Abstract
Background
Heart Failure (HF) is associated with increased morbidity and mortality. Identification of patients at risk for adverse events could lead to improved outcomes. Few studies address the association of echocardiographic-derived PAWP with exercise capacity, readmissions, and mortality in HF.
Methods
HF-ACTION enrolled 2331 outpatients with HF with reduced ejection fraction (HFrEF) who were randomized to aerobic exercise training versus usual care. All patients underwent baseline echocardiography. Echocardiographic-derived PAWP (ePAWP) was assessed using the Nagueh formula. We evaluated the relationship between ePAWP to clinical outcomes.
Results
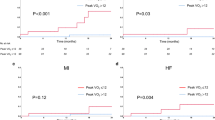
Among the 2331 patients in the HF-ACTION trial, 2125 patients consented and completed follow-up with available data. 807 of these patients had complete echocardiographic data that allowed the calculation of ePAWP. Of this cohort, mean age (SD) was 58 years (12.7), and 255 (31.6%) were female. The median ePAWP was 14.06 mmHg. ePAWP was significantly associated with cardiovascular death or HF hospitalization (Hazard ratio [HR] 1.02, coefficient 0.016, CI 1.002–1.030, p = 0.022) and all-cause death or HF hospitalization (HR 1.01, coefficient 0.010, CI 1.001–1.020, p = 0.04). Increased ePAWP was also associated with decreased exercise capacity leading to lower peak VO2 (p = < 0.001), high Ve/VCO2 slope (p = < 0.001), lower exercise duration (p = < 0.001), oxygen uptake efficiency (p = < 0.001), and shorter 6-MWT distance (p = < 0.001).
Conclusions
Among HFrEF patients, echocardiographic-derived PAWP was associated with increased mortality, reduced functional capacity and heart failure hospitalization. ePAWP may be a viable noninvasive marker to risk stratify HFrEF patients.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available via the Biologic Specimen and Data Repository Information Coordinating Center (BioLINCC) from the National Heart, Lung and Blood Institute (NHLBI). Restrictions apply to the availability of these data, which were used under license for this study.
Abbreviations
- 6-MWT:
-
6-Minute walk test
- ACEi:
-
Angiotensin-converting enzyme inhibitor
- ARB:
-
Angiotensin receptor blocker
- BMI:
-
Body mass index
- BioLINCC:
-
National heart-lung blood institute biological specimen and data repository information coordinating center
- COPD:
-
Chronic obstructive pulmonary disease
- CPX:
-
Cardiopulmonary exercise test
- ePAWP:
-
Echocardiographic-derived pulmonary arterial wedge pressure
- HF:
-
Heart Failure
- HF-ACTION:
-
Heart failure: a controlled trial investigating outcomes of exercise training
- HFrEF:
-
Heart failure with reduced ejection fraction
- HR:
-
Hazard ratio
- KCCQ:
-
Kansas city cardiomyopathy questionnaire
- LVEF:
-
Left ventricular ejection fraction
- NYHA:
-
New York heart association
- PAWP:
-
Pulmonary arterial wedge pressure
- PCI:
-
Percutaneous coronary intervention
- SAS:
-
Statistical analysis system
- SD:
-
Standard deviation
References
Virani SS, Alvaro A, Benjamin EJ, Bittencourt MS, Callaway CW, Carson AP, et al. Heart disease and stroke statistics—2020 update: A report from the American Heart Association. Circulation. 2020;141:139–596.
Hickson SS, Butlin M, Mir FA, Graggaber J, Cheriyan J, Khan F, et al. The accuracy of central SBP determined from the second systolic peak of the peripheral pressure waveform. J Hypertens. 2009;27:1784–8.
Chen J, Normand S-LT, Wang Y, Krumholz HM. National and regional trends in heart failure hospitalization and mortality rates for medicare beneficiaries, 1998–2008. JAMA. 2011;306:1669–78.
Loehr LR, Rosamond WD, Chang PP, Folsom AR, Chambless LE. Heart failure incidence and survival (from the atherosclerosis risk in communities study). Am J Cardiol Elsevier. 2008;101:1016–22.
Chang PP, Chambless LE, Shahar E, Bertoni AG, Russell SD, Ni H, et al. Incidence and survival of hospitalized acute decompensated heart failure in Four US communities (from the atherosclerosis risk in communities study). Am J Cardiol Elsevier. 2014;113:504–10.
Gottlieb DJ, Yenokyan G, Newman AB, O’Connor GT, Punjabi NM, Quan SF, et al. A Prospective Study of Obstructive Sleep Apnea and Incident Coronary Heart Disease and Heart Failure: The Sleep Heart Health Study. Circulation. 2010;122:352–60.
Hartupee J, Mann DL. Neurohormonal activation in heart failure with reduced ejection fraction. Nat Rev Cardiol. 2017;14:30–8.
Sachdeva A, Horwich TB, Fonarow GC. Comparison of usefulness of each of five predictors of mortality and urgent transplantation in patients with advanced heart failure. Am J Cardiol. 2010;106:830–5.
Sobieszczańska-Małek M, Zieliński T, Piotrowski W, Korewicki J, Of Polkard-Hf OBOTP. Prognostic value of pulmonary hemodynamic parameters in cardiac transplant candidates. Cardiol J. 2014;21:532–8.
Nagueh SF, Bhatt R, Vivo RP, Krim SR, Sarvari SI, Russell K, et al. Echocardiographic evaluationEvaluation of hemodynamicsHemodynamics in patients with decompensated systolic heart failure. Patients with decompensated systolic heart failure. Circ Cardiovasc Imaging. 2011;4:220–7.
Mohan R, Mehta H, Narula A, Smith M, Rubenson D, Johnson A, et al. Estimation of pulmonary capillary wedge pressure by echocardiography: a simplified approach. J Card Fail. 2015;21:S22. https://doi.org/10.1016/j.cardfail.2015.06.097.
Tachjian A, Sanghai SR, Stencel J, Parker MW, Kakouros N, Aurigemma GP. Estimation of mean left atrial pressure in patients with acute coronary syndromes: a doppler echocardiographic and cardiac catheterization study. J Am Soc Echocardiogr. 2019;32:365-374.e1.
Wang J, Nagueh SF. Echocardiographic assessment of left ventricular filling pressures. Heart Fail Clin. 2008;4:57–70.
Kim YJ, Sohn DW. Mitral annulus velocity in the estimation of left ventricular filling pressure: prospective study in 200 patients. J Am Soc Echocardiogr Off Publ Am Soc Echocardiogr. 2000;13:980–5.
Nagueh SF, Kopelen HA, Quinones MA. Assessment of left ventricular filling pressures by doppler in the presence of atrial fibrillation. Circulation. 1996;94:2138–45.
Nagueh SF, Mikati I, Kopelen HA, Middleton KJ, Quiñones MA, Zoghbi WA. Doppler estimation of left ventricular filling pressure in sinus tachycardia. A new application of tissue doppler imaging. Circulation. 1998;98:1644–50.
Whellan DJ, O’Connor CM, Lee KL, Keteyian SJ, Cooper LS, Ellis SJ, et al. Heart failure and a controlled trial investigating outcomes of exercise training (HF-ACTION): design and rationale. Am Heart J. 2007;153:201–11.
Flynn KE, Piña IL, Whellan DJ, Lin L, Blumenthal JA, Ellis SJ, et al. Effects of exercise training on health status in patients with chronic heart failure: HF-ACTION randomized controlled trial. JAMA. 2009;301:1451–9.
O’Connor CM, Whellan DJ, Lee KL, Keteyian SJ, Cooper LS, Ellis SJ, et al. Efficacy and safety of exercise training in patients with chronic heart failure: HF-ACTION randomized controlled trial. JAMA. 2009;301:1439–50.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr Off Publ Am Soc Echocardiogr. 2015;28:1-39.e14.
Nagueh SF, Middleton KJ, Kopelen HA, Zoghbi WA, Quiñones MA. Doppler tissue imaging: a noninvasive technique for evaluation of left ventricular relaxation and estimation of filling pressures. J Am Coll Cardiol. 1997;30:1527–33.
Oh JK. Echocardiography as a noninvasive Swan-Ganz Catheter. Circulation American Heart Association. 2005;111:3192–4.
Weil BR, Suzuki G, Young RF, Iyer V, Canty JM. Troponin release and reversible left ventricular dysfunction after transient pressure overload. J Am Coll Cardiol. 2018;71:2906–16.
Echouffo-Tcheugui JB, Erqou S, Butler J, Yancy CW, Fonarow GC. Assessing the risk of progression from asymptomatic left ventricular dysfunction to overt heart failure: a systematic overview and meta-analysis. JACC Heart Fail. 2016;4:237–48.
Stevenson LW, Tillisch JH, Hamilton M, Luu M, Chelimsky-Fallick C, Moriguchi J, et al. Importance of hemodynamic response to therapy in predicting survival with ejection fraction ≤20% secondary to ischemic or nonischemic dilated cardiomyopathy. Am J Cardiol. 1990;66:1348.
Grigioni F, Potena L, Galiè N, Fallani F, Bigliardi M, Coccolo F, et al. Prognostic implications of serial assessments of pulmonary hypertension in severe chronic heart failure. J Heart Lung Transplant. 2006;25:1241–6.
2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines [Internet]. [cited 2022 Nov 17]. Available from: https://www.ahajournals.org/doi/epub/https://doi.org/10.1161/CIR.0000000000001063
Ommen SR, Nishimura RA, Appleton CP, Miller FA, Oh JK, Redfield MM, et al. Clinical utility of Doppler echocardiography and tissue Doppler imaging in the estimation of left ventricular filling pressures: A comparative simultaneous Doppler-catheterization study. Circulation. 2000;102:1788–94.
Pinamonti B, Di Lenarda A, Sinagra G, Camerini F. Restrictive left ventricular filling pattern in dilated cardiomyopathy assessed by Doppler echocardiography: clinical, echocardiographic and hemodynamic correlations and prognostic implications Heart Muscle Disease Study Group. J Am Coll Cardiol. 1993;22:808–15.
Giannuzzi P, Imparato A, Temporelli PL, de Vito F, Silva PL, Scapellato F, et al. Doppler-derived mitral deceleration time of early filling as a strong predictor of pulmonary capillary wedge pressure in postinfarction patients with left ventricular systolic dysfunction. J Am Coll Cardiol. 1994;23:1630–7.
Pozzoli M, Capomolla S, Pinna G, Cobelli F, Tavazzi L. Doppler echocardiography reliably predicts pulmonary artery wedge pressure in patients with chronic heart failure with and without mitral regurgitation. J Am Coll Cardiol. 1996;27:883–93.
Traversi E, Pozzoli M, Cioffi G, Capomolla S, Forni G, Sanarico M, et al. Mitral flow velocity changes after 6 months of optimized therapy provide important hemodynamic and prognostic information in patients with chronic heart failure. Am Heart J. 1996;132:809–19.
Nishimura RA, Appleton CP, Redfield MM, Ilstrup DM, Holmes DR, Tajik AJ. Noninvasive doppler echocardiographic evaluation of left ventricular filling pressures in patients with cardiomyopathies: a simultaneous Doppler echocardiographic and cardiac catheterization study. J Am Coll Cardiol. 1996;28:1226–33.
Rivas-Gotz C, Manolios M, Thohan V, Nagueh SF. Impact of left ventricular ejection fraction on estimation of left ventricular filling pressures using tissue Doppler and flow propagation velocity. Am J Cardiol. 2003;91:780–4.
Stein JH, Neumann A, Preston LM, Costanzo MR, Parrillo JE, Johnson MR, et al. Echocardiography for hemodynamic assessment of patients with advanced heart failure and potential heart transplant recipients. J Am Coll Cardiol. 1997;30:1765–72.
Temporelli PL, Scapellato F, Eleuteri E, Imparato A, Giannuzzi P. Doppler echocardiography in advanced systolic heart failure: a noninvasive alternative to Swan-Ganz catheter. Circ Heart Fail. 2010;3:387–94.
Zile MR, Bennett TD, St. John SM, Cho YK, Adamson PB, Aaron MF, et al. Transition from chronic compensated to acute decompensated heart failure. Circulation. 2008;118:1433–41.
Andersen OS, Smiseth OA, Dokainish H, Abudiab MM, Schutt RC, Kumar A, et al. Estimating left ventricular filling pressure by echocardiography. J Am Coll Cardiol. 2017;69:1937–48.
Butler J, Chomsky DB, Wilson JR. Pulmonary hypertension and exercise intolerance in patients with heart failure. J Am Coll Cardiol. 1999;34:1802–6.
Aronson D, Eitan A, Dragu R, Burger AJ. Relationship between reactive pulmonary hypertension and mortality in patients with acute decompensated heart failure. Circ Heart Fail. 2011;4:644–50.
McMurray JJV, Packer M, Desai AS, Gong J, Lefkowitz MP, Rizkala AR, et al. Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med. 2014;371:993–1004.
Acknowledgements
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Younghoon Kwon is supported by NIH grants R01HL158765, R21AG070576, and R21HL150502. Khadijah Breathett is supported by NIH grants R01HL159216, R56HL159216, and K01HL142848. Kenneth Bilchick is supported by NIH/NHLBI grants R56HL135556, R21HL140445, R01HL147104, and U01HL127654, as well as grant 18TPA34170579 from the American Heart Association. Nishaki Mehta is supported with prior research funding by Boston Scientific, as well as speaking honoraria by Boston Scientific and Medtronic. The other authors declare no conflict of interest for this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Stafford, P.L., Purvis, A., Bilchick, K. et al. Echocardiographic derived pulmonary artery wedge pressure is associated with mortality, heart hospitalizations, and functional capacity in chronic systolic heart failure: insights from the HF-ACTION trial. J Echocardiogr (2023). https://doi.org/10.1007/s12574-023-00630-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12574-023-00630-y