Abstract
Background
Erythema nodosum can be associated with a number of systemic diseases. There is, however, a paucity of information in the pediatric literature on this condition. The purpose of this article is to familiarize pediatricians with the evaluation, diagnosis, and treatment of erythema nodosum.
Data sources
A PubMed search was completed in Clinical Queries using the key terms “erythema nodosum”.
Results
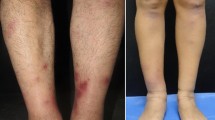
Clinically, erythema nodosum presents with a sudden onset of painful, erythematous, subcutaneous nodules mainly localized to the pretibial areas. Lesions are usually bilateral and symmetrical, ranging from 1 to 5 cm in diameter. Erythema nodosum may be associated with a variety of conditions such as infection, medications, sarcoidosis, pregnancy, inflammatory bowel disease, vaccination, autoimmune disease, malignancy, and miscellaneous causes. The condition is idiopathic in approximately 50% of cases. The diagnosis is mainly clinical with biopsy reserved for atypical cases. To evaluate for the underlying cause, some basic laboratory screening studies are worthwhile in most cases and include a complete blood cell count, erythrocyte sedimentation rate and/or C-reactive protein, throat swab culture, antistreptococcal O titers, and a chest radiograph. Other tests should be individualized, guided by the history and physical examination results. Most cases of erythema nodosum are self-limited and require no treatment. Bed rest and leg elevation are generally recommended to reduce the discomfort. Nonsteroidal anti-inflammatory drugs are the first-line treatment for pain management.
Conclusions
As erythema nodosum is often a cutaneous manifestation of a systemic disease, a thorough search should be performed to reveal the underlying cause.



Similar content being viewed by others
References
Min MS, Fischer R, Fournier JB. Unilateral erythema nodosum following norethindrone acetate, ethinyl estradiol, and ferrous fumarate combination therapy. Case Rep Obstet Gynecol. 2016;2016:5726416.
González-Gay MA, García-Porrúa C, Pujol RM, Salvarani C. Erythema nodosum: a clinical approach. Clin Exp Rheumatol. 2001;19:365–8.
Willan R. On cutaneous diseases, vol. 1. London: J. Johnson, St Paul’s Church-Yard; 1798.
Blake T, Manahan M, Rodins K. Erythema nodosum-a review of an uncommon panniculitis. Dermatol Online J. 2014;20:22376.
Ozbagcivan O, Akarsu S, Avci C, Inci BB, Fetil E. Examination of the microbial spectrum in the etiology of erythema nodosum: a retrospective descriptive study. J Immunol Res. 2017;2017:8139591.
Chowaniec M, Starba A, Wiland P. Erythema nodosum-review of the literature. Reumatologia. 2016;54:79–82.
Xu X, Liang G, Duan M, Zhang L. Acute myeloid leukemia presenting as erythema nodosum: a case report. Medicine (Baltimore). 2017;96:e8666.
Kakourou T, Drosatou P, Psychou F, Aroni K, Nicolaidou P. Erythema nodosum in children: a prospective study. J Am Acad Dermatol. 2001;44:17–21.
Labbé L, Perel Y, Maleville J, Taïeb A. Erythema nodosum in children: a study of 27 patients. Pediatr Dermatol. 1996;13:447–50.
Wallis P, Starr M, Phillips RJ. An uncommon cause of erythema nodosum. J Paediatr Child Health. 2016;52:961–3.
Aydın-Teke T, Tanır G, Bayhan GI, Metin O, Oz N. Erythema nodosum in children: evaluation of 39 patients. Turk J Pediatr. 2014;56:144–9.
Hafsi W, Haseer Koya H. Erythema nodosum. StatPearls [Internet]. Treasure Island: StatPearls Publishing; 2018 Jan-.2017 Dec 12.
Requena L, Yus ES. Erythema nodosum. Dermatol Clin. 2008;26:425–38.
Schwartz RA, Nervi SJ. Erythema nodosum: a sign of systemic disease. Am Fam Physician. 2007;75:695–700.
De Simone C, Caldarola G, Scaldaferri F, Petito V, Perino F, Arena V, et al. Clinical, histopathological, and immunological evaluation of a series of patients with erythema nodosum. Int J Dermatol. 2016;55:e289–94.
Kroshinsky D. Erythema nodosum. In: Post TW, editor. UpToDate. Waltham; 2018.
Sehrawat M, Dixit N, Sardana K, Malhotra P. Exploring the combination of SSKI and topical heparin in a case of erythema nodosum migrans. Dermatol Ther. 2018;31:e12610.
Faulkes RE. Upper limb erythema nodosum: the first presentation of Crohn’s disease. Clin Case Rep. 2014;2:183–5.
Golisch KB, Gottesman SP, Segal RJ. Compression stockings as an effective treatment for erythema nodosum: case series. Int J Womens Dermatol. 2017;3:231–3.
Bjorn-Mortensen K, Ladefoged K, Simonsen J, Michelsen SW, Sørensen HC, Koch A, et al. Erythema nodosum and the risk of tuberculosis in a high incidence setting. Int J Circumpolar Health. 2016;75:32666.
Yotsu R, Mii S, Hayashi R, Harada H, Furukawa K, Eto H. Erythema nodosum associated with Yersinia enterocolitica infection. J Dermatol. 2010;37:819–22.
Borsje A, van der Reijden W, Soetekouw R. Lymphogranuloma venereum presenting with erythema nodosum. Int J STD AIDS. 2016;27:1354–5.
Cheng H, Yung A, Lamont D. Pretibial fever: a forgotten cause of erythema nodosum. Australas J Dermatol. 2014;55:236–7.
Gilchrist H, Patterson JW. Erythema nodosum and erythema induratum (nodular vasculitis): diagnosis and management. Dermatol Ther. 2010;23:320–7.
Greco F, Catania R, Pira AL, Saporito M, Scalora L, Aguglia MG, et al. Erythema nodosum and mycoplasma pneumoniae infections in childhood: further observations in two patients and a literature review. J Clin Med Res. 2015;7:274–7.
Mantadakis E, Arvanitidou V, Tsalkidis A, Thomaidis S, Chatzimichael A. Erythema nodosum associated with Salmonella enteritidis. Hippokratia. 2010;14:51–3.
Meriglier E, Asquier L, Roblot F, Roblot P, Landron C. A case of Q fever with erythema nodosum. Infection. 2018;46:127–9.
Sawada T, Suehiro M, Takaya K. Lower-leg cellulitis-like manifestations of erythema nodosum induced by Chlamydophila pneumoniae infection. Indian J Dermatol. 2016;61:237.
Tanveer A, Majeed I, Naeem M, Rana WA, Kazmi SY, Haroon ZH. Brucella melitensis presenting as erythema nodosum-like lesions. J Coll Physicians Surg Pak. 2009;19:794–5.
Mukherjee T, Basu A. Disseminated histoplasmosis presenting as a case of erythema nodosum and hemophagocytic lymphohistiocytosis. Med J Armed Forces India. 2015;71(Suppl 2):S598–600.
Papaiordanou F, da Silveira BR, Abulafia LA. Hypersensitivity reaction to Sporothrix schenckii: erythema nodosum associated with sporotrichosis. Rev Soc Bras Med Trop. 2015;48:504.
Romano C, Gaviria EM, Feci L, Fimiani M. Erythema nodosum complicating kerion of the scalp caused by Trichophyton mentagrophytes. J Eur Acad Dermatol Venereol. 2016;30:357–9.
Satish G, Rajam L, Regi S, Nazar PK. Multiple amoebic abscesses with erythema nodosum. Indian J Pediatr. 2012;79:532–4.
Coleman EL, Cowper SE, Stein SM, Leventhal JS. Erythema nodosum-like eruption in the setting of sorafenib therapy. JAMA Dermatol. 2018;154:369–70.
Emre S, Ozdemir D, Orhun S, Kalkan G, Sener S. A case of severe erythema nodosum induced by methimazole. Saudi Pharm J. 2017;25:813–5.
González-Olivares M, Khedaoui R, Martínez-Morán C, Borbujo J. Azathioprine-induced hypersensitivity reaction presenting as erythema nodosum. Actas Dermosifiliogr. 2017;108:591–3 (in English, Spanish).
Petukhova TA, Tartar DM, Mayo K, Fung MA, Tuscano J, Jagdeo J. Erythema nodosum-like septal panniculitis secondary to lenalidomide therapy in a patient with janus kinase 2-positive myelofibrosis. J Drugs Dermatol. 2016;15:1024–5.
Woo YR, Koo DW, Jung KE, Lee JS. Erythema nodosum associated with valproate. Ann Dermatol. 2015;2:765–6.
Simpson SM, Farmer J, Kratky V. Acute orbital sarcoidosis with preceding fever and erythema nodosum. Can J Ophthalmol. 2017;52:e233–5.
Starba A, Chowaniec M, Wiland P. Erythema nodosum-presentation of three cases. Reumatologia. 2016;54:83–5.
Toh JW, Salindera S, Sarofim M, Turner C, Patapanian H. An unusual cause of bilateral lower limb pitting oedema: Crohn’s septal panniculitis diagnostic of erythema nodosum. ANZ J Surg. 2018;88:E566–7.
Cohen PR. Combined reduced-antigen content tetanus, diphtheria, and acellular pertussis (Tdap) vaccine-related erythema nodosum: case report and review of vaccine-associated erythema nodosum. Dermatol Ther (Heidelb). 2013;3:191–7.
Kaliyadan F, Dharmaratnam AM. Erythema nodosum—an association with rabies vaccination. Dermatol Online J. 2008;14:22.
Wu YL, Tsai MH, Liu LL. Erythema nodosum and hepatitis B: a case report and literature review. J Microbiol Immunol Infect. 2008;41:437–9.
Ajmani S, Chowdhury AC, Misra DP, Agarwal V. Behcet’s disease without oral ulcers presenting with erythema nodosum and deep venous thrombosis. Trop Dr. 2016;46:34–6.
Eugénio G, Tavares J, Ferreira JF, Malcata A. Unusual association between erythema nodosum and autoimmune atrophic gastritis. BMJ Case Rep. 2018;2018:bcr-2017-223638.
Fruchter R, Castilla C, Ng E, Pomeranz MK, Femia AN. Erythema nodosum in association with idiopathic granulomatous mastitis: a case series and review of the literature. J Eur Acad Dermatol Venereol. 2017;31:e391–3.
Gupta M, Singh K, Lehl SS, Bhalla M. Recurrent erythema nodosum: a red flag sign of hidden systemic vasculitis. BMJ Case Rep. 2013;2013:bcr2013009507.
Kalaycı TÖ, Koruyucu MB, Apaydın M, Etit D, Varer M. Idiopathic granulomatous mastitis associated with erythema nodosum. Balkan Med J. 2016;33:228–31.
Kavehmanesh Z, Beiraghdar F, Saburi A, Hajihashemi A, Amirsalari S, Movahed M. Pediatric autoimmune hepatitis in a patient who presented with erythema nodosum: a case report. Hepat Mon. 2012;12:42–5.
Loetscher J, Fistarol S, Walker UA. Pyoderma gangrenosum and erythema nodosum revealing Takayasu’s arteritis. Case Rep Dermatol. 2016;8:354–7.
Balamurugesan K, Viswanathan S. Henoch-Schonlein purpura presenting sequentially as nodular rash, erythema nodosum, and palpable purpura. J Family Community Med. 2014;21:58–60.
Leung AK, Robson WL. Recurrent panniculitis in an adolescent boy with Prader–Willi syndrome. J Natl Med Assoc. 2006;98:1700–1.
Babamahmoudi F, Amuzgar A, Mousavi T, Davoodi L. Erythema nodosum: what should we consider about it? Casp J Intern Med. 2016;7:304–5.
Hueber AJ, Schett G, Manger B. Unilateral plantar erythema nodosum in sarcoidosis. Arthritis Rheumatol. 2018;70:297.
Lazaridou E, Apalla Z, Patsatsi A, Trigoni A, Ioannides D. Erythema nodosum migrans in a male patient with hepatitis B infection. Clin Exp Dermatol. 2009;34:497–9.
Hern AE, Shwayder TA. Unilateral plantar erythema nodosum. J Am Acad Dermatol. 1992;26:259–60.
Suarez SM, Paller AS. Plantar erythema nodosum: cases in two children. Arch Dermatol. 1993;129:1064–5.
Leung AK, Kellner JD. Group A beta-hemolytic streptococcal pharyngitis in children. Adv Ther. 2004;21:277–87.
Leung AK, Newman R, Kumar A, Davies HD. Rapid antigen detection testing in diagnosing group A beta-hemolytic streptococcal pharyngitis. Expert Rev Mol Diagn. 2006;6:761–6.
Polycarpou A, Walker SL, Lockwood DN. A systematic review of immunological studies of erythema nodosum leprosum. Front Immunol. 2017;8:233.
Saber M, Bourassa-Fulop C, Bouffard D, Provost N. Canadian case report of erythema nodosum leprosum successfully treated with prednisone and thalidomide. J Cutan Med Surg. 2010;14:95–9.
Leung AK, Barankin B. An annular lesion on the elbow. Am Fam Physician. 2016;93:397–8.
Vinay K, Chatterjee D, Yanamandra U, Saikia UN, Malhotra P, Dogra S. Leukemia cutis mimicking erythema nodosum or vice versa: a histological conundrum. Indian J Dermatol Venereol Leprol. 2018;84:91–3.
Papagrigoraki A, Gisondi P, Rosina P, Cannone M, Girolomoni G. Erythema nodosum: etiological factors and relapses in a retrospective cohort study. Eur J Dermatol. 2010;20:773–7.
Rohatgi S, Basavaraj KH, Ashwini PK, Kanthraj GR. Role of tetracycline in recalcitrant erythema nodosum. Indian Dermatol Online J. 2014;5:314–5.
Funding
There is no honorarium, grant, or other form of payment given to any of the author/coauthor.
Author information
Authors and Affiliations
Contributions
AKCL wrote the first draft of the manuscript, contributed to drafting and revising the manuscript, as well as a statement of whether an honorarium, grant, or other form of payment was given to anyone to produce the manuscript. KFL and JML contributed to drafting and revising the manuscript. All the authors have seen and approved the final version submitted for publication and take full responsibility for the manuscript.
Corresponding author
Ethics declarations
Ethical approval
Not needed.
Conflict of interest
No financial or non-financial benefits have been received or will be received from any party related directly or indirectly to the subject of this article.
Rights and permissions
About this article
Cite this article
Leung, A.K.C., Leong, K.F. & Lam, J.M. Erythema nodosum. World J Pediatr 14, 548–554 (2018). https://doi.org/10.1007/s12519-018-0191-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-018-0191-1