psychological wellbeing among undergraduate students: A structural equation modeling approach. Personality and Individual Differences, 91, 63–68. https://doi.org/10.1016/j.paid.2015.11.034
Lilja, J. L., Lundh, L.-G., Josefsson, T., & Falkenström, F. (2013). Observing as an essential facet of mindfulness: A comparison of FFMQ patterns in meditating and non-meditating individuals. Mindfulness, 4(3), 203–212. https://doi.org/10.1007/s12671-012-0111-8
Liu, C. H., Zhang, E., Wong, G. T. F., & Hyun, S. (2020). Factors associated with depression, anxiety, and PTSD symptomatology during the COVID-19 pandemic: Clinical implications for US young adult mental health. Psychiatry Research, 290, 113172. https://doi.org/10.1016/j.psychres.2020.113172
Liu, X., Wen, X., Zhang, Q., & Xu, W. (2023). Buffering traumatic reactions to COVID-19: Mindfulness moderates the relationship between the severity of the pandemic and posttraumatic stress symptoms. Psychological Trauma: Theory, Research, Practice, and Policy, 15(3), 474–482. https://doi.org/10.1037/tra0001227
Marjanovic, Z., Ward Struthers, C., Cribbie, R., & Greenglass, E. R. (2014). The Conscientious Responders Scale: A new tool for discriminating between conscientious and random responders. SAGE Open, 4(3), 1–10. https://doi.org/10.1177/2158244014545964
Martin, C. E., Bartlett, B. A., Reddy, M. K., Gonzalez, A., & Vujanovic, A. A. (2018). Associations between mindfulness facets and PTSD symptom severity in psychiatric inpatients. Mindfulness, 9(5), 1571–1583. https://doi.org/10.1007/s12671-018-0904-5
Mattson, E., James, L., & Engdahl, B. (2018). Personality factors and their impact on PTSD and post-traumatic growth is mediated by coping style among OIF/OEF veterans. Military Medicine, 183(9–10), e475–e480. https://doi.org/10.1093/milmed/usx201
Norrholm, S. D., Zalta, A., Zoellner, L., Powers, A., Tull, M. T., Reist, C., Schnurr, P. P., Weathers, F., & Friedman, M. J. (2021). Does COVID-19 count?: Defining Criterion A trauma for diagnosing PTSD during a global crisis. Depression and Anxiety, 38(9), 882–885. https://doi.org/10.1002/da.23209
Owens, G. P., Walter, K. H., Chard, K. M., & Davis, P. A. (2012). Changes in mindfulness skills and treatment response among veterans in residential PTSD treatment. Psychological Trauma: Theory, Research, Practice, and Policy, 4(2), 221–228. https://doi.org/10.1037/a0024251
Pacella, M. L., Hruska, B., & Delahanty, D. L. (2013). The physical health consequences of PTSD and PTSD symptoms: A meta-analytic review. Journal of Anxiety Disorders, 27(1), 33–46. https://doi.org/10.1016/j.janxdis.2012.08.004
Park, A. L., Velez, C. V., Kannan, K., & Chorpita, B. F. (2020). Stress, functioning, and coping during the COVID-19 pandemic: Results from an online convenience sample. The Behavior Therapist, 42(6), 210–216. https://doi.org/10.31234/osf.io/jmctv
Polizzi, C., Gautam, A., & Lynn, S. J. (2018). Trait mindfulness: A multifaceted evaluation. Imagination, Cognition and Personality, 38(2), 106–138. https://doi.org/10.1177/0276236618774321
Polizzi, C., Lynn, S. J., & Perry, A. (2020). Stress and coping in the time of COVID-19: Pathways to resilience and recovery. Clinical Neuropsychiatry: Journal of Treatment Evaluation, 17(2), 59–62. https://doi.org/10.1177/2F0276236618774321
Reffi, A. N., Pinciotti, C. M., Darnell, B. C., & Orcutt, H. K. (2019). Trait mindfulness and PTSD symptom clusters: Considering the influence of emotion dysregulation. Personality and Individual Differences, 137, 62–70. https://doi.org/10.1016/j.paid.2018.08.010
Reynolds, W. M. (1982). Development of reliable and valid short forms of the Marlowe Crowne Social Desirability Scale. Journal of Clinical Psychology, 38(1), 119–125. https://doi.org/10.1002/1097-4679(198201)38:1%3C119::AID-JCLP2270380118%3E3.0.CO;2-I
Roos, C., Bowen, S., & Witkiewitz, K. (2020). Approach coping and substance use outcomes following mindfulness-based relapse prevention among individuals with negative affect symptomatology. Mindfulness, 11(10), 2397–2410. https://doi.org/10.1007/s12671-020-01456-w
Rubin, G. J., & Wessely, S. (2020). The psychological effects of quarantining a city. BMJ Online, 368, m313. https://doi.org/10.1136/bmj.m313
Schumer, M. C., Lindsay, E. K., & Creswell, J. D. (2018). Brief mindfulness training for negative affectivity: A systematic review and meta-analysis. Journal of Consulting and Clinical Psychology, 86(7), 569–583. https://doi.org/10.1037/ccp0000324
Short, N. A., Boffa, J. W., Clancy, K., & Schmidt, N. B. (2018). Effects of emotion regulation strategy use in response to stressors on PTSD symptoms: An ecological momentary assessment study. Journal of Affective Disorders, 230, 77–83. https://doi.org/10.1016/j.jad.2017.12.063
Solomon, Z., Ginzburg, K., Ohry, A., & Mikulincer, M. (2021). Overwhelmed by the news: A longitudinal study of prior trauma, posttraumatic stress disorder trajectories, and news watching during the COVID-19 pandemic. Social Science & Medicine, 278, 113956. https://doi.org/10.1016/j.socscimed.2021.113956
Spielberger, C. D. (1983). State-Trait Anxiety Inventory for Adults (STAI-AD) [Database record]. APA PsycTests. https://doi.org/10.1037/t06496-000
Stanley, I. H., Boffa, J. W., Tran, J. K., Schmidt, N. B., Joiner, T. E., & Vujanovic, A. A. (2019). Posttraumatic stress disorder symptoms and mindfulness facets in relation to suicide risk among firefighters. Journal of Clinical Psychology, 75(4), 696–709. https://doi.org/10.1002/jclp.22748
Stephenson, K. R., Simpson, T. L., Martinez, M. E., & Kearney, D. J. (2017). Changes in mindfulness and posttraumatic stress disorder symptoms among veterans enrolled in mindfulness-based stress reduction. Journal of Clinical Psychology, 73(3), 201–217. https://doi.org/10.1002/jclp.22323
Sun, L. N., Gu, J. W., Huang, L. J., Shang, Z. L., Zhou, Y. G., Wu, L. L., Jia, Y. P., Liu, N. Q., & Liu, W. Z. (2021). Military-related posttraumatic stress disorder and mindfulness meditation: A systematic review and meta-analysis. Chinese Journal of Traumatology, 24(4), 221–230. https://doi.org/10.1016/2Fj.cjtee.2021.05.003
Tan, H. C., Ho, J. A., Kumarusamy, R., & Sambasivan, M. (2022). Measuring social desirability bias: Do the full and short versions of the Marlowe-Crowne Social Desirability scale matter? Journal of Empirical Research on Human Research Ethics, 17(3), 382–400. https://doi.org/10.1177/15562646211046091
Tang, W., Hu, T., Hu, B., Jin, C., Wang, G., Xie, C., Chen, S., & Xu, J. (2020). Prevalence and correlates of PTSD and depressive symptoms one month after the outbreak of the COVID-19 epidemic in a sample of home-quarantined Chinese university students. Journal of Affective Disorders, 274, 1–7. https://doi.org/10.1016/j.jad.2020.05.009
Thompson, R. W., Arnkoff, D. B., & Glass, C. R. (2011). Conceptualizing mindfulness and acceptance as components of psychological resilience to trauma. Trauma, Violence, & Abuse, 12(4), 220–235. https://doi.org/10.1177/1524838011416375
Tu, Y. K., Gunnell, D., & Gilthorpe, M. S. (2008). Simpson’s paradox, lord’s paradox, and suppression effects are the same phenomenon-The reversal paradox. Emerging Themes in Epidemiology, 5(1), 2. https://doi.org/10.1186/1742-7622-5-2
van Son, J., Nyklíček, I., Nefs, G., Speight, J., Pop, V. J., & Pouwer, F. (2015). The association between mindfulness and emotional distress in adults with diabetes: Could mindfulness serve as a buffer? Results from Diabetes MILES: The Netherlands. Journal of Behavioral Medicine, 38(2), 251–260. https://doi.org/10.1007/s10865-014-9592-3
Velotti, P., Civilla, C., Rogier, G., & BeomonteZobel, S. (2021). A fear of COVID-19 and PTSD symptoms in pathological personality: The mediating effect of dissociation and emotion dysregulation. Frontiers in Psychiatry, 12, 590021. https://doi.org/10.3389/fpsyt.2021.590021
Watson, D., Clark, L. A., & Tellegen, A. (1988). Development and validation of brief measures of positive and negative affect: The PANAS scales. Journal of Personality and Social Psychology, 54(6), 1063–1070. https://doi.org/10.1037//0022-3514.54.6.1063
Wielgus, B., Urban, W., Patriak, A., & Cichocki, Ł. (2020). Examining the associations between psychological flexibility, mindfulness, psychosomatic functioning, and anxiety during the COVID-19 pandemic: A path analysis. International Journal of Environmental Research and Public Health, 17(23), 8764. https://doi.org/10.3390/ijerph17238764
Williston, S. K., Grossman, D., Mori, D. L., & Niles, B. L. (2021). Mindfulness interventions in the treatment of posttraumatic stress disorder. Professional Psychology: Research and Practice, 52(1), 46–57. https://doi.org/10.1037/pro0000363
Zhu, J. L., Schülke, R., Vatansever, D., Xi, D., Yan, J., Zhao, H., Xie, X., Feng, J., Chen, M. Y., Sahakian, B. J., & Wang, S. (2021). Mindfulness practice for protecting mental health during the COVID-19 pandemic. Translational Psychiatry, 11(1), 1–11. https://doi.org/10.1038/s41398-021-01459-8
Author information
Authors and Affiliations
Contributions
Craig P. Polizzi, Fiona G. Sleight, and Steven Jay Lynn contributed to the study conception and design. Material preparation and data collection and analysis were performed by Craig P. Polizzi and Fiona G. Sleight. The first draft of the manuscript was written by Craig P. Polizzi, Fiona G. Sleight, Damla E. Aksen, and Charlie W. McDonald and all authors commented on previous versions of the manuscript. All authors read, edited, and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Institutional Review Board of Binghamton University (SUNY).
Informed Consent
Online informed consent was obtained for all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Polizzi, C.P., Sleight, F.G., Aksen, D.E. et al. Mindfulness and COVID-19-Related Stress: Staying Present During Uncertain Times. Mindfulness 14, 1135–1147 (2023). https://doi.org/10.1007/s12671-023-02132-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-023-02132-5