Abstract
Background
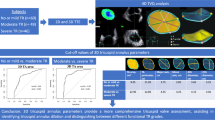
It is unclear how upper septal hypertrophy (USH) affects Doppler-derived left ventricular stroke volume (SV) in patients with AS. The aims of this study were to: (1) validate the accuracy of 3D transesophageal echocardiography (TEE) measurements of the left ventricular outflow tract (LVOT), (2) evaluate the differences in LVOT geometry between AS patients with and without USH, and (3) assess the impact of USH on measurement of SV.
Methods
In protocol 1, both 3D TEE and multi-detector computed tomography were performed in 20 patients with AS [aortic valve area (AVA) ≤ 1.5 cm2]. Multiplanar reconstruction was used to measure the LVOT short and long diameters in four parts from the tip of the septum to the annulus. In protocol 2, the same 3D TEE measurements were performed in AS patients (AVA ≤ 1.5 cm2, n = 129) and controls (n = 30). We also performed 2D and 3D transthoracic echocardiography in all patients.
Results
In protocol 1, excellent correlations of LVOT parameters were found between the two modalities. In protocol 2, the USH group had smaller LVOT short and long diameters than the non-USH group. Although no differences in mean pressure gradient, or SV calculated with the 3D method existed between the two groups, the USH group had greater SV calculated with the Doppler method (73 ± 15 vs. 66 ± 15 ml) and aortic valve area (0.89 ± 0.26 vs. 0.73 ± 0.24 cm2) than the non-USH group.
Conclusions
3D TEE can provide a precise assessment of the LVOT in AS. USH affects the LVOT geometry in patients with AS, which might lead to inaccurate assessments of disease severity.








Similar content being viewed by others
References
Nkomo VT, Gardin JM, Skelton TN, et al. Burden of valvular heart diseases: a population-based study. Lancet. 2006;368:1005–11.
Carabello BA, Paulus WJ. Aortic stenosis. Lancet. 2009;373:956–66.
Carabello BA. Clinical practice. Aortic stenosis. N Engl J Med. 2002;346:677–82.
Saikrishnan N, Kumar G, Sawaya FJ, et al. Accurate assessment of aortic stenosis: a review of diagnostic modalities and hemodynamics. Circulation. 2014;129:244–53.
Delgado V, Ng AC, Schuijf JD, et al. Automated assessment of the aortic root dimensions with multidetector row computed tomography. Ann Thorac Surg. 2011;91:716–23.
Tops LF, Wood DA, Delgado V, et al. Noninvasive evaluation of the aortic root with multislice computed tomography implications for transcatheter aortic valve replacement. J Am Coll Cardiol Img. 2008;1:321–30.
Akhtar M, Tuzcu EM, Kapadia SR, et al. Aortic root morphology in patients undergoing percutaneous aortic valve replacement: evidence of aortic root remodeling. J Thorac Cardiovasc Surg. 2009;137:950–6.
Stolzmann P, Knight J, Desbiolles L, et al. Remodelling of the aortic root in severe tricuspid aortic stenosis: implications for transcatheter aortic valve implantation. Eur Radiol. 2009;19:1316–23.
Otani K, Takeuchi M, Kaku K, et al. Assessment of the aortic root using real-time 3D transesophageal echocardiography. Circ J. 2010;74:2649–57.
Wu VC, Kaku K, Takeuchi M, et al. Aortic root geometry in patients with aortic stenosis assessed by real-time three-dimensional transesophageal echocardiography. J Am Soc Echocardiogr. 2014;27:32–41.
Lang RM, Bierig M, Devereux RB, et al. Chamber Quantification Writing Group; American Society of Echocardiography’s Guidelines and Standards Committee; European Association of Echocardiography. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr. 2005;18:1440–63.
Pibarot P, Clavel MA. Left ventricular outflow tract geometry and dynamics in aortic stenosis: Implications for the echocardiographic assessment of aortic valve area. J Am Soc Echocardiogr. 2015;28:1267–9.
Goor D, Lillehei W, Edwards JE. The “sigmoid septum” variation in the contour of the left ventricular outlet. AJR Am J Roentgenol. 1969;107:366–76.
Diaz T, Pencina MJ, Benjamin EJ, et al. Prevalence, clinical correlates, and prognosis of discrete upper septal thickening on echocardiography: the Framingham Heart Study. Echocardiography. 2009;26:247–53.
Funabashi N, Umazume T, Takaoka H, et al. Sigmoid shaped interventricular septum exhibit normal myocardial characteristics and has a relationship with aging, ascending aortic sclerosis and its tilt to left ventricle. Int J Cardiol. 2013;168:4484–8.
Jilaihawi H, Kashif M, Fontana G, et al. Cross-sectional computed tomographic assessment improves accuracy of aortic annular sizing for transcatheter aortic valve replacement and reduces the incidence of paravalvular aortic regurgitation. J Am Coll Cardiol. 2012;59:1275–86.
Hachicha Z, Dumesnil JG, Bogaty P, et al. Paradoxical low-flow, low-gradient severe aortic stenosis despite preserved ejection fraction is associated with higher afterload and reduced survival. Circulation. 2007;115:2856–64.
Lancellotti P, Magne J, Donal E, et al. Clinical outcome in asymptomatic severe aortic stenosis: insights from the new proposed aortic stenosis grading classification. J Am Coll Cardiol. 2012;59:235–43.
Ozkan A, Hachamovitch R, Kapadia SR, et al. Impact of aortic valve replacement on outcome of symptomatic patients with severe aortic stenosis with low gradient and preserved left ventricular ejection fraction. Circulation. 2013;128:622–31.
Doddamani S, Grushko MJ, Makaryus AN, et al. Demonstration of left ventricular outflow tract eccentricity by 64-slice multi-detector CT. Int J Cardiovasc Imaging. 2009;25:175–81.
Saitoh T, Shiota M, Izumo M, et al. Comparison of left ventricular outflow geometry and aortic valve area in patients with aortic stenosis by 2-dimensional versus 3-dimensional echocardiography. Am J Cardiol. 2012;109:1626–31.
Garcia J, Kadem L, Larose E, et al. Comparison between cardiovascular magnetic resonance and transthoracic Doppler echocardiography for the estimation of effective orifice area in aortic stenosis. J Cardiovasc Magn Reson. 2011;13:25.
Le Ven F, Freeman M, Webb J, et al. Impact of low flow on the outcome of high-risk patients undergoing transcatheter aortic valve replacement. J Am Coll Cardiol. 2013;62:782–8.
Clavel MA, Berthelot-Richer M, Le Ven F, et al. Impact of classic and paradoxical low flow on survival after aortic valve replacement for severe aortic stenosis. J Am Coll Cardiol. 2015;65:645–53.
Dayan V, Vignolo G, Magne J, et al. Outcome and impact of aortic valve replacement in patients with preserved LVEF and low-gradient aortic stenosis. J Am Coll Cardiol. 2015;66:2594–603.
Poh KK, Levine RA, Solis J, et al. Assessing aortic valve area in aortic stenosis by continuity equation: a novel approach using real-time three-dimensional echocardiography. Eur Heart J. 2008;29:2526–35.
Mehrotra P, Flynn AW, Jansen K, et al. Differential left ventricular outflow tract remodeling and dynamics in aortic stenosis. J Am Soc Echocardiogr. 2015;28:1259–66.
Sato K, Seo Y, Ishizu T, et al. Reliability of aortic stenosis severity classified by 3-dimensional echocardiography in the prediction of cardiovascular events. Am J Cardiol. 2016;118:410–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dan Koto, Masaki Izumo, Takafumi Machida, Kihei Yoneyama, Tomomi Suzuki, Ryo Kamijima, Yasuyuki Kobayashi, Tomoo Harada, and Yoshihiro J. Akashi declare that they have no conflicts of interest.
Human rights statements and informed consent
All procedure followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later revisions. The participants were well-informed prior to the test; written informed consent was obtained before enrollment.
Rights and permissions
About this article
Cite this article
Koto, D., Izumo, M., Machida, T. et al. Geometry of the left ventricular outflow tract assessed by 3D TEE in patients with aortic stenosis: impact of upper septal hypertrophy on measurements of Doppler-derived left ventricular stroke volume. J Echocardiogr 16, 162–172 (2018). https://doi.org/10.1007/s12574-018-0383-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12574-018-0383-7